Dr. Rajesh Shah on Ankylosing Spondylitis
With over four decades of clinical experience, Dr. Rajesh Shah has managed Ankylosing Spondylitis using research-backed homeopathic protocols. His approach focuses on identifying individual triggers, reducing the frequency and intensity of inflammatory episodes, and supporting long-term disease stability. With extensive global documentation and outcome monitoring, Dr. Shah’s ethical and experience-based guidance forms the foundation of Ankylosing Spondylitis care at Life Force Homeopathy. Ankylosing Spondylitis cannot be fully cured, but with appropriate management, it can be effectively controlled.
180+
Countries
1100+
Ankylosing Spondylitis Patients Treated
30+
Team of Expert Doctors
40+
Years of experience
100% Satisfaction
If you are not satisfied after 6 weeks of treatment, you may return the unused medicines for a refund as per our policy. No cure is to be expected. Refunds are processed only when the parcel is returned within the stipulated time, with applicable administrative or shipping deductions. Our team is available to guide you through the refund process. For full terms, please visit our Detailed Refund Policy page.
What is Ankylosing Spondylitis?
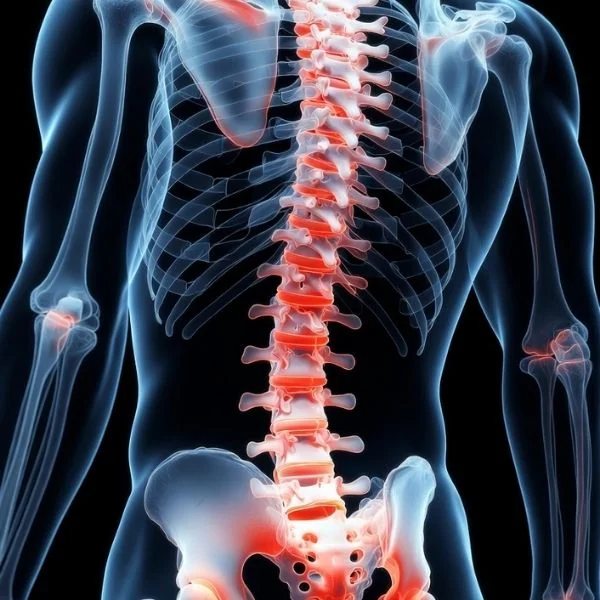
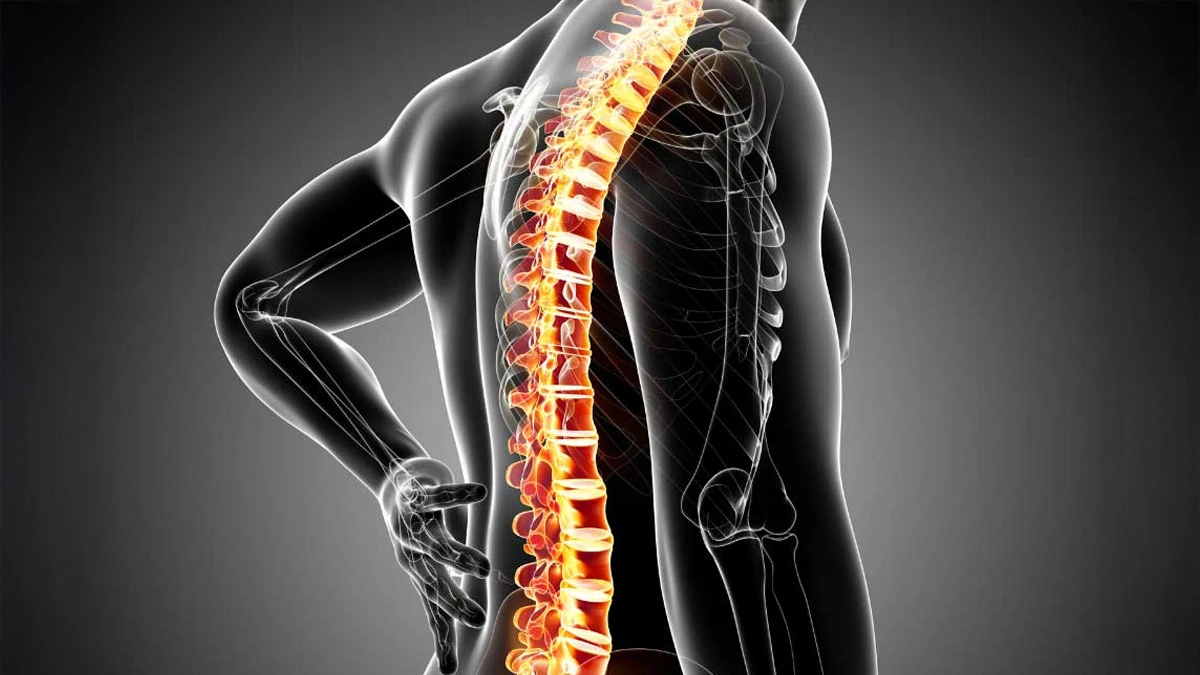
Ankylosing spondylitis (AS) is a chronic inflammatory and degenerative joint disorder. It primarily affects the spine and the sacroiliac joints that connect the spine to the pelvis. Inflammation of the joints, commonly referred to as arthritis, gradually leads to pain, stiffness, and reduced spinal flexibility.
As the disease progresses, spinal joints may fuse, resulting in persistent pain and restricted movement. This advanced stage is often called “bamboo spine.” When rib joints are involved, chest expansion may be reduced, causing breathing difficulty. In some cases, Ankylosing Spondylitis may also affect the eyes, heart, lungs, or, rarely, the kidneys.
Genetic factors play a significant role. Many patients carry the HLA-B27 gene, although not everyone with this gene develops the disease. Early diagnosis and structured management can help slow disease progression and reduce long-term complications.
-
Alopecia Areata
-
Ankylosing Spondylitis
-
Asthma
-
Cancer
-
Child Asthma
-
Eczema
-
Frequent Colds
-
Hair Fall
-
Hepatitis C
-
Irritable Bowel Syndrome (IBS)
-
Lichen Planus
-
Psoriasis
-
Trigeminal Neuralgia
-
Ulcerative Colitis
-
Underactive Thyroid
-
Urticaria
-
Vitiligo
Find out your chances of recovery, now
Select the disease from the list

