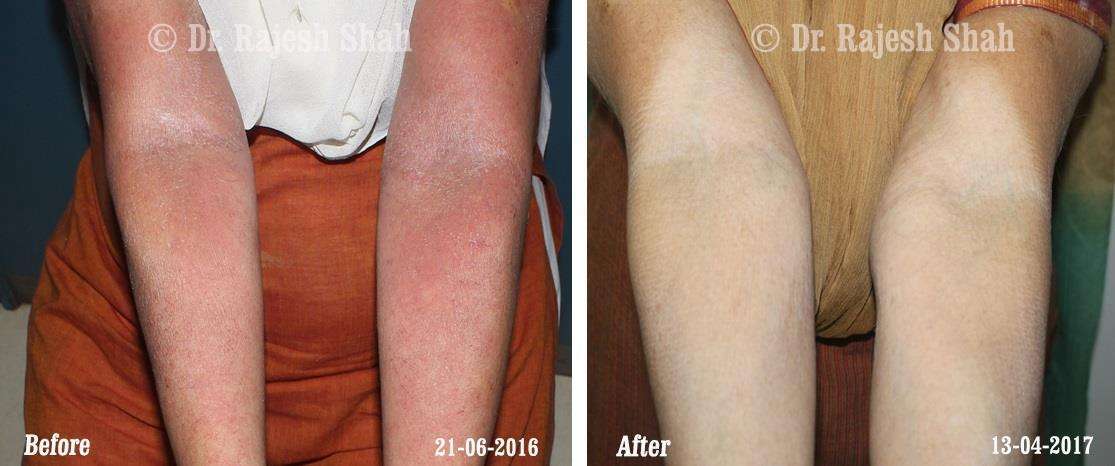
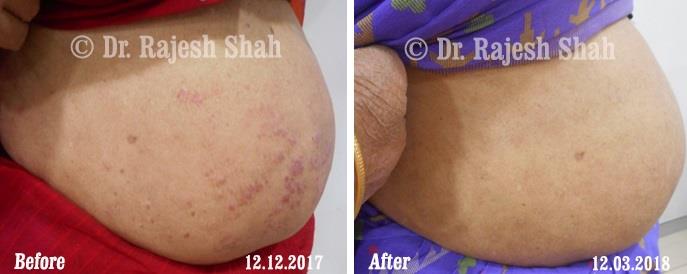
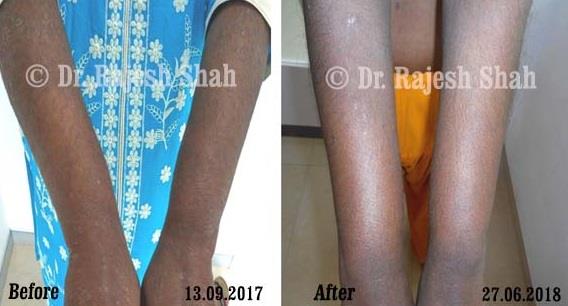
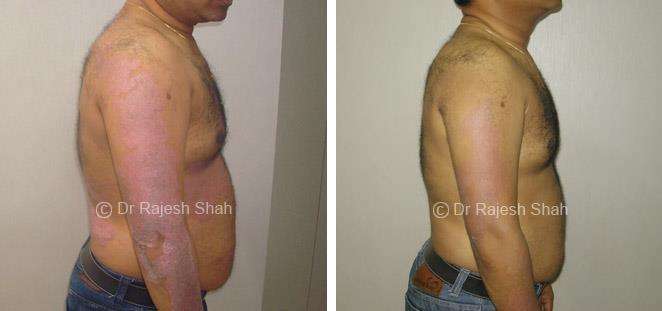
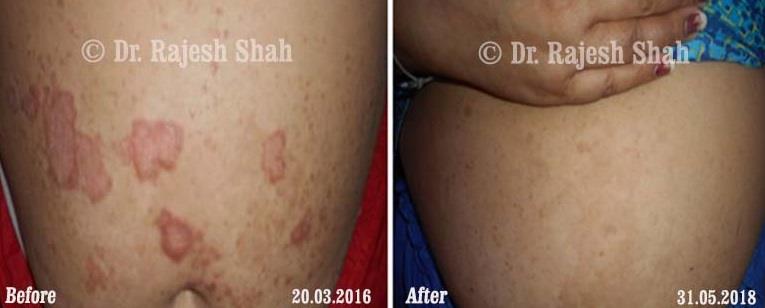
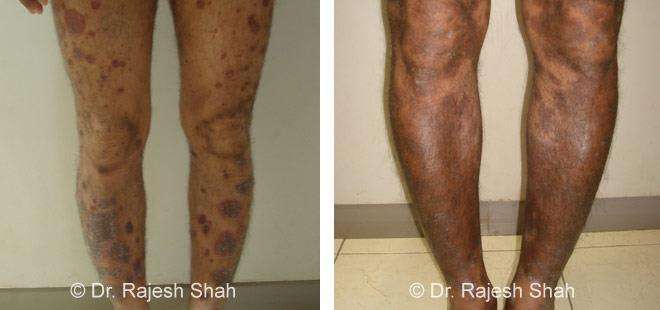
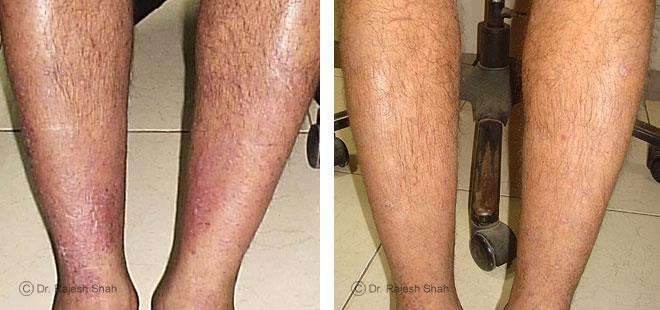
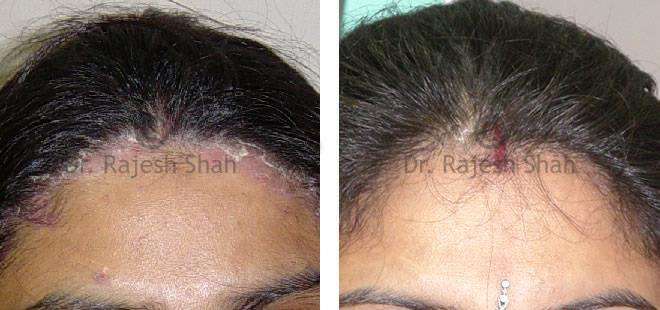
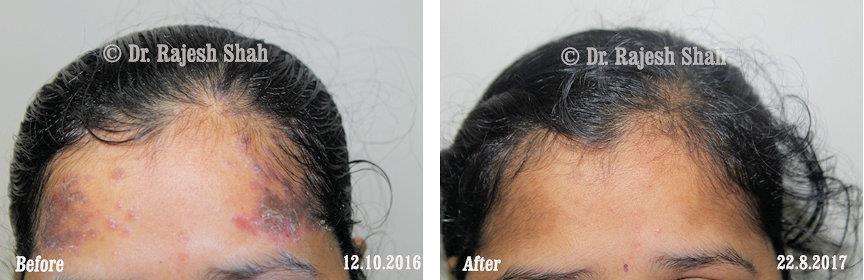
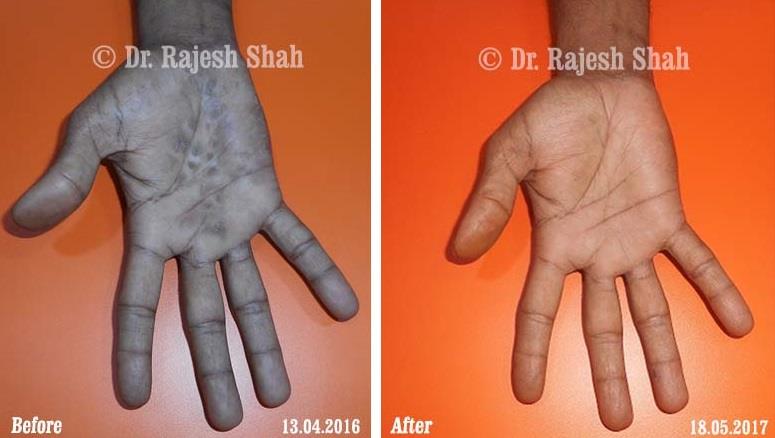
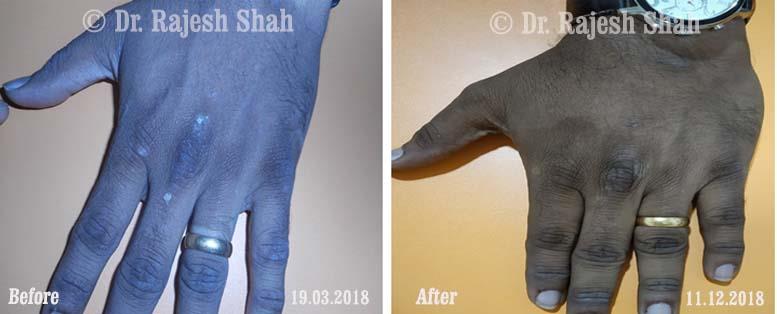
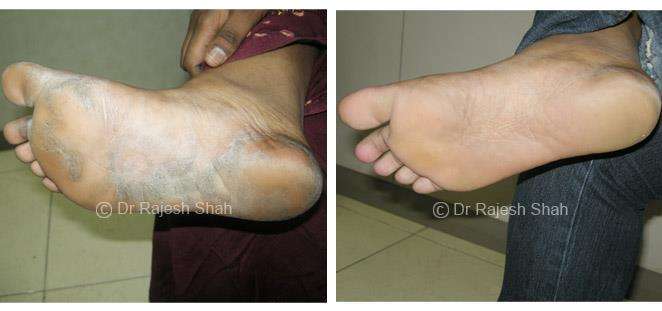
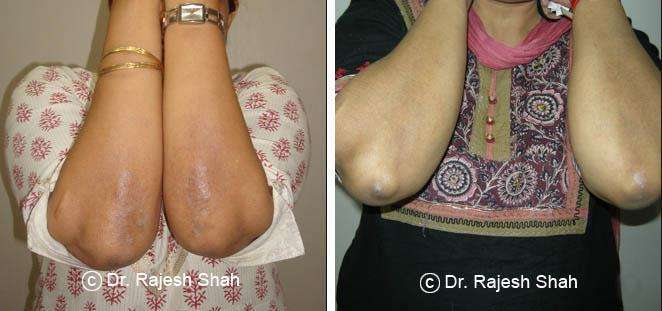
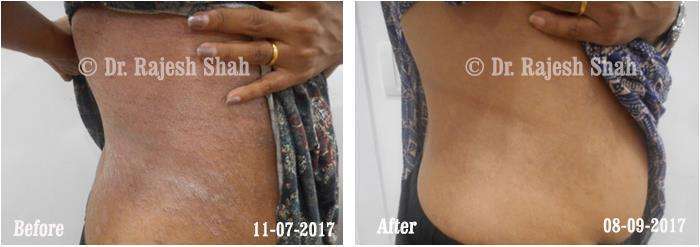
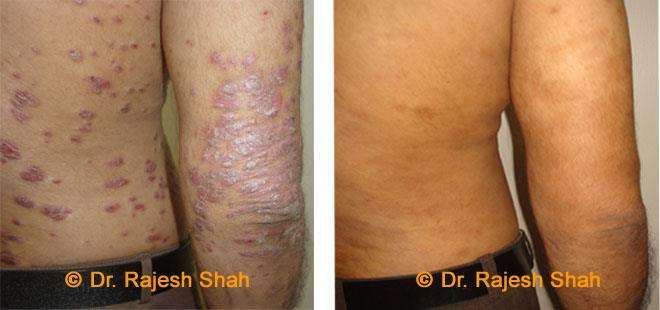
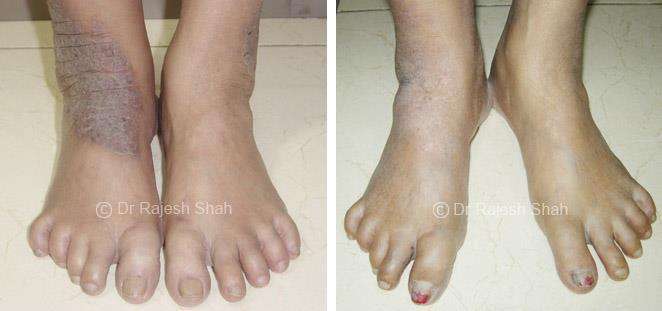
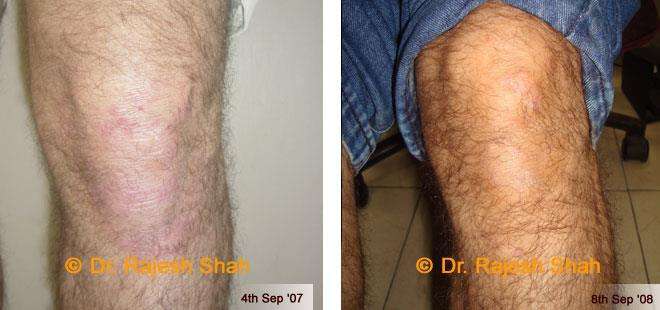
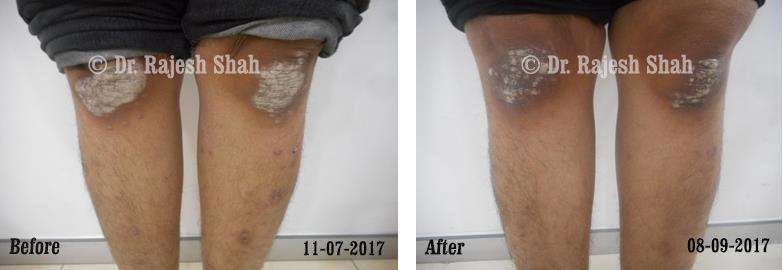
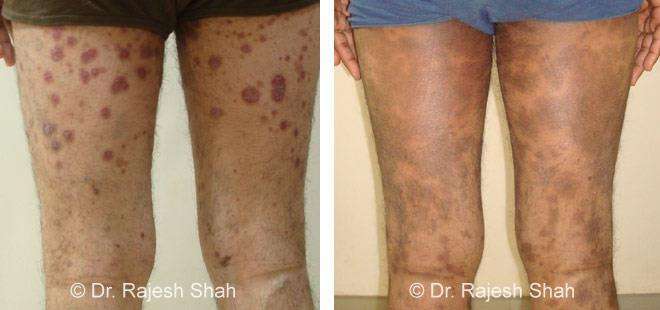
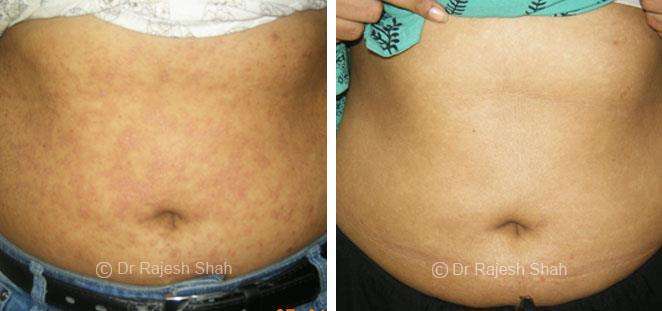
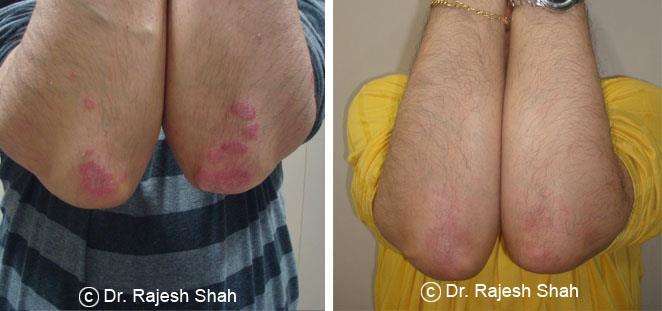
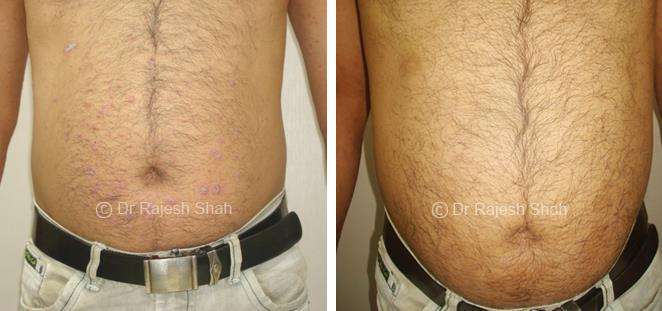
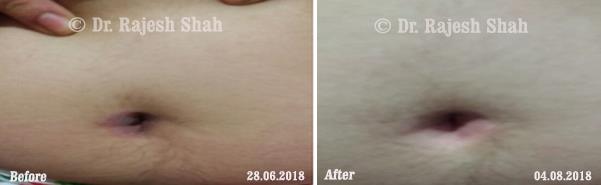
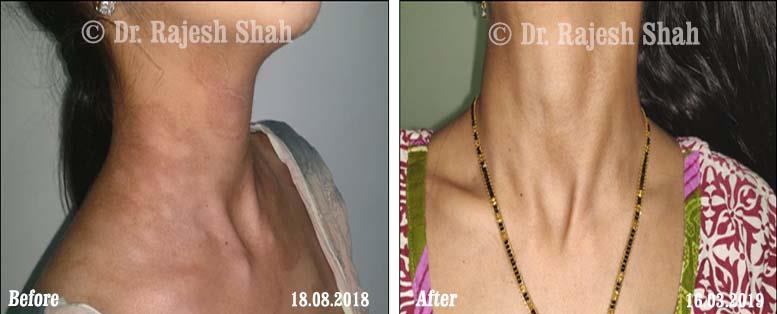
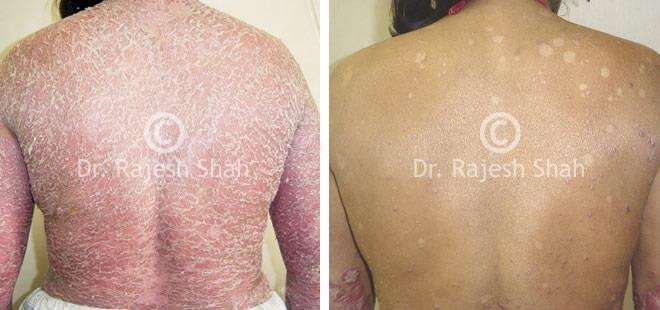
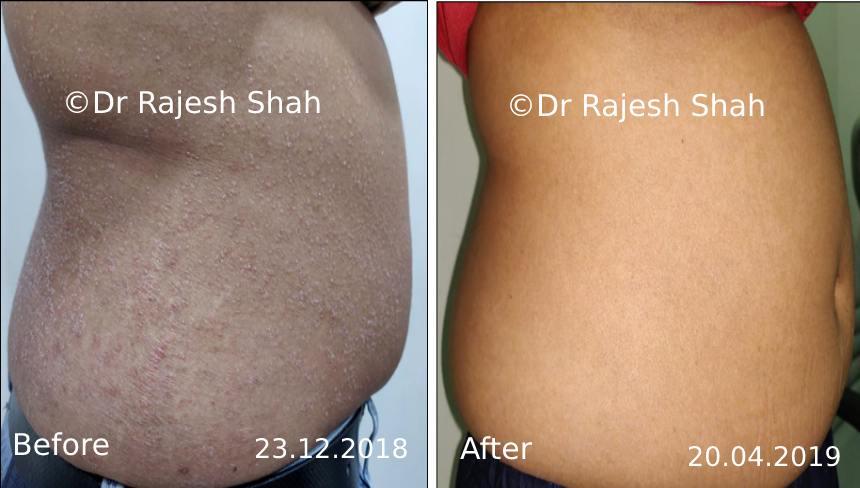
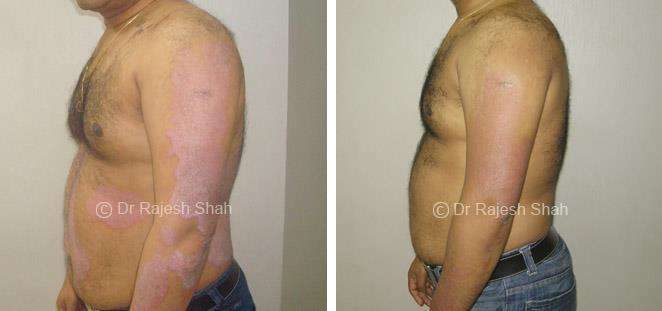
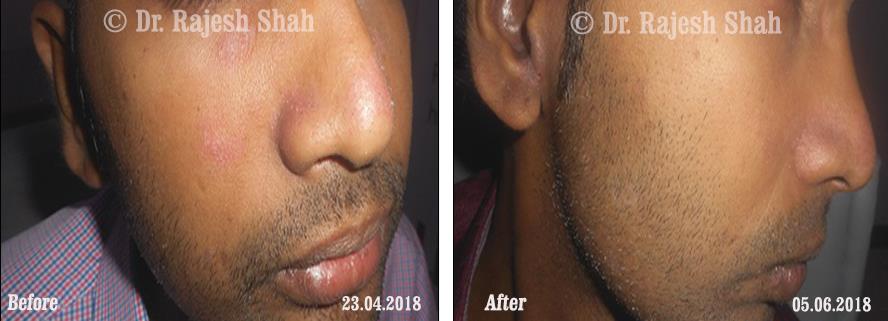
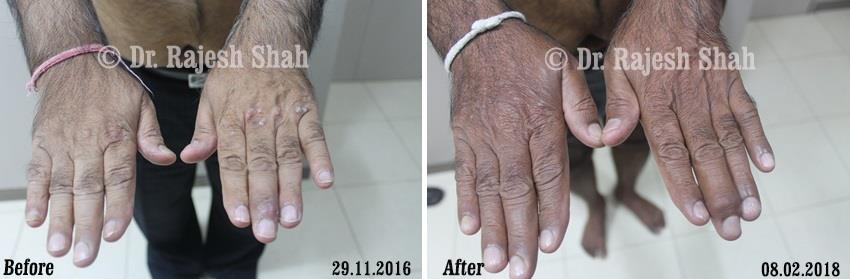
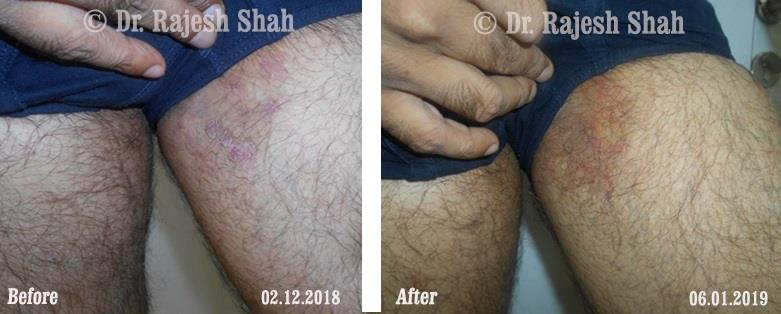
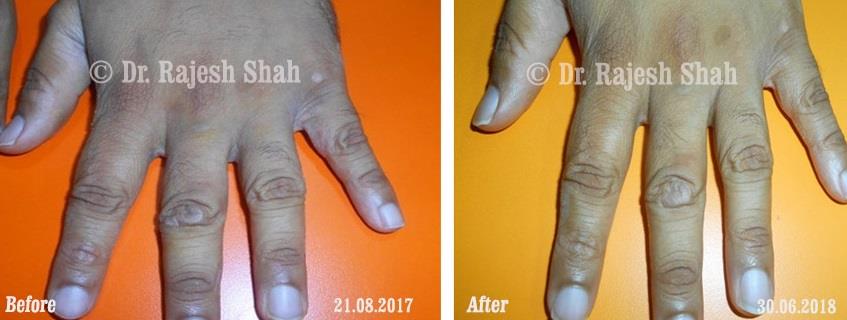
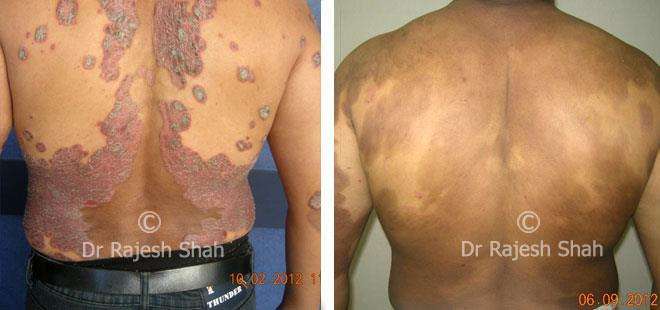
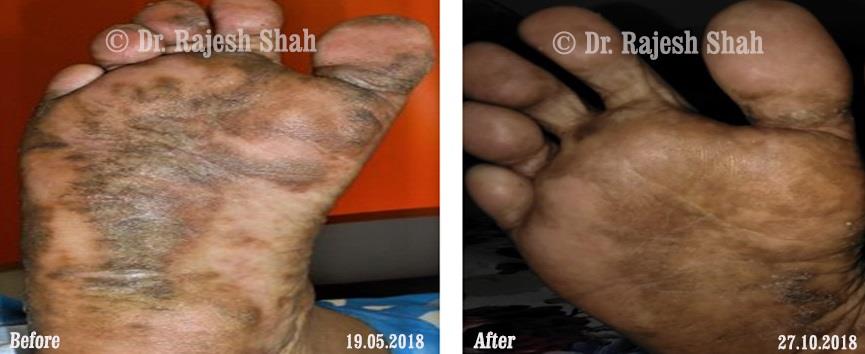
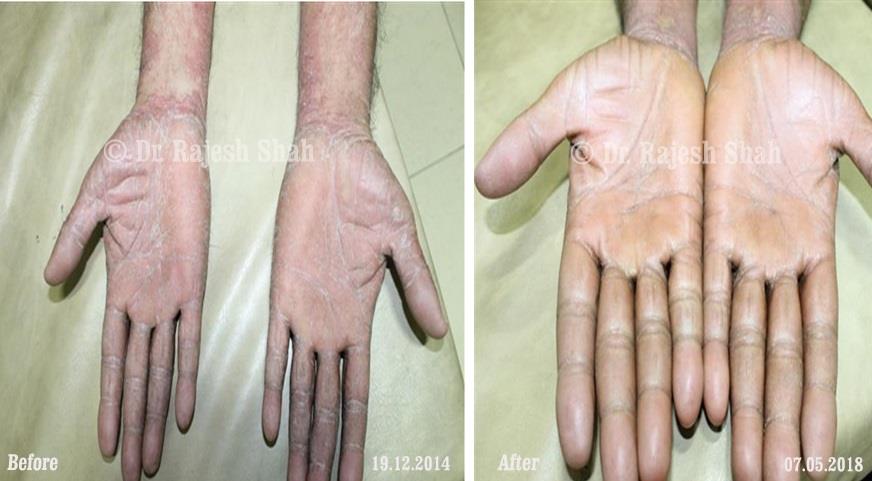
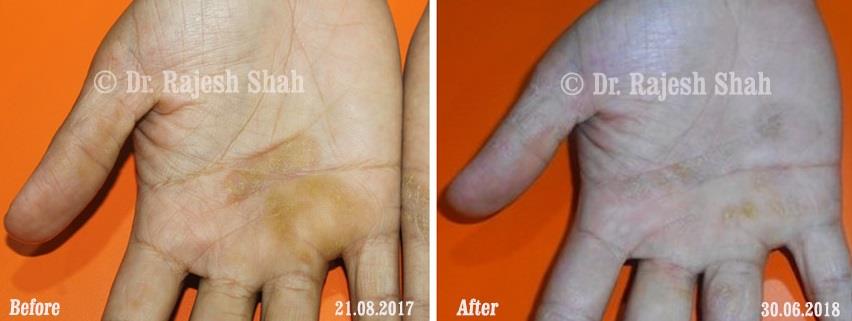
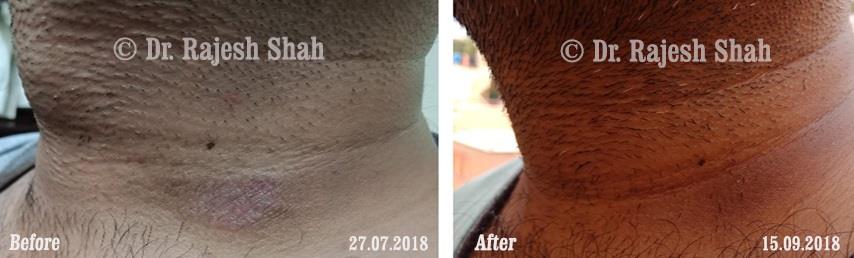
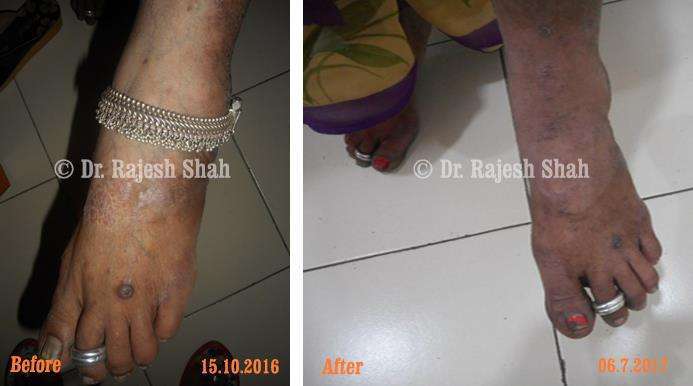
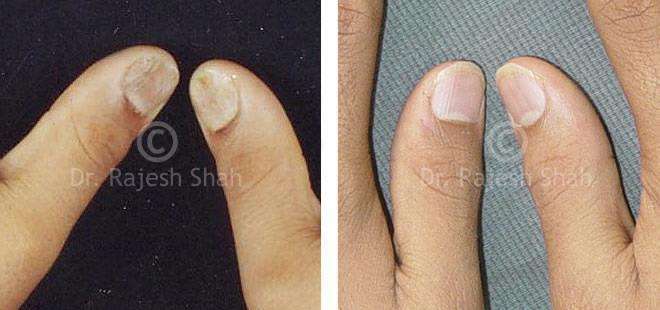
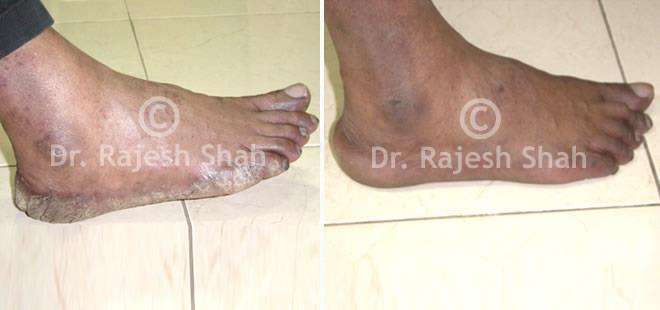
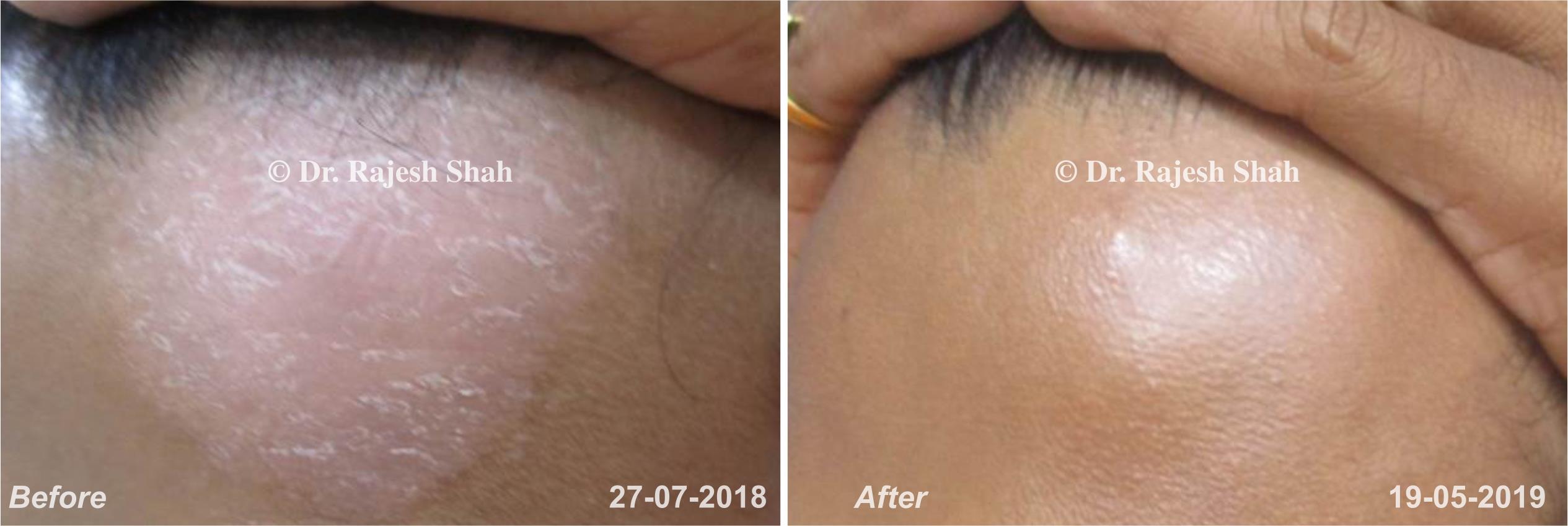
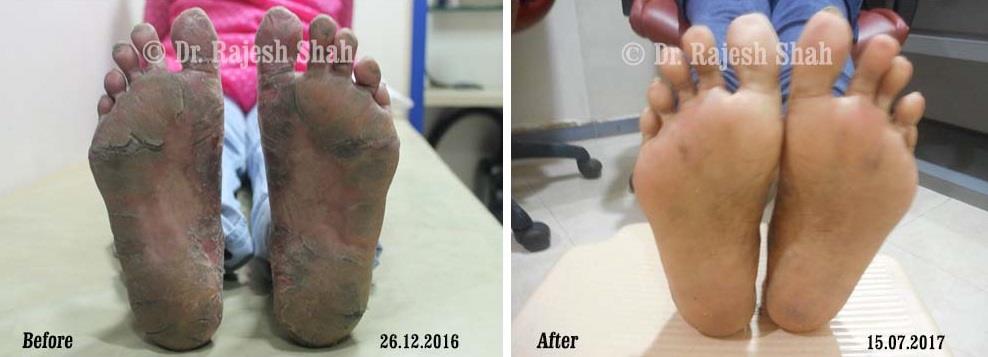
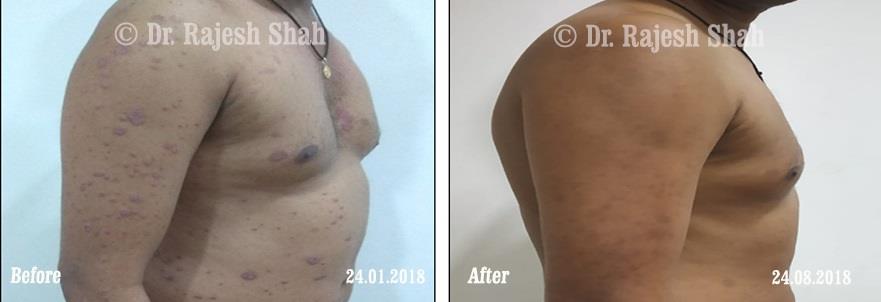
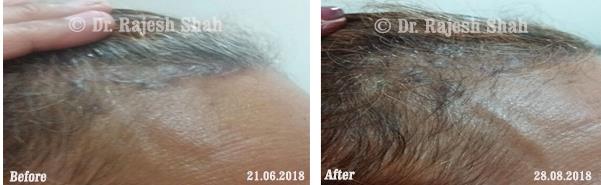
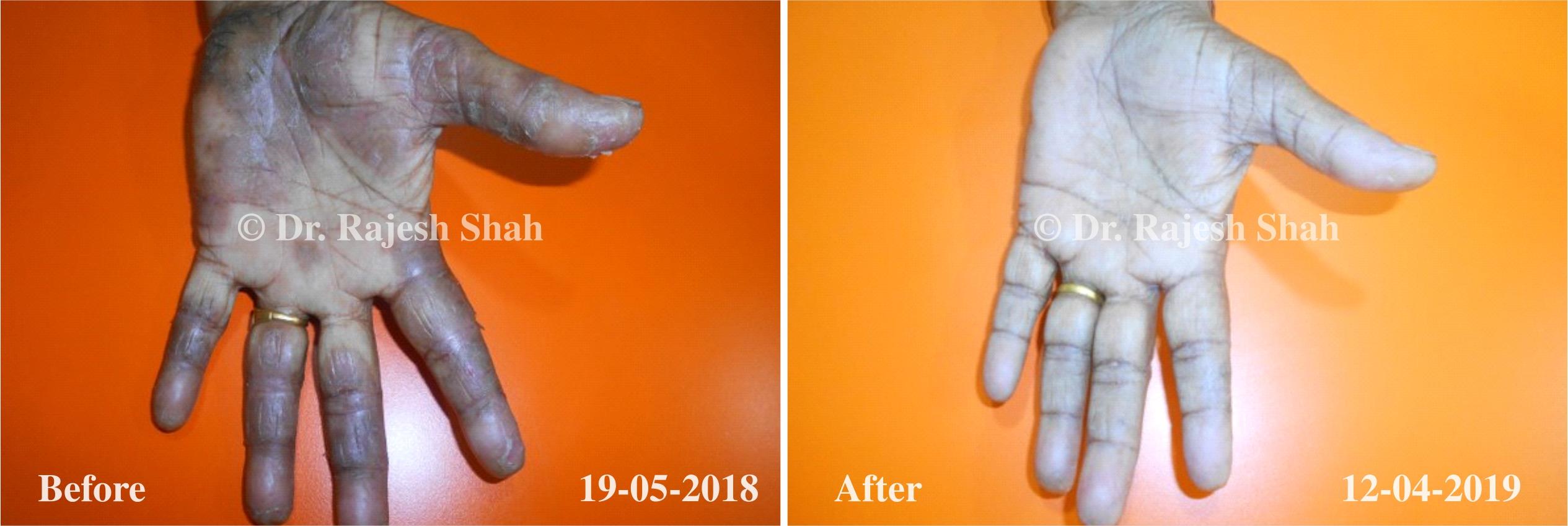
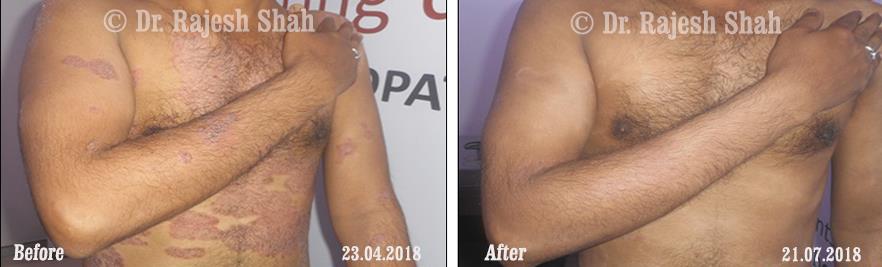
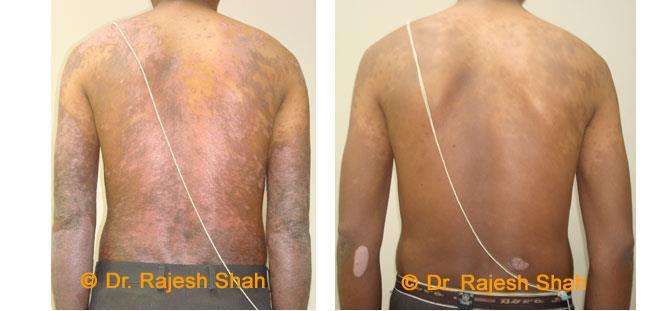
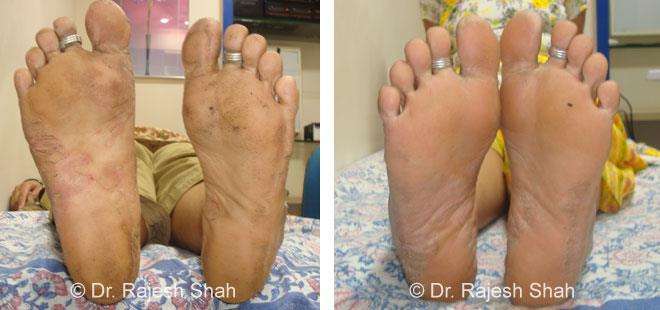
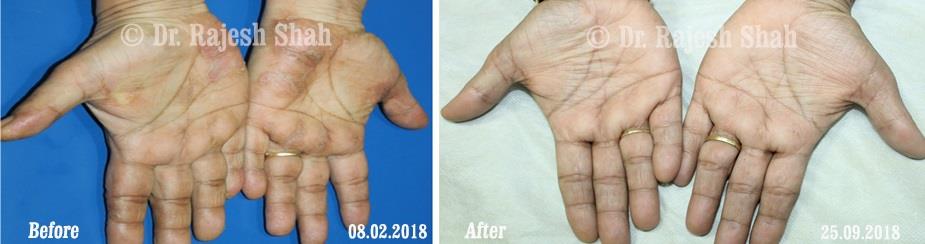
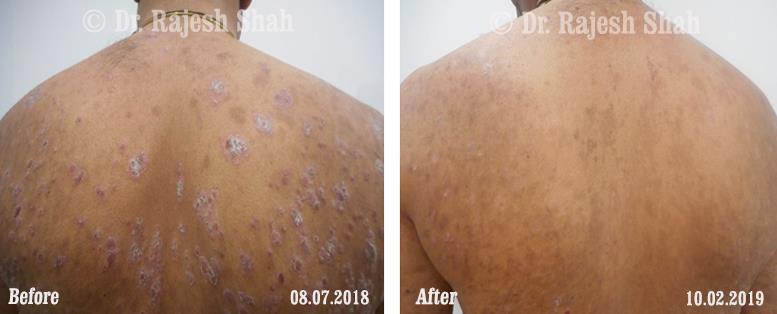
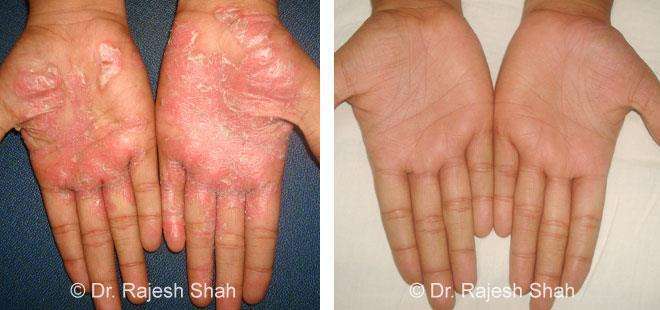
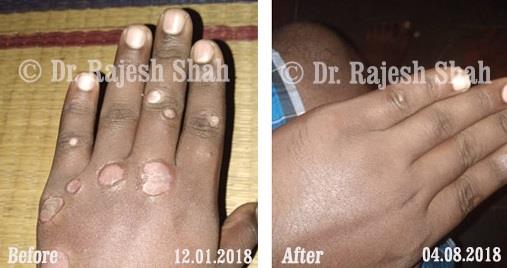
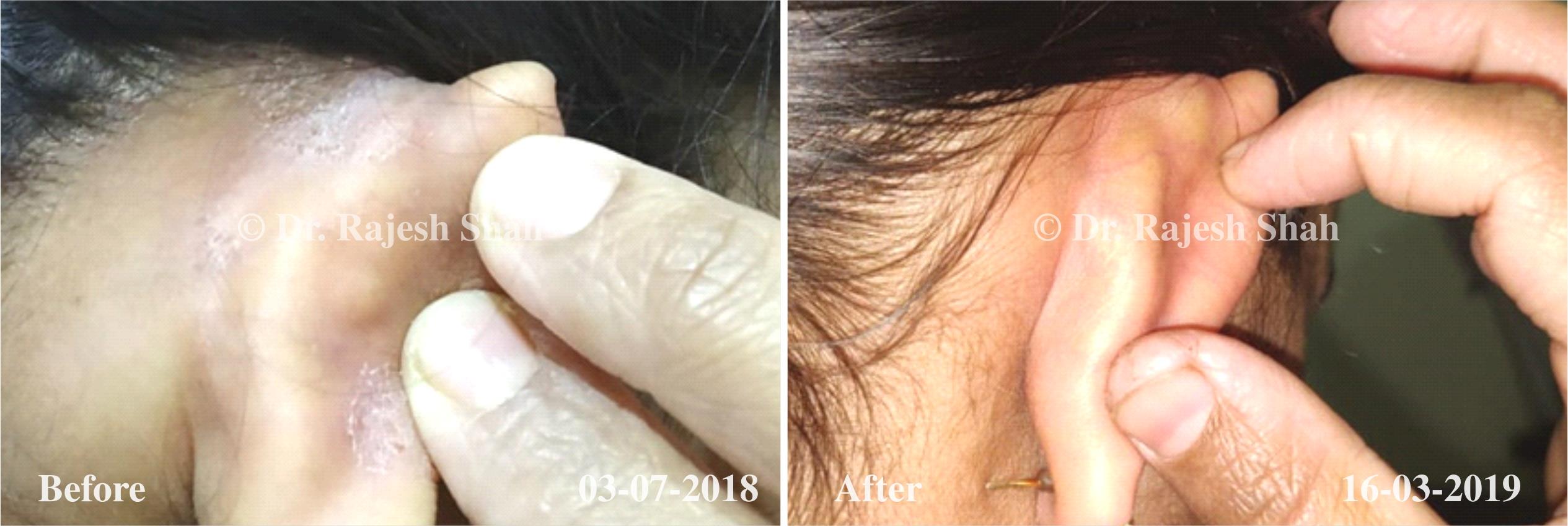
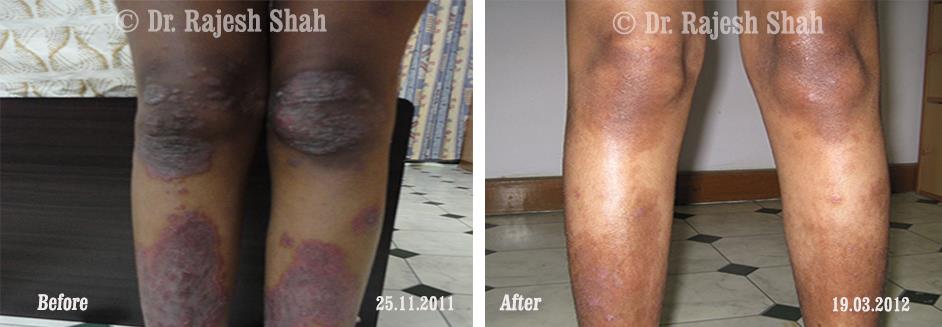
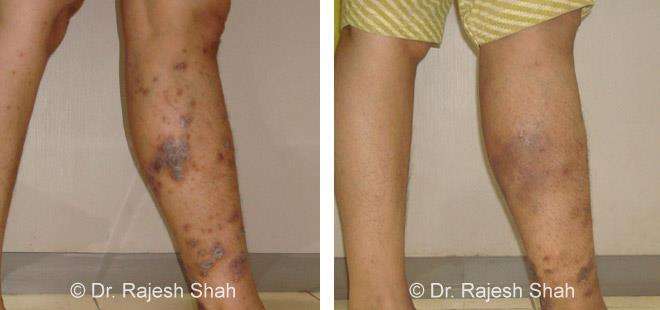
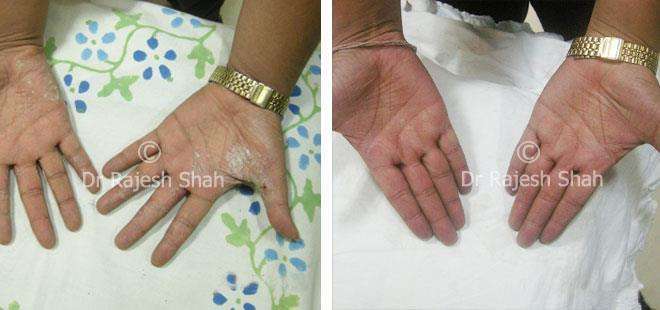
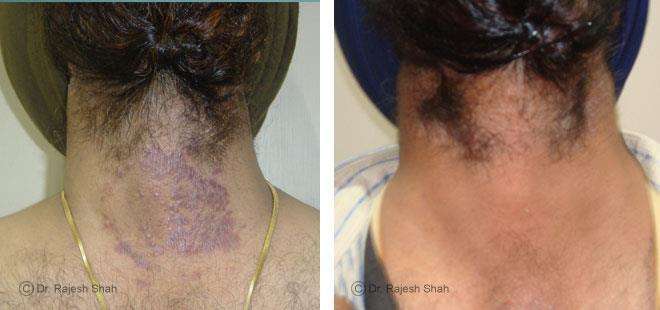
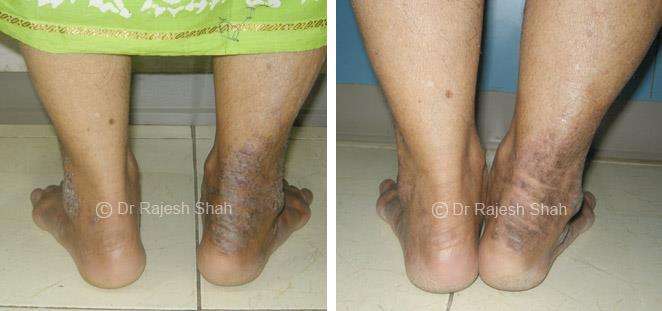
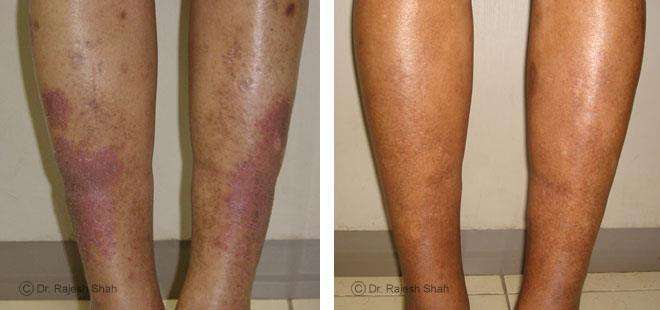
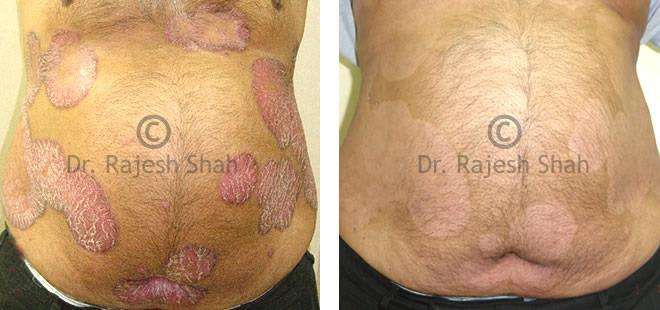
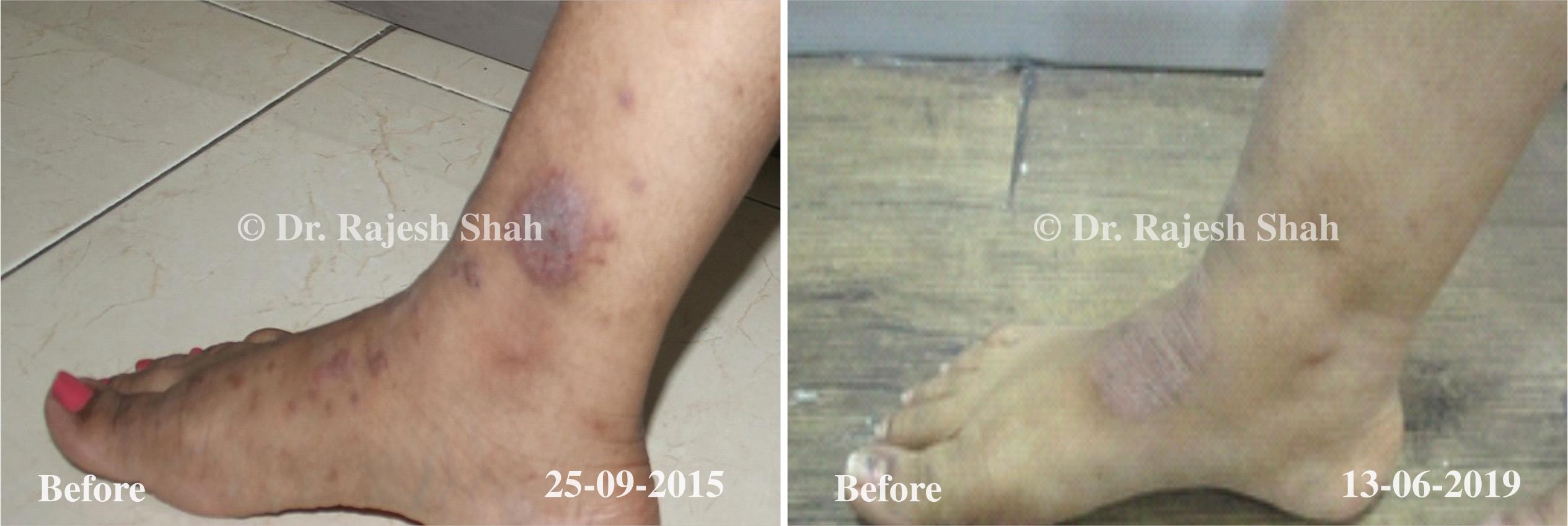
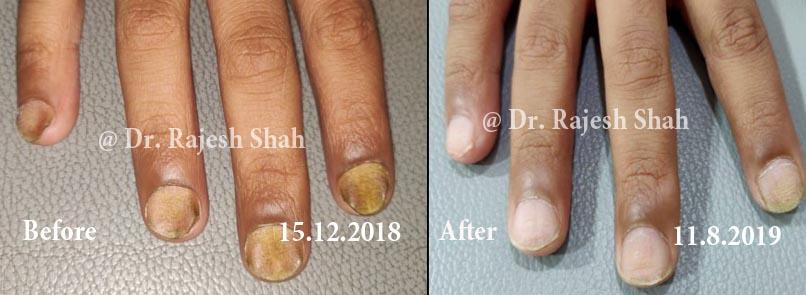
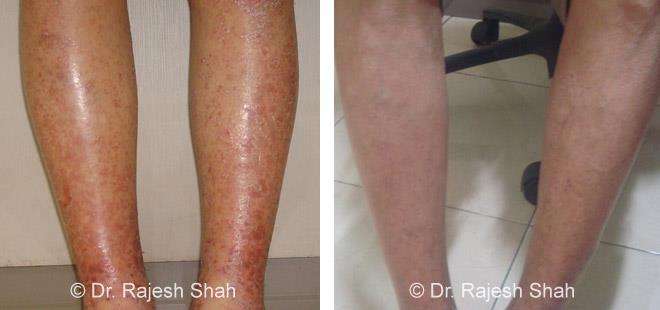
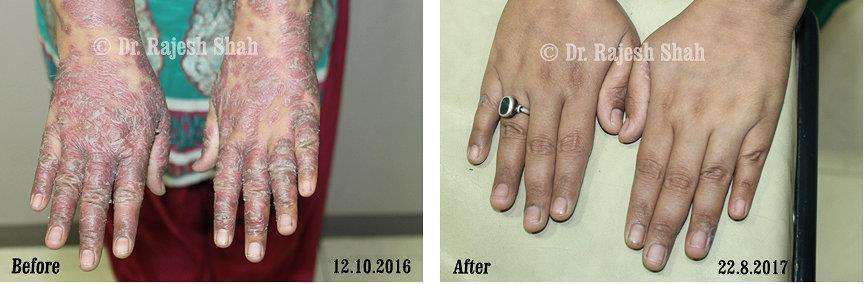
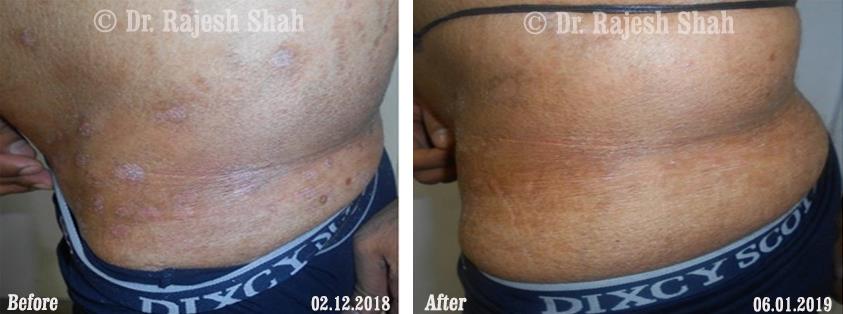
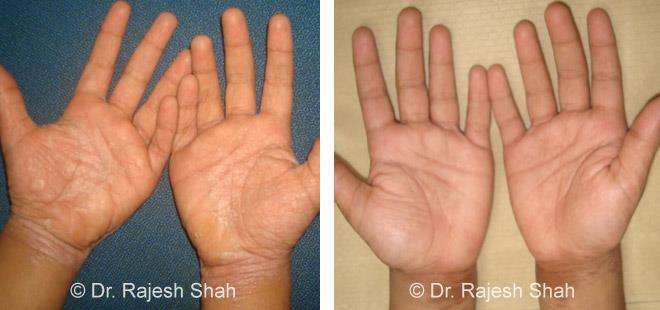
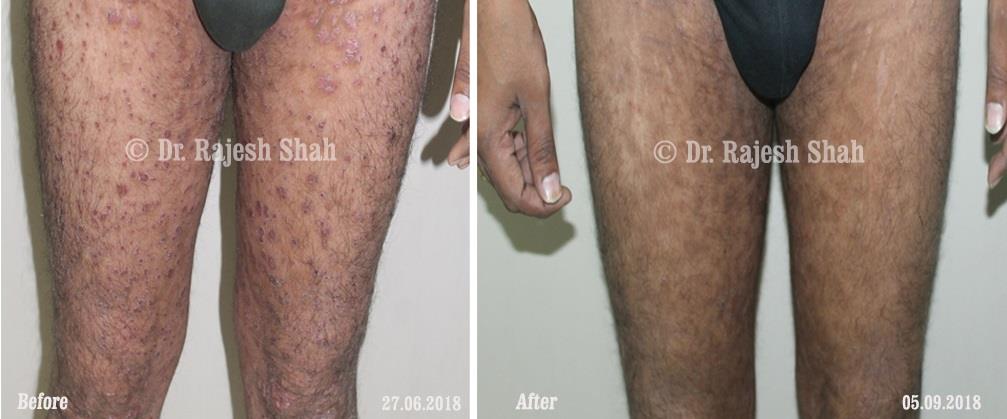
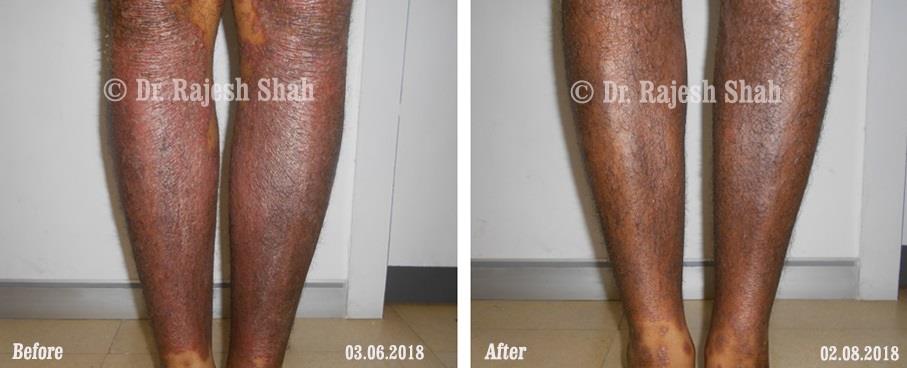
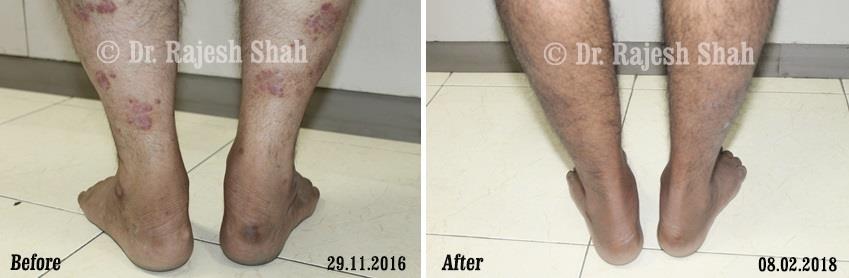
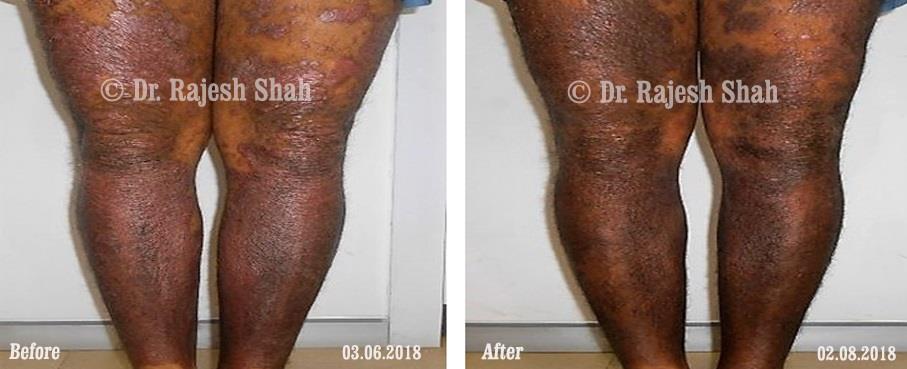
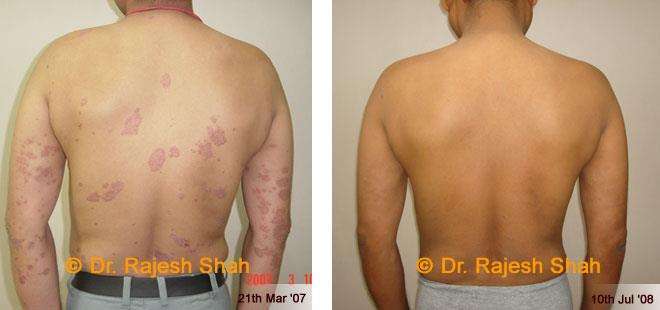
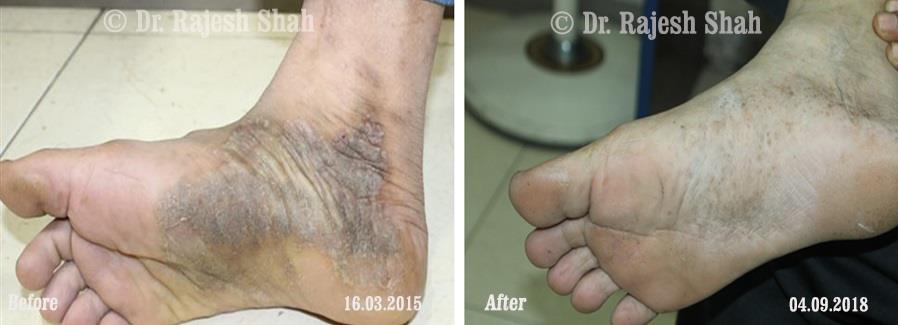
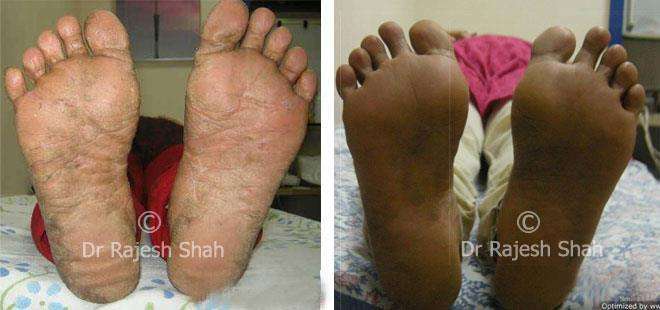
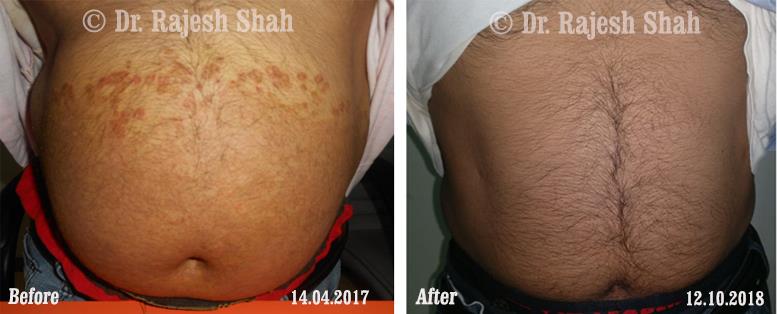
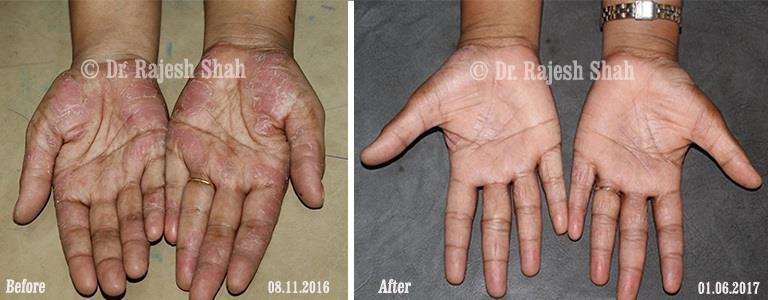
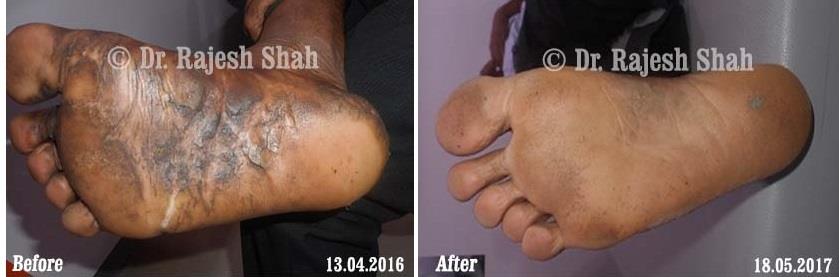
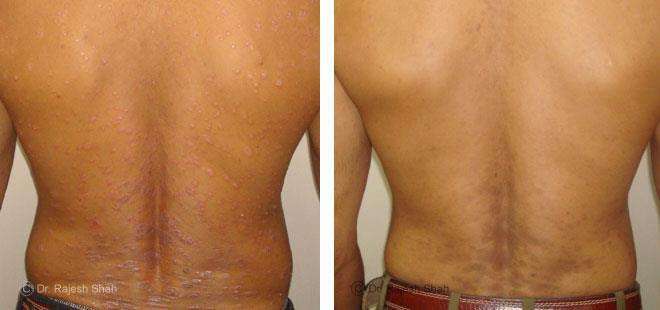
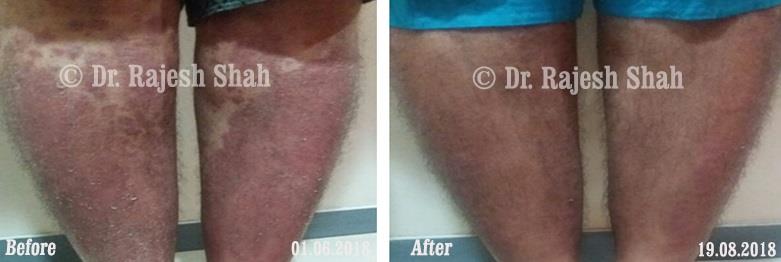
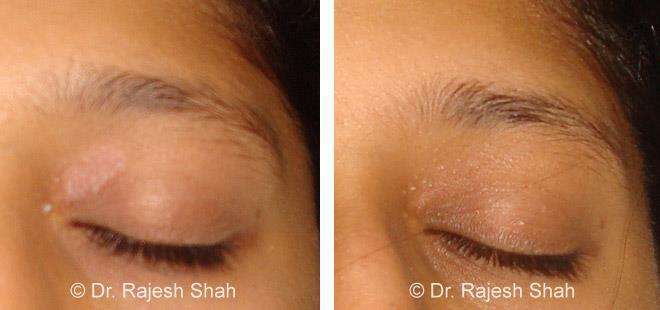
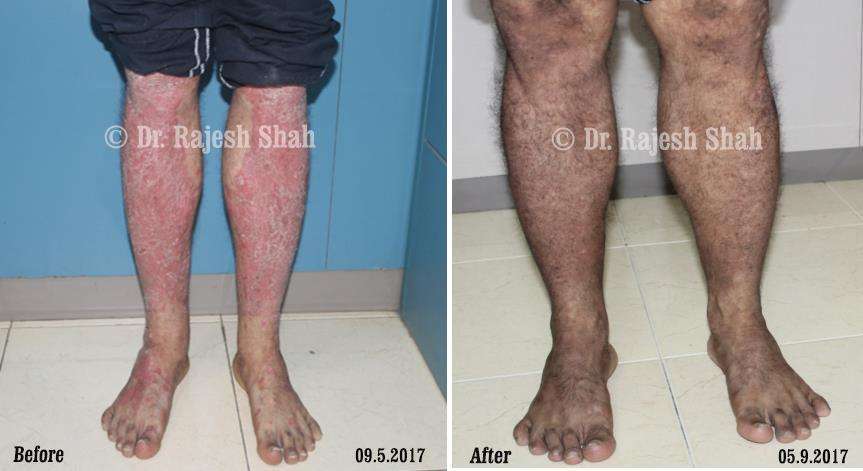
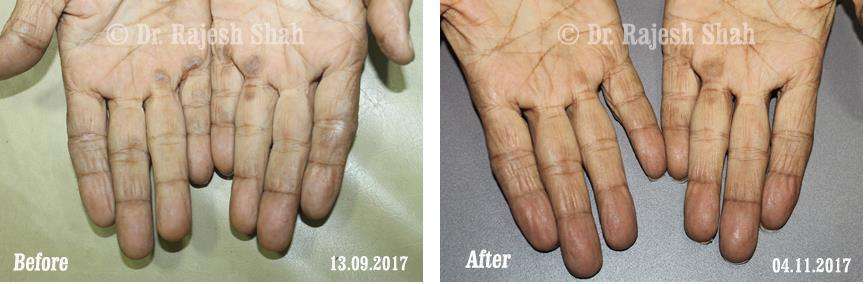
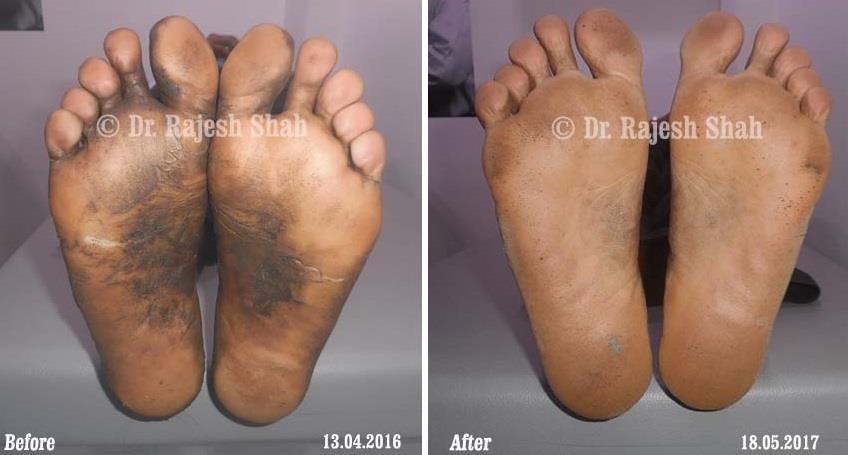
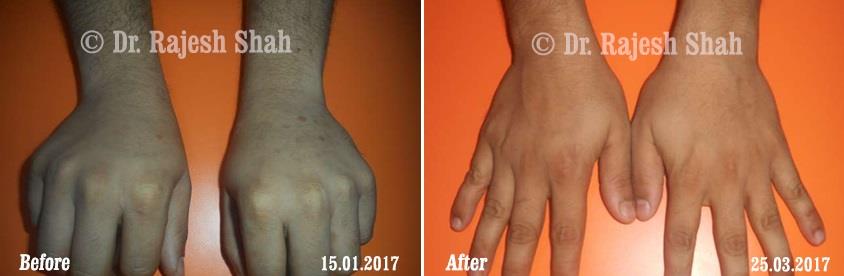
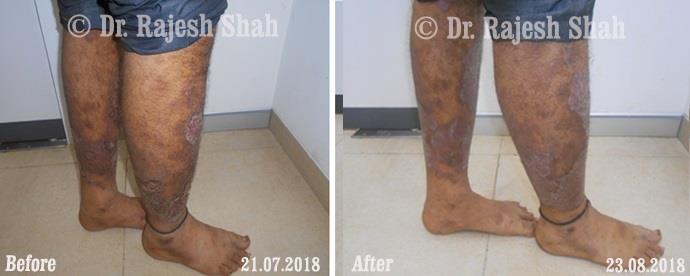
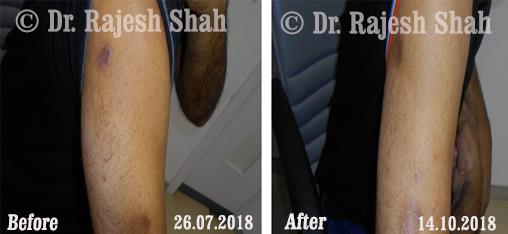
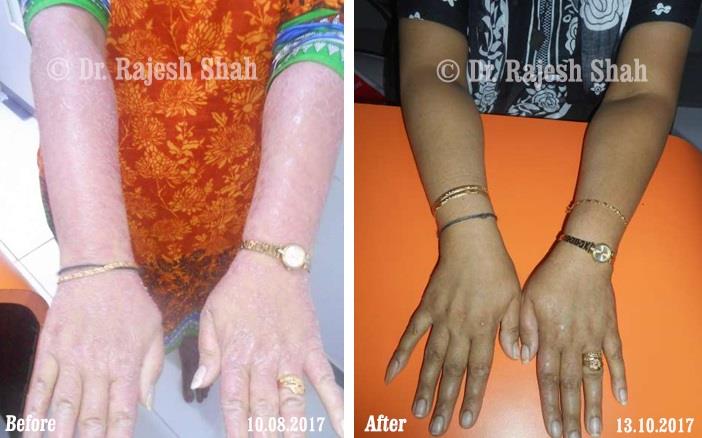
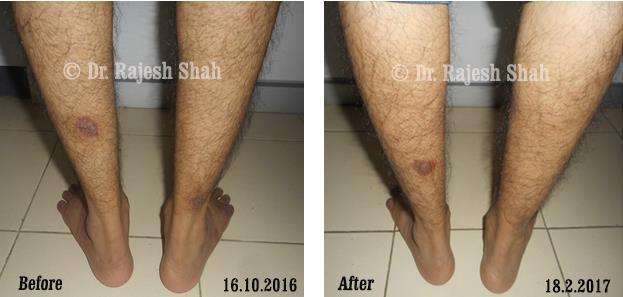
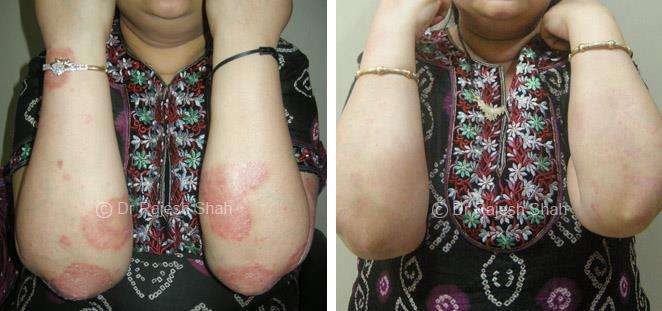
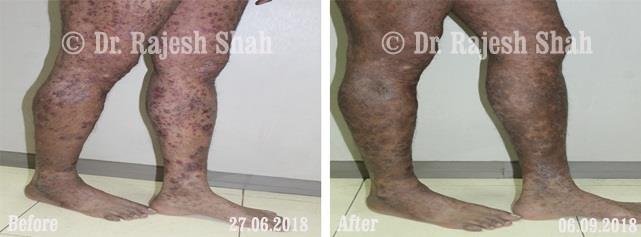
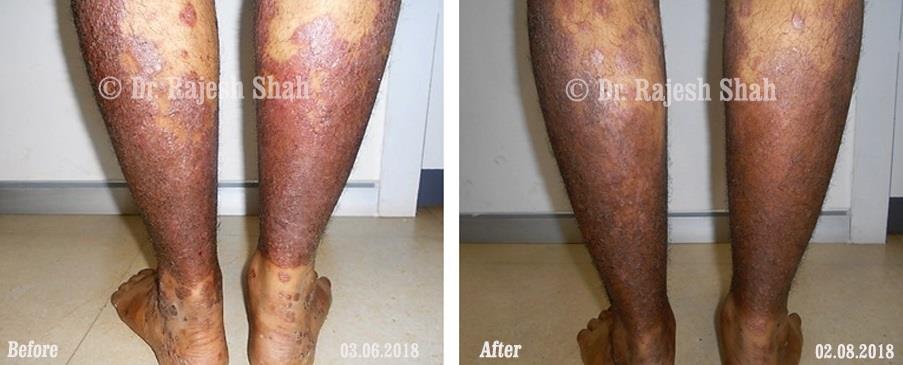
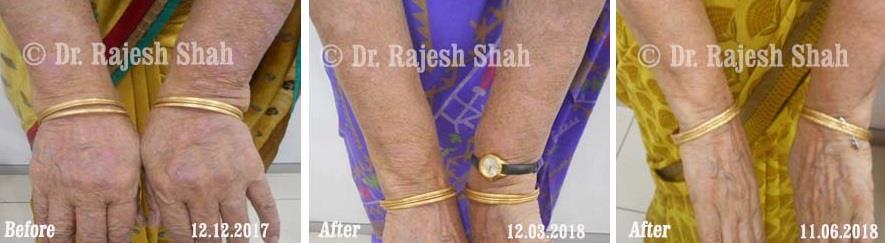
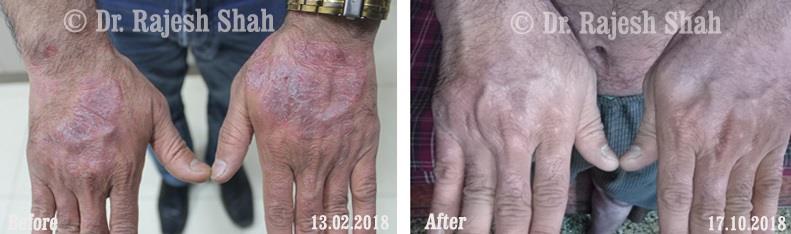
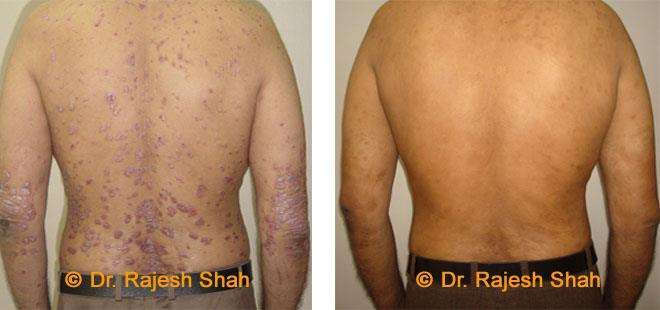
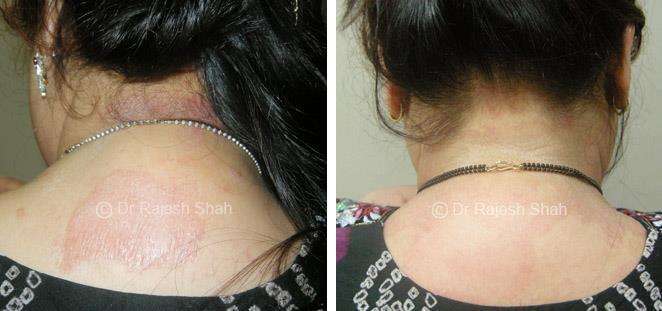
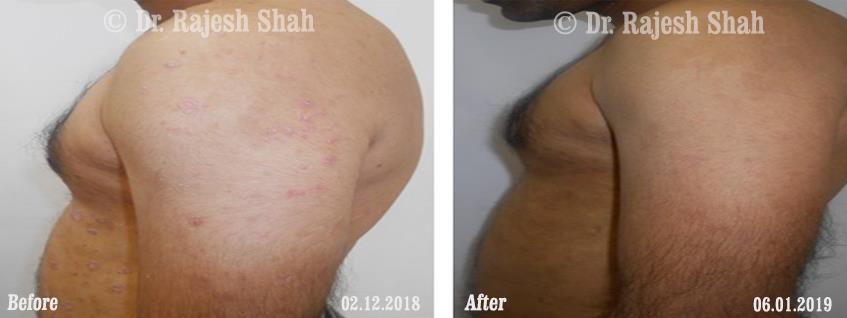
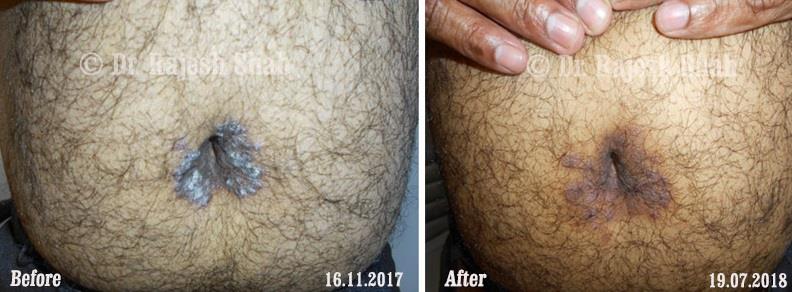
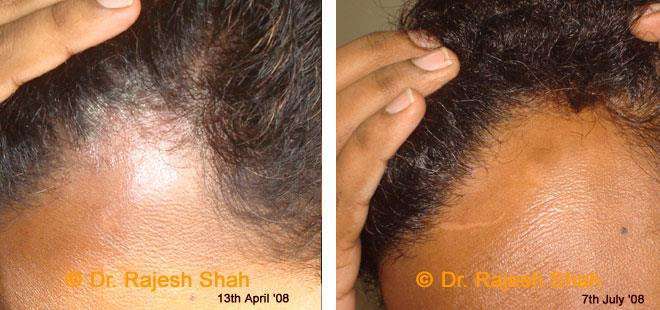
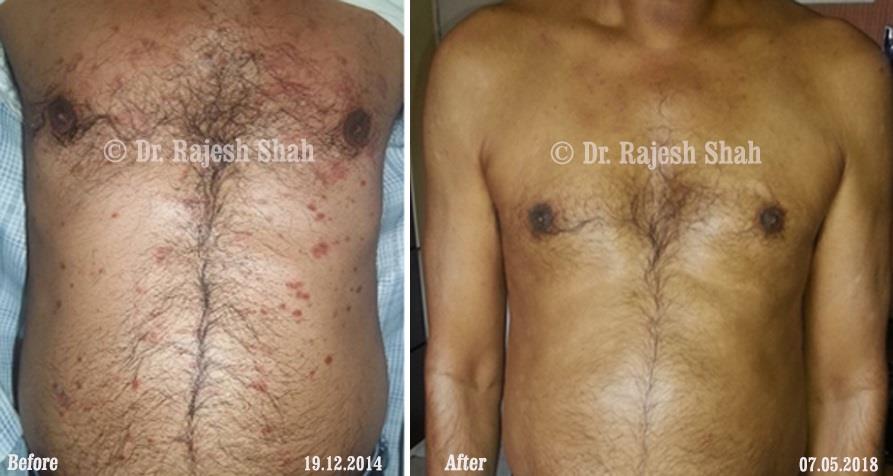
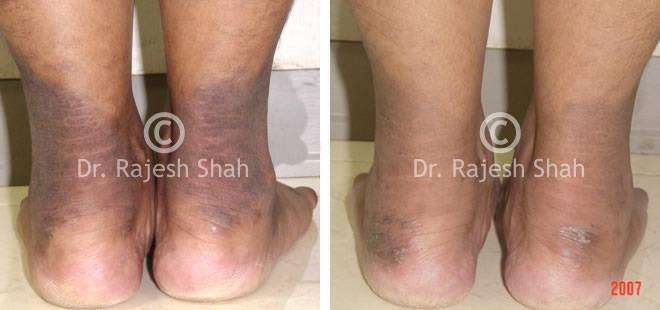
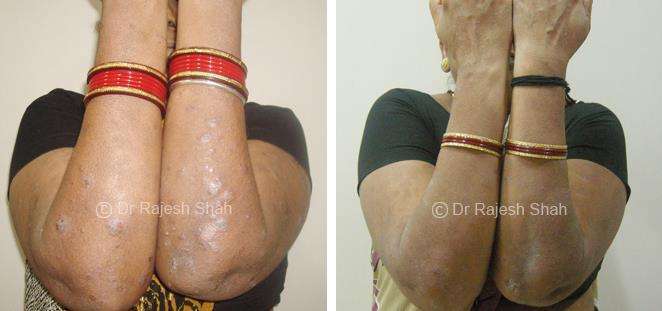
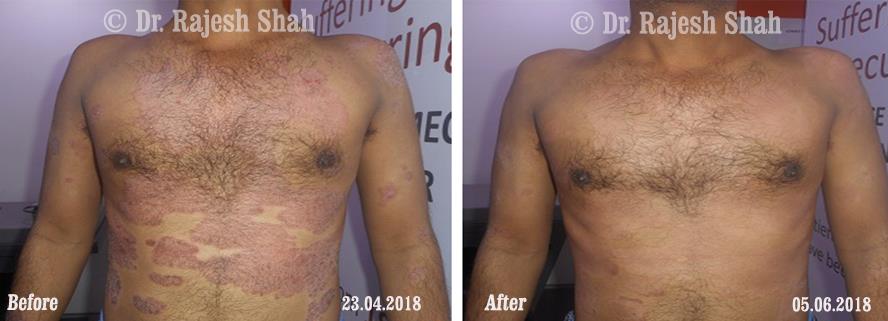
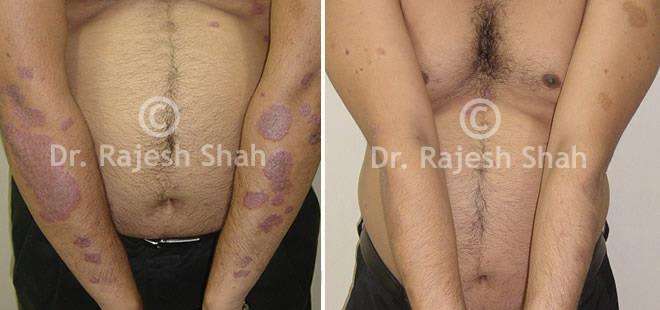
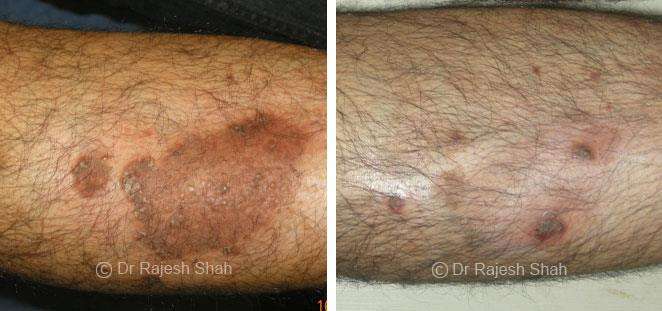
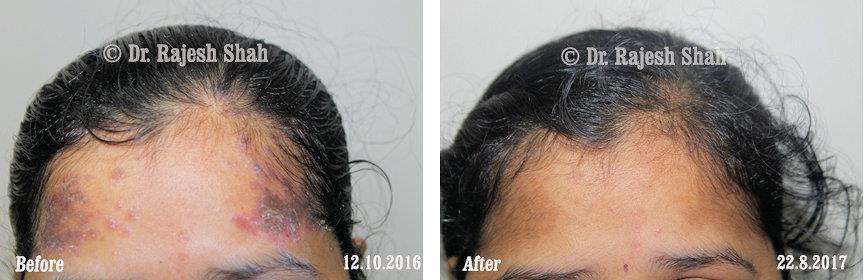
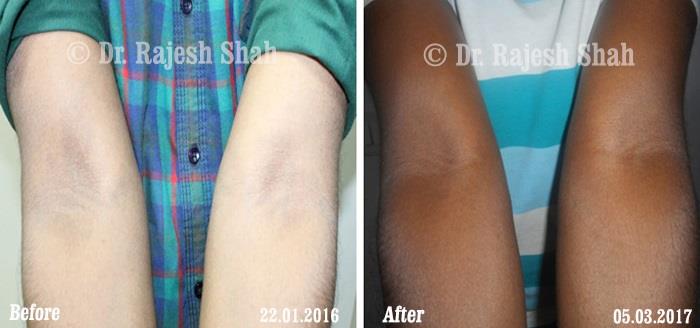
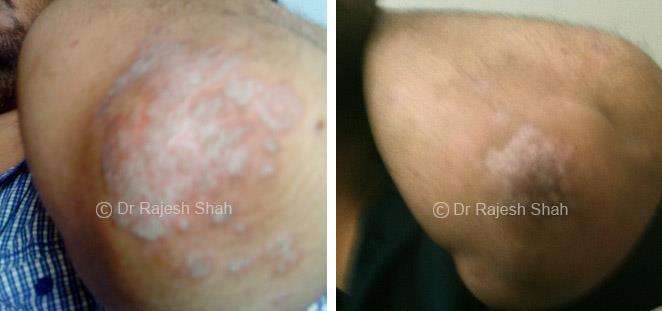
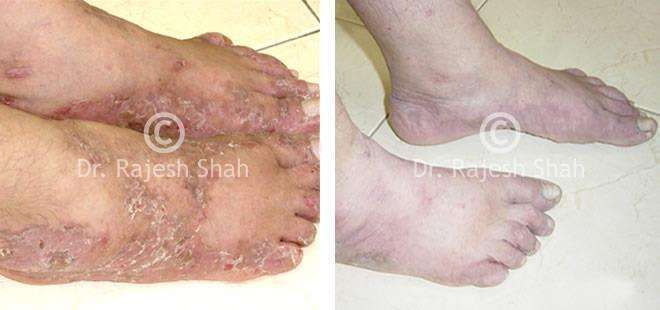
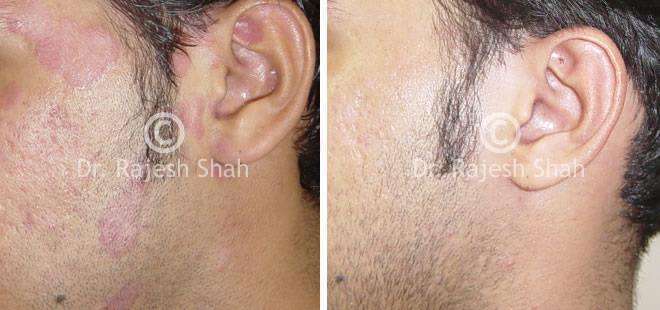
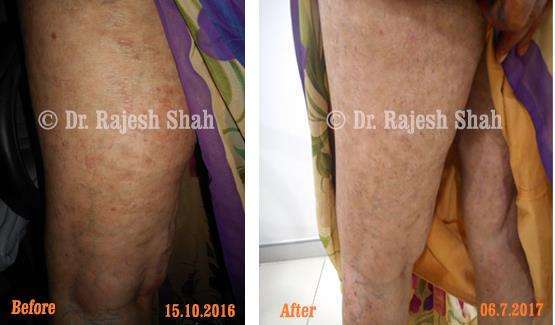
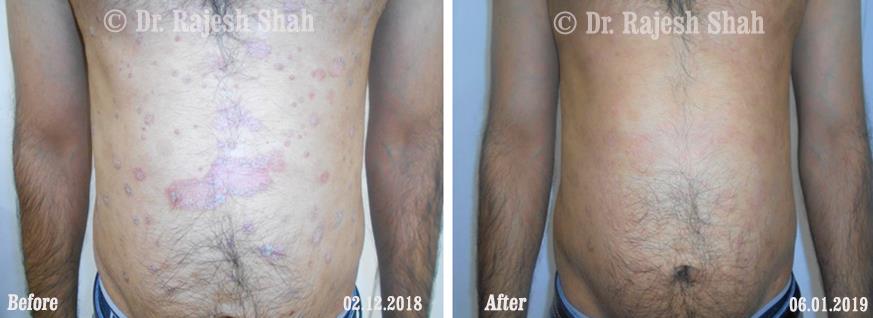
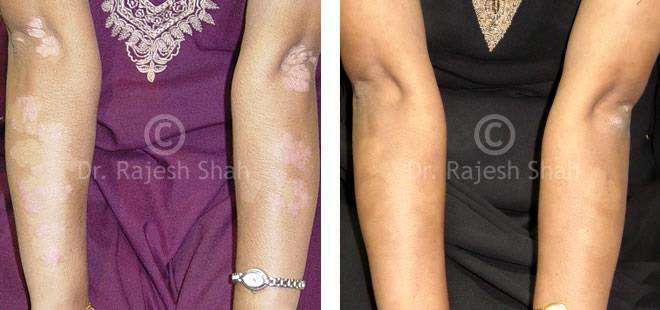
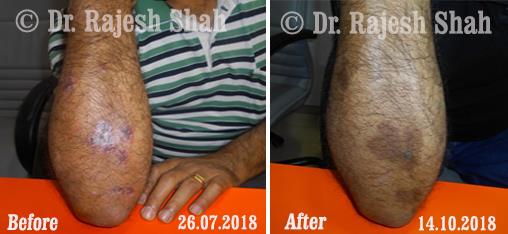
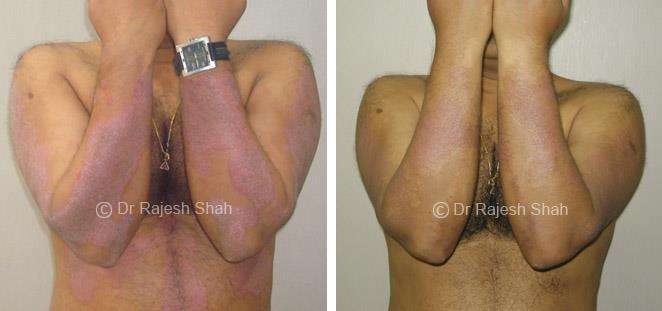
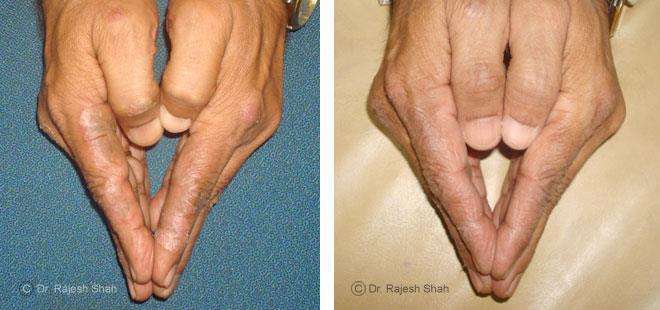
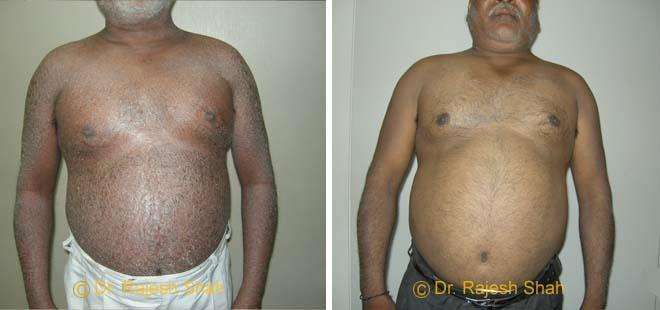
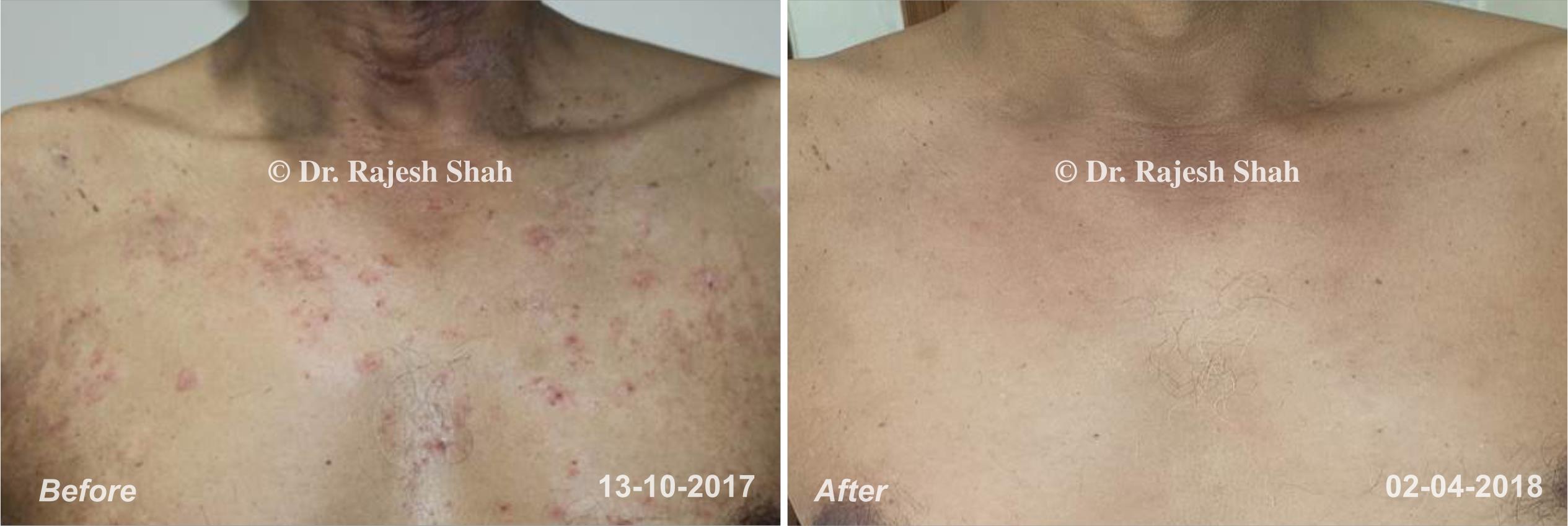
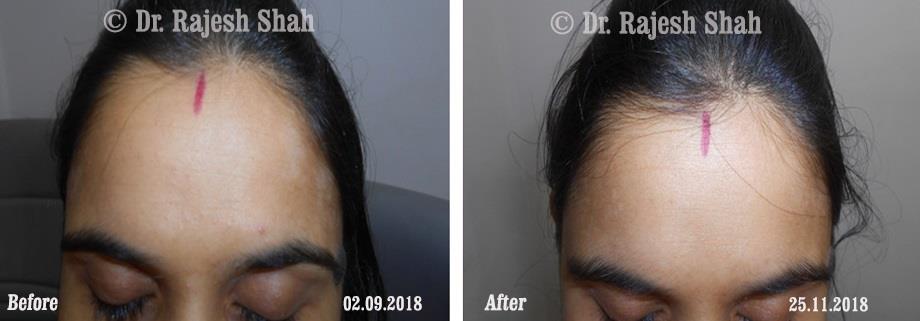
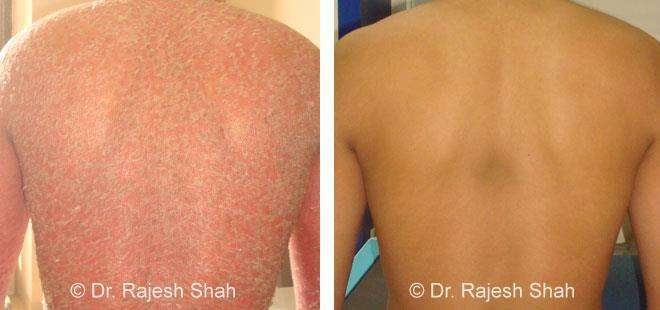
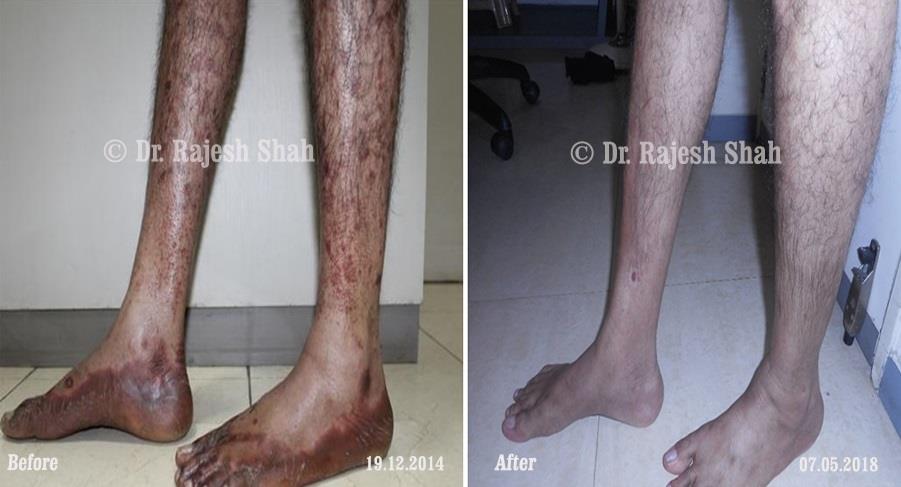
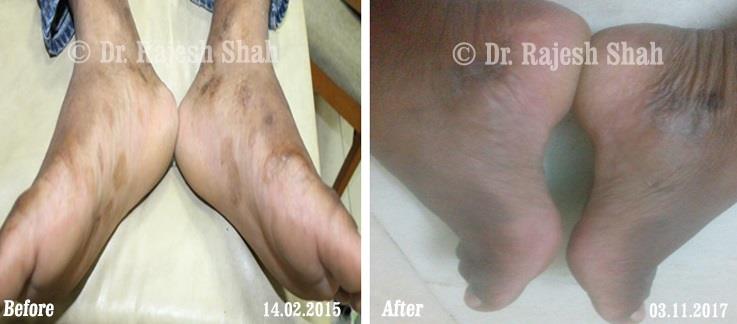
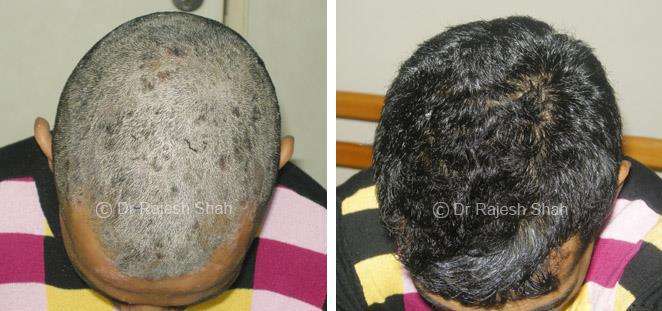
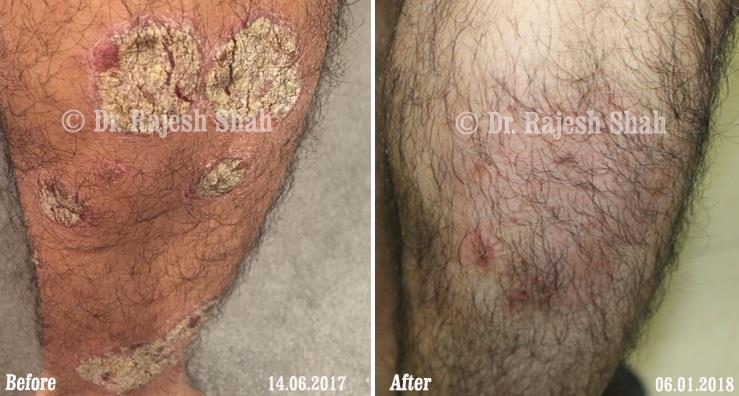
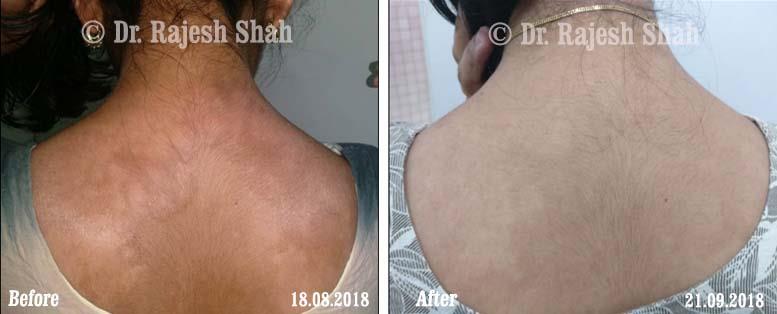
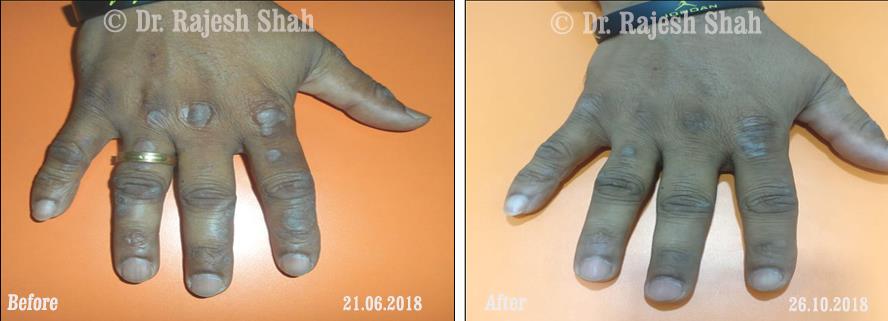
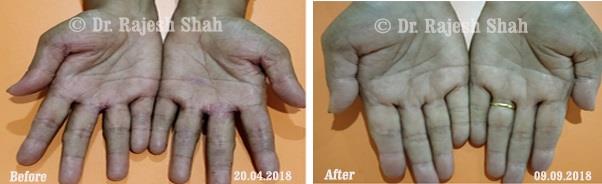
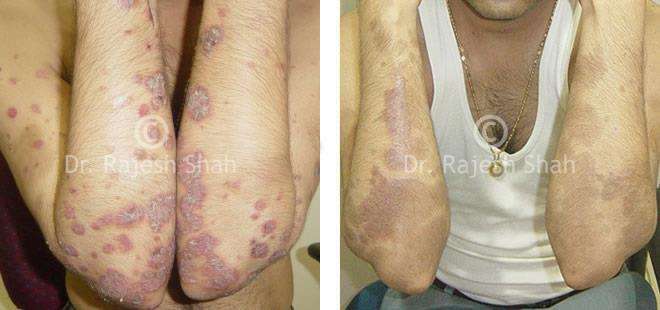
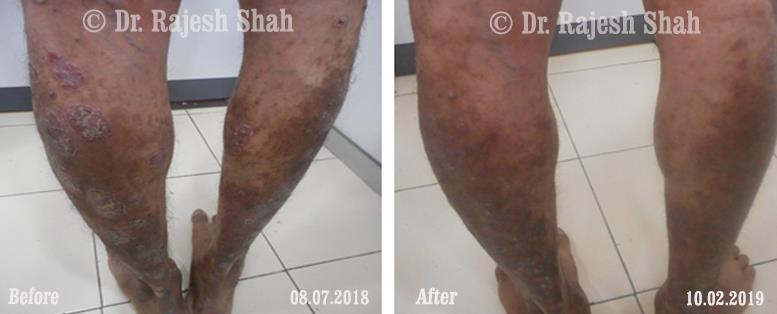
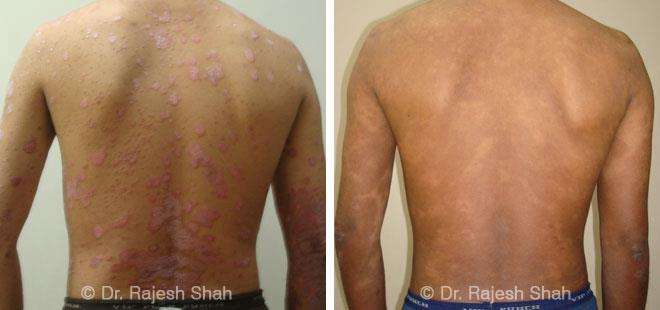
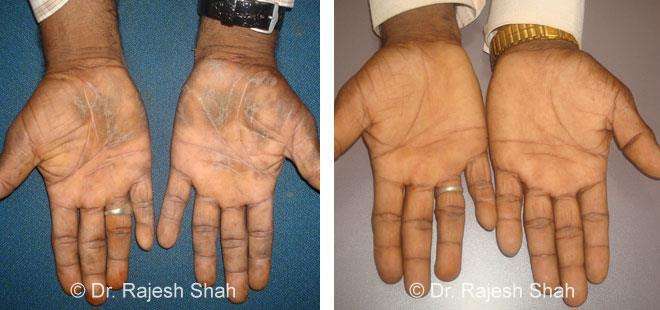
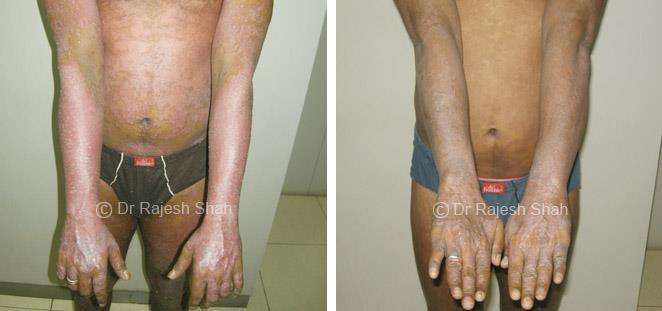
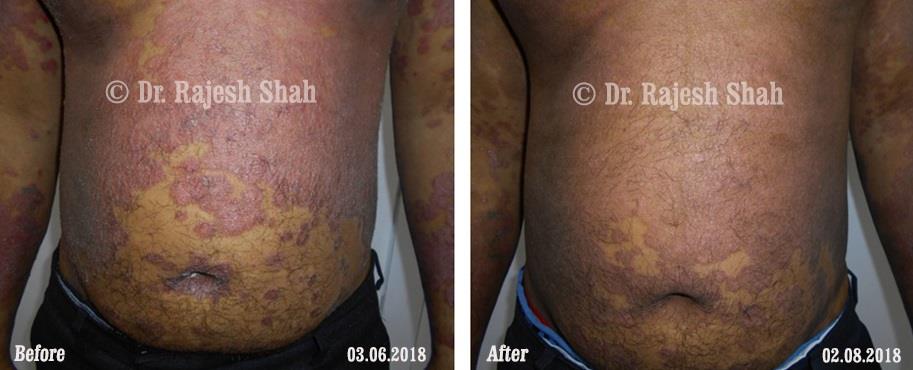
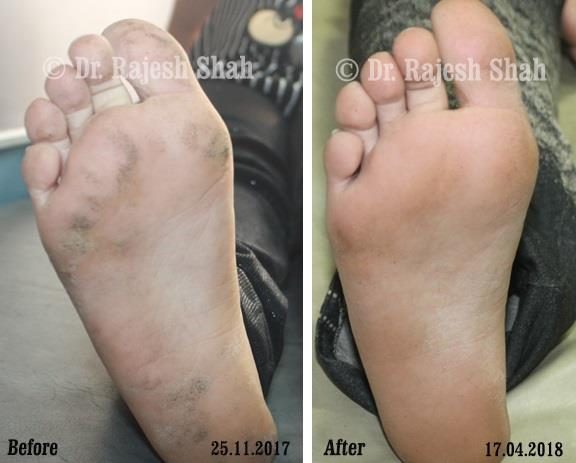
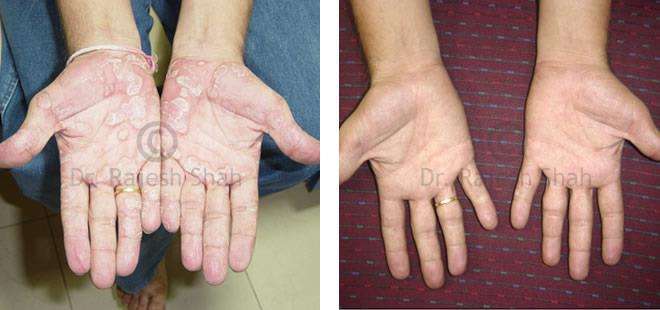
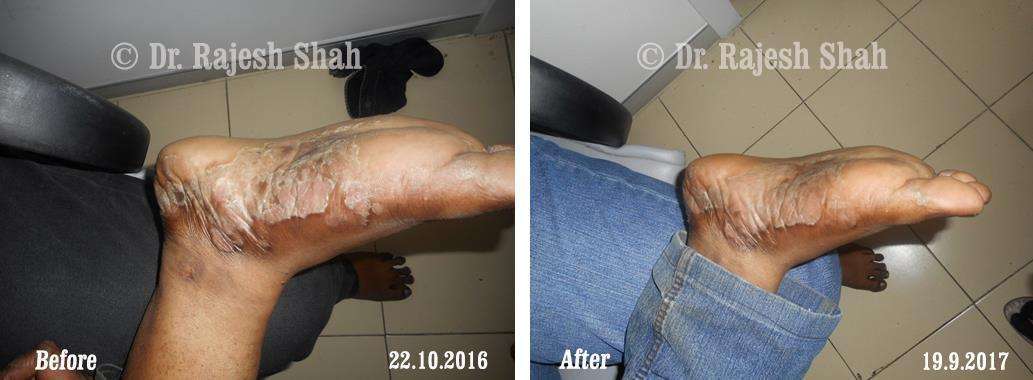
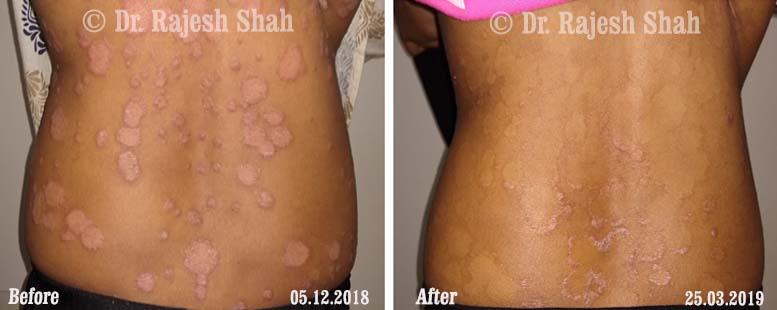
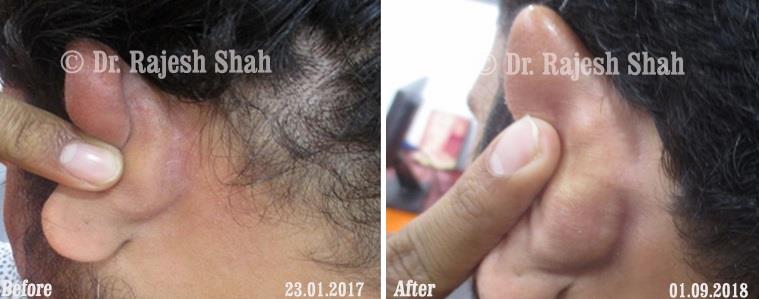
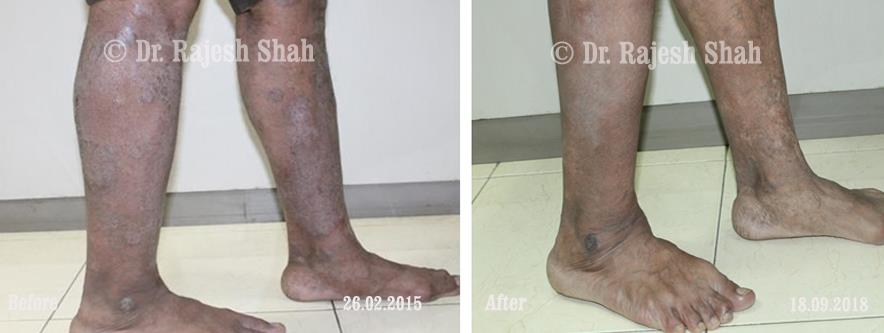
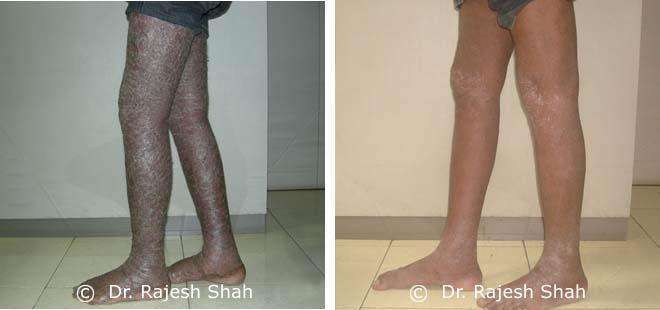
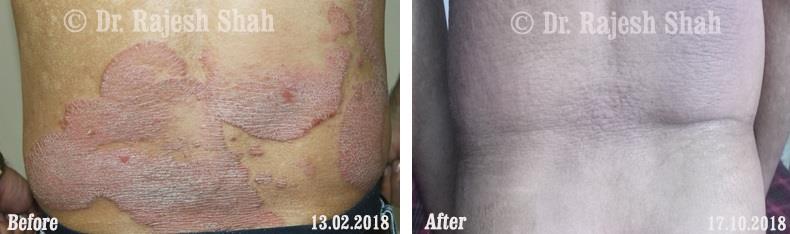
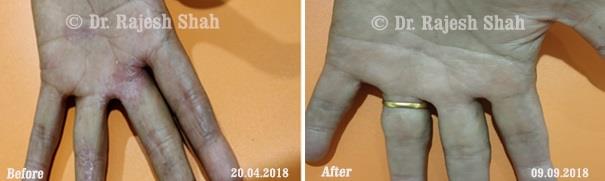
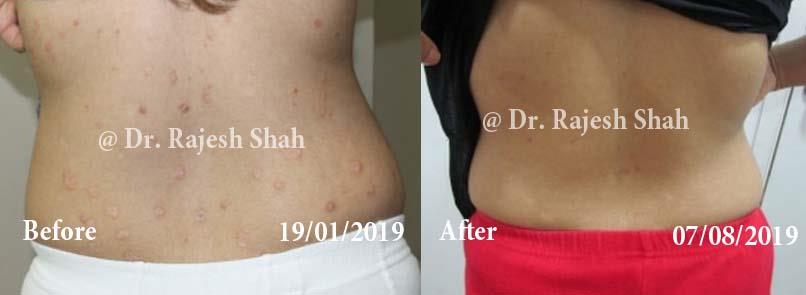
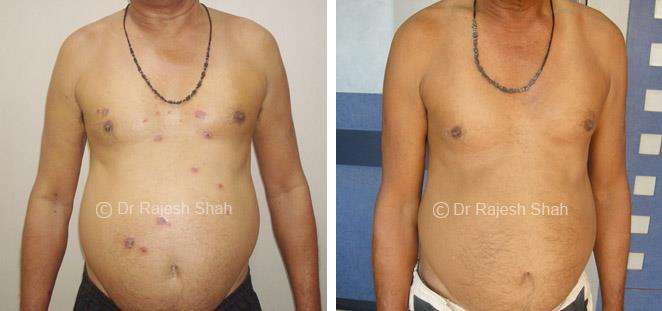
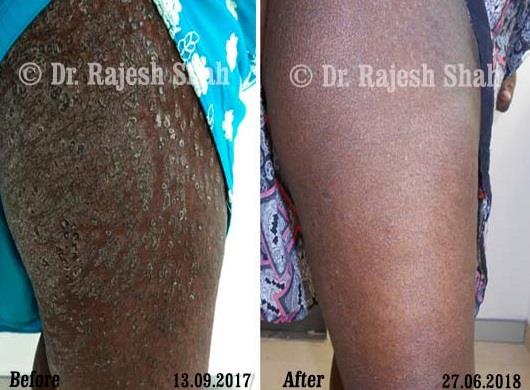
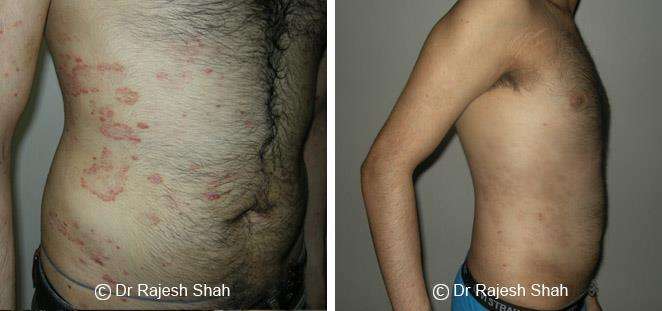
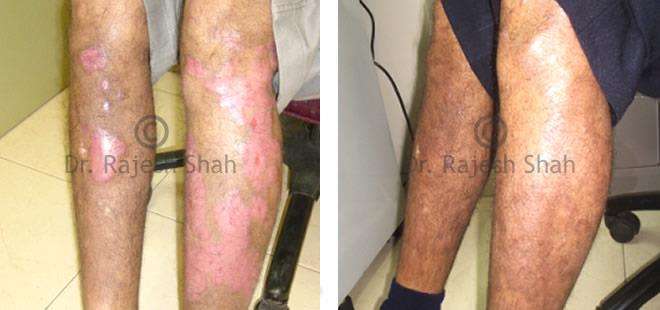
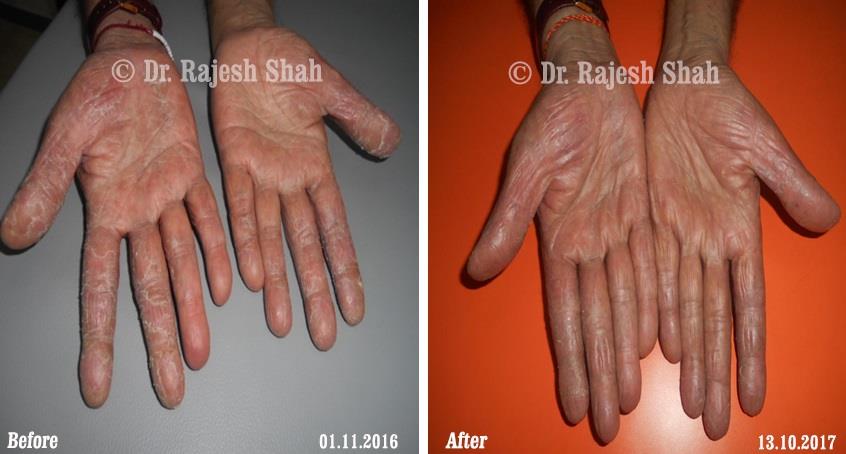
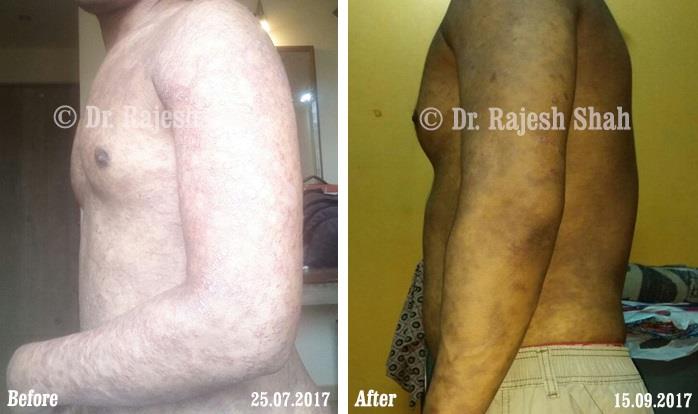
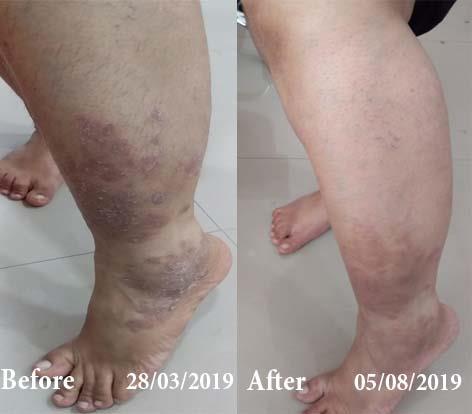
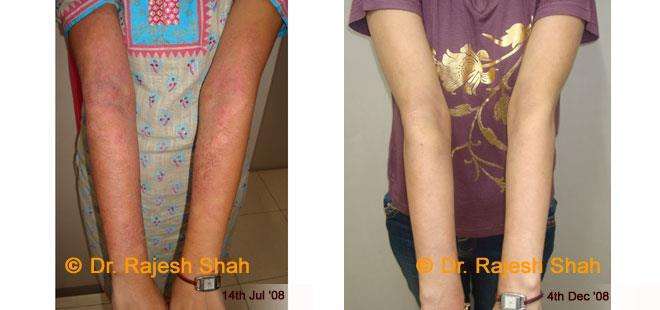
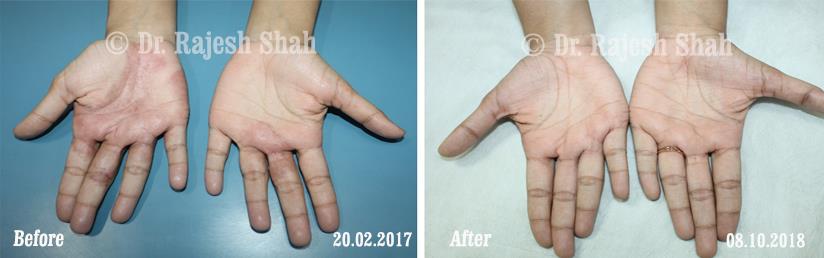
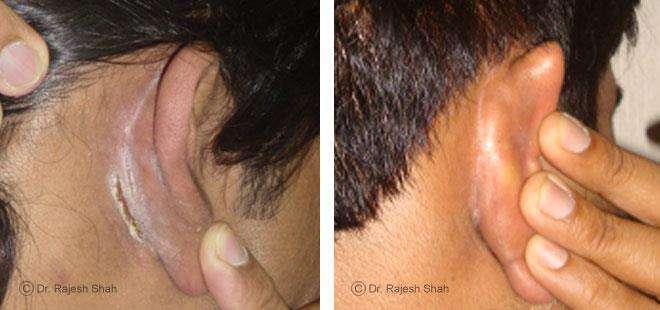
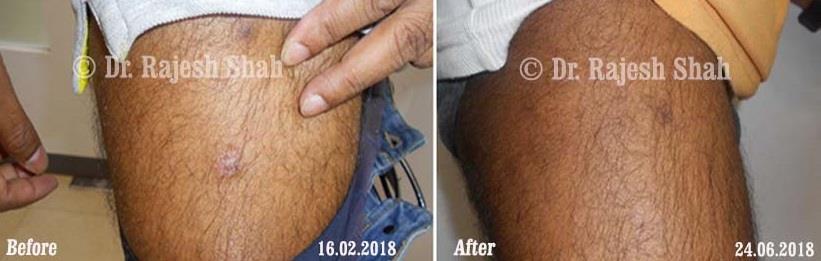
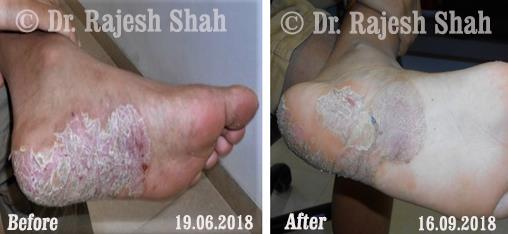
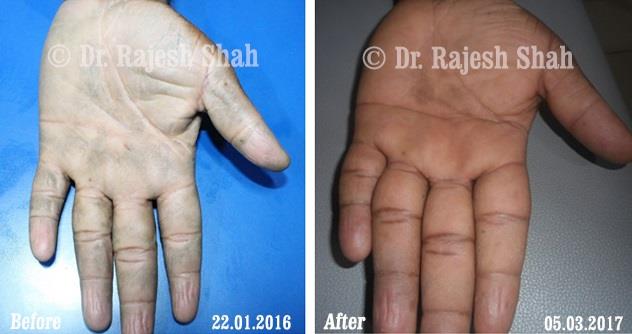
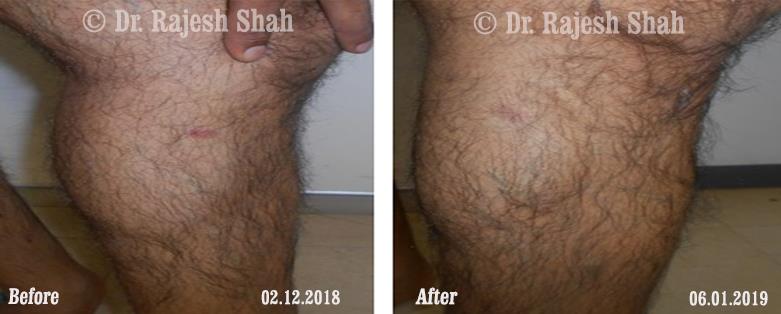
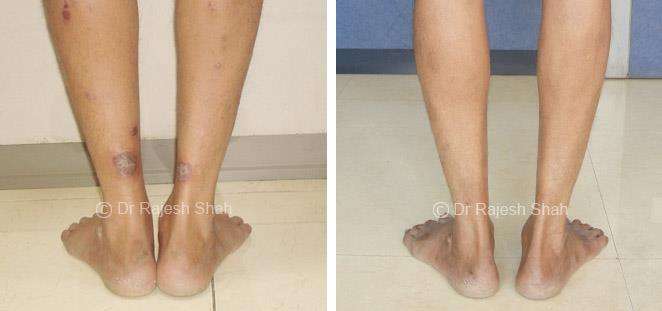
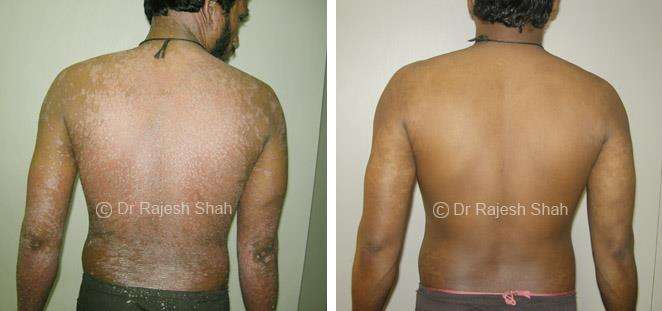
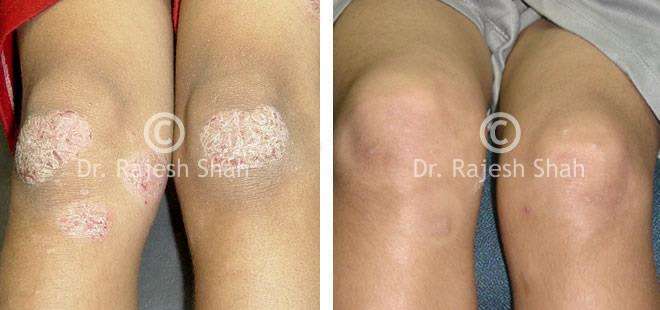
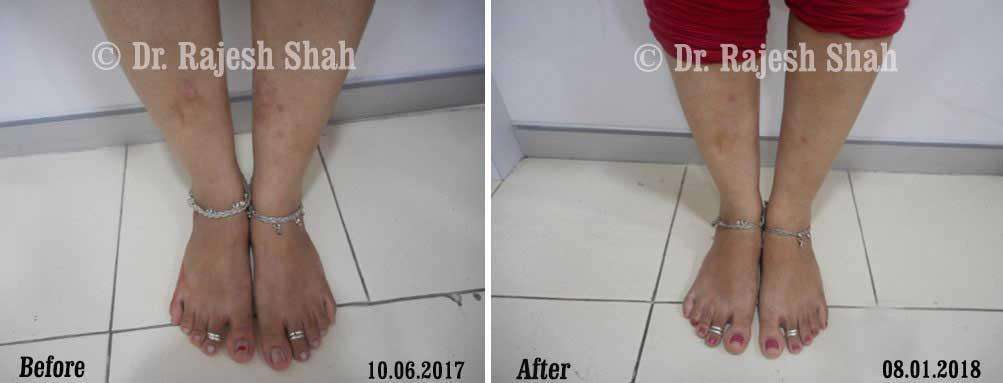
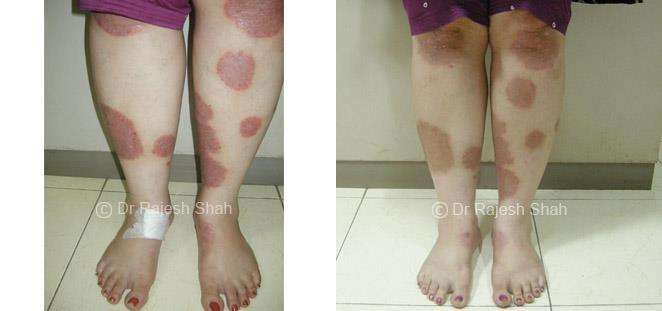
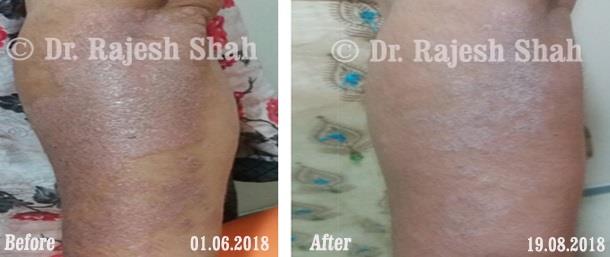
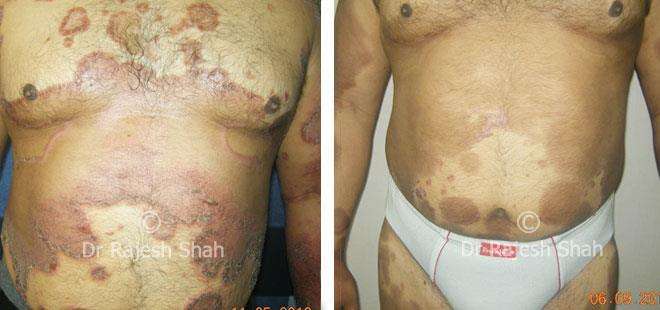
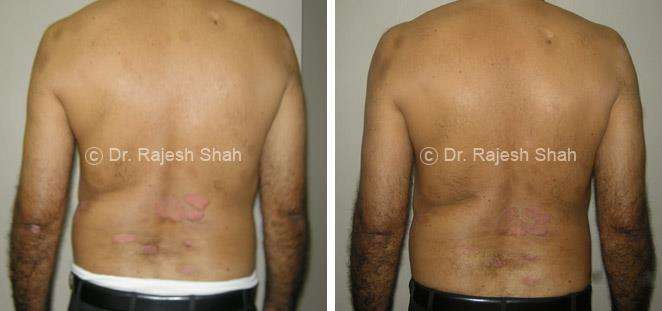
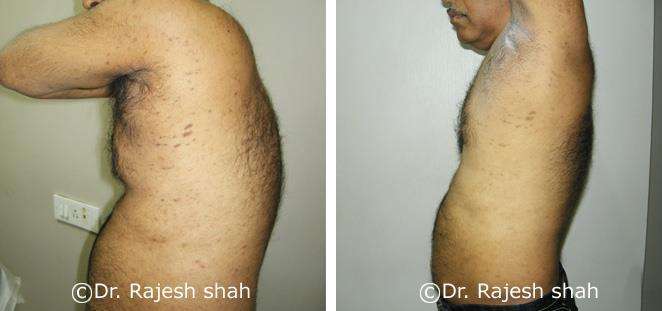
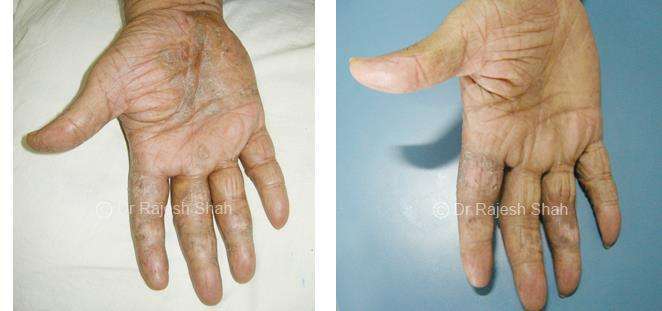
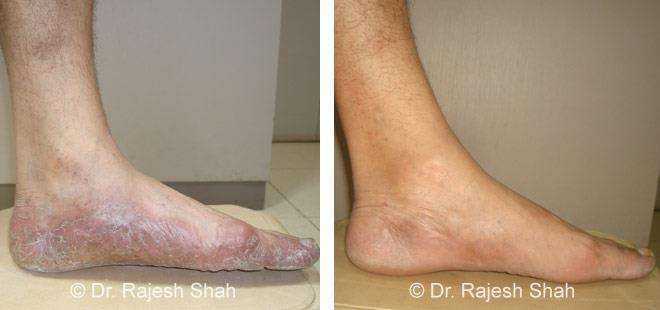
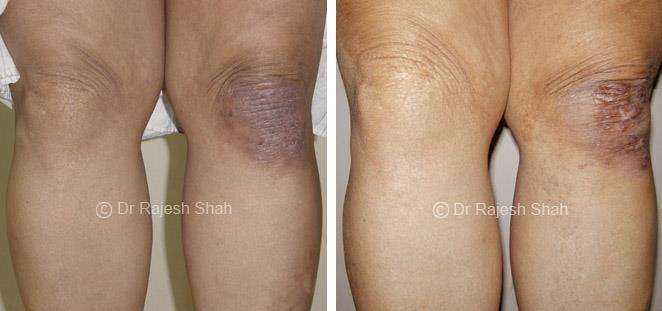
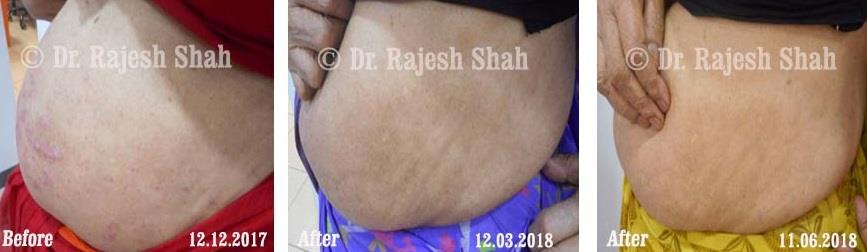
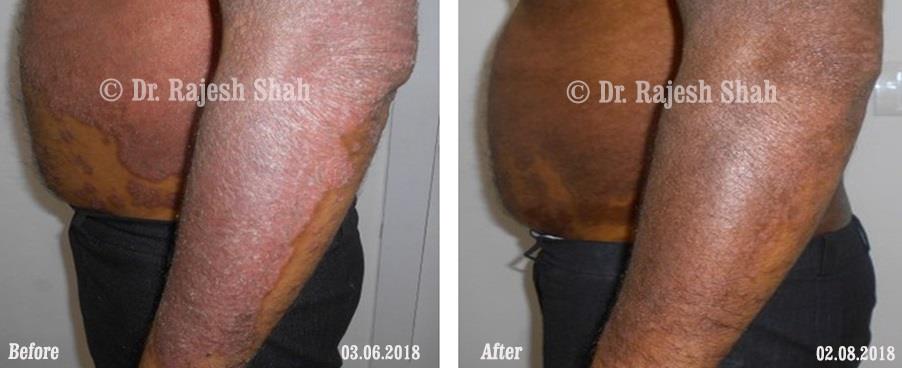
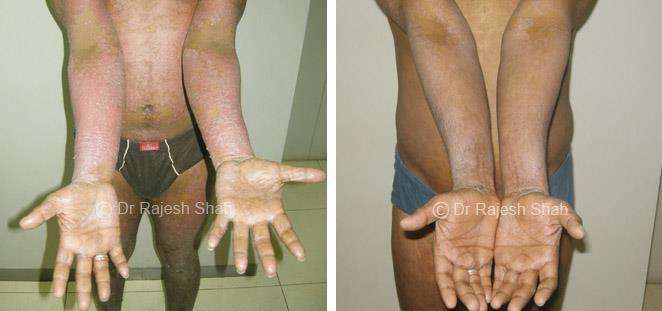
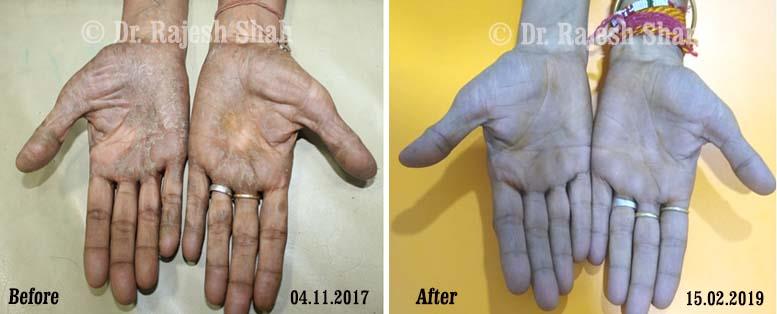
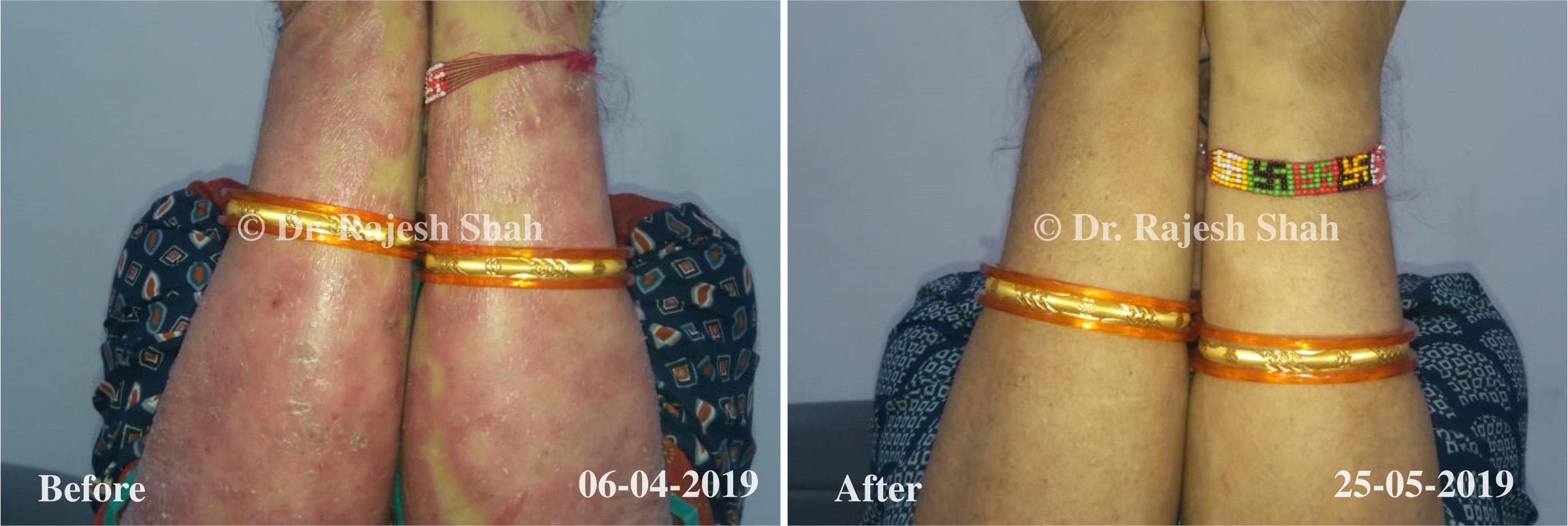
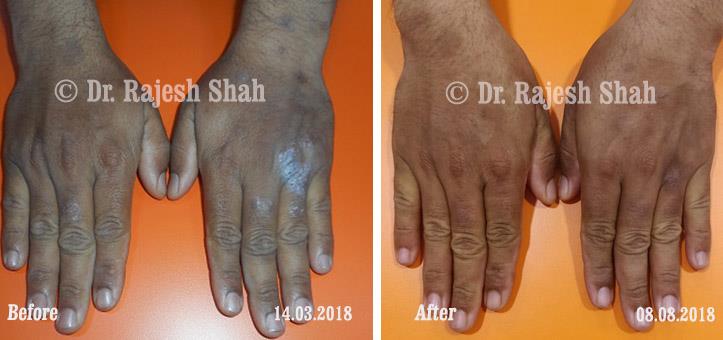
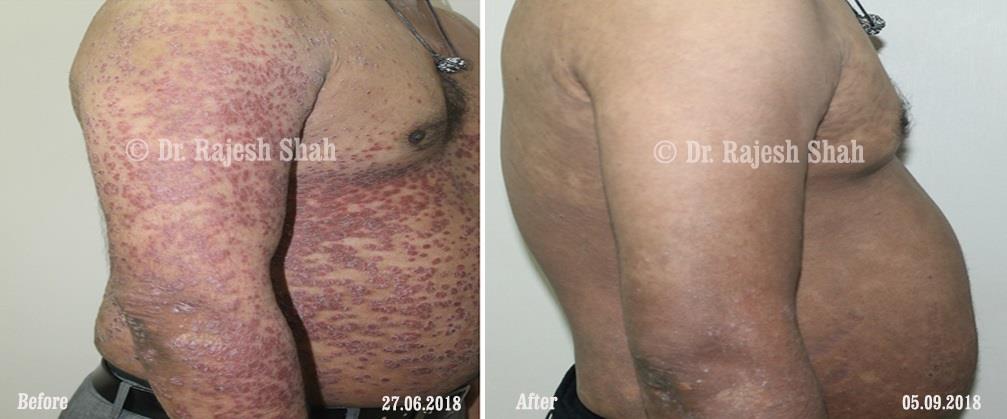
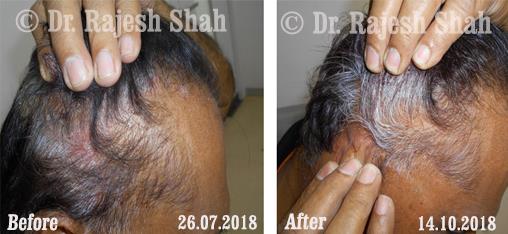
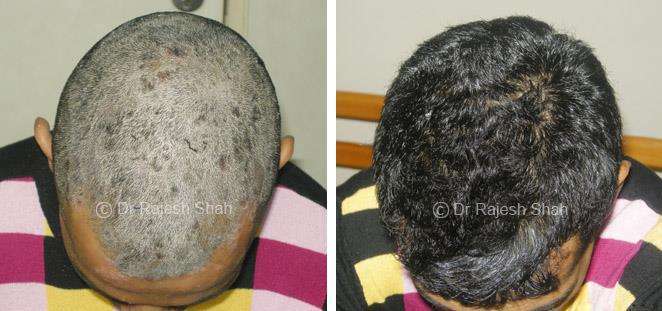
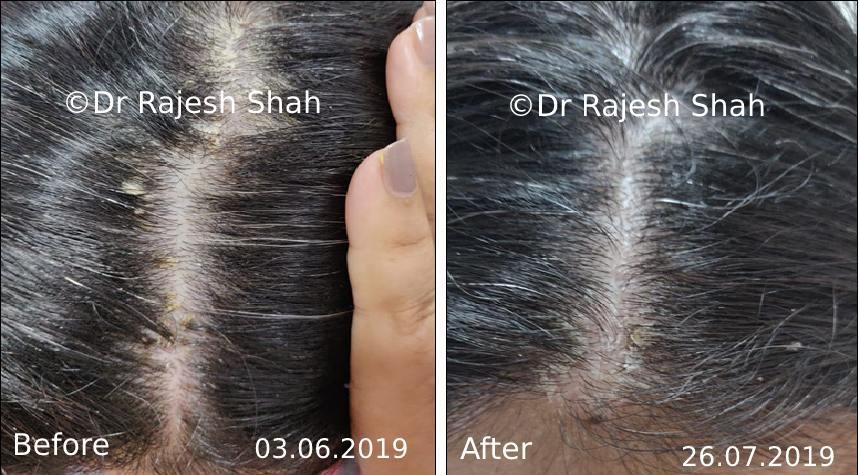
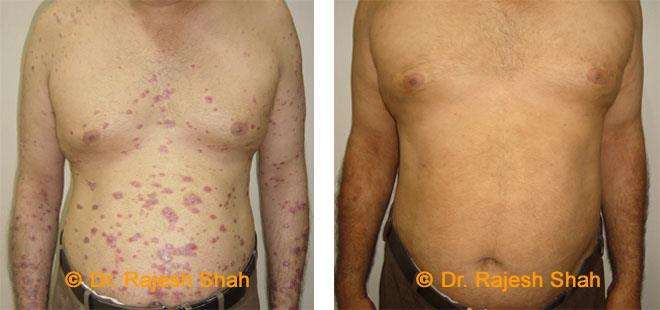
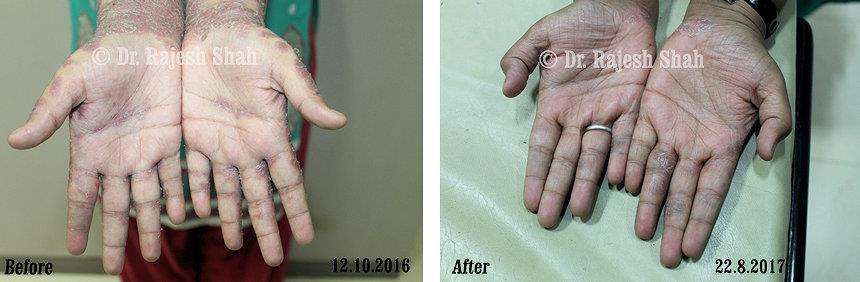
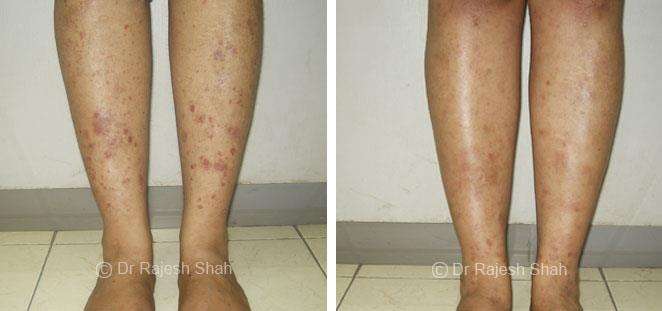
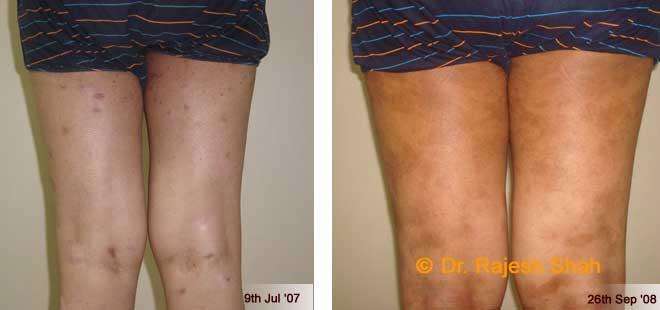
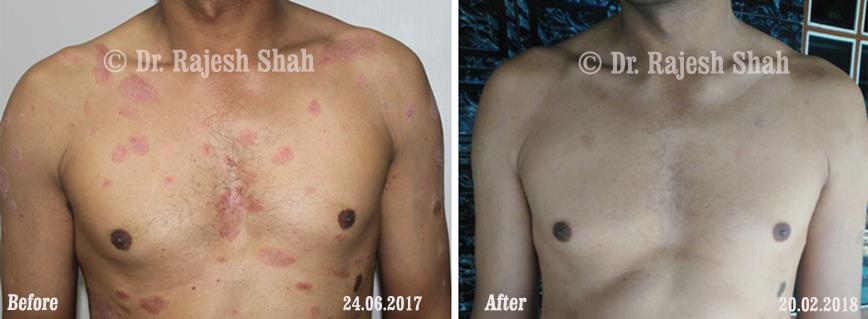
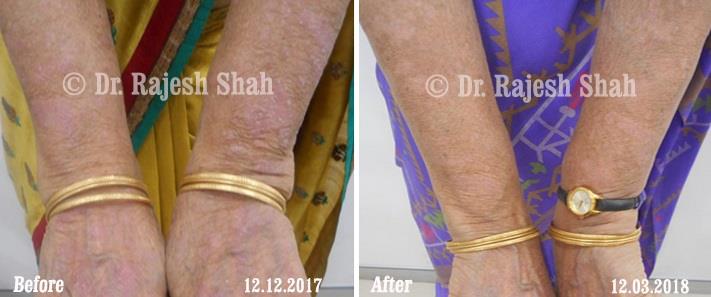
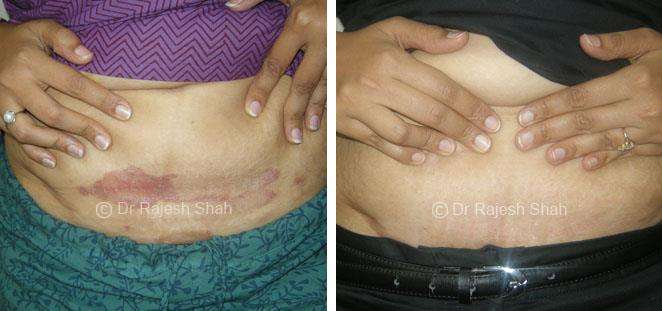
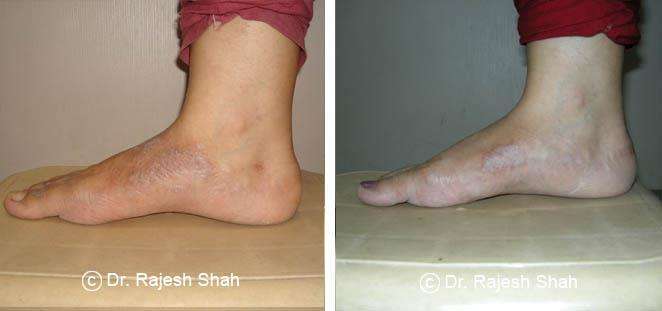
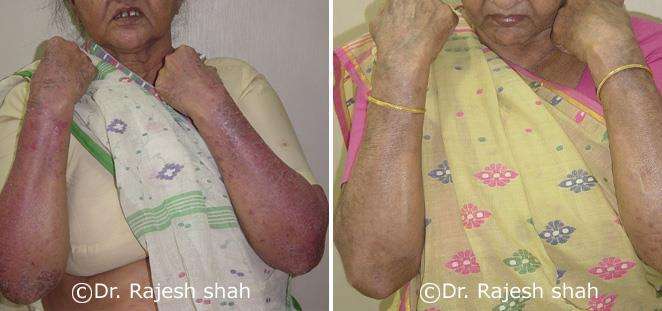
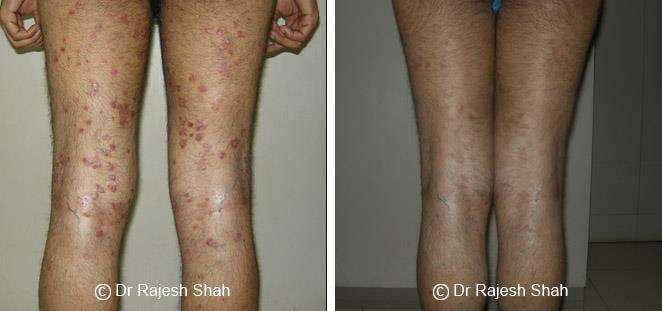
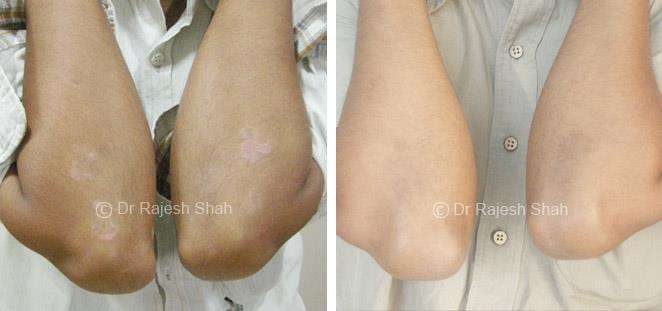
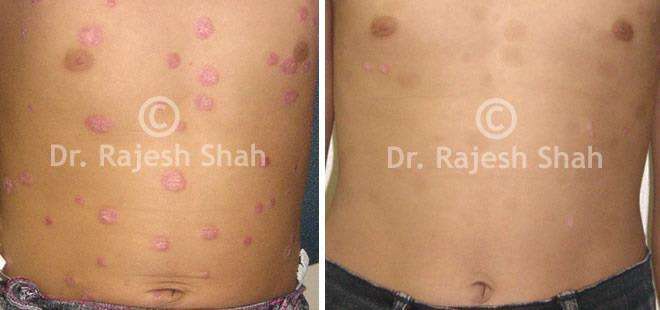
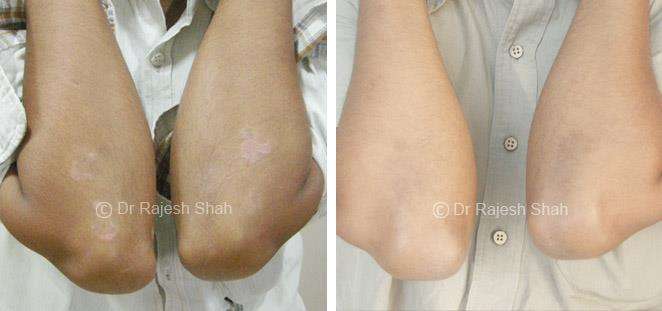
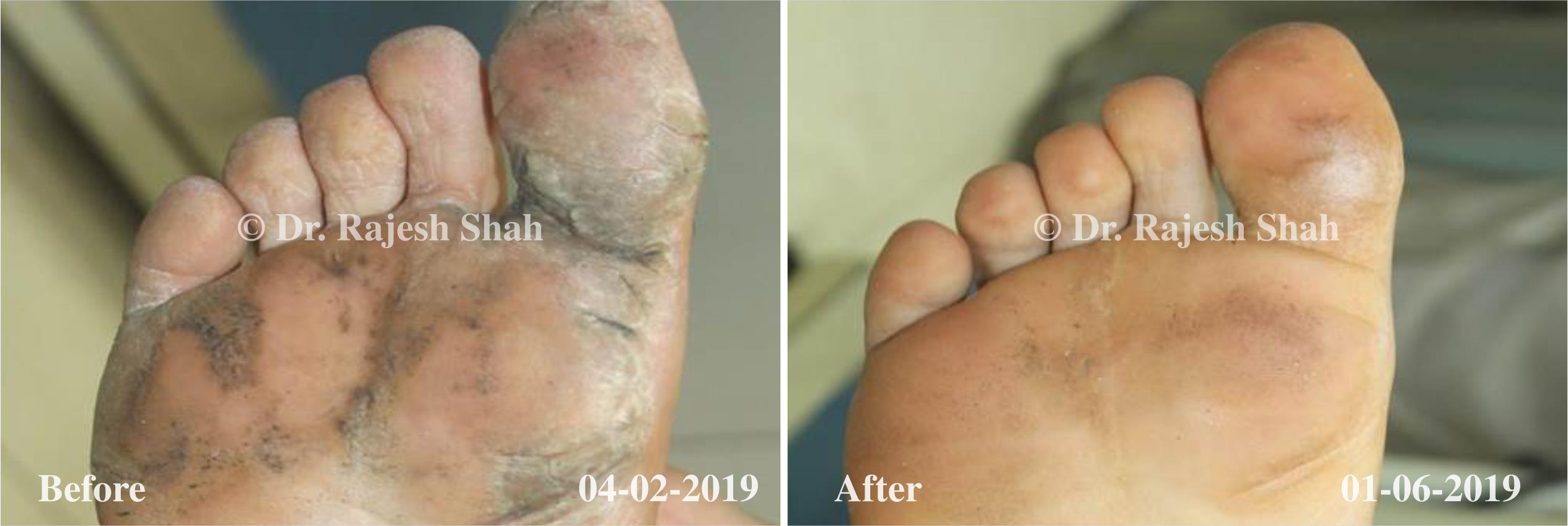
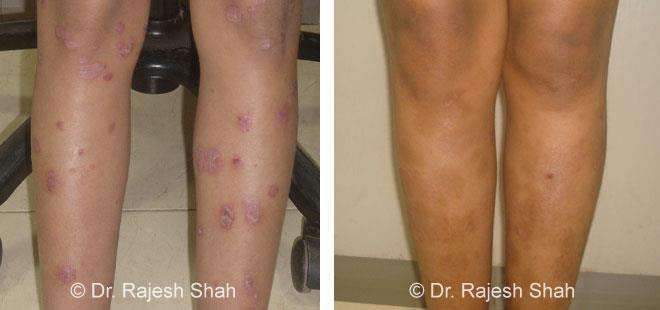
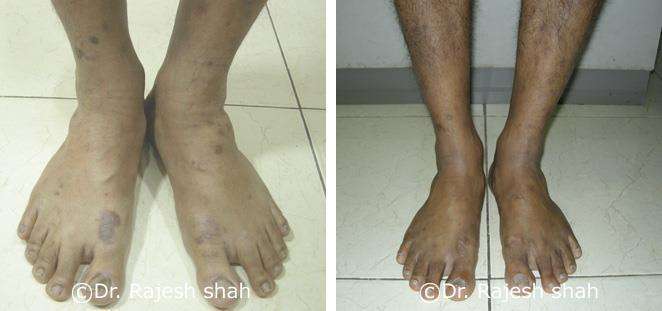
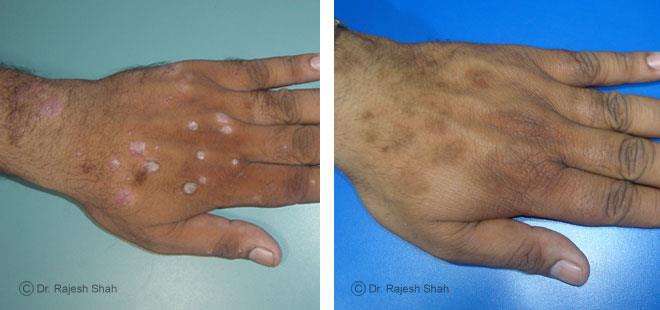
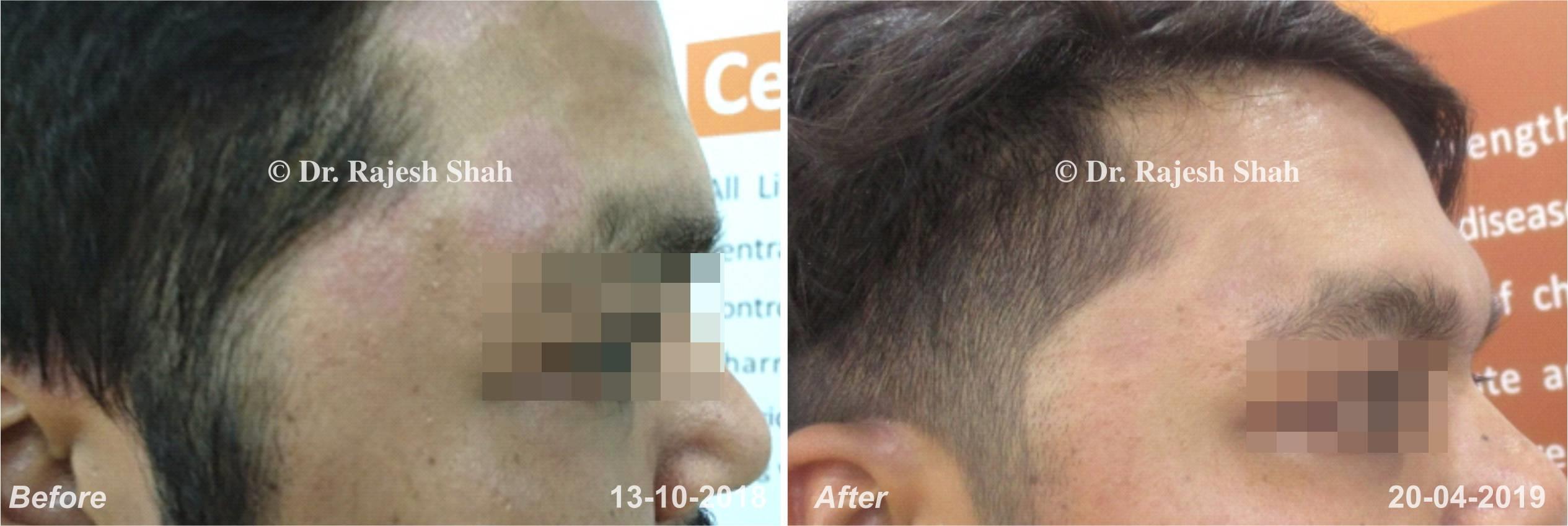
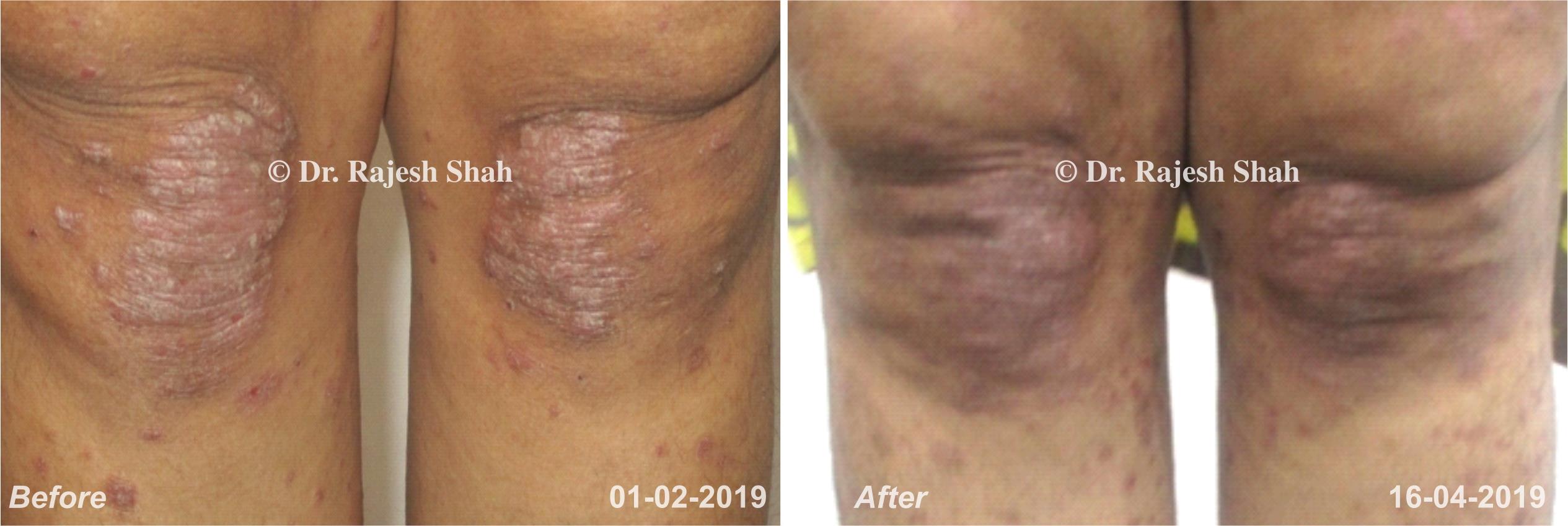
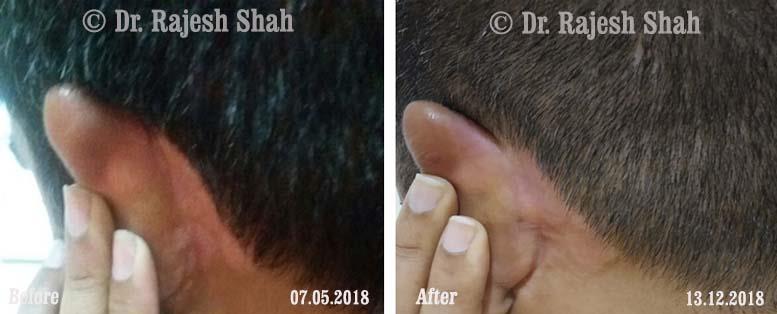
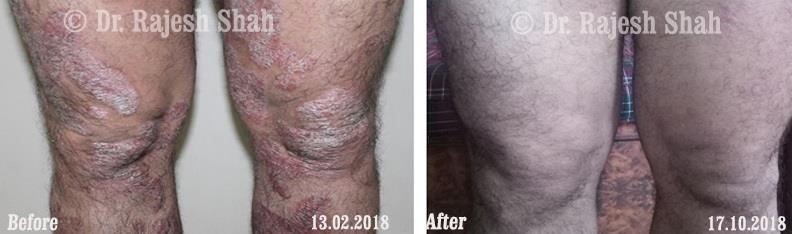
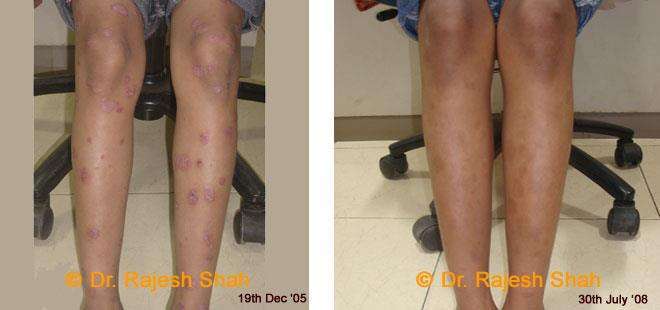
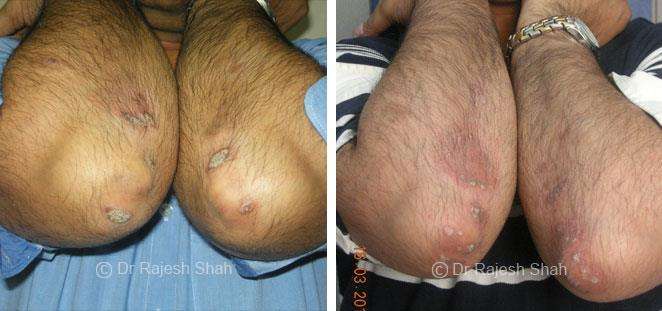
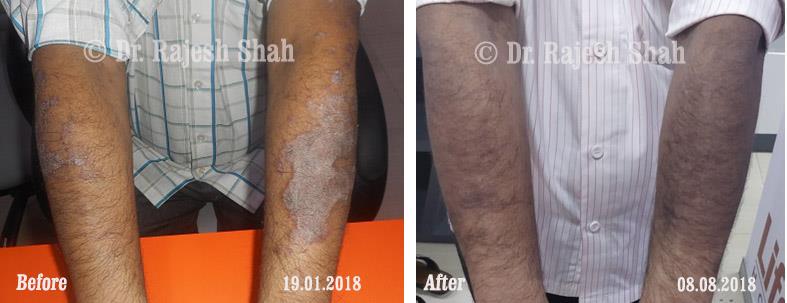
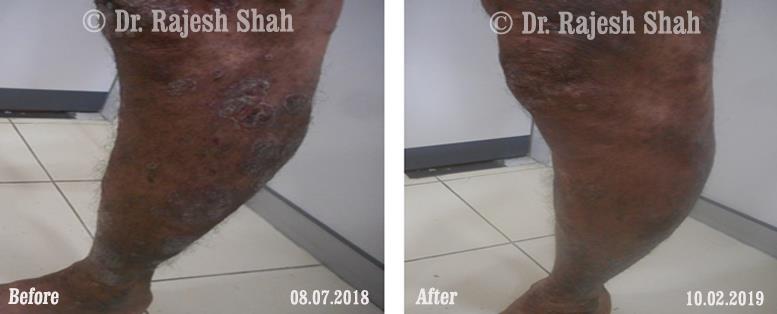
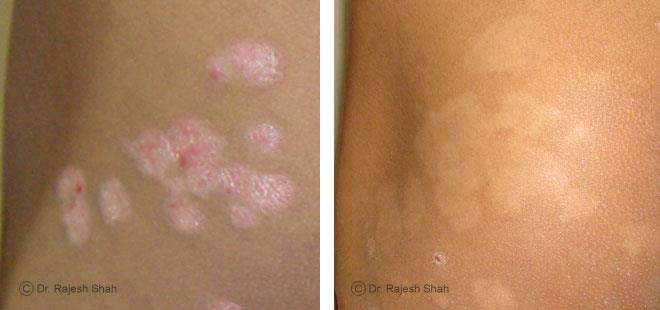
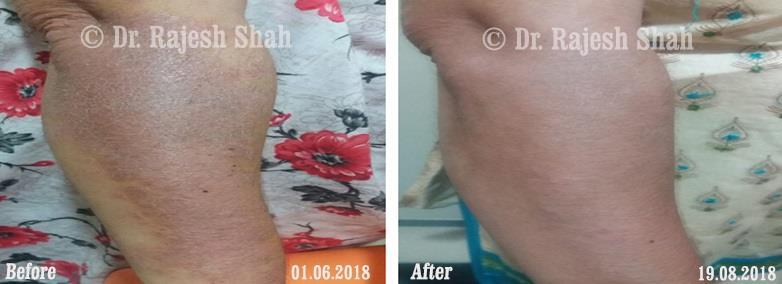
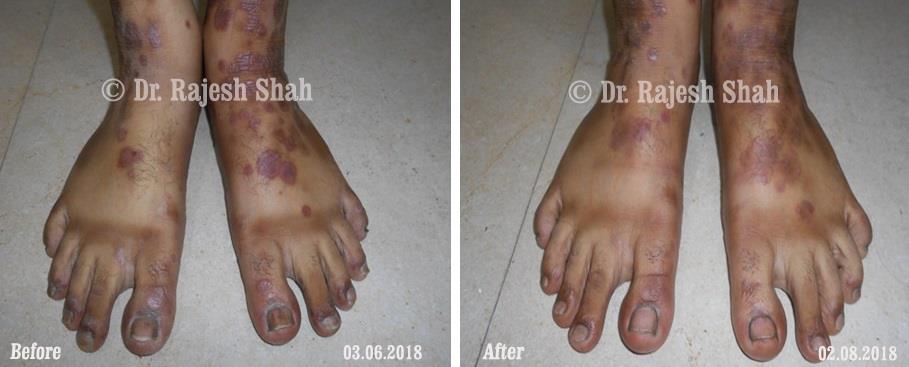
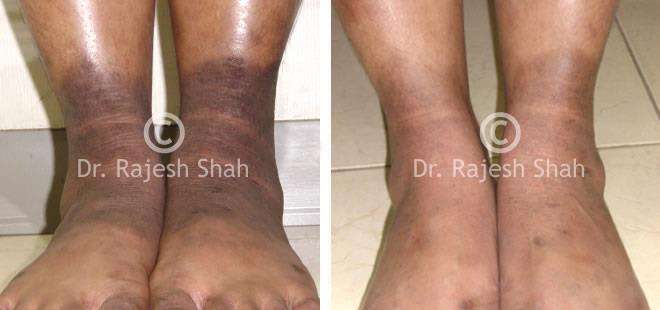
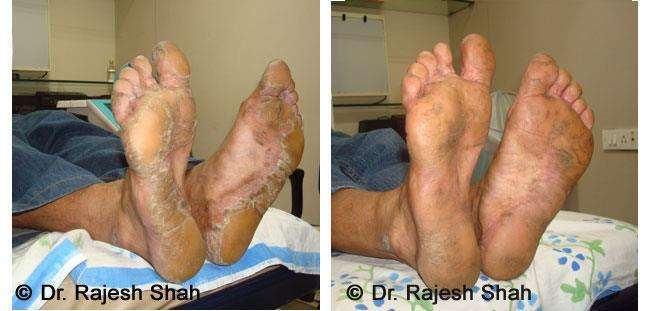
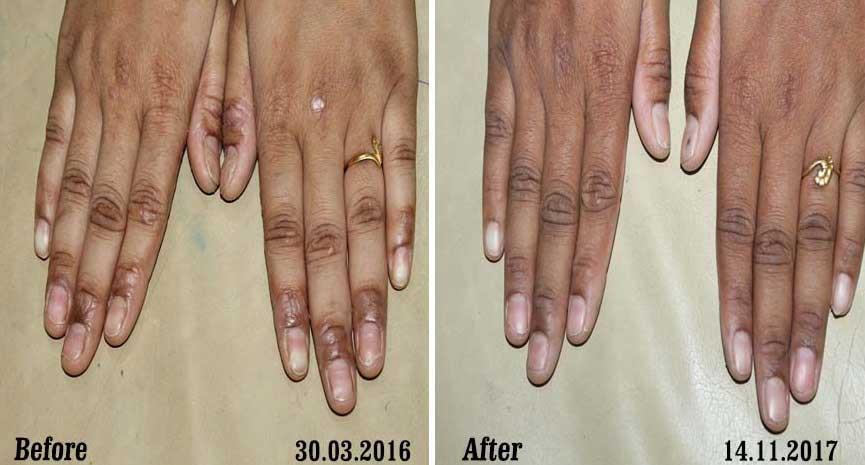
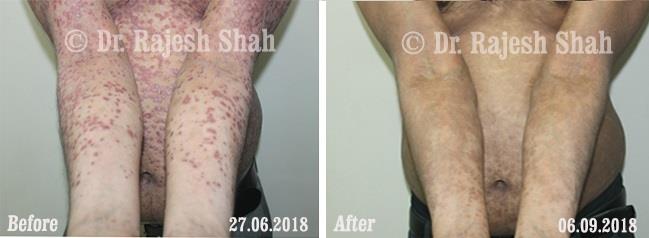
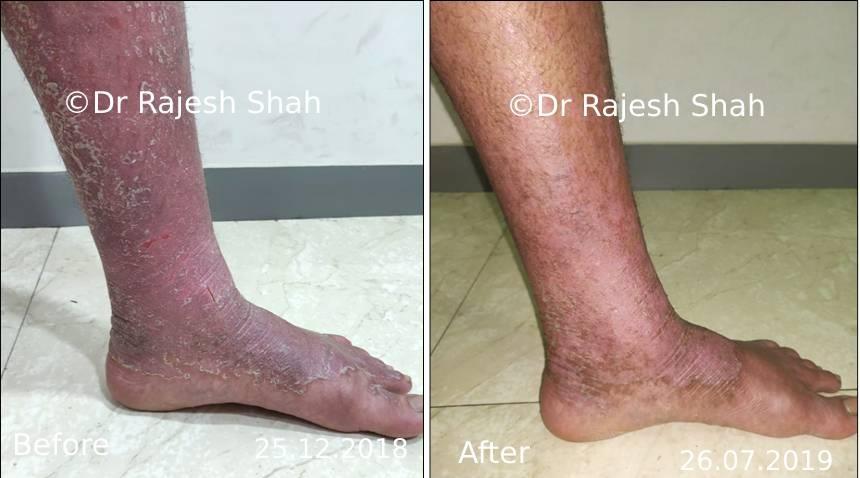
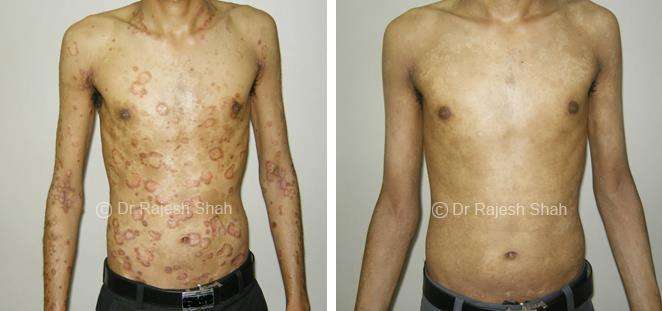
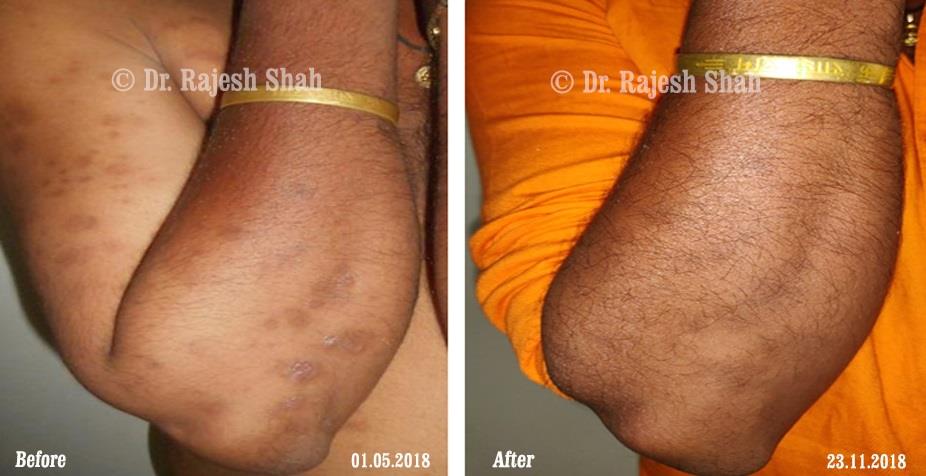
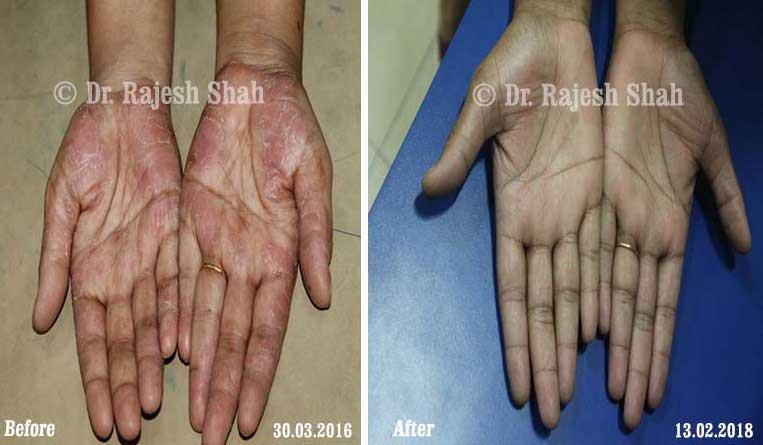
Dr. Rajesh Shah's Insights on Psoriasis
Dr. Rajesh Shah’s experience, psoriasis is not just a skin disorder but a deep-rooted autoimmune condition influenced by genetics, immune imbalance, stress, and environmental triggers. As a Homeopathic Psoriasis Specialist, he emphasizes individualized evaluation to ensure each patient feels understood and confident in their treatment plan. At Life Force Homeopathy, the approach to psoriasis focuses on understanding each patient’s unique disease pattern and on offering personalized care using homeopathic medicines for psoriasis, selected according to constitutional principles.
This approach aims to help control relapses, relieve symptoms, and support safe, long-term remission. After managing over 8,000 cases worldwide, it is evident that while psoriasis may not be completely curable, it is clearly manageable with the right long-term approach, encouraging a sense of hope and empowerment for patients seeking effective management options.
Long-term clinical experience also suggests that immunosuppressants like corticosteroids and methotrexate often fail to provide sustained relief, as psoriasis frequently flares after stopping these medications. Homeopathy can therefore be considered a supportive, long-term approach in the comprehensive management of psoriasis, helping to reduce dependency on conventional drugs.
180+
Countries
10000+
Psoriasis Patients Treated
30+
Team of Expert Doctors
40+
Years of Experience
100% Satisfaction
If you are not satisfied after 6 weeks of treatment, you may return any unused medicines for a refund, in accordance with our policy. Refunds are processed only when the parcel is returned within the stipulated time, with applicable administrative or shipping deductions. For full terms, please visit our Detailed Refund Policy page.
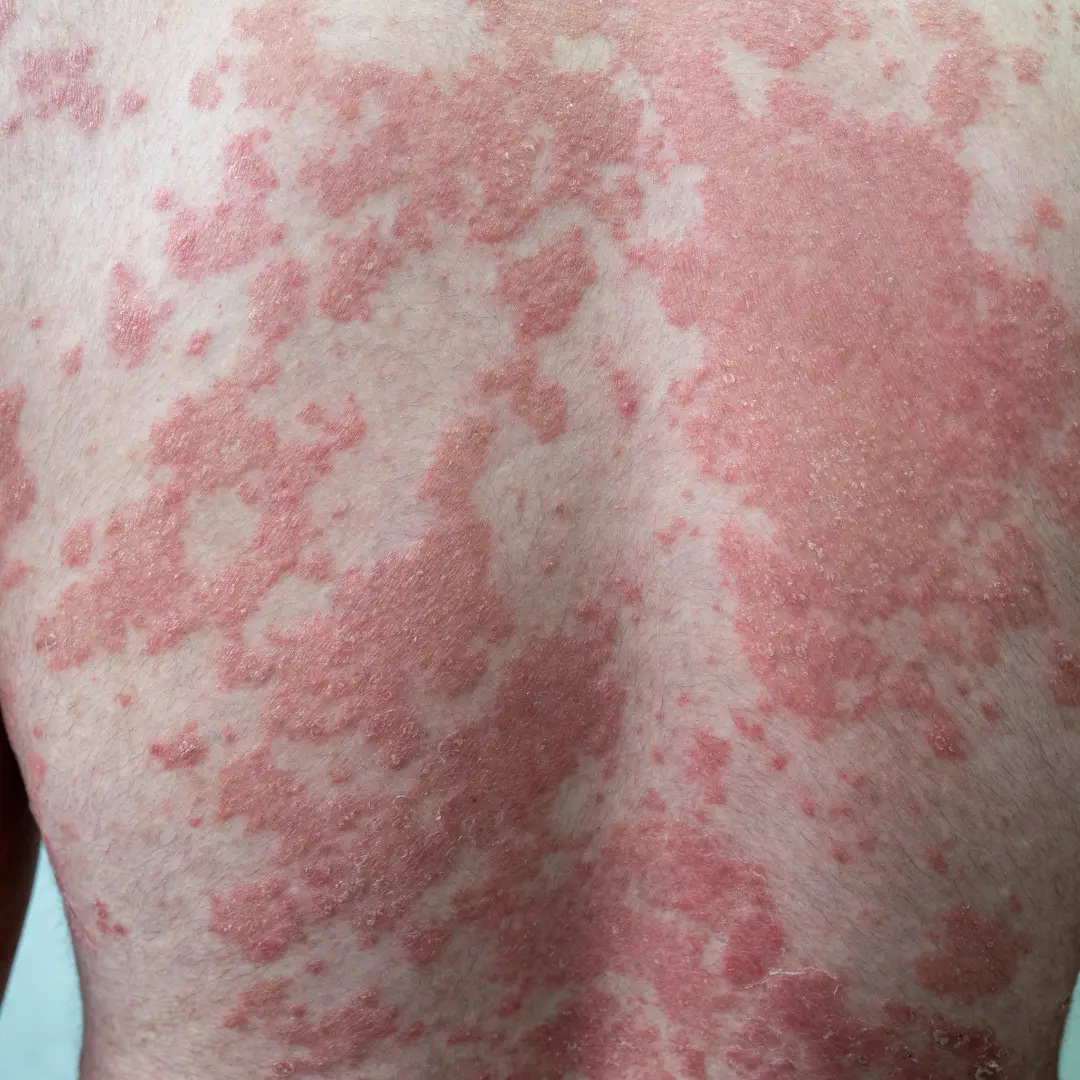
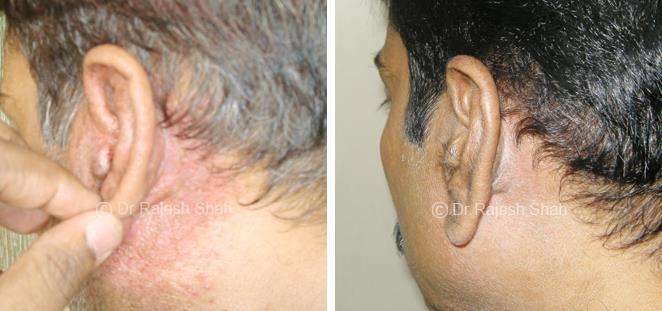
What is Psoriasis?
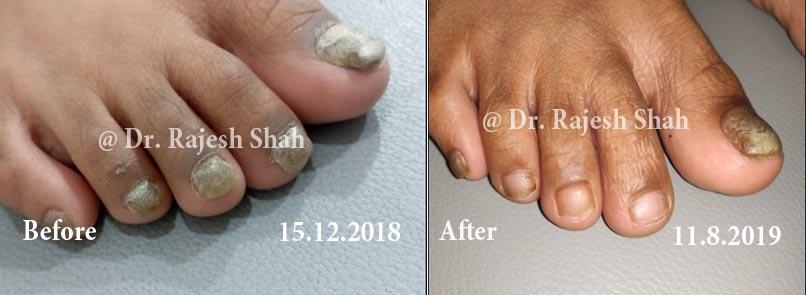
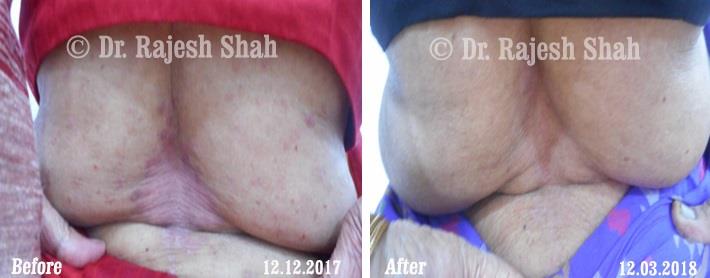
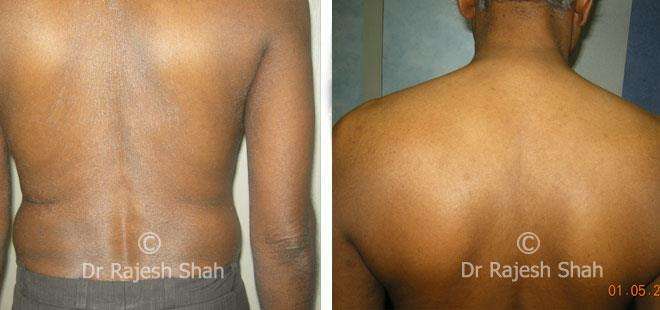
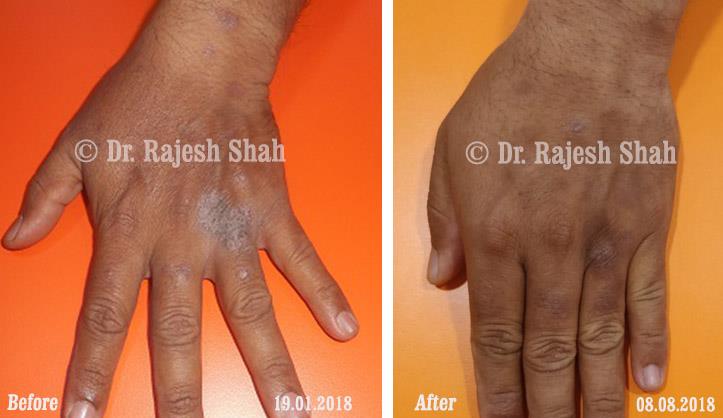
Psoriasis is a long-standing autoimmune condition in which the immune system becomes overactive, accelerating the growth cycle of skin cells. Instead of shedding normally, new cells rise to the surface too quickly, forming inflamed, scaly plaques. These patches commonly appear on the scalp, elbows, knees, and lower back, and on the nails.
Psoriasis is not contagious and varies widely in severity. While it is a chronic disorder, many individuals manage it effectively through timely care, lifestyle measures, and Psoriasis treatment in homeopathy that addresses immune regulation rather than only external symptoms.
-
Alopecia Areata
-
Ankylosing Spondylitis
-
Asthma
-
Cancer
-
Child Asthma
-
Eczema
-
Frequent Colds
-
Hair Fall
-
Hepatitis C
-
Irritable Bowel Syndrome (IBS)
-
Lichen Planus
-
Psoriasis
-
Trigeminal Neuralgia
-
Ulcerative Colitis
-
Underactive Thyroid
-
Urticaria
-
Vitiligo
Find out your chances of recovery, now
Select the disease from the list

STEP 01
Select your condition

STEP 02
Submit the Form

STEP 03
Get report Instantly
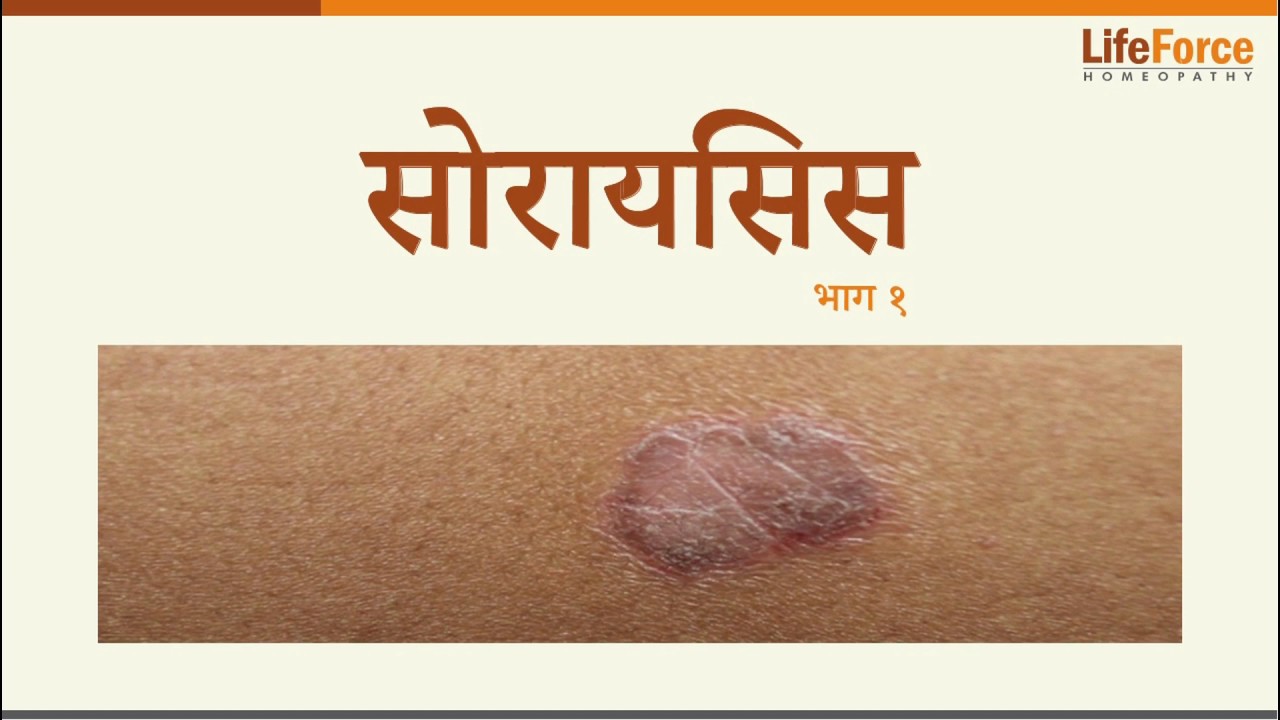
Understanding Psoriasis
Types of Psoriasis
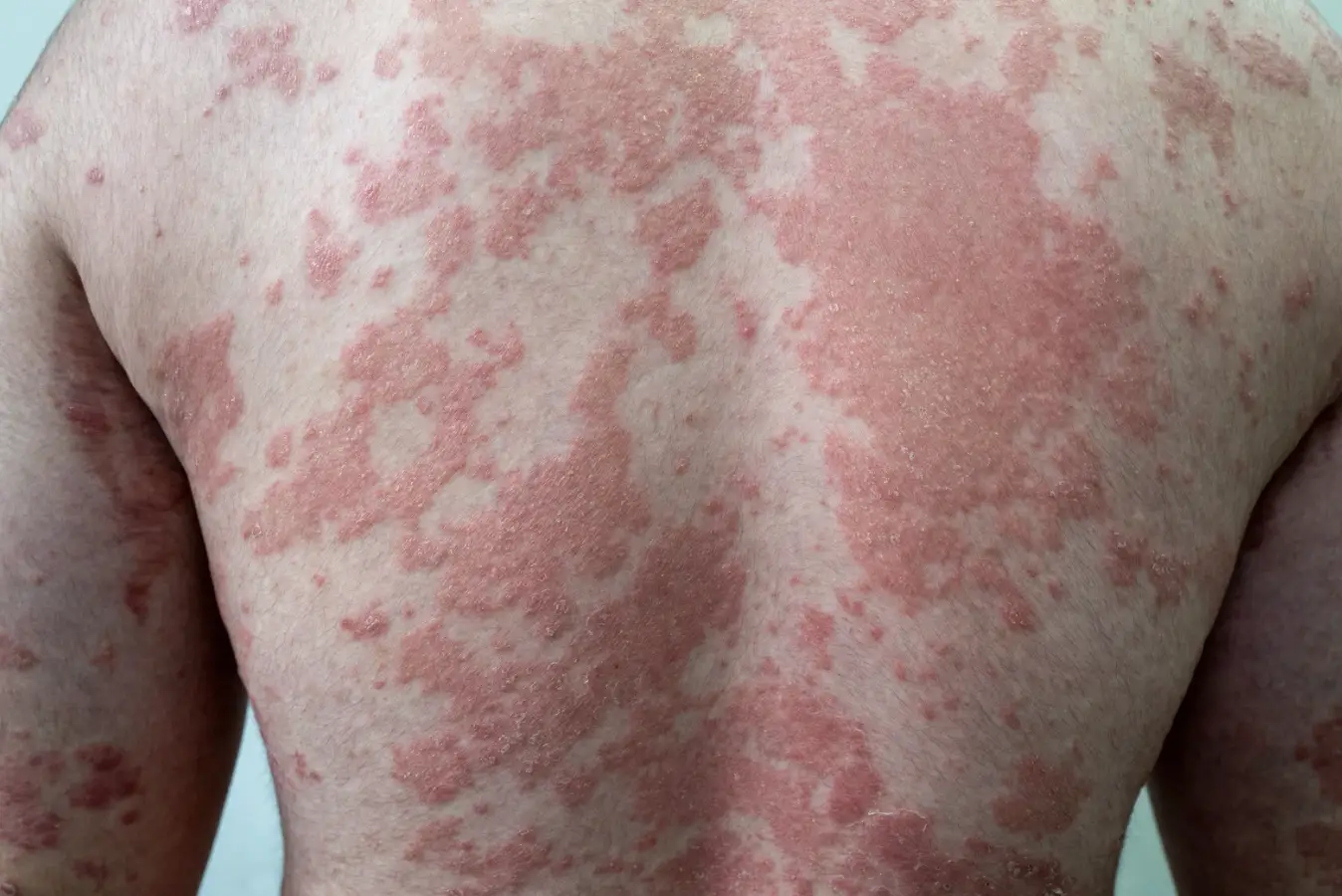
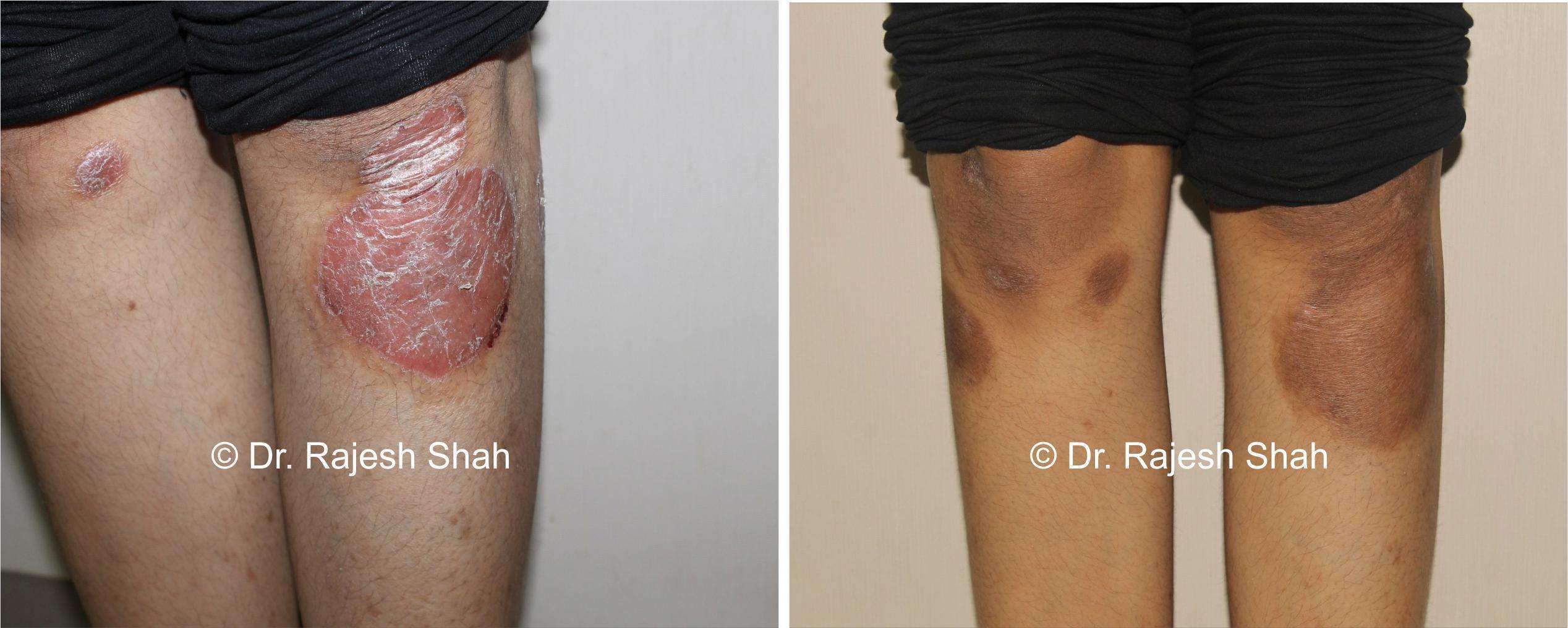
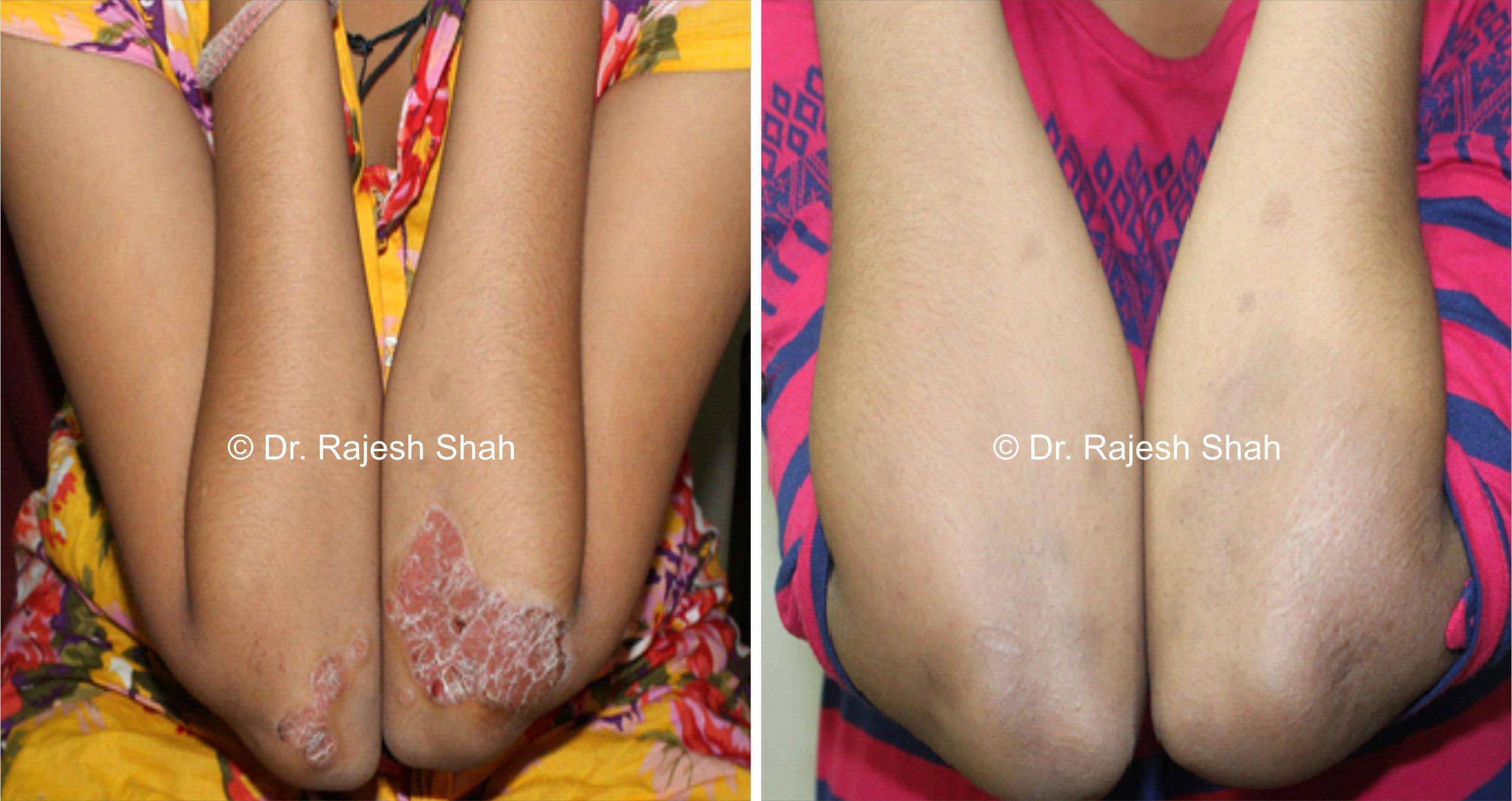
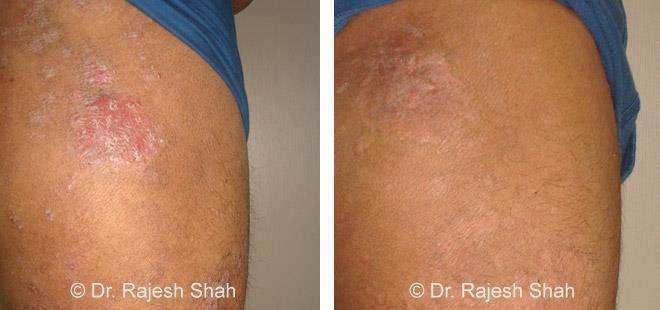
Psoriasis Vulgaris
Causes red, scaly patches on the skin and is the most commonly seen form of psoriasis.
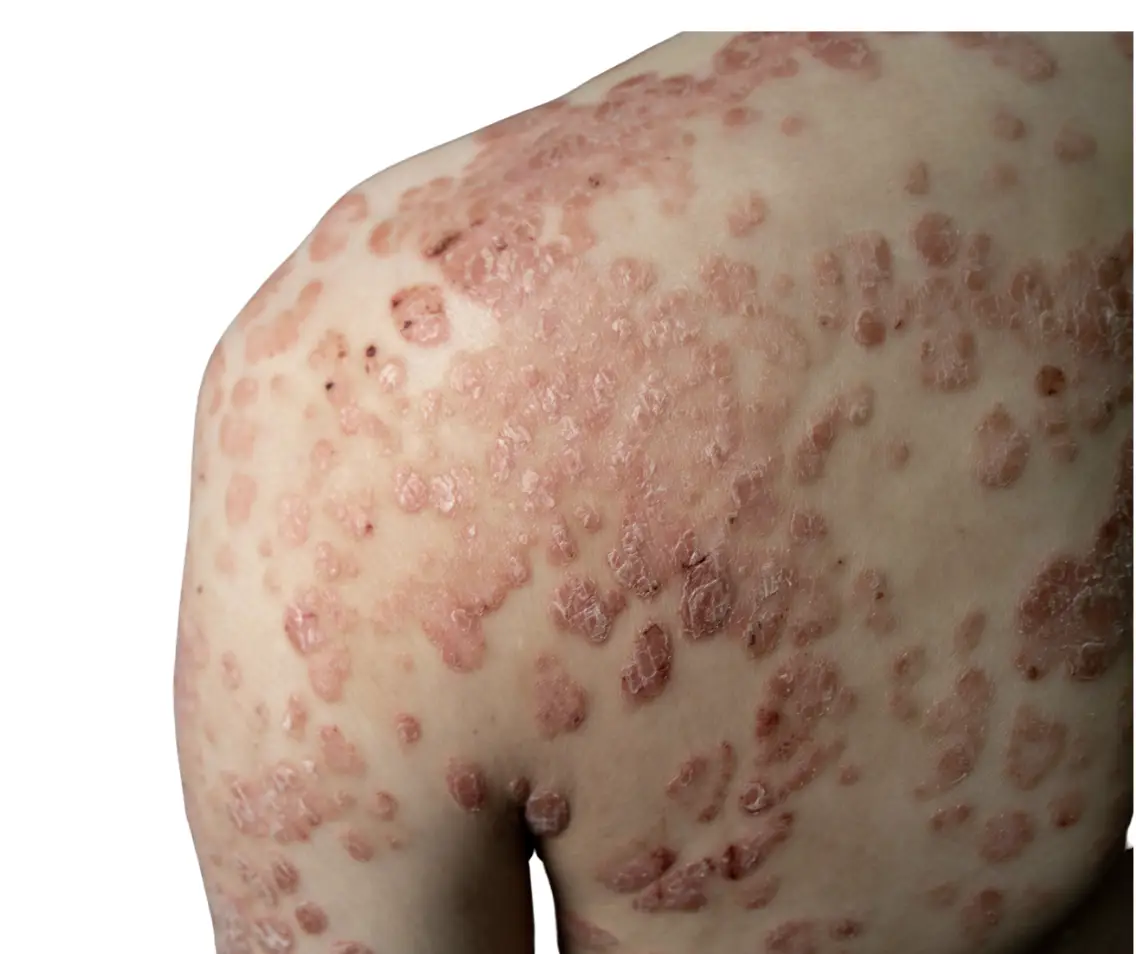
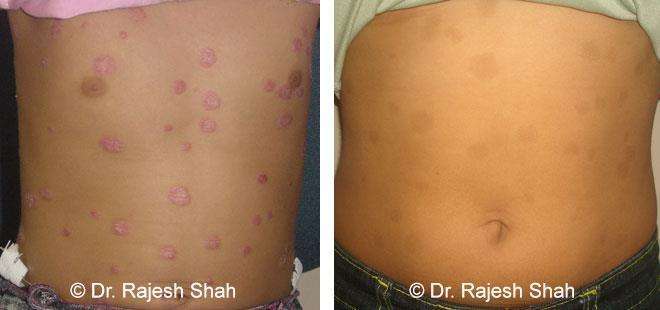
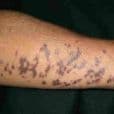
Guttate Psoriasis
Shows small, drop-like spots on the skin, often appearing after infections or sudden triggers.
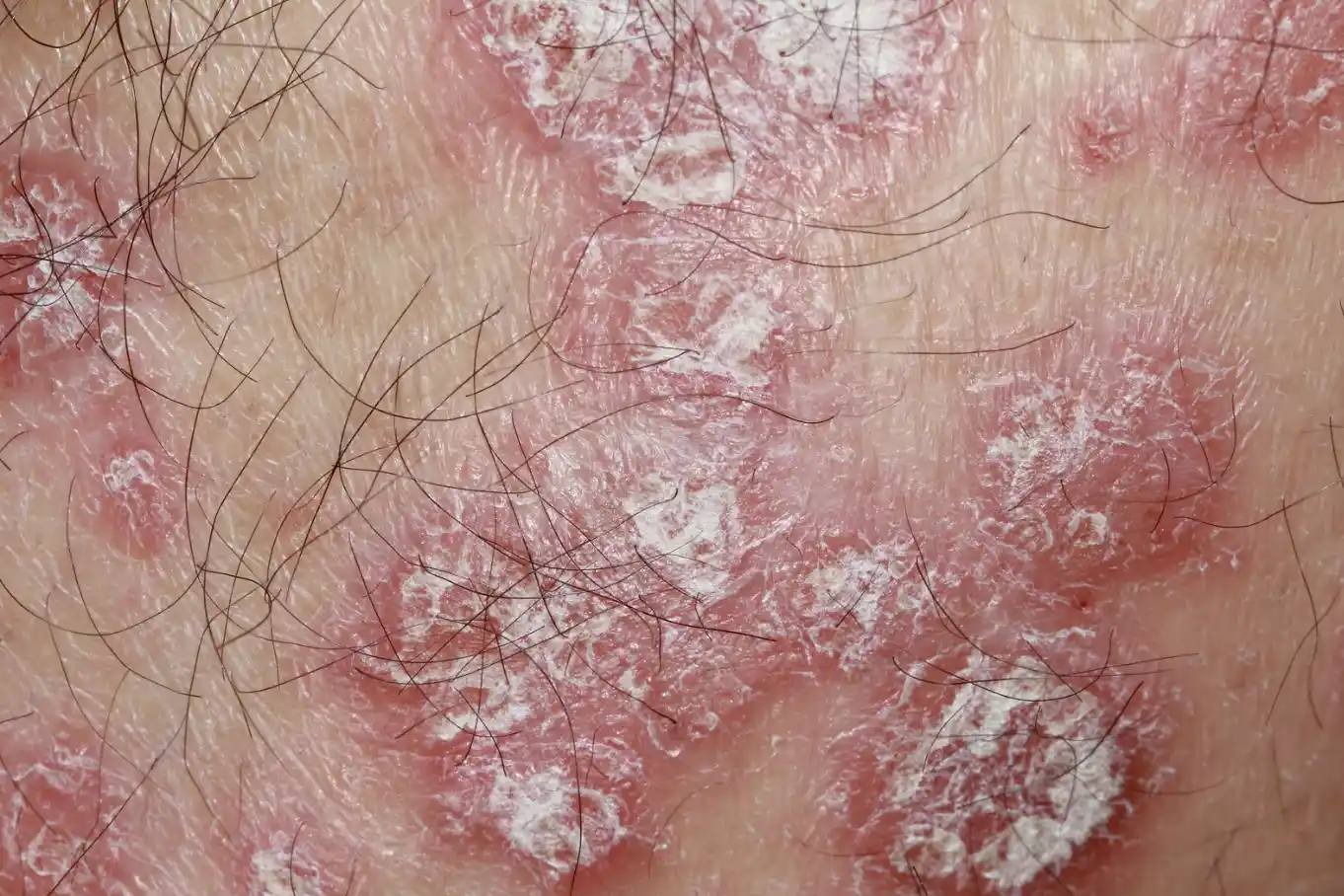
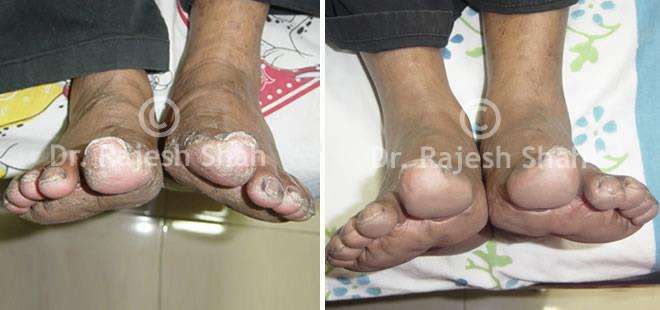
Pustular Psoriasis
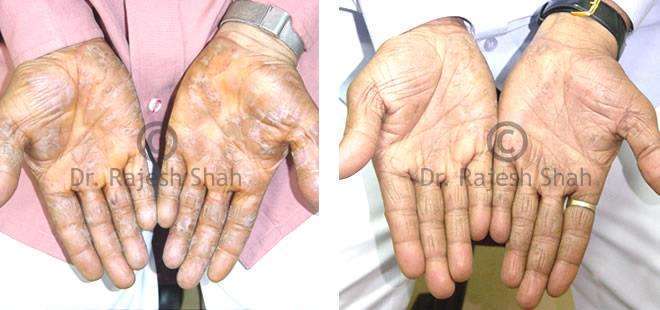
Presents white, sterile blisters on red skin, usually affecting hands, feet, or larger areas.
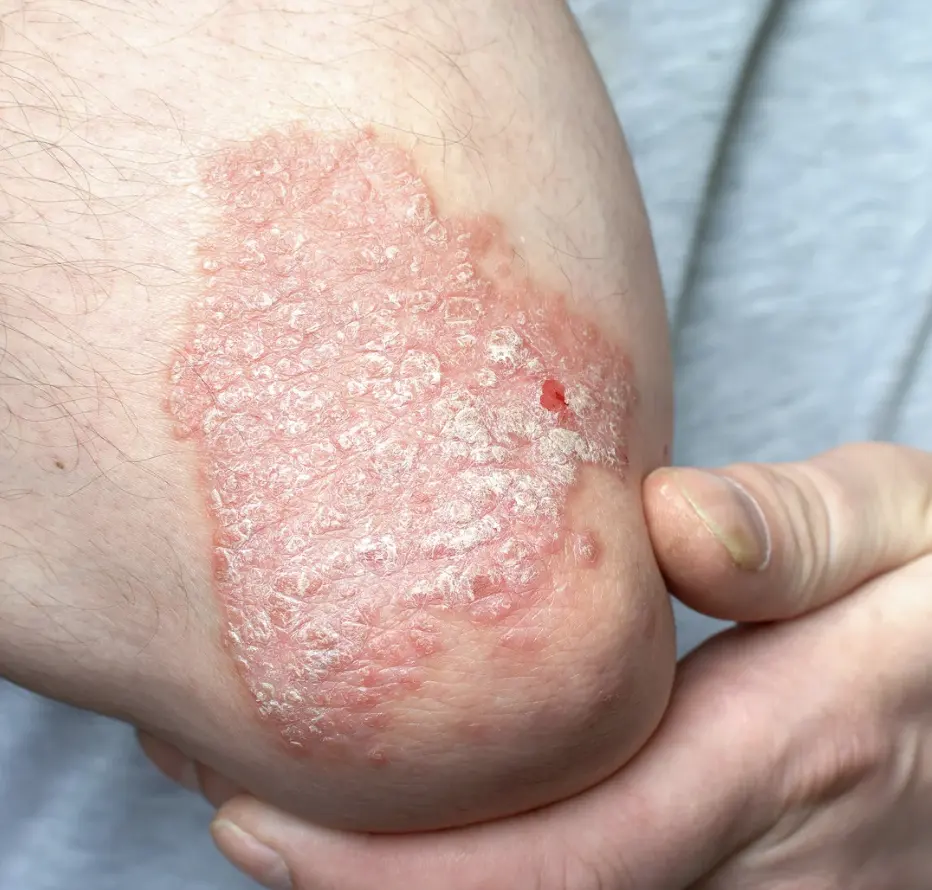
Inverse Psoriasis
Develops in skin folds with smooth, red patches that worsen with friction and sweating.

Our Expertise
-
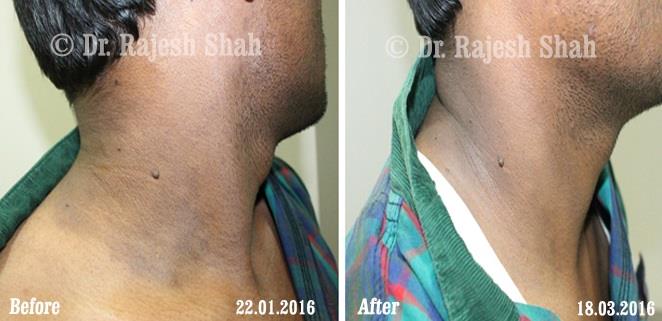
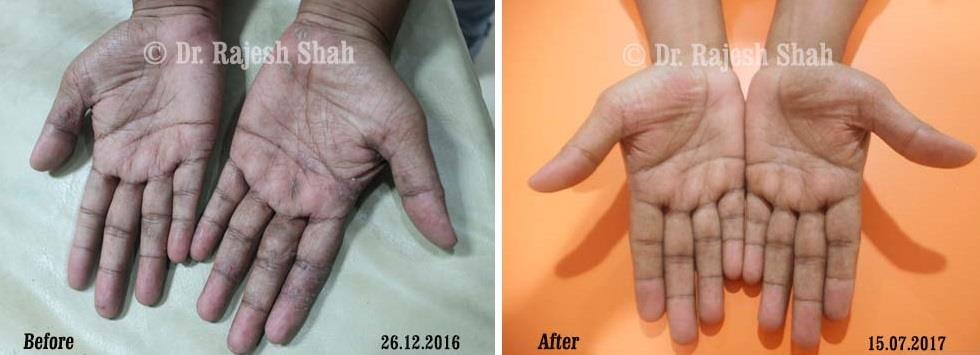
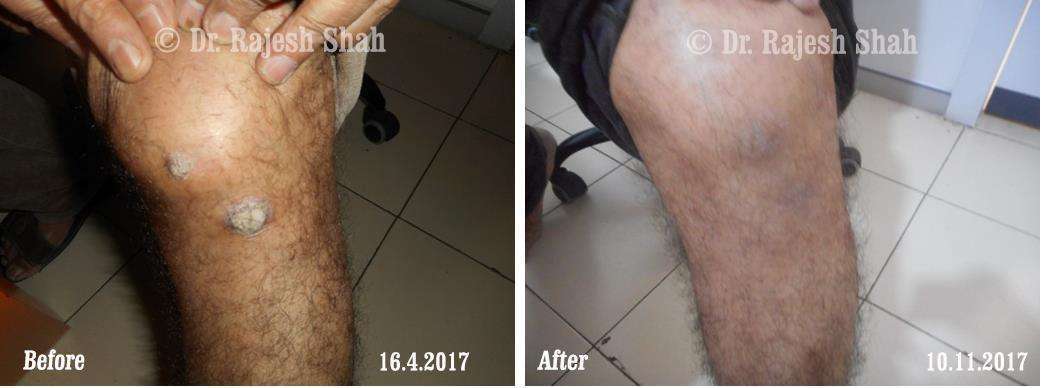
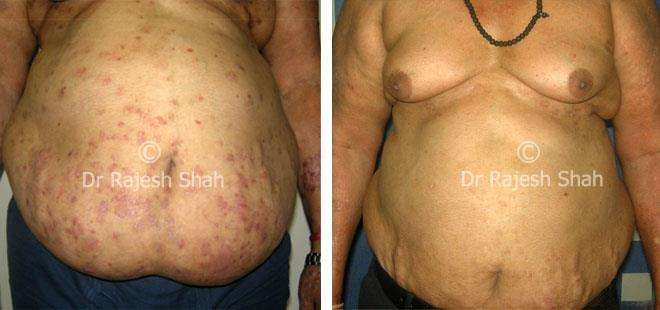
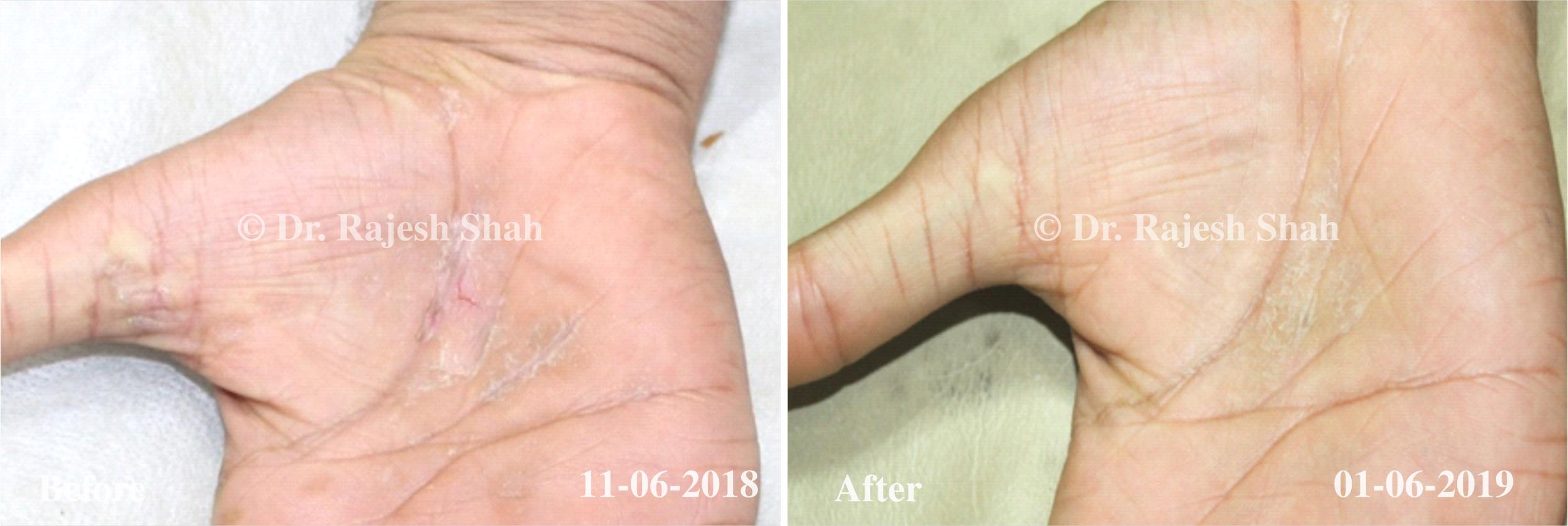
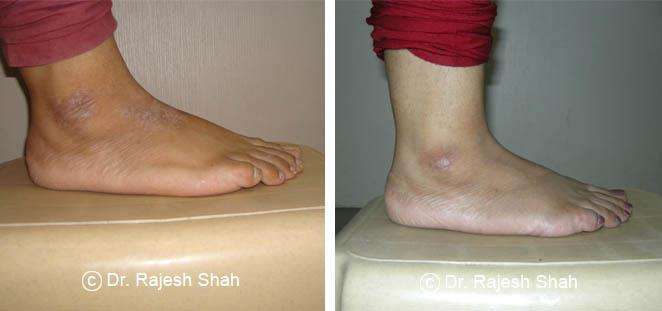
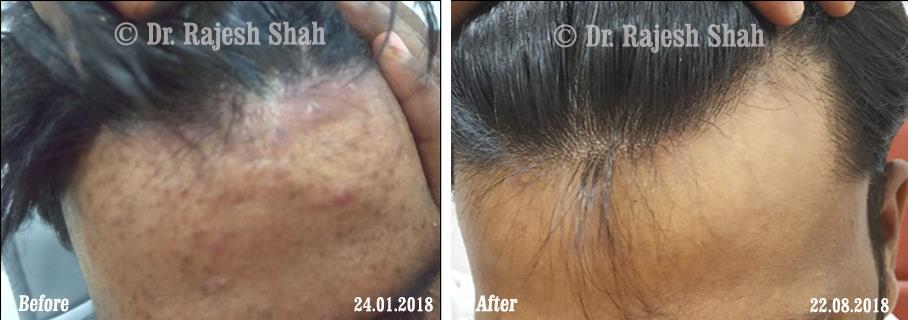
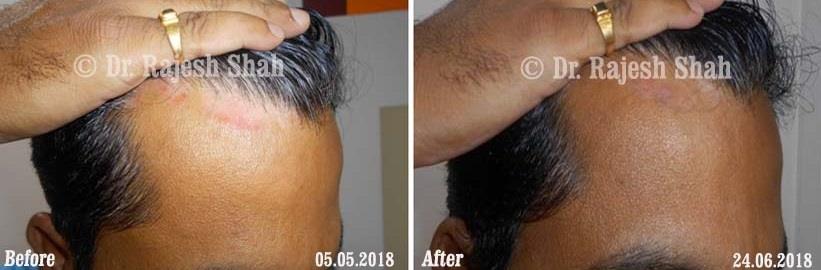
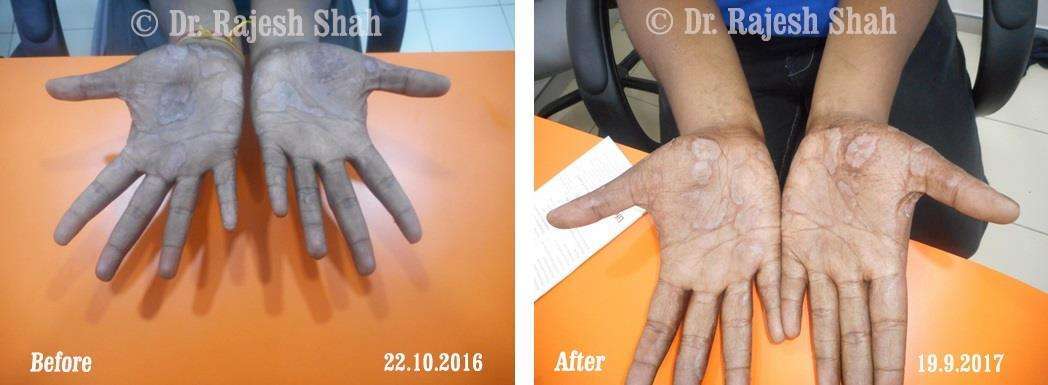
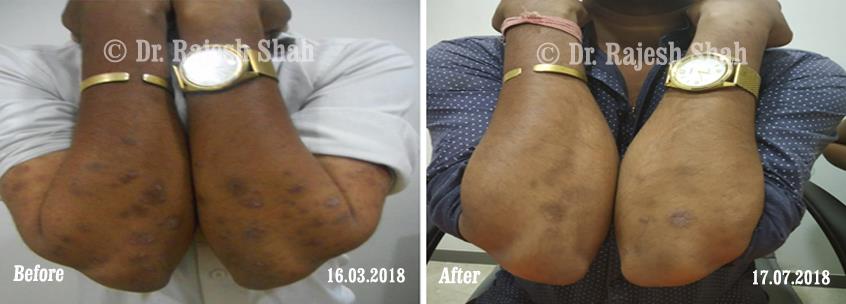
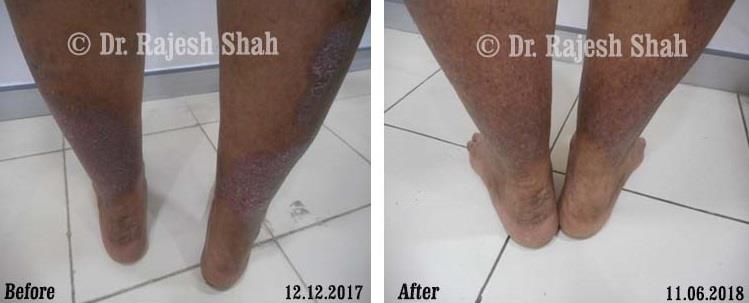
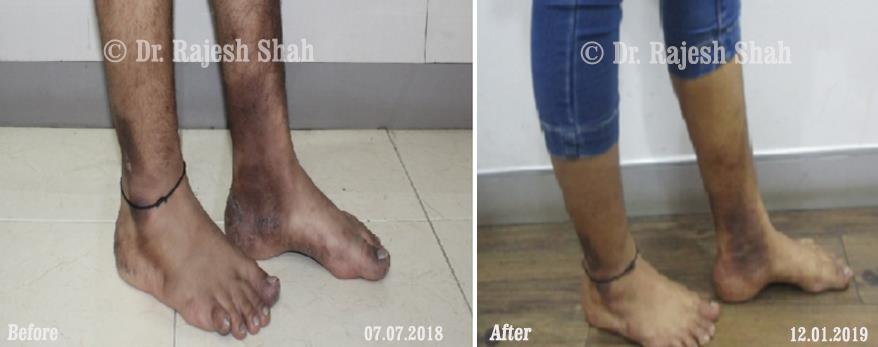
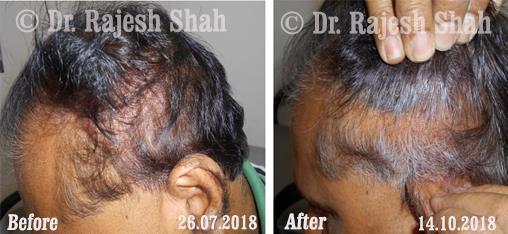
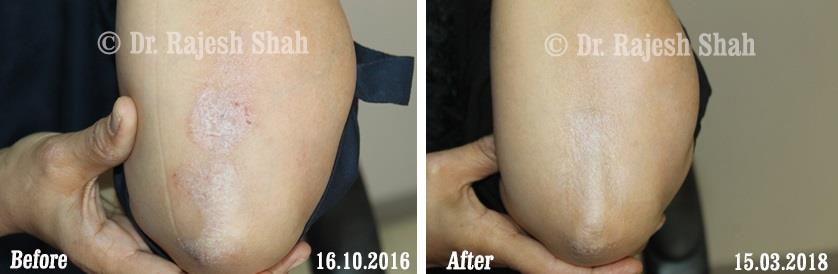
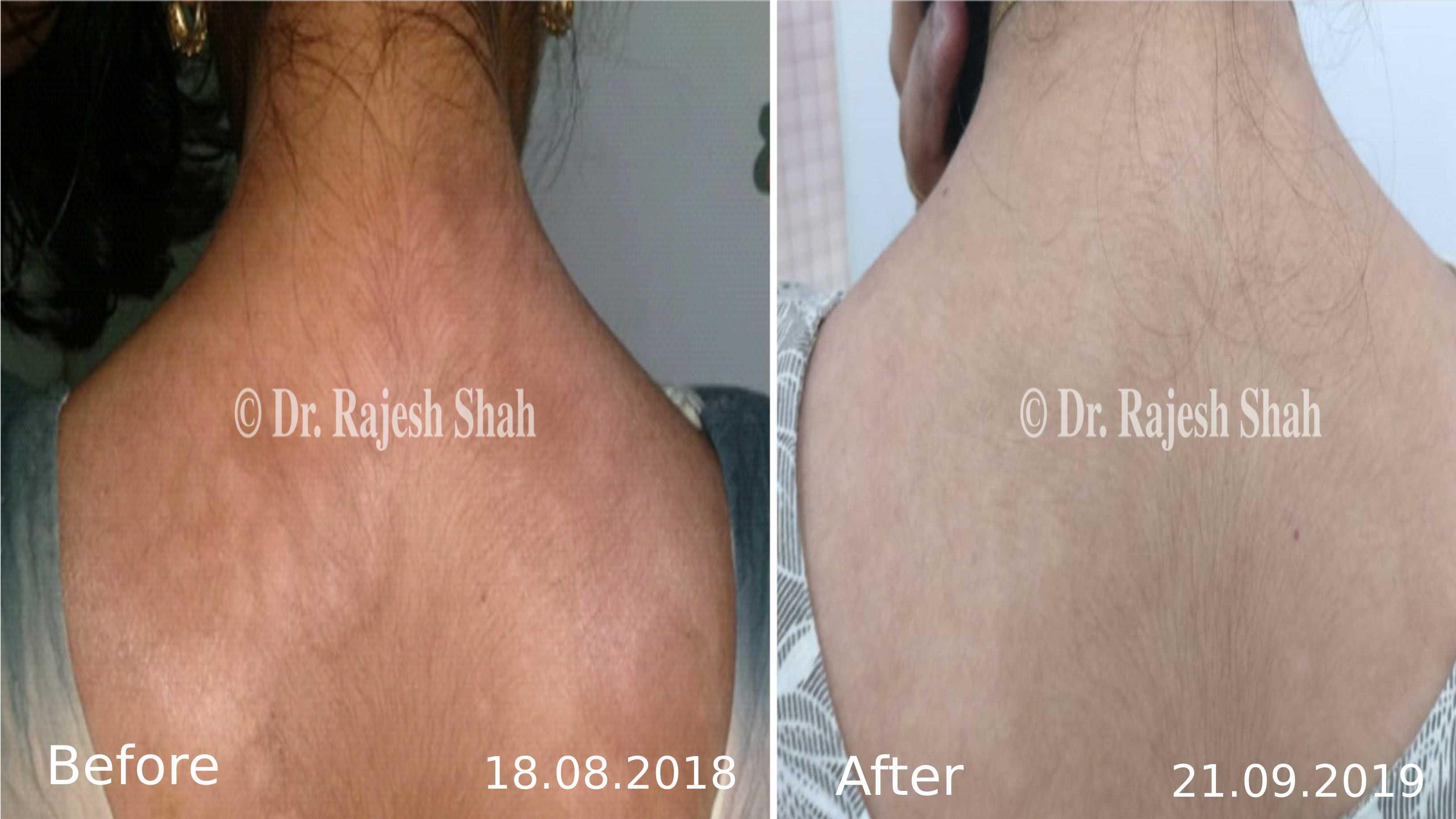
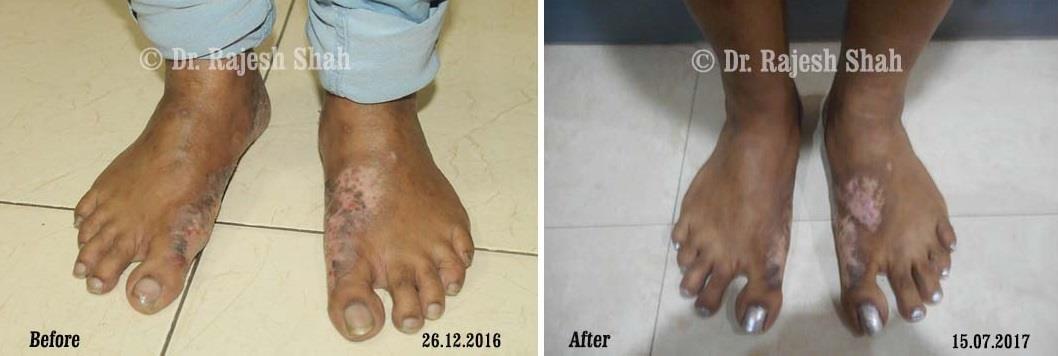
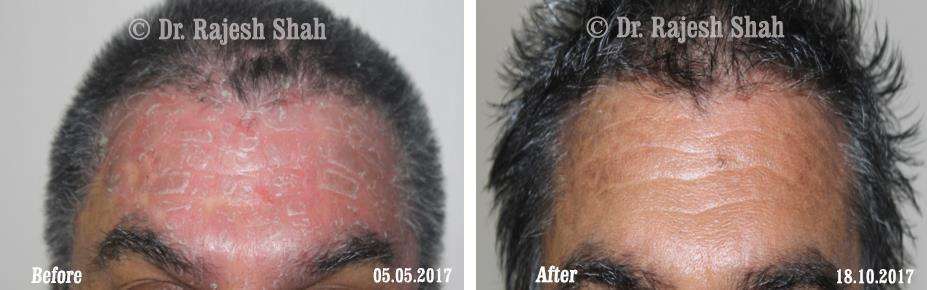
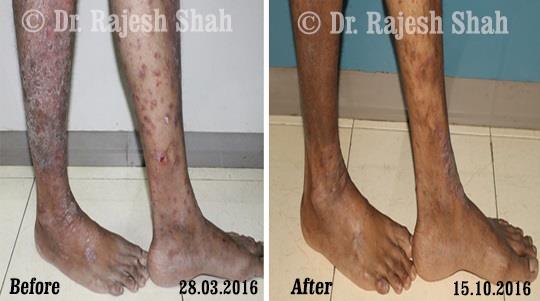
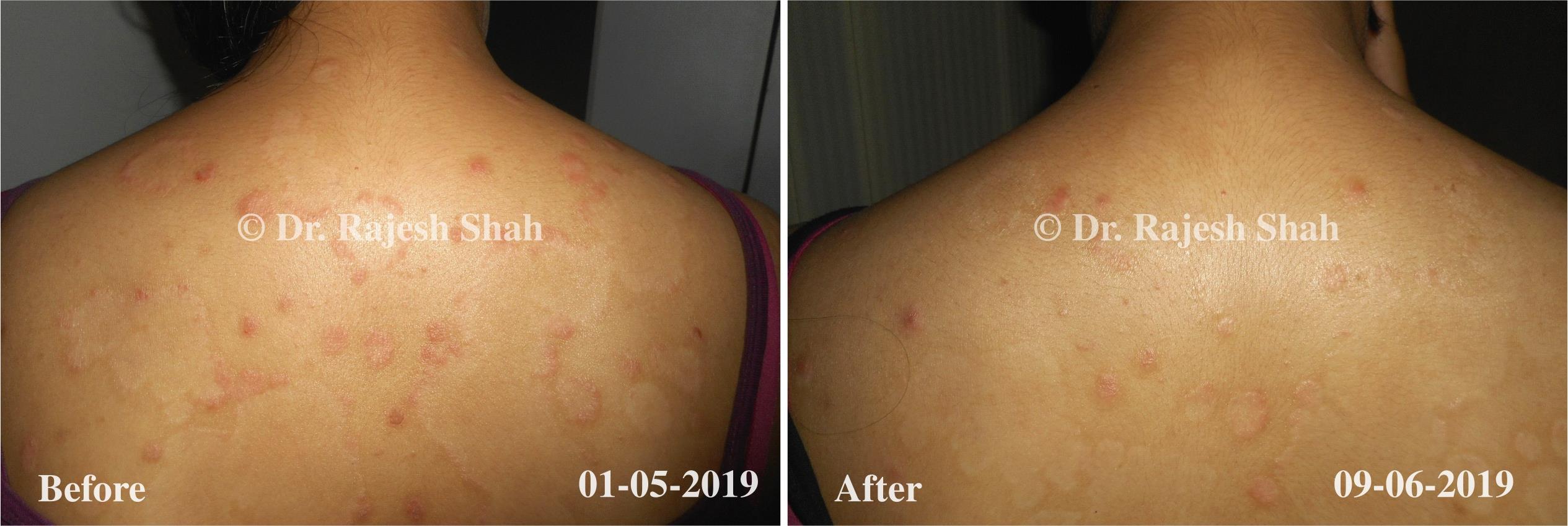
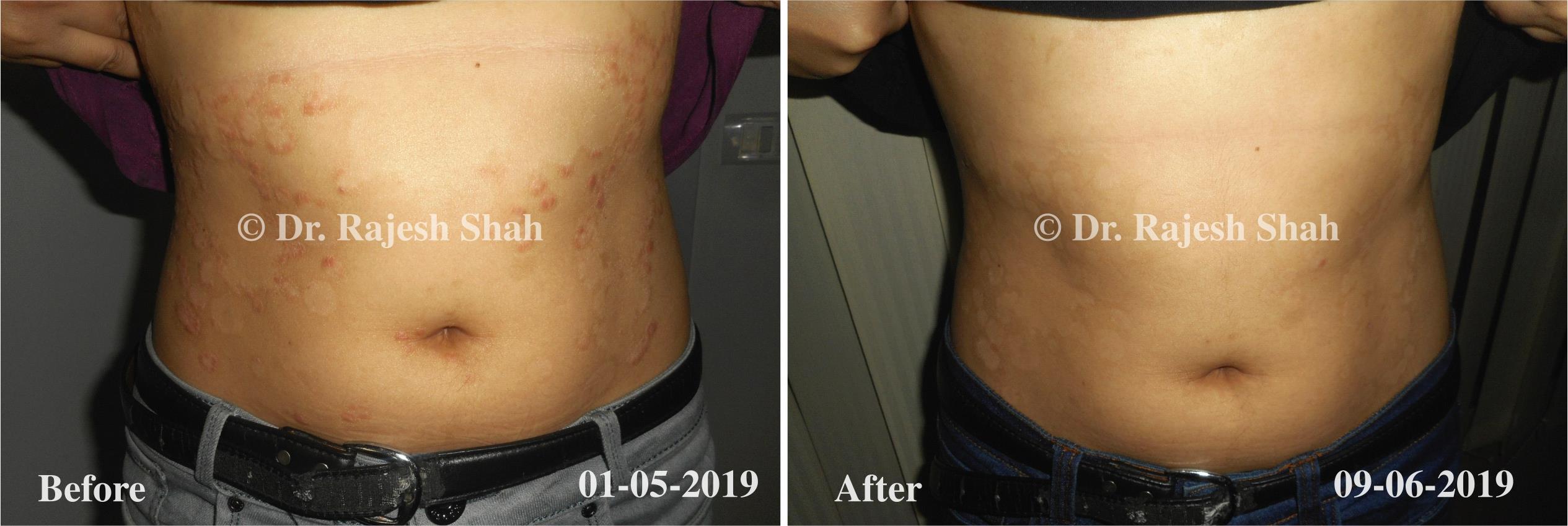
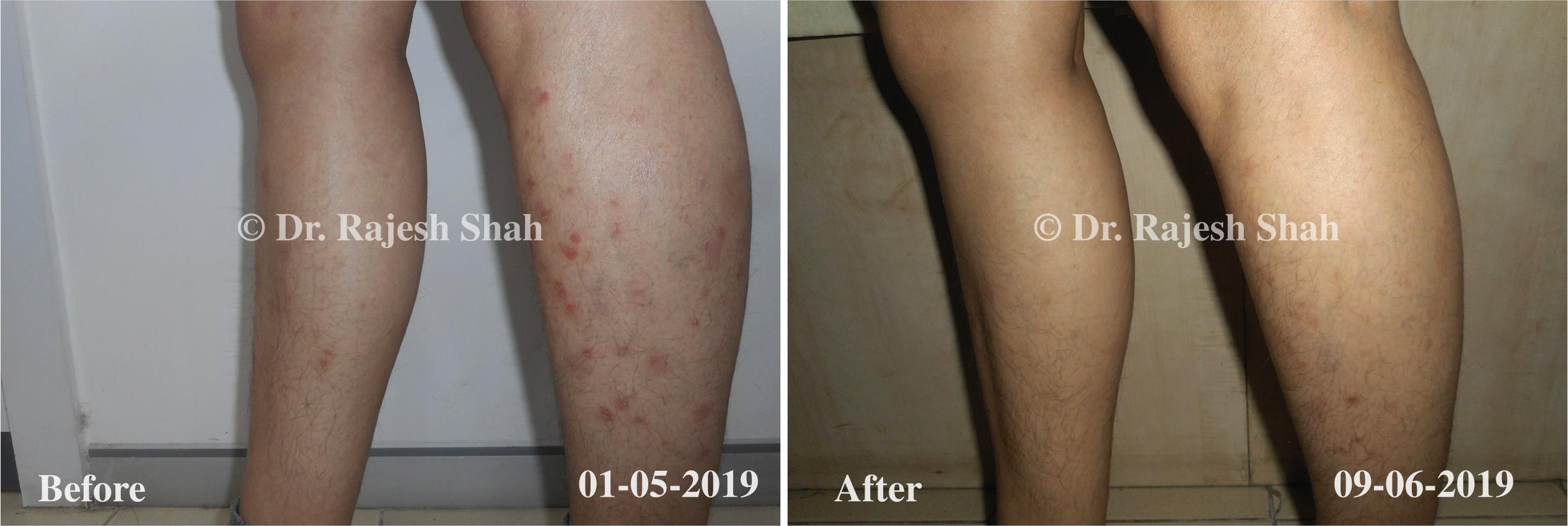
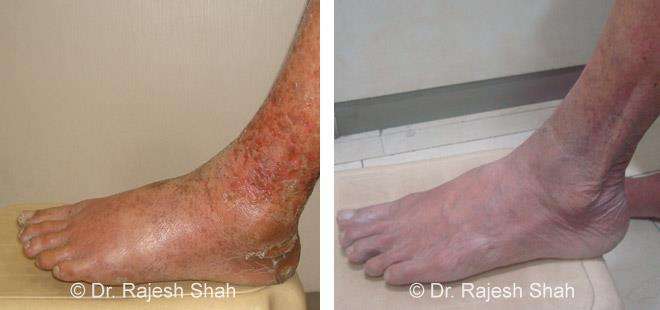
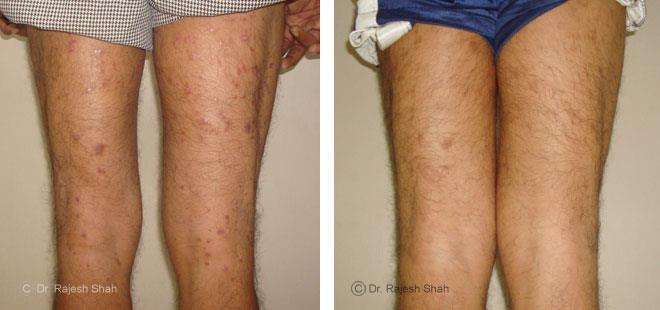
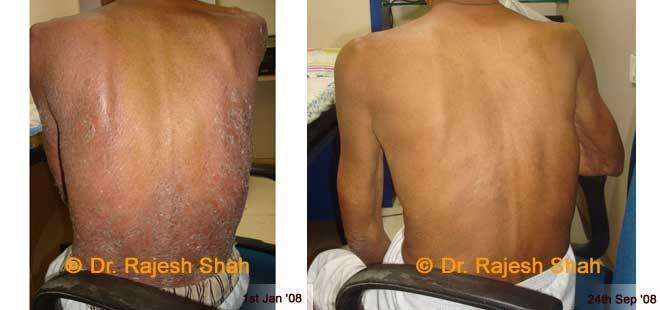
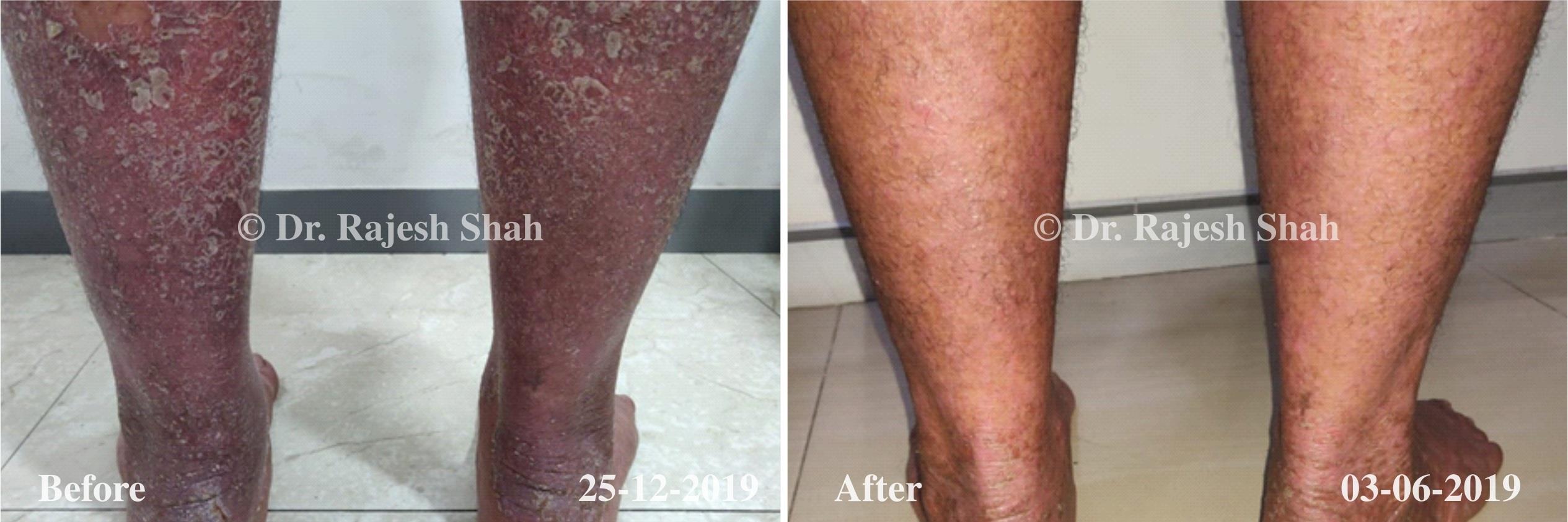
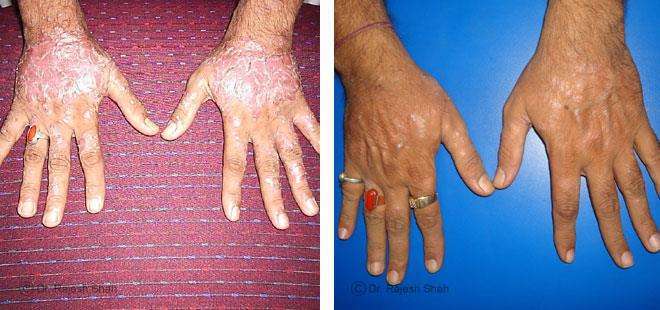
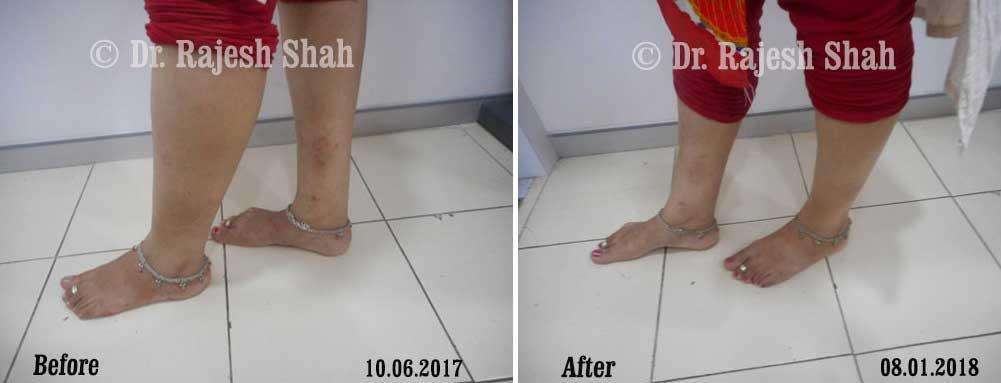
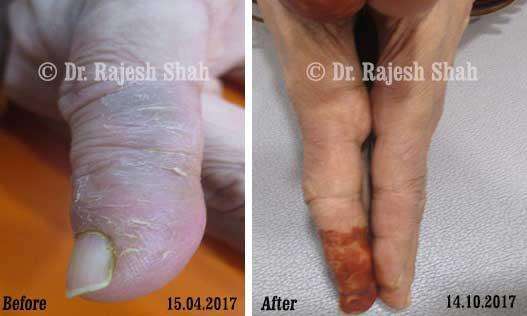
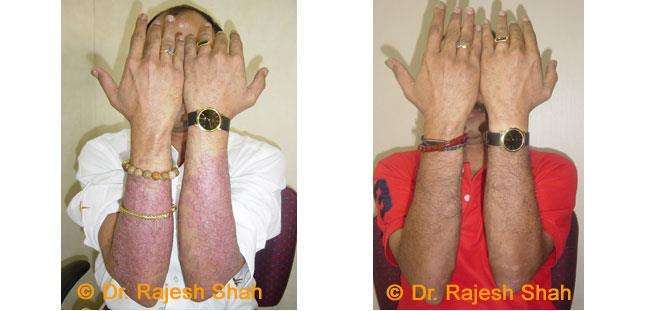
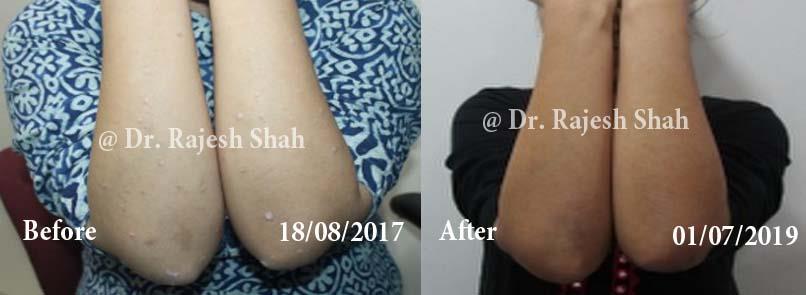
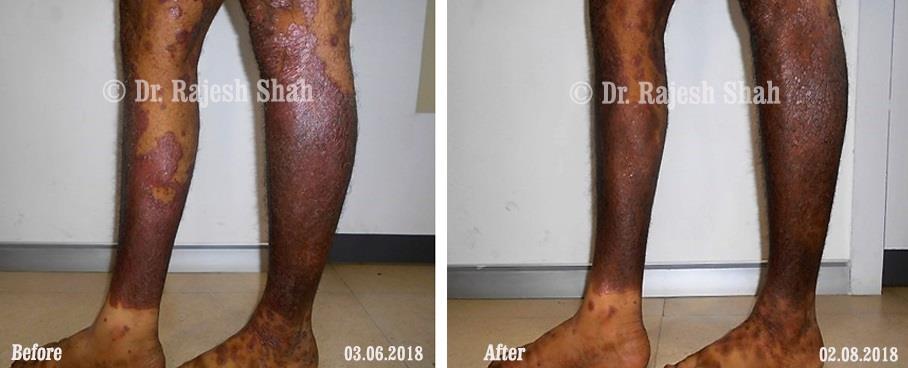
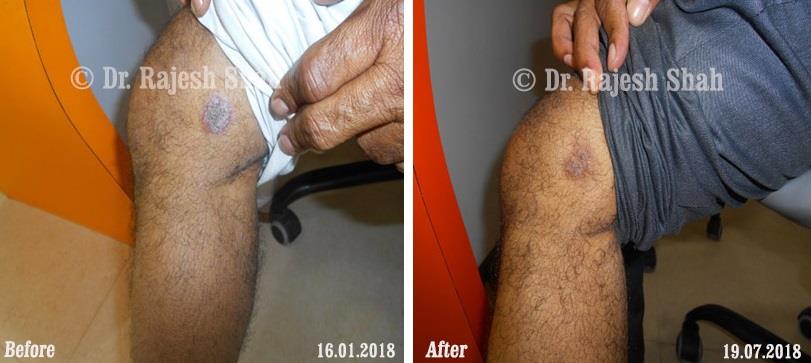
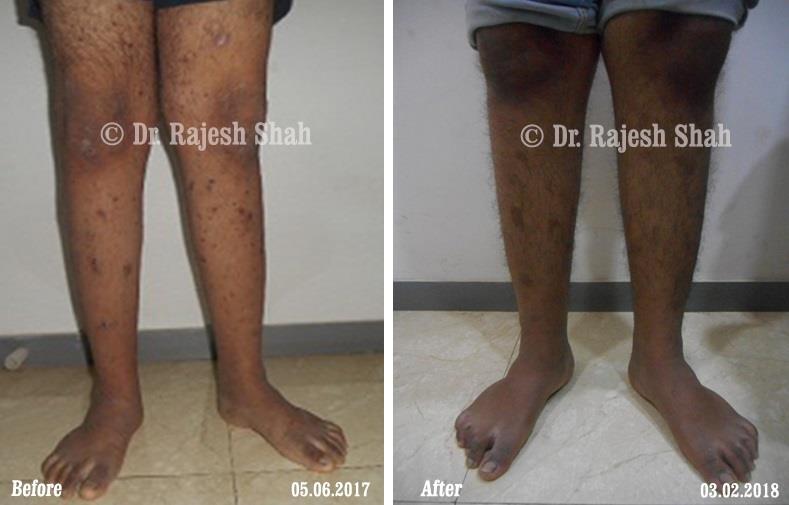
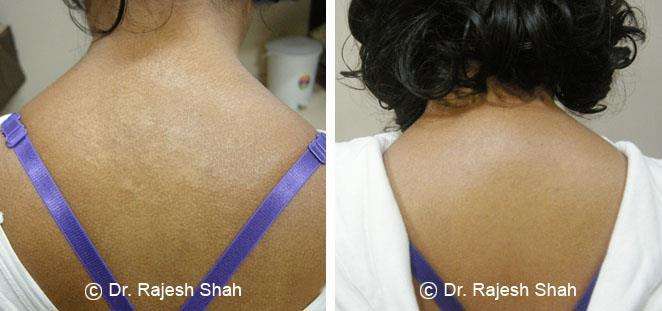
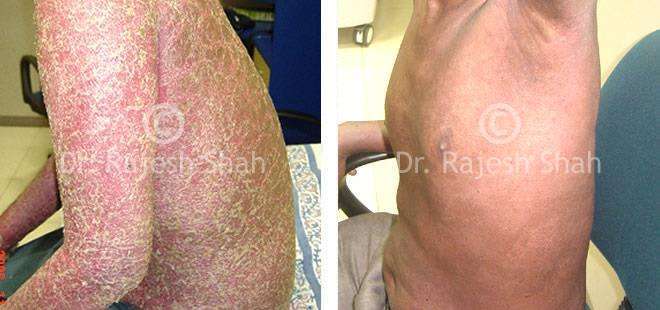
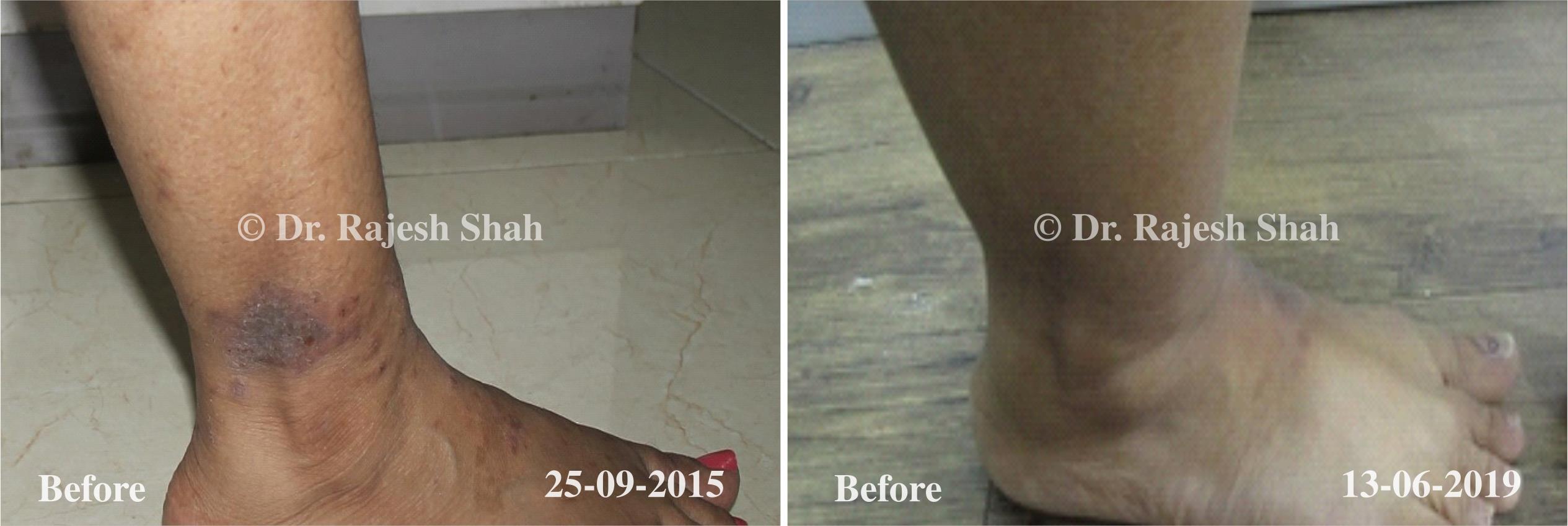
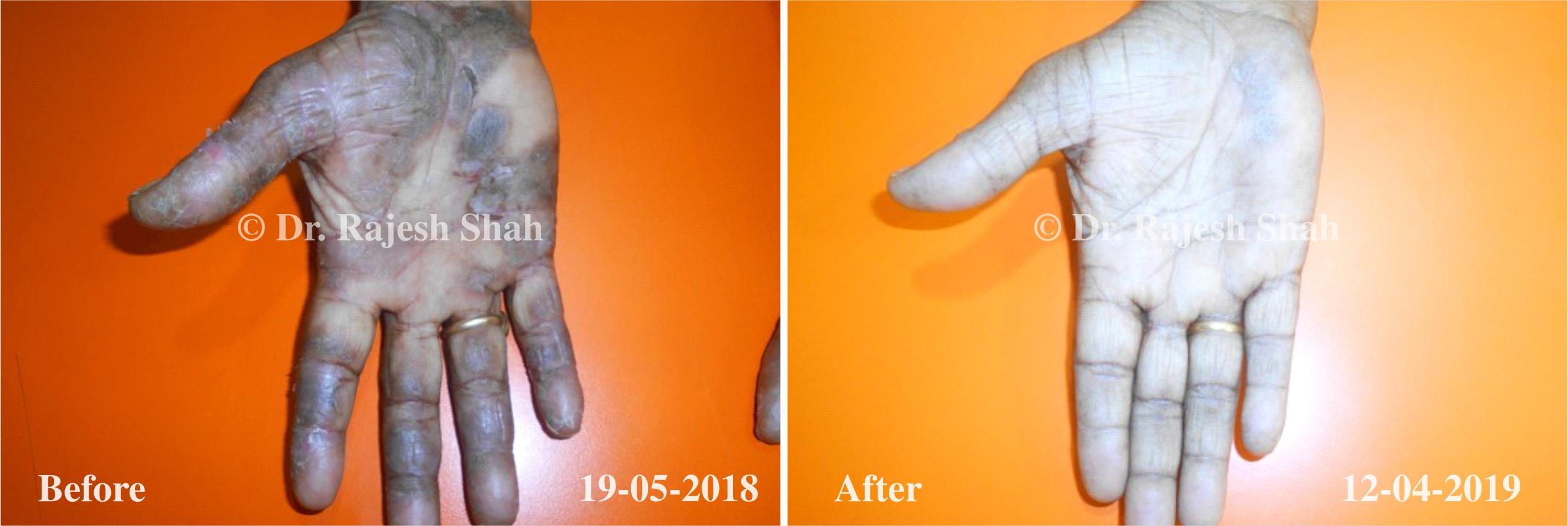
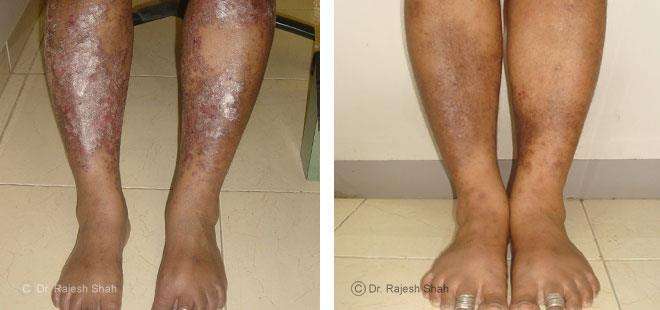
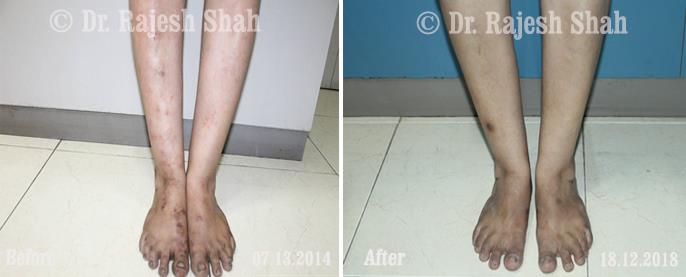
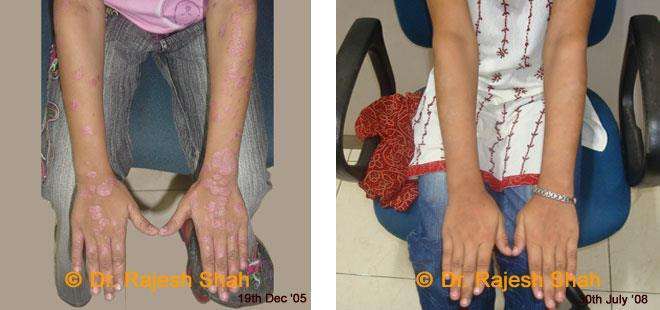
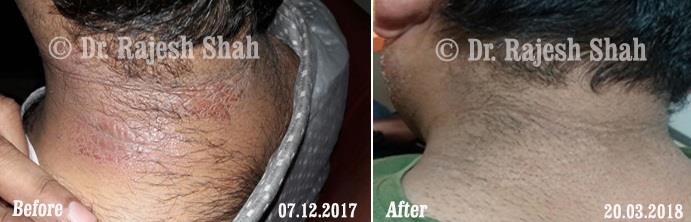
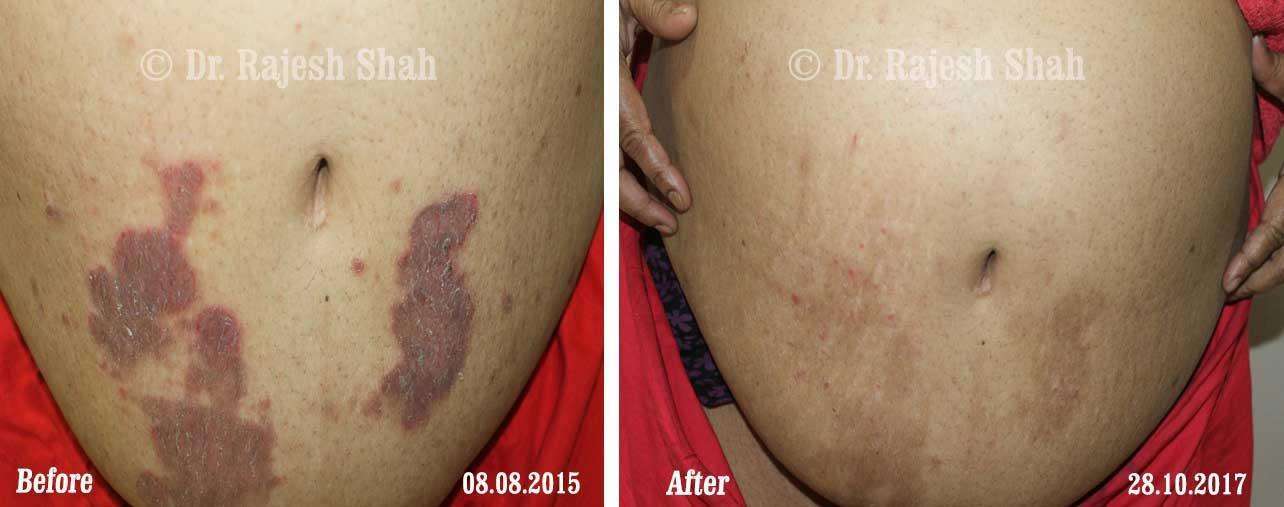
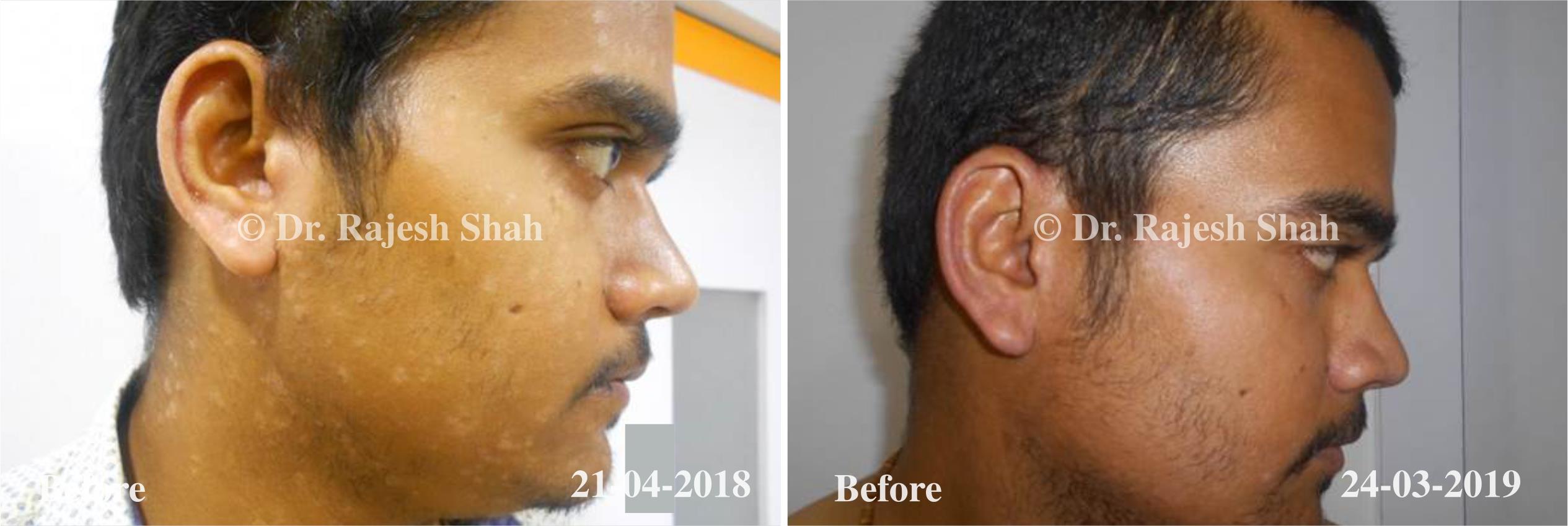
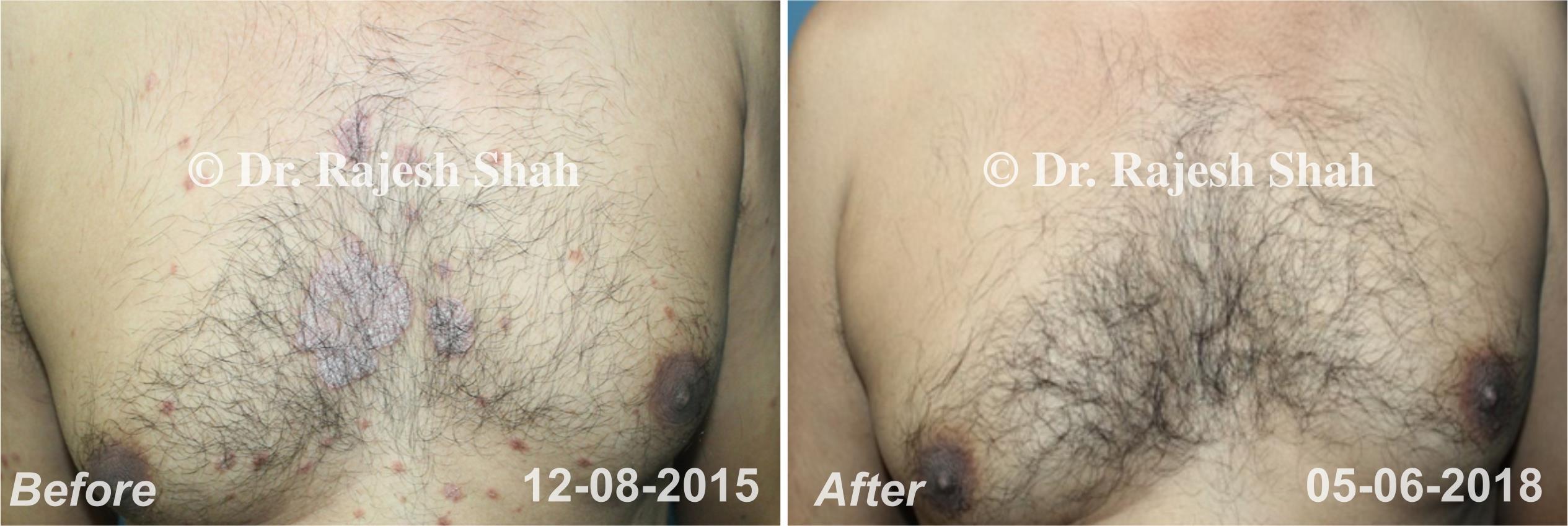
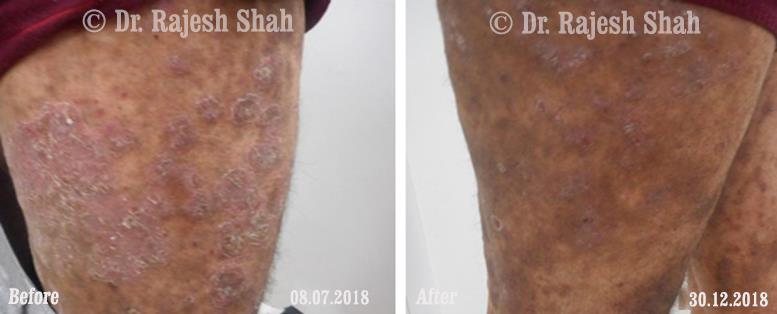
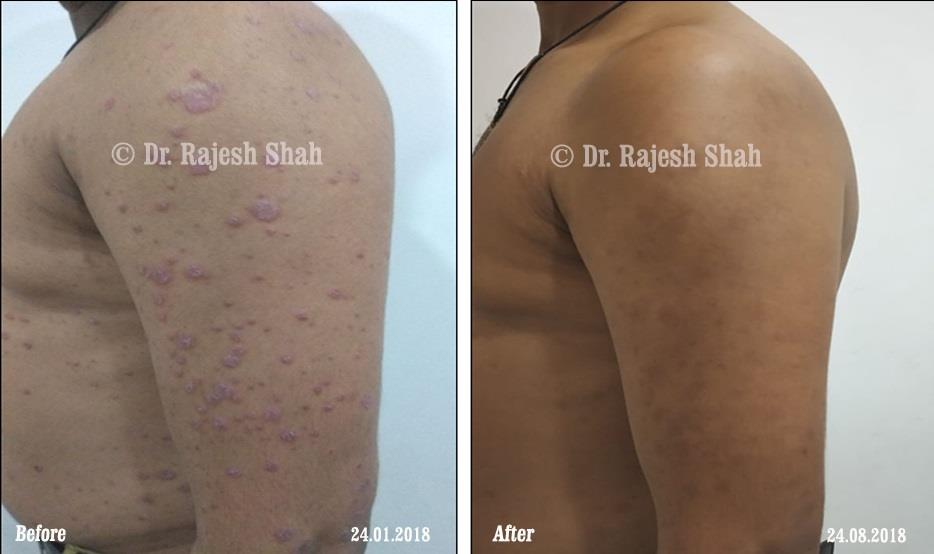
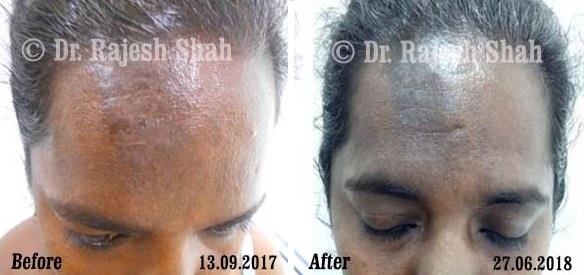
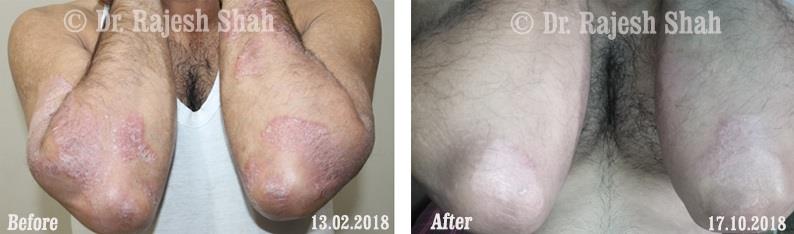
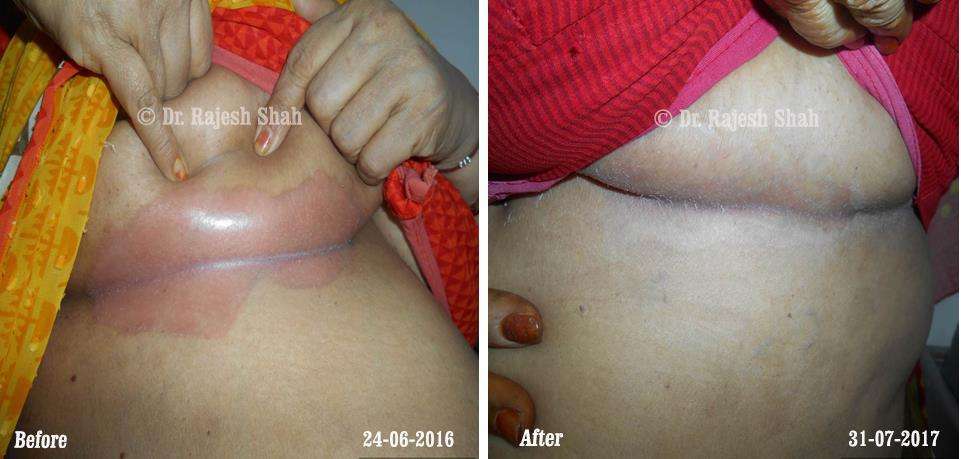
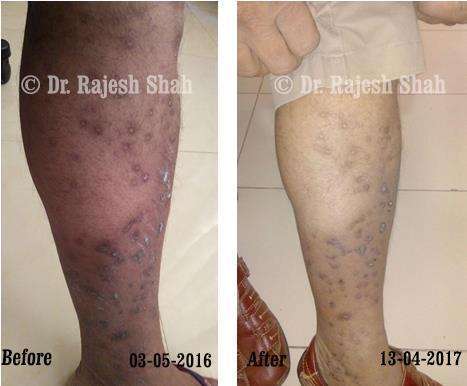
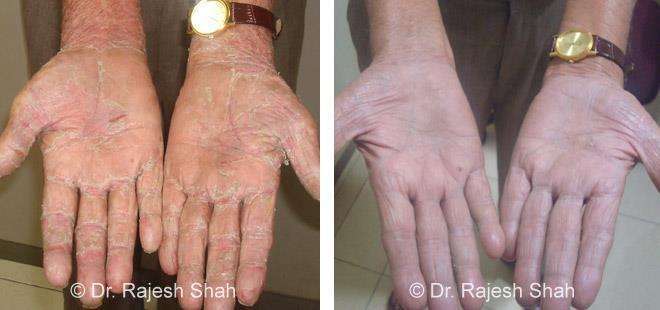
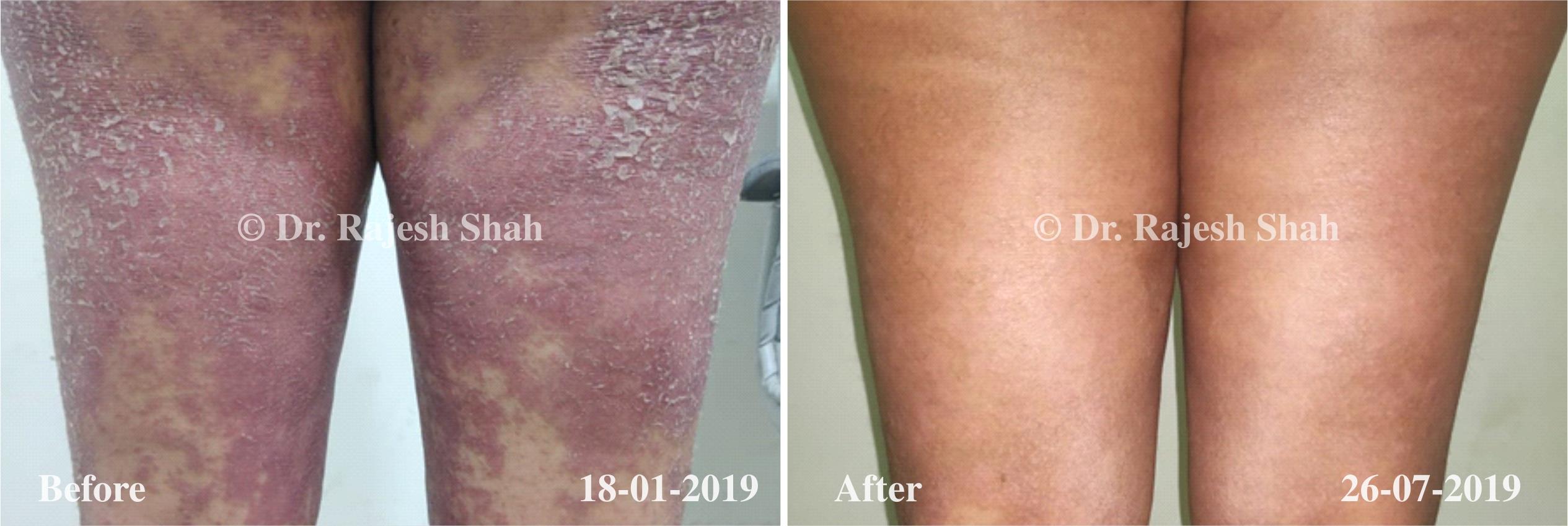
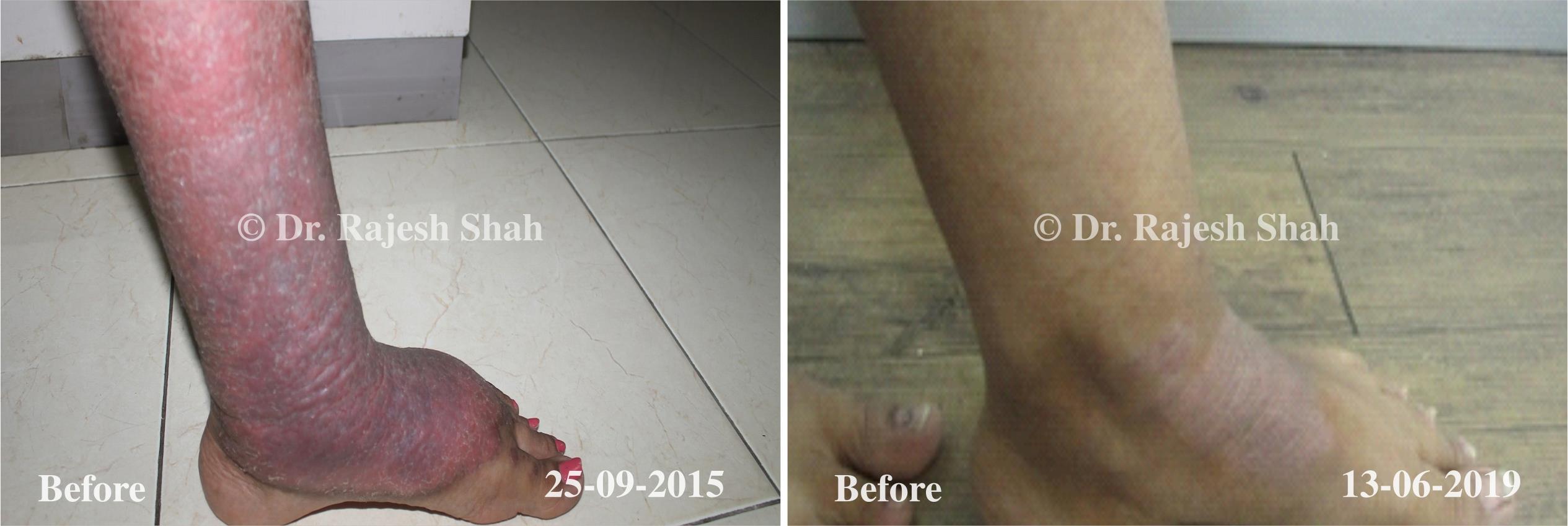
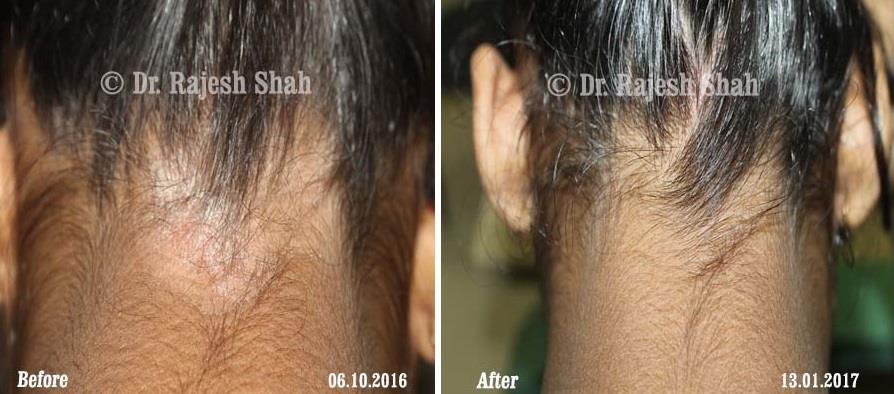
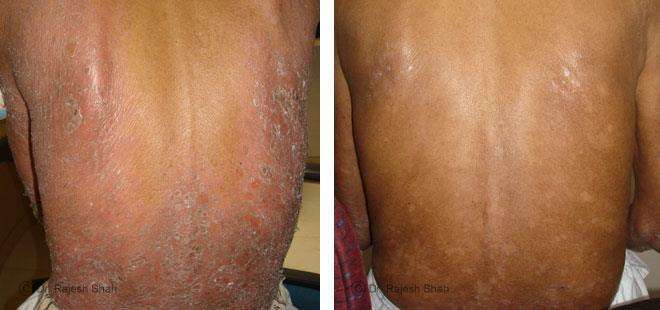
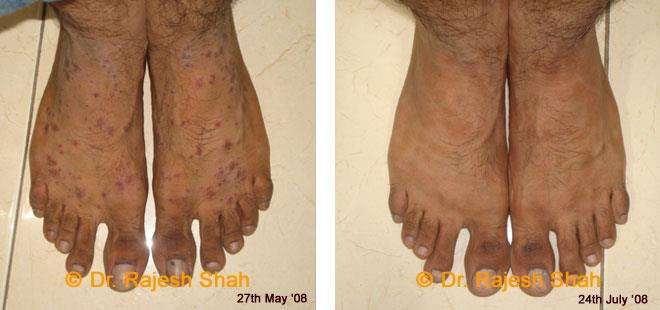
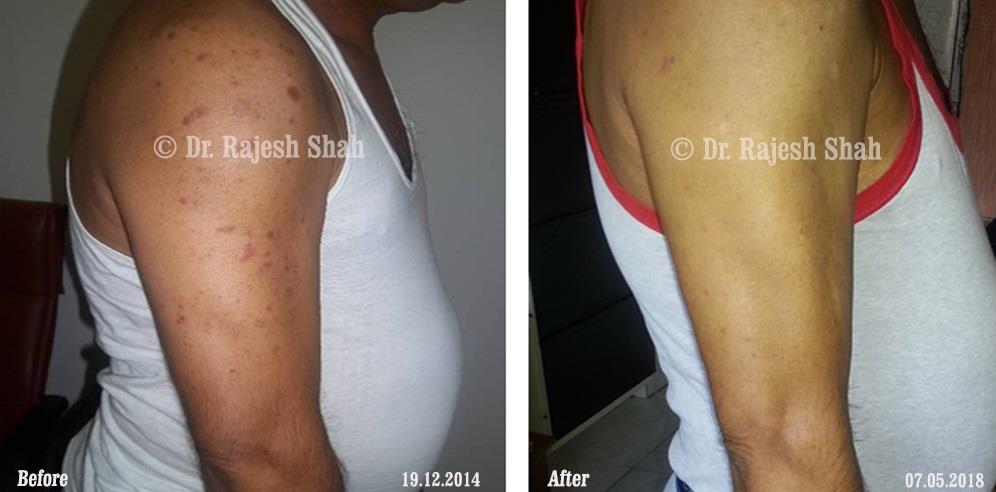
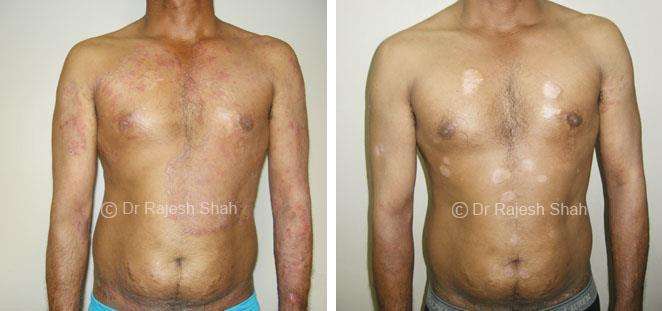
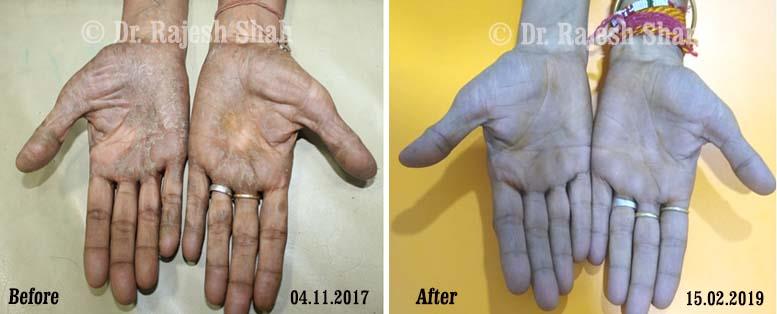
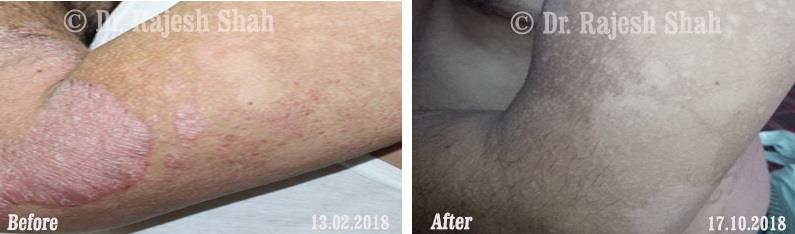
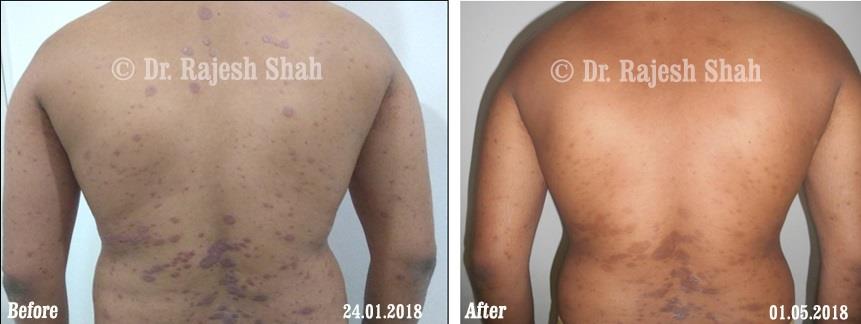
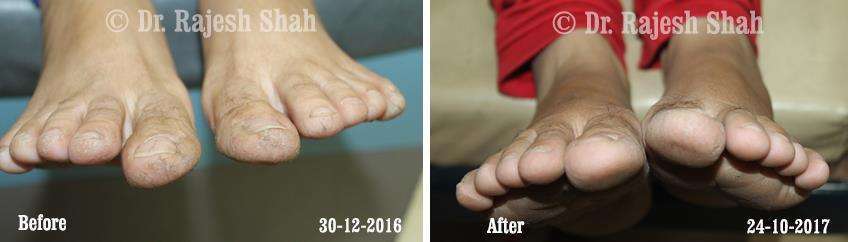
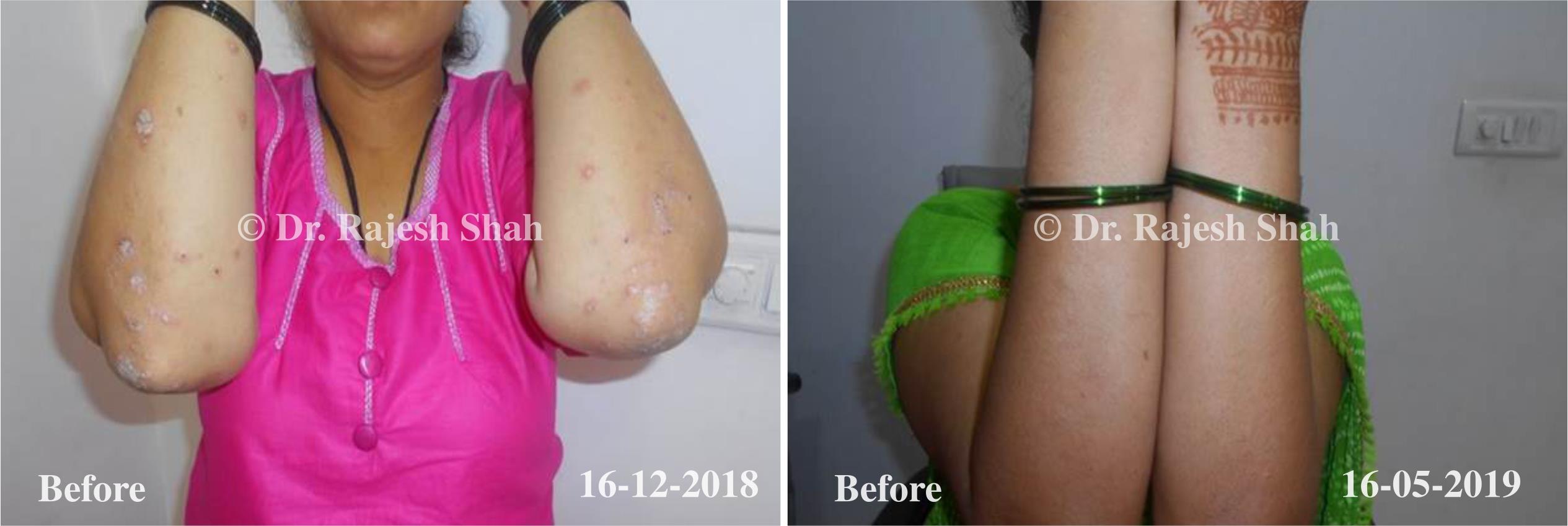
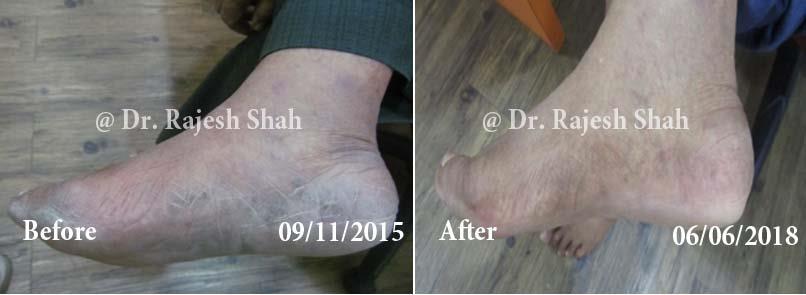
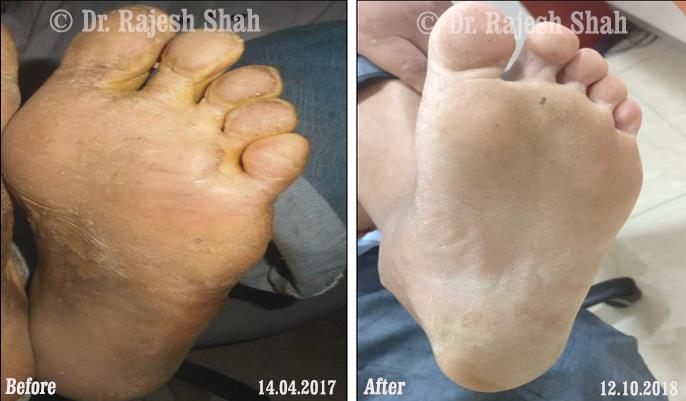
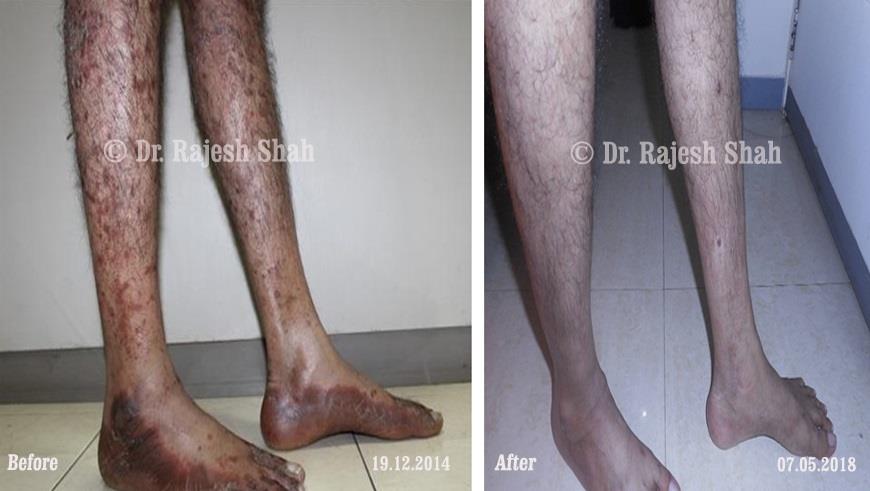
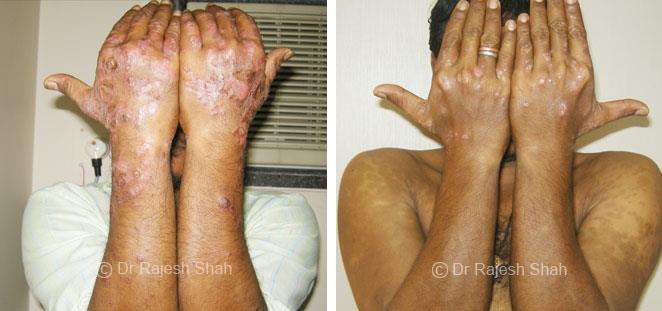
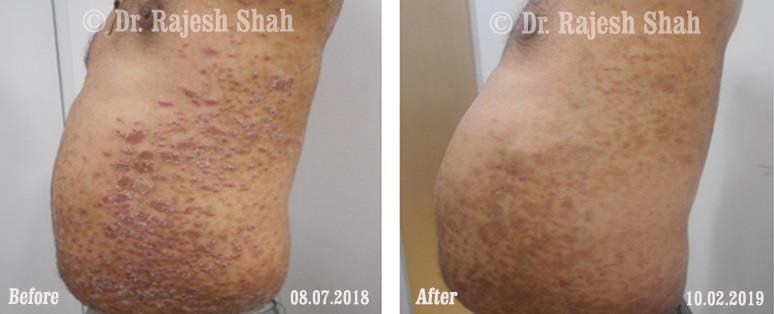
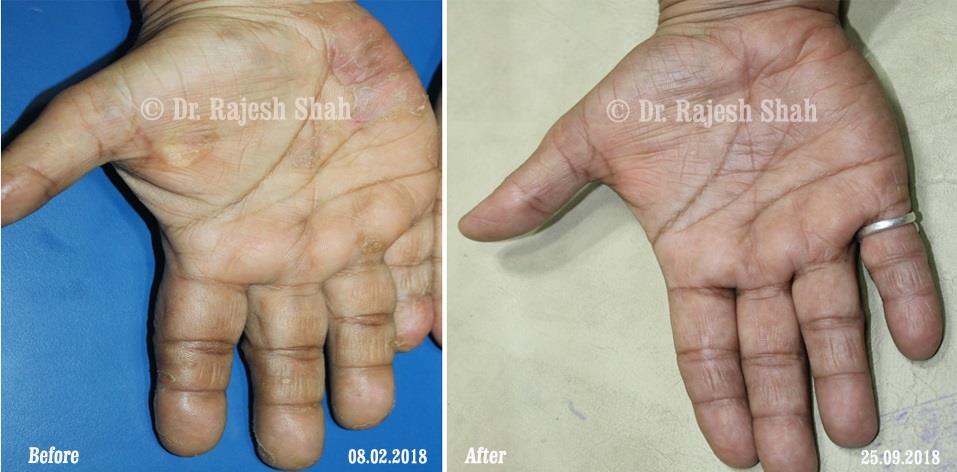
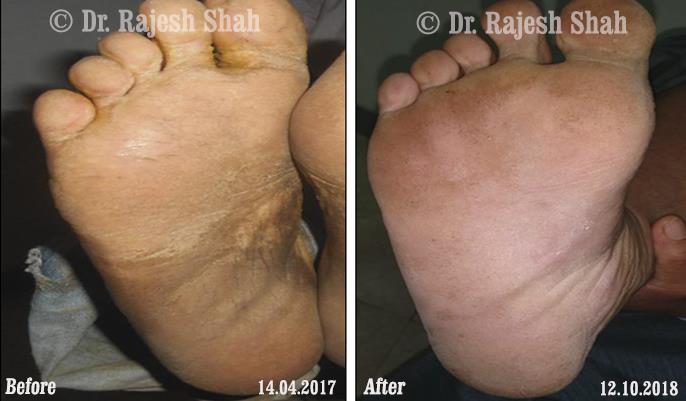
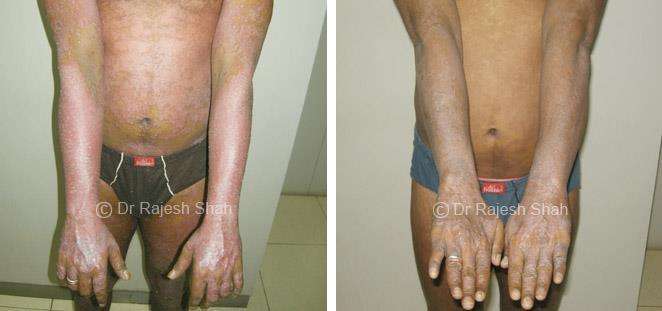
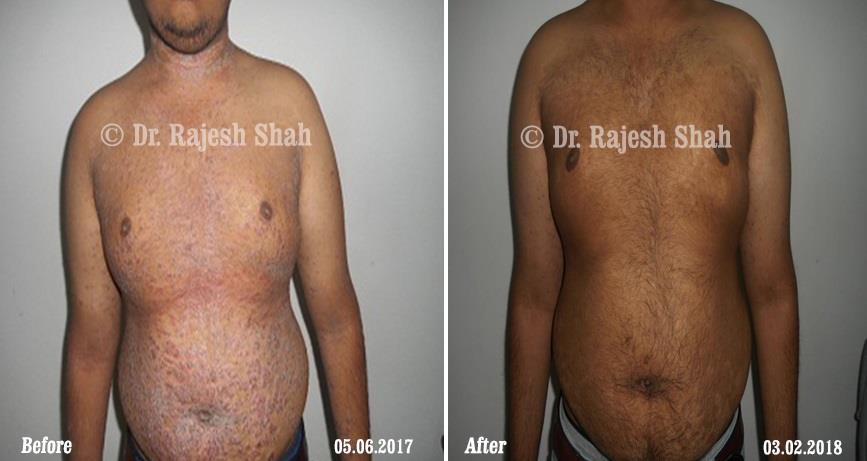
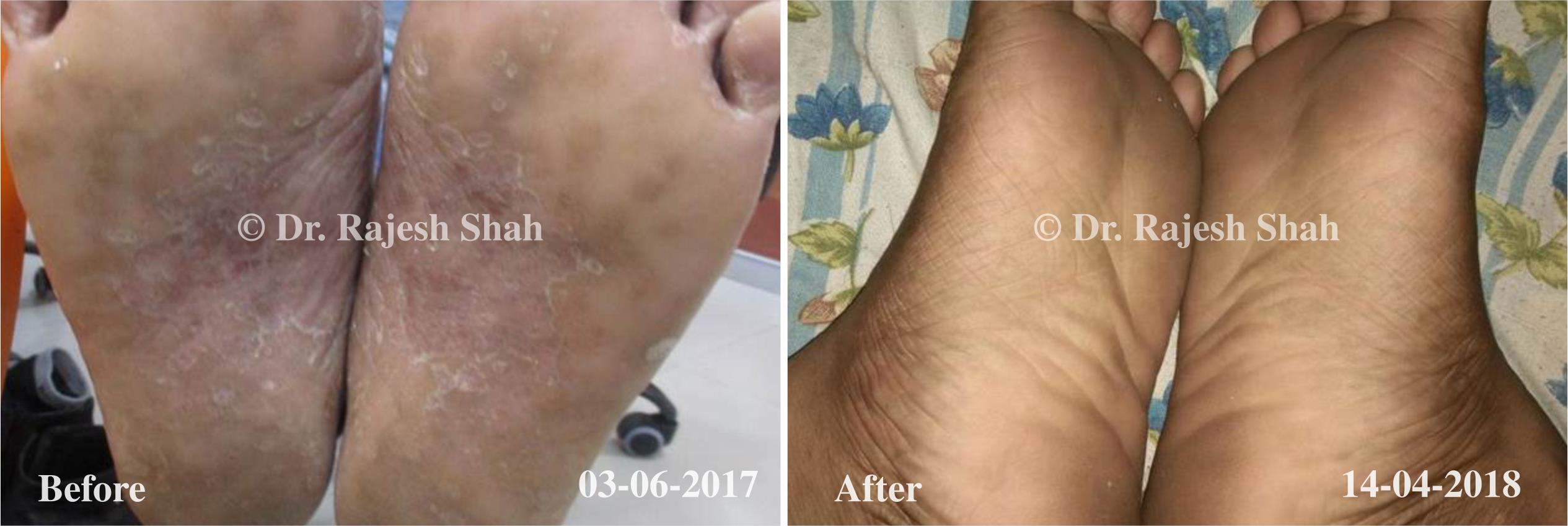
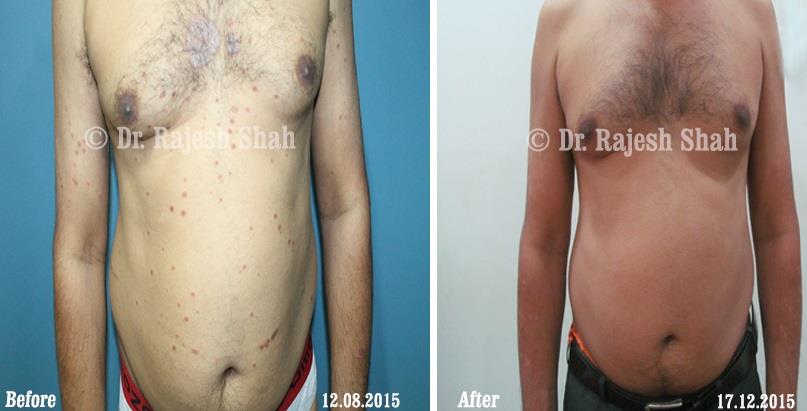
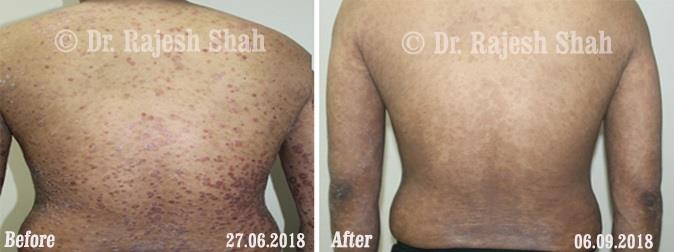
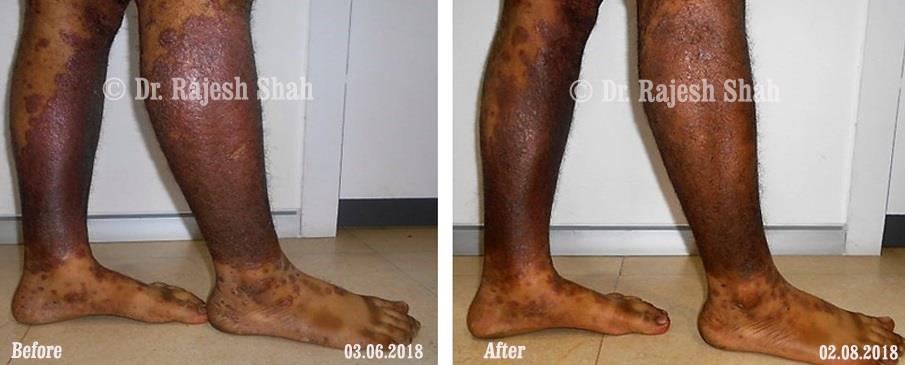
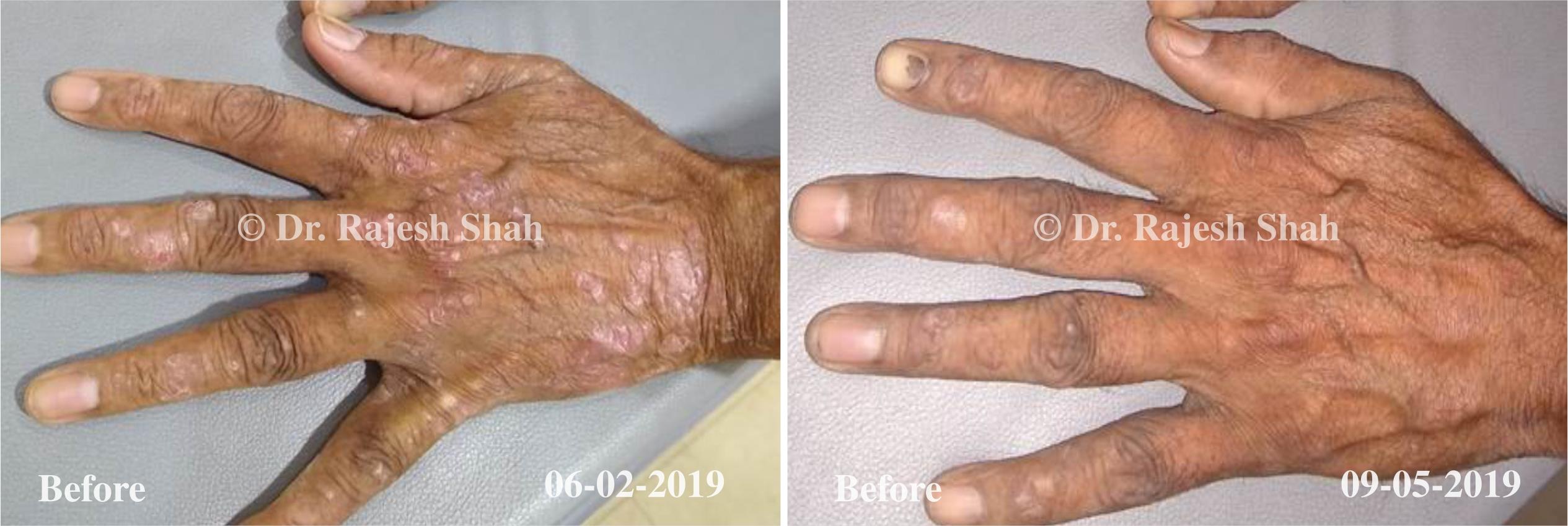
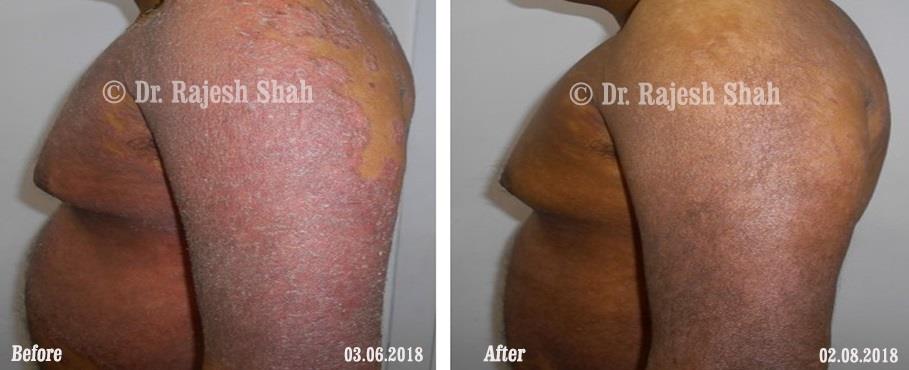
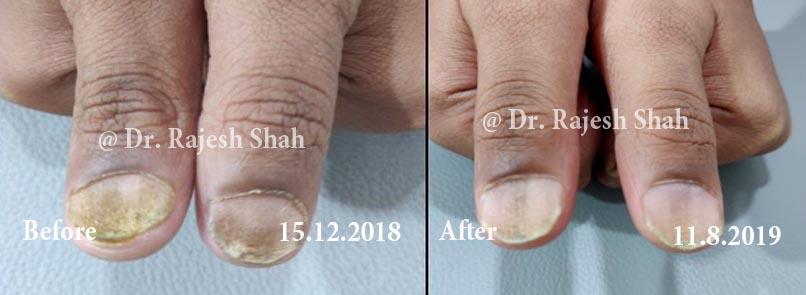
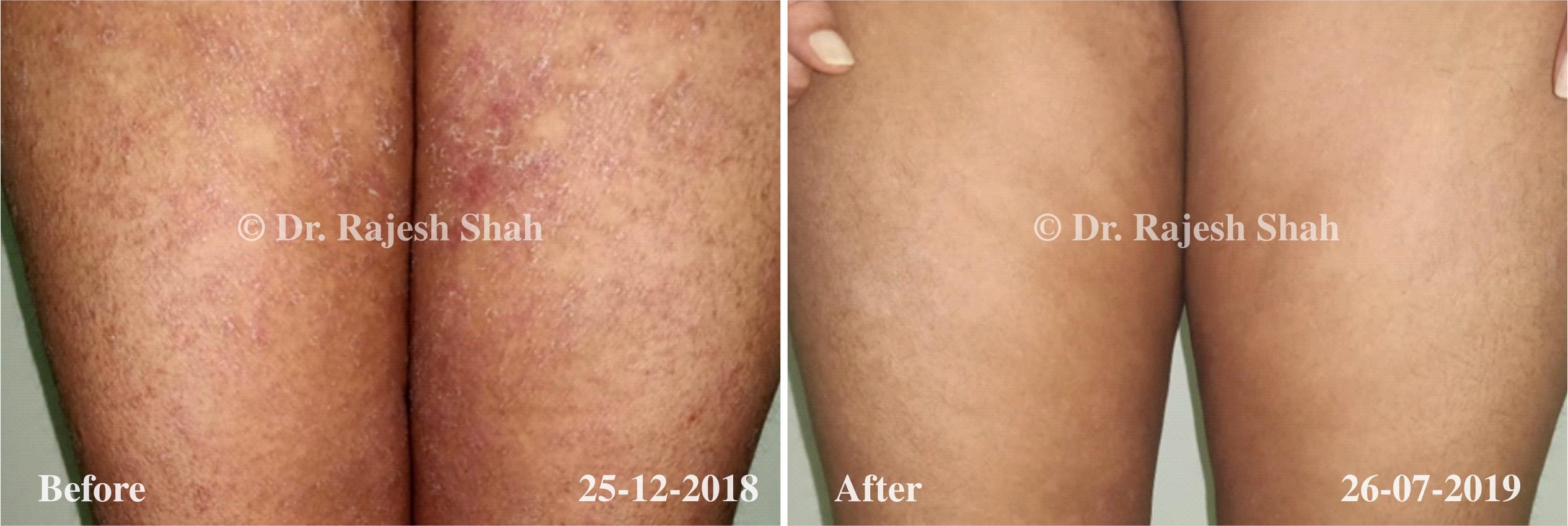
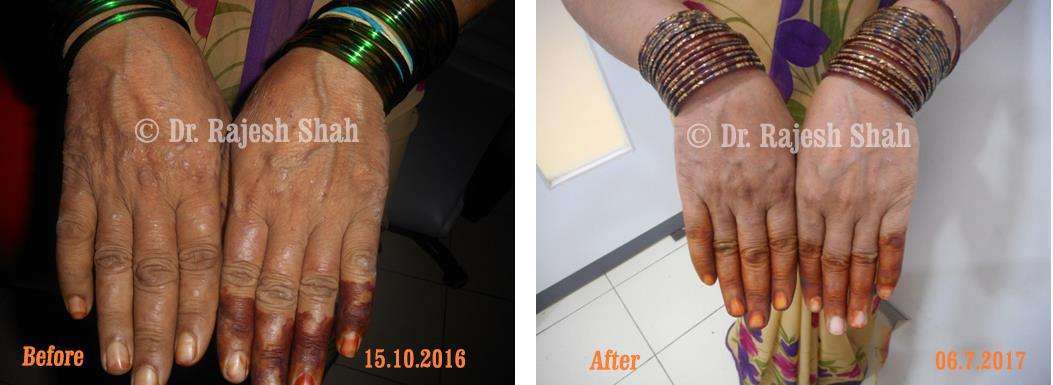
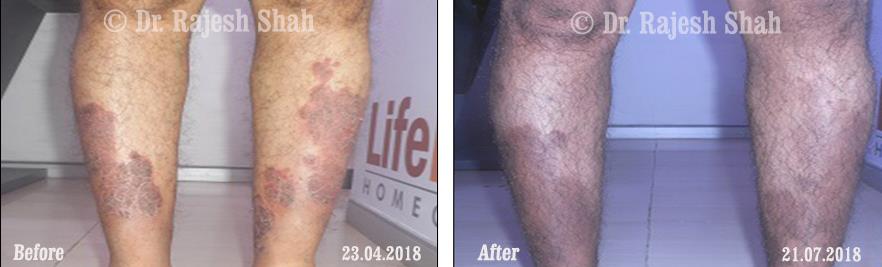
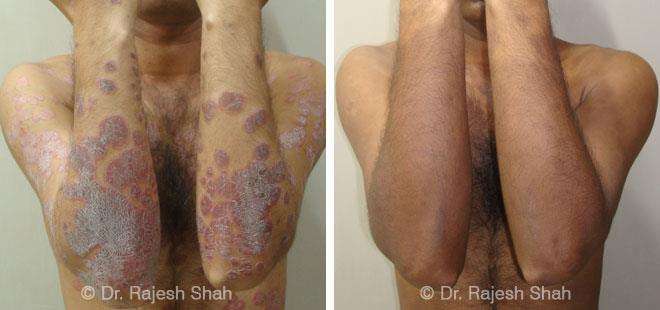
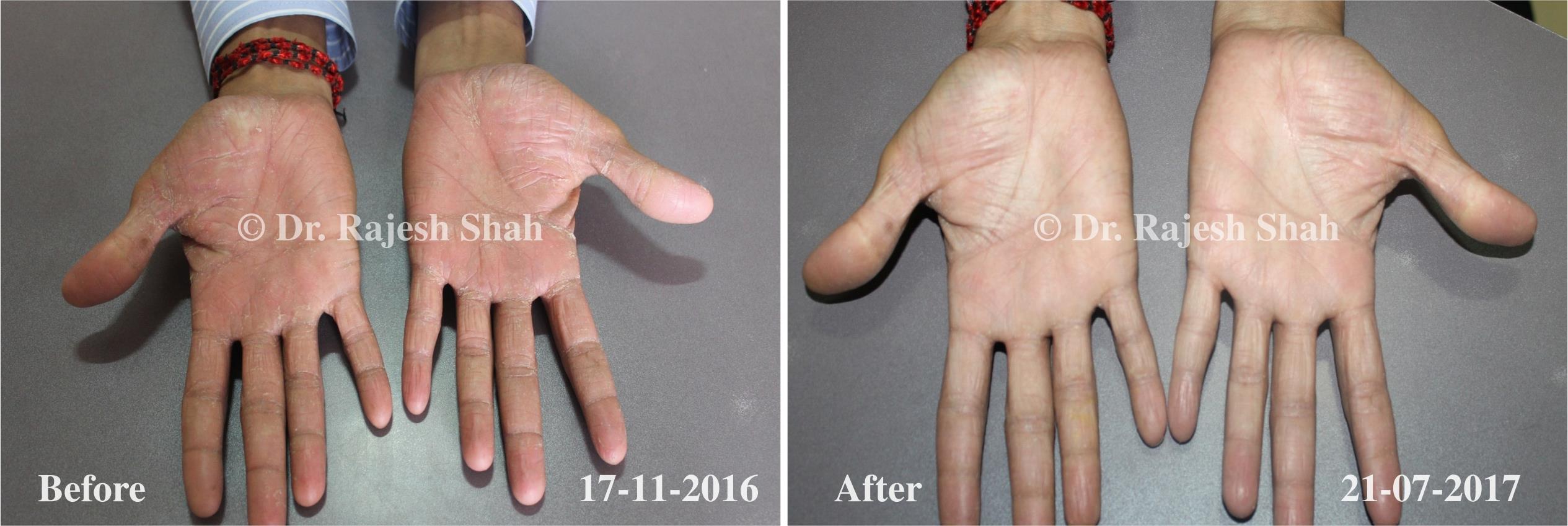
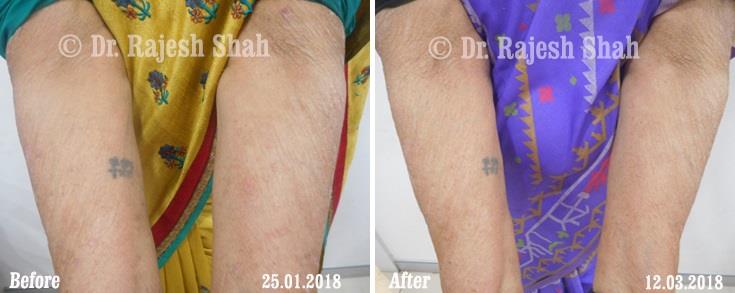
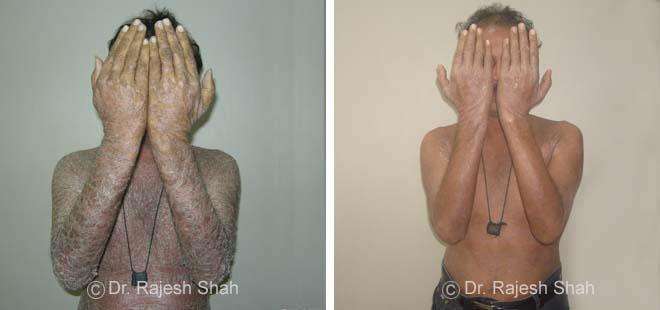
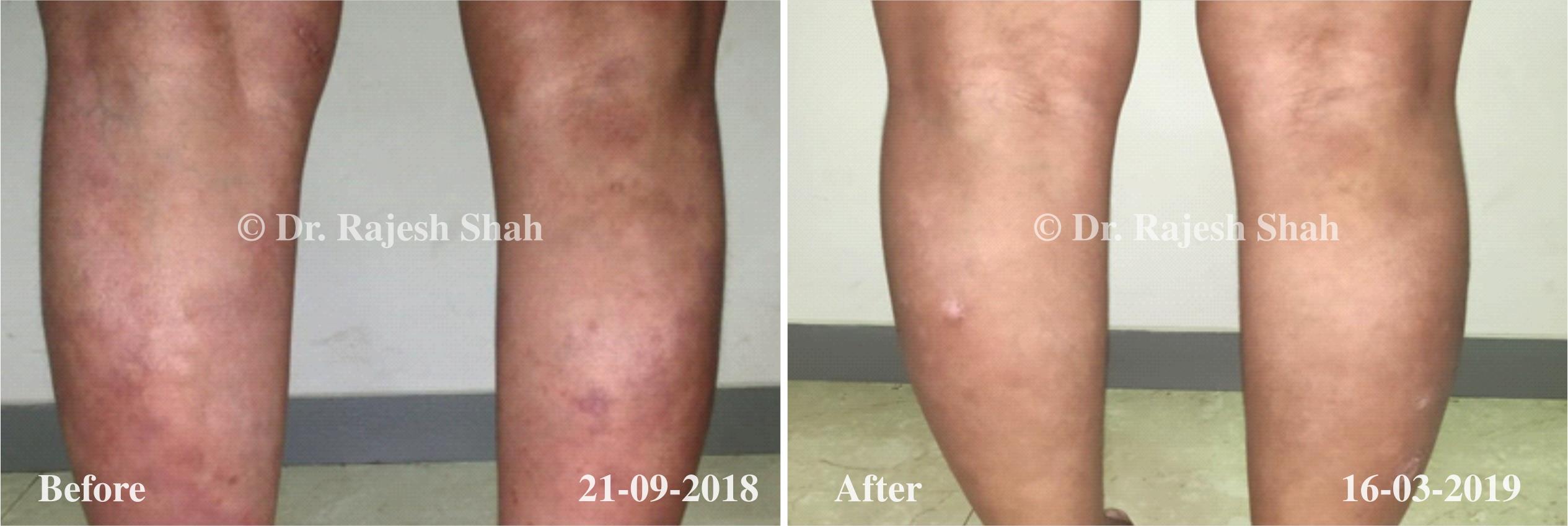
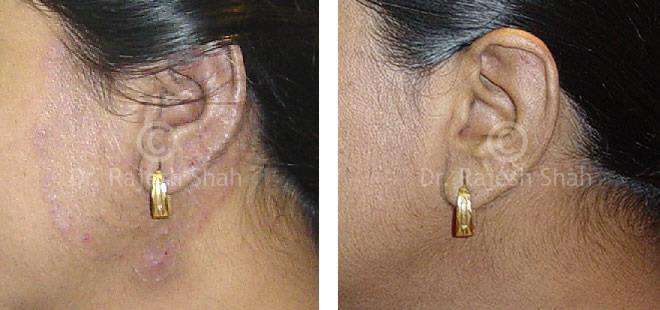
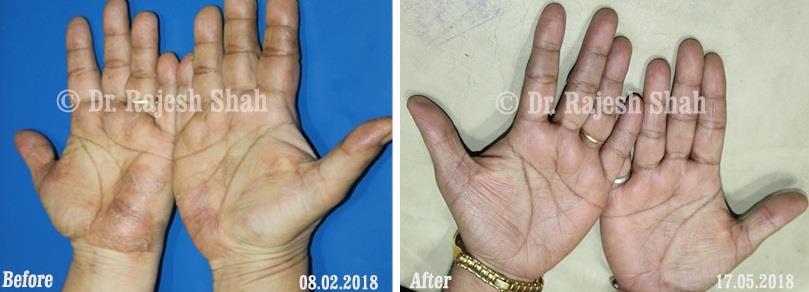
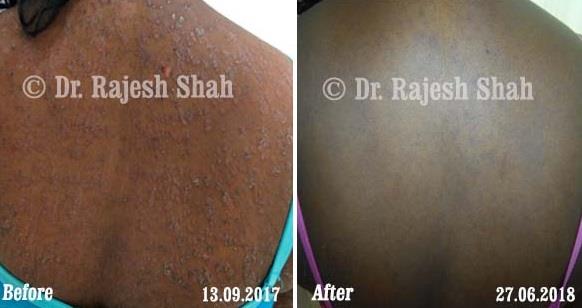
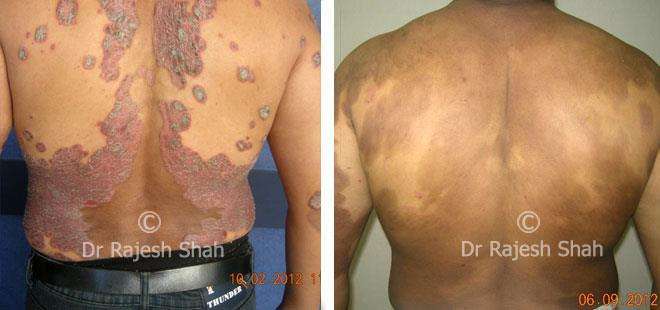
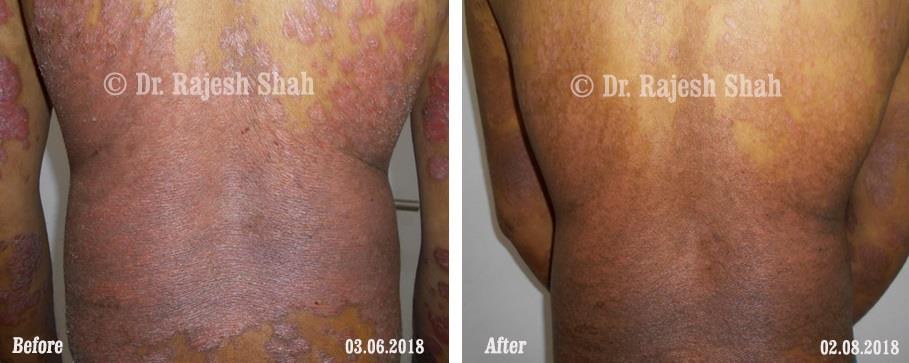
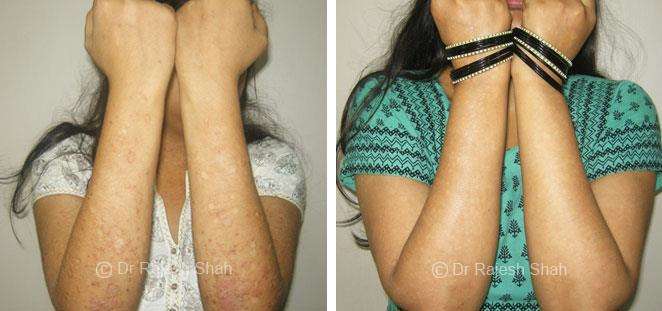
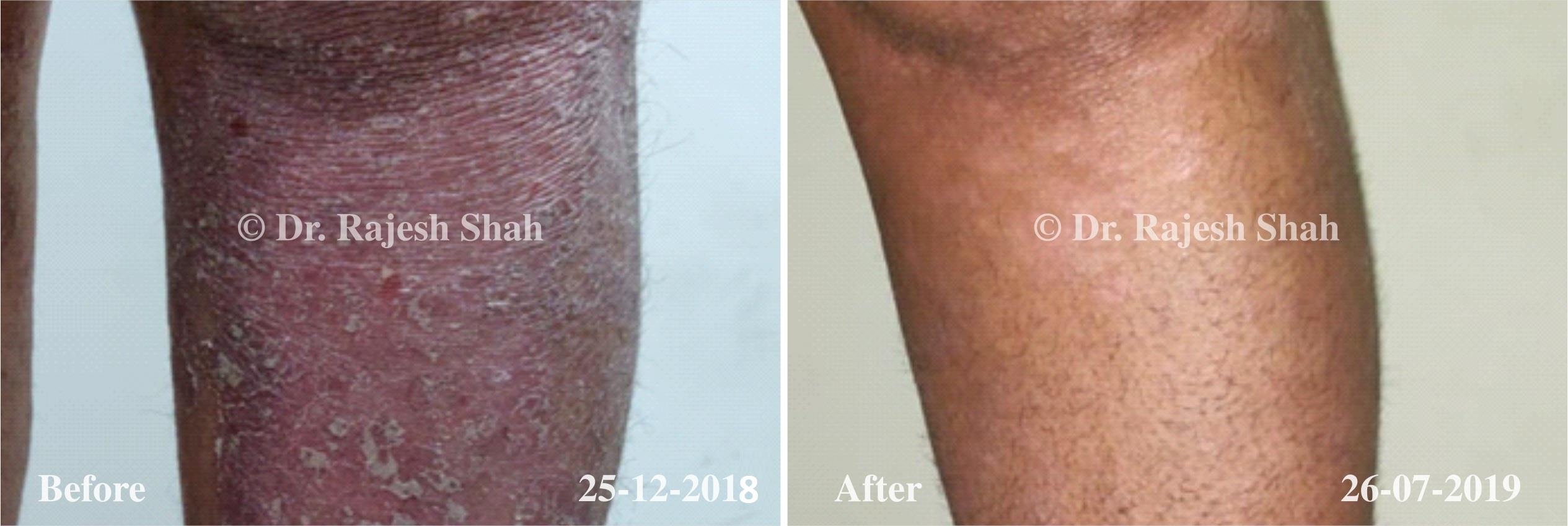
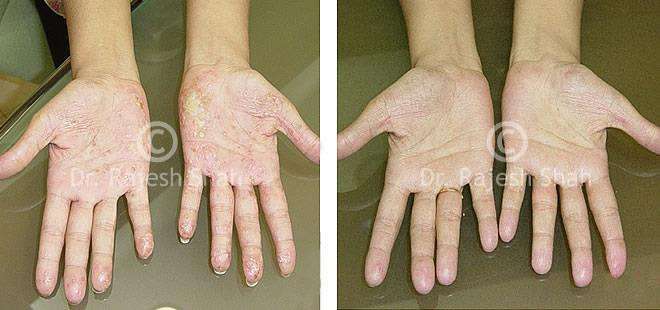
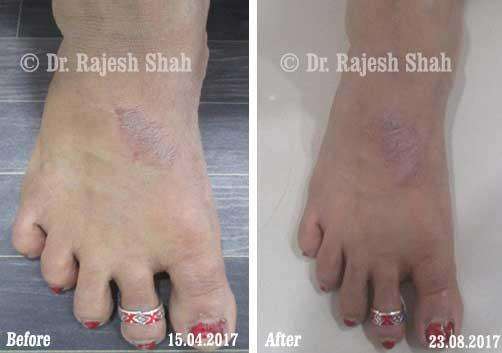
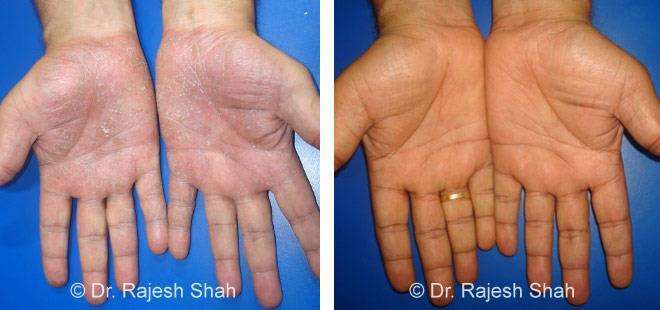
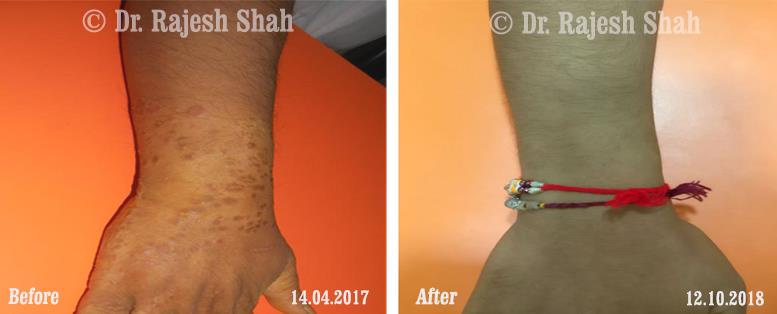
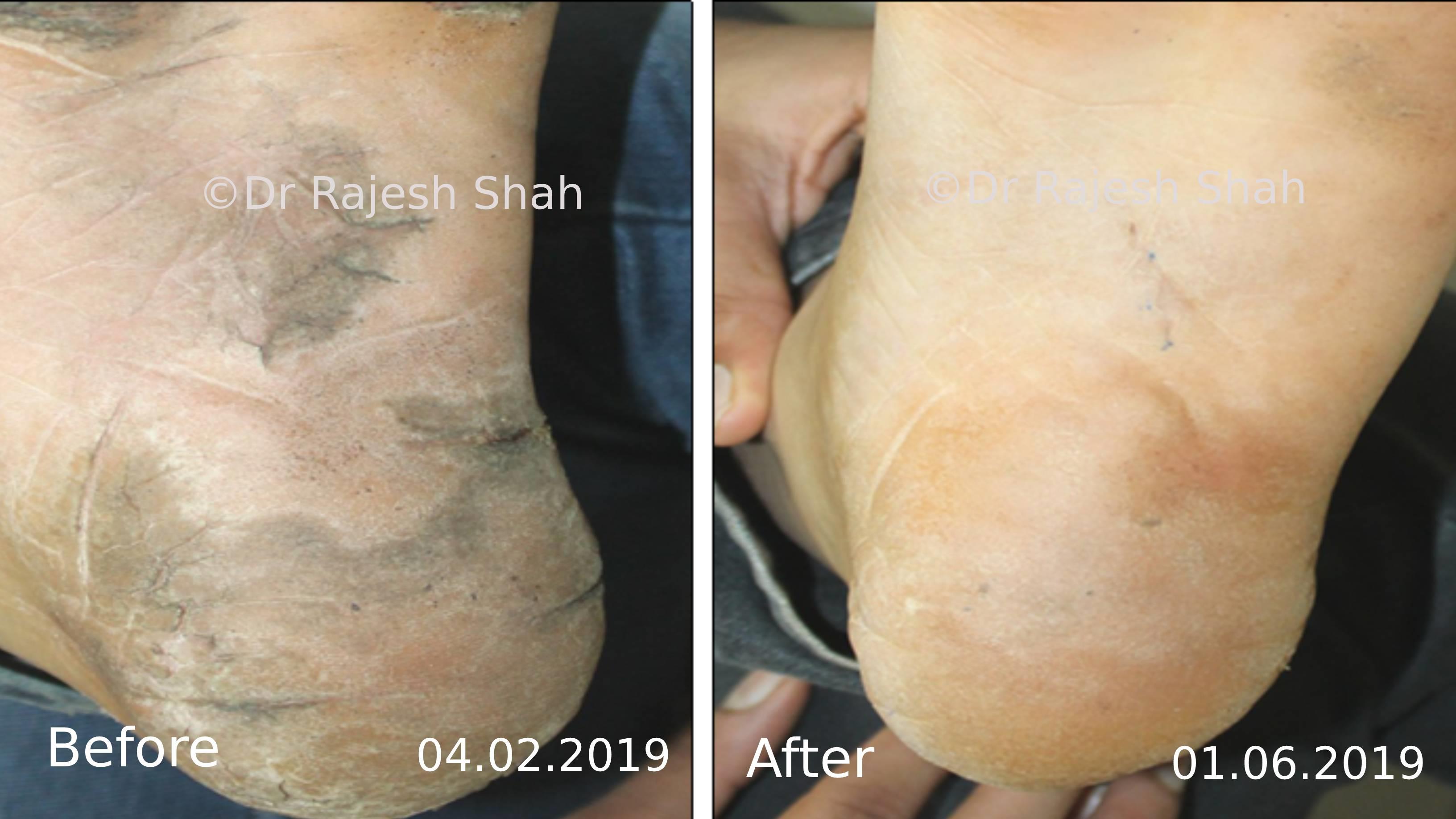
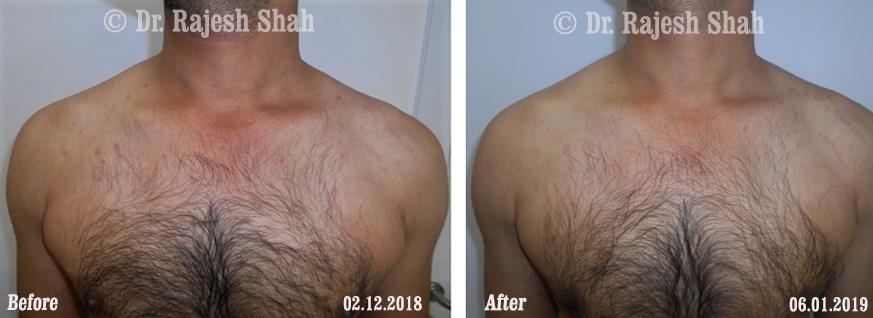
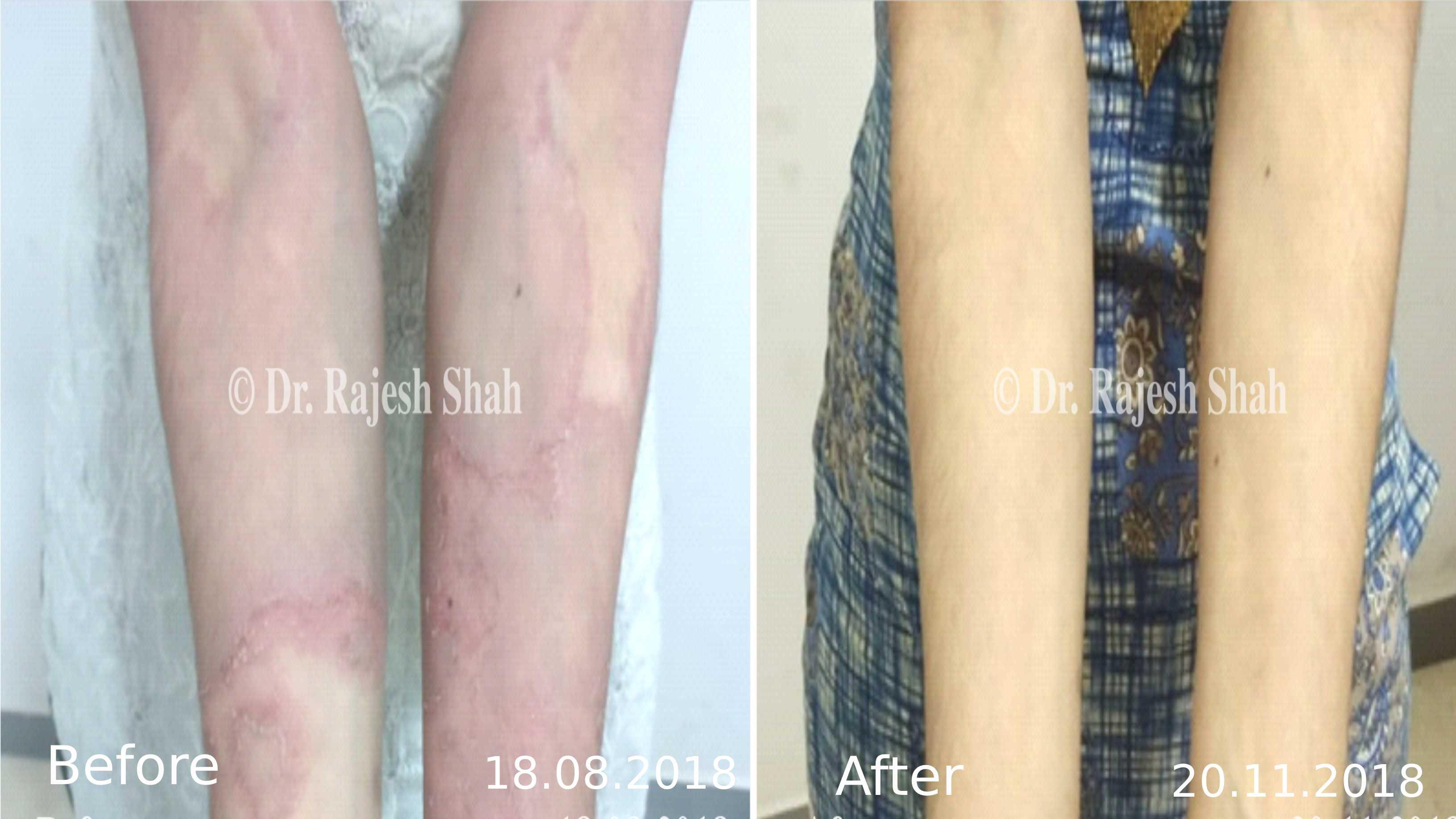
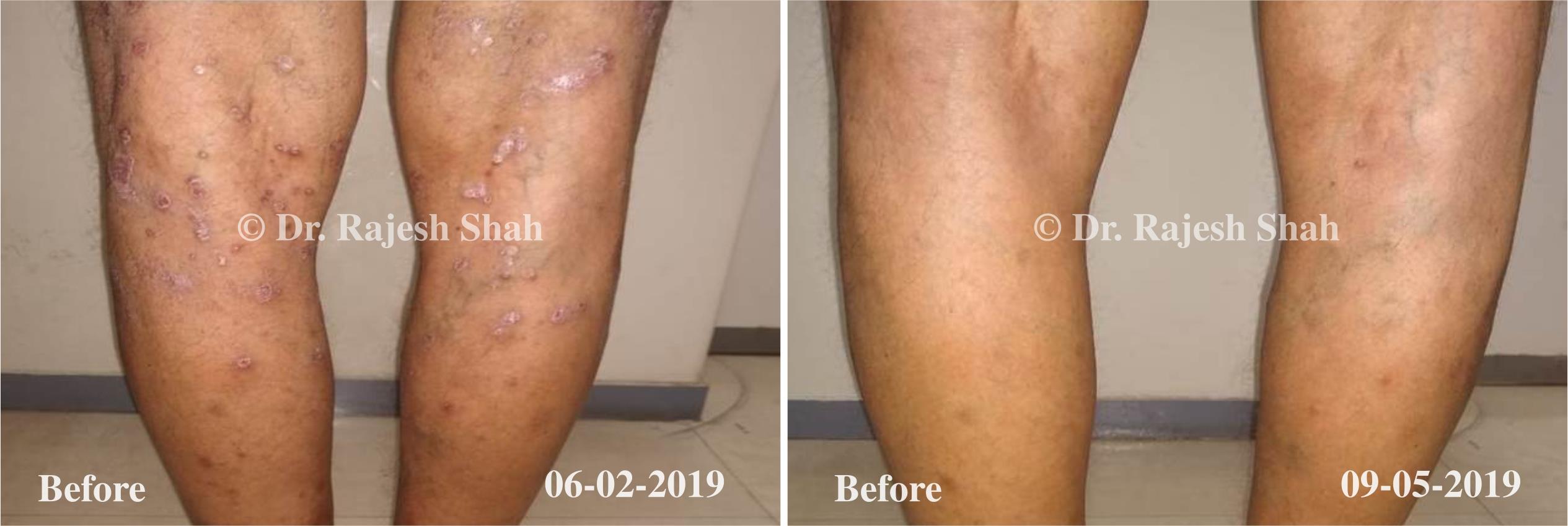
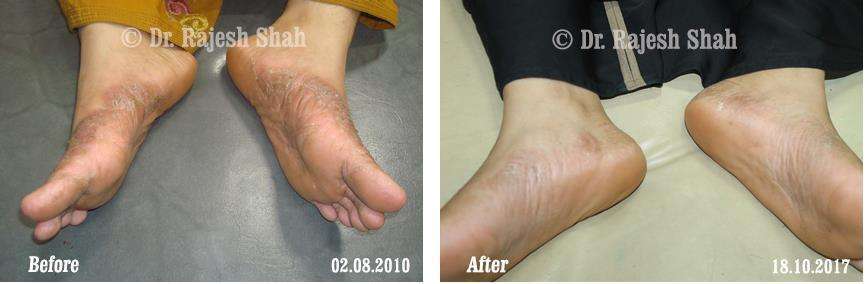
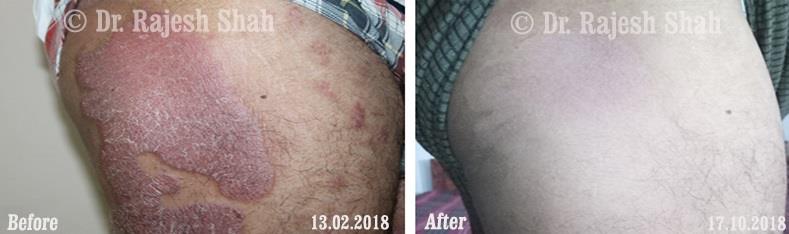
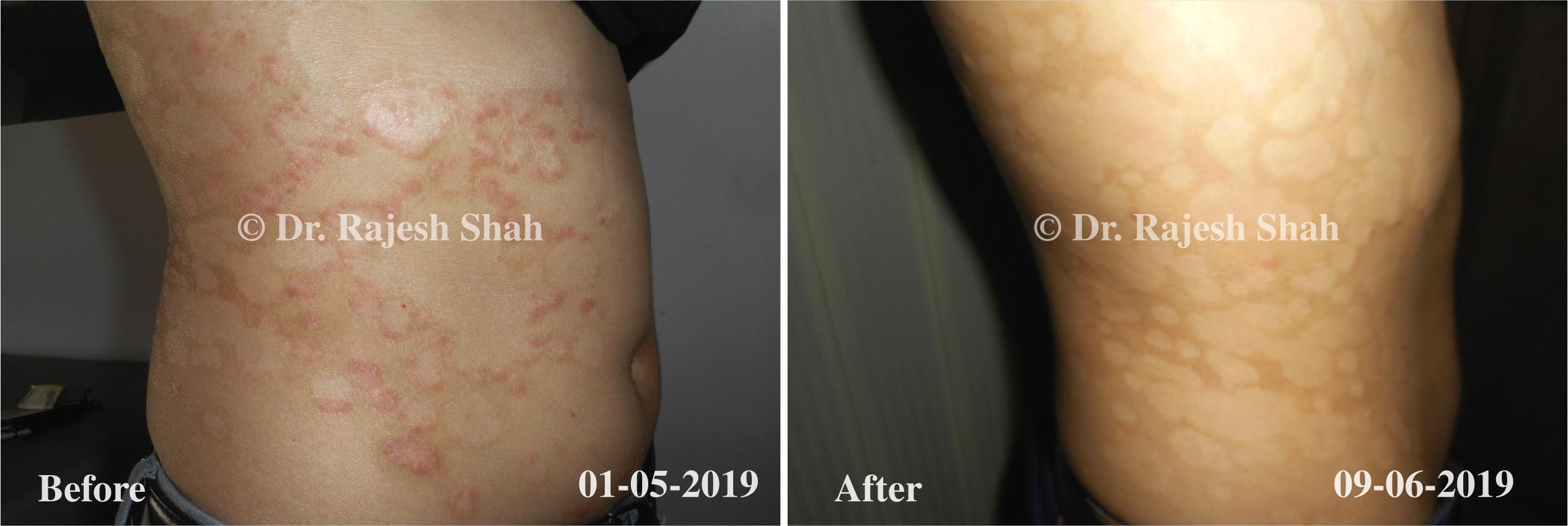
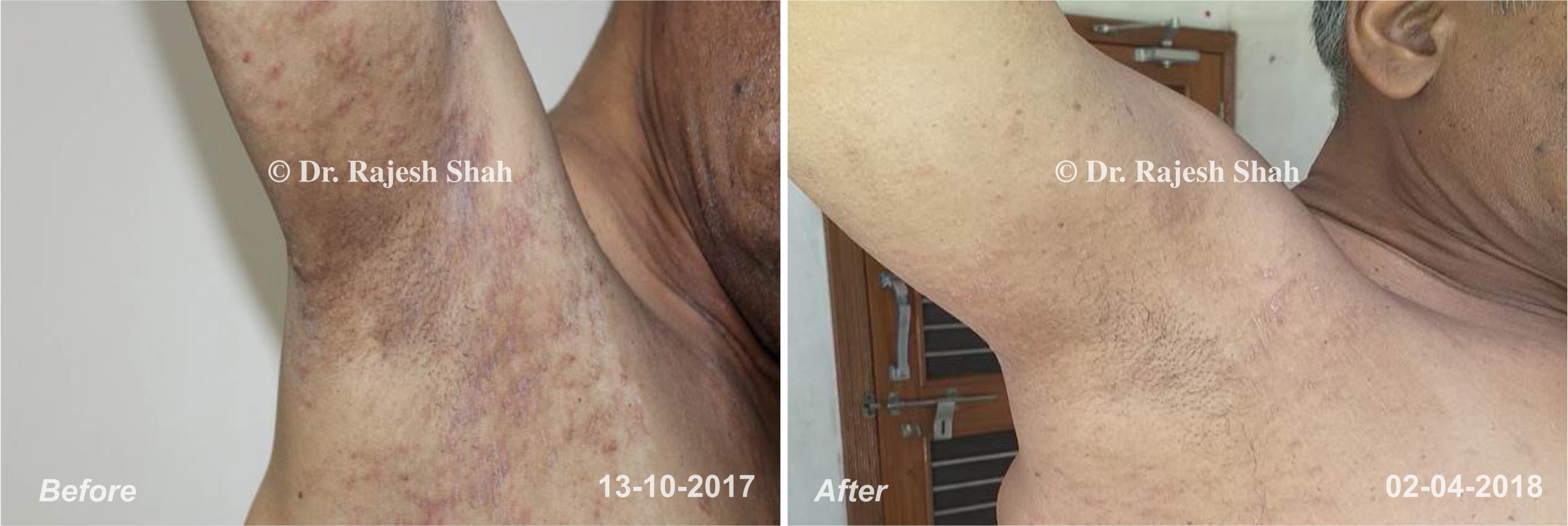
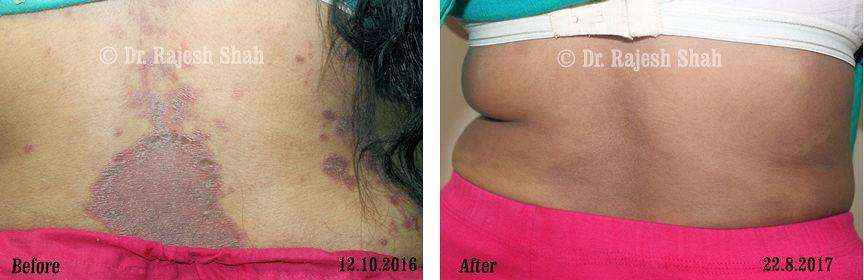
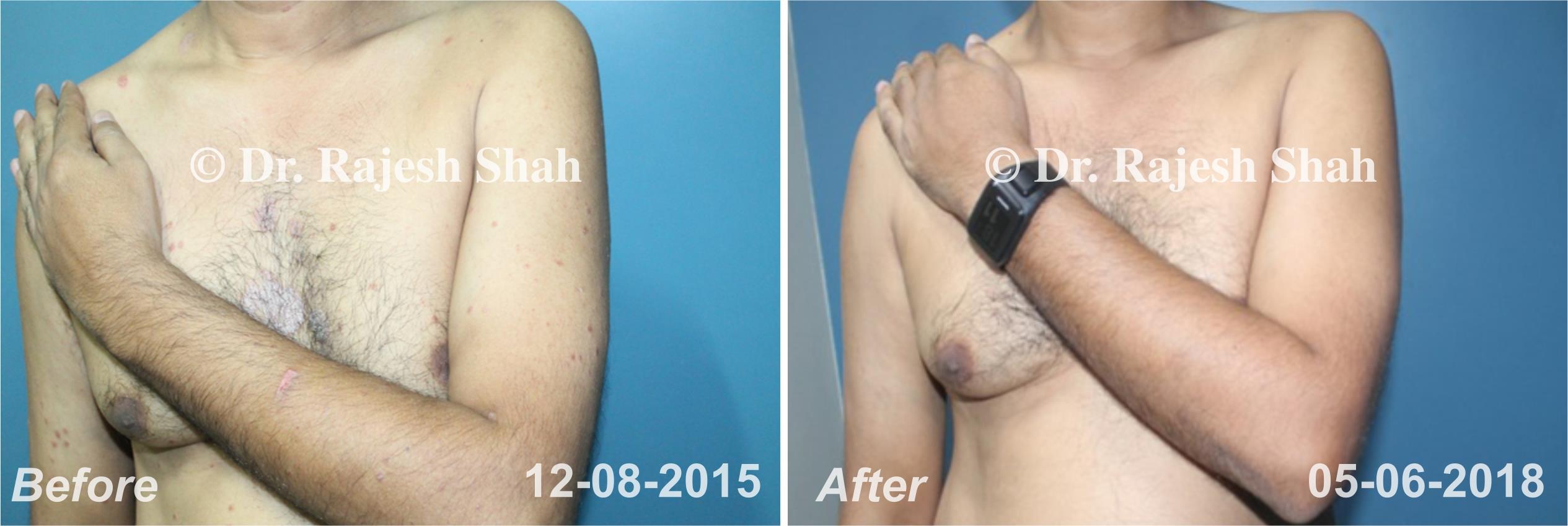
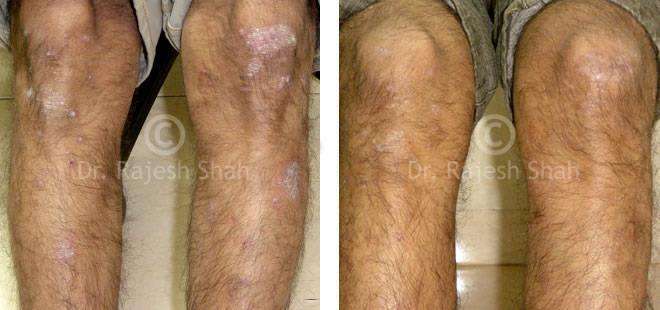
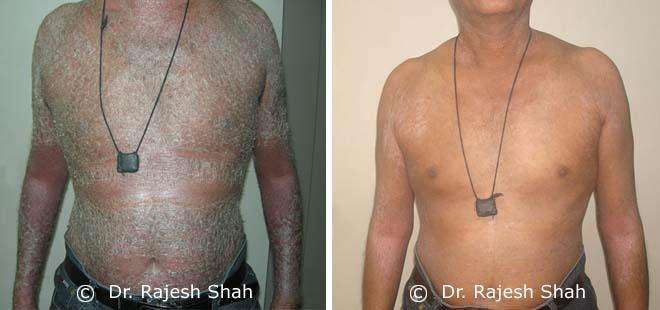