STEP 01
Select your condition

STEP 02
Submit the Form

STEP 03
Get report Instantly
Understanding Ankylosing Spondylitis
Types of Ankylosing Spondylitis
Axial Ankylosing Spondylitis
PPrimarily affects the spine and sacroiliac joints, leading to inflammatory back pain and possible fusion.
Peripheral Ankylosing Spondylitis
Involves joints outside the spine such as knees, ankles, and shoulders.
Non-Radiographic Axial Spondyloarthritis
Early disease stage with symptoms present but no visible X-ray changes; MRI detects inflammation.
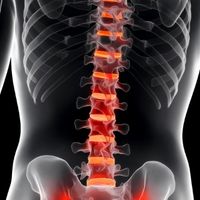
Non-Radiographic axSpA
Short episodes of vision loss or visual disturbances in one eye followed by headache.
Our Expertise
- With over 40 years of experience since 1985, Dr. Rajesh Shah has successfully treated numerous patients.
- With Ankylosing Spondylitis across the world, using research-based homeopathic molecules alongside conventional therapy.
- At Life Force, our experience shows that early introduction of homeopathy significantly controls pain, stiffness, and disease progression at all stages.
- Patients receive honest guidance on prognosis and realistic expectations from homeopathic treatment.
Homeopathic Treatment for Ankylosing Spondylitis
Homeopathic treatment for Ankylosing Spondylitis focuses on long-term management of this chronic autoimmune condition. Treatment aims to control disease activity, ease pain and stiffness, improve mobility, and support overall well-being. As a deep-seated condition, Ankylosing Spondylitis requires personalized internal remedies selected based on physical symptoms, genetic tendencies, immune response, and emotional factors. This supportive approach is designed to enhance quality of life safely and ethically.
Case Studies

Ankylosing Spondylitis
Pain & Discomfort Due To Ankylosing Spondylitis Reduced With Homeopathy At Life Force
Mr. T.J.V (PIN 16991) visited the clinic on 15th September 2012 for the complaints of his joint pains.Mr. T.J.V presented…
Ankylosing Spondylitis
A young female tides over the crisis of ankylosing spondylitis with homeopathic medication.
A young female Mrs. M.W. (Pin Number L-9585) eagerly visited the clinic with complaints of ankylosing spondylitis. She was in distress…

Ankylosing Spondylitis
Ankylosing spondylitis gets wonderful recovery with homeopathy leading to a pain free life.
Mr. V. K. (PIN Number L-8425) came to the clinic for treatment of backache. He had severe low back pain.…
FAQ on Ankylosing Spondylitis
Expert Answers to Common Questions
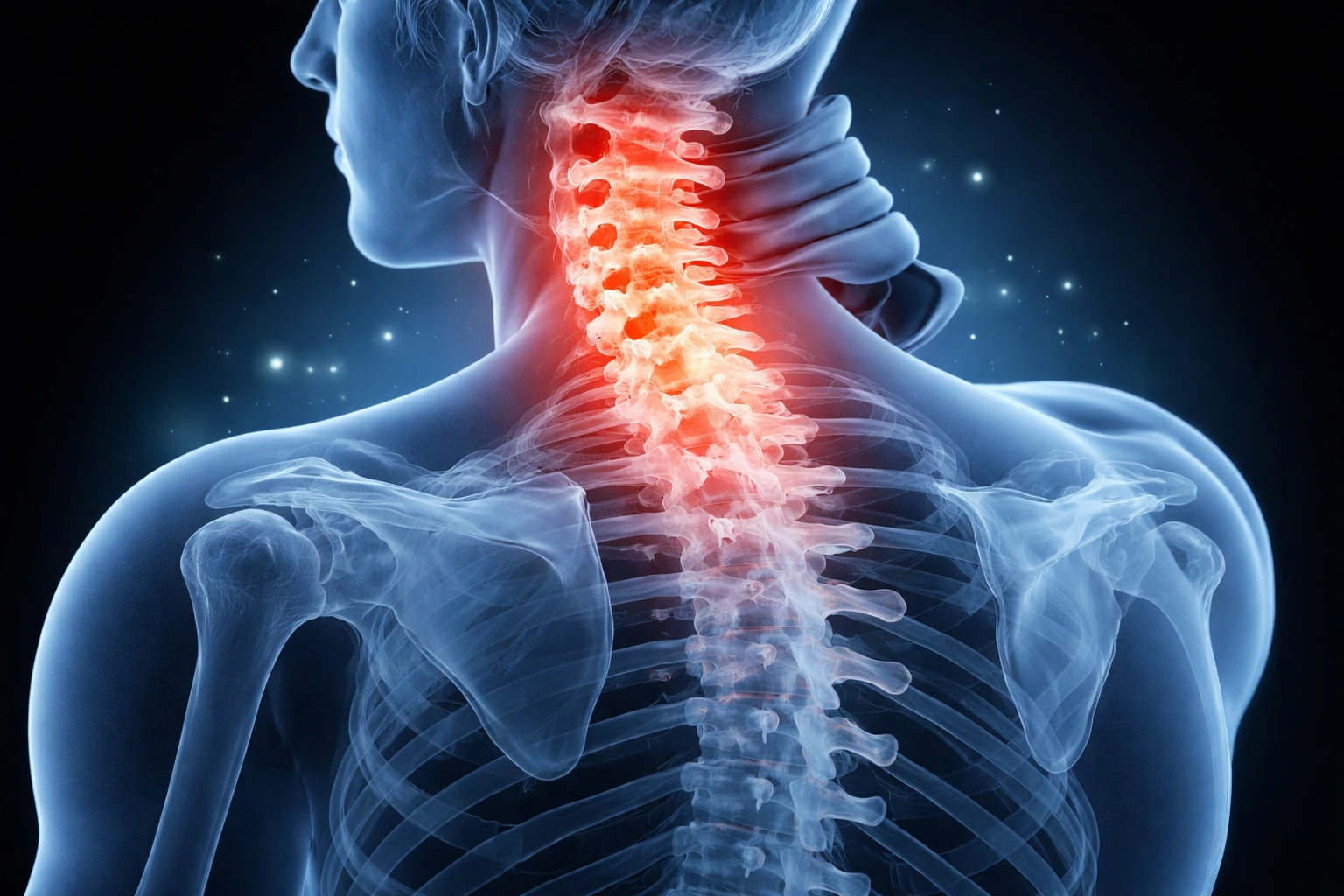
Stiffness and pain in the joints, especially the neck and/or lower back, are among the early signs. Some patients may have hip pain and stiffness. Over time, the joints and spine tend to become stiff.
Jerky movements and overstraining must be avoided. Exercises such as running, jogging, jumping, and weightlifting are best avoided
A blood test for the HLA-B27 gene is mandatory for diagnosing ankylosing spondylitis. A positive test in the presence of clinical symptoms may help to confirm the diagnosis. However, a negative test does not always rule out the disease, and similarly, a positive test may not confirm ankylosing spondylitis, as false-positive results can occur.
Yes, the blood test is an HLA-B27 test.
Genetic and immunological factors cause ankylosing spondylitis. The HLA-B27 gene is responsible for this inflammatory autoimmune disease, which often leads to deformity.
Early cases may be mildly painful. As the disease progresses, some patients may experience more pain and stiffness. Some patients may experience very little pain, while it could be moderately to severely painful in many patients over many years. The symptoms may vary from patient to patient. With a proper lifestyle, exercise, and medications, the symptoms may be kept under control.
Regular walks and exercises may help to reduce the symptoms of ankylosing spondylitis.
Ankylosing spondylitis may affect the spine, neck, back, knees, shoulders, hips, and eyes (uveitis). Not all patients may have all the organs or joints affected.
Spondylosis refers to stiffness and pain in the spinal disk and joints, related to aging. Pain, stiffness, and restricted mobility are the early signs and symptoms of spondylosis.
Related Diseases
Ask Dr. Shah
Dr. Rajesh Shah, MD (Homeopathy), is a renowned Mumbai-based homeopath, recognized for treating patients from 180 countries, including celebrities and underprivileged individuals.
Contact Us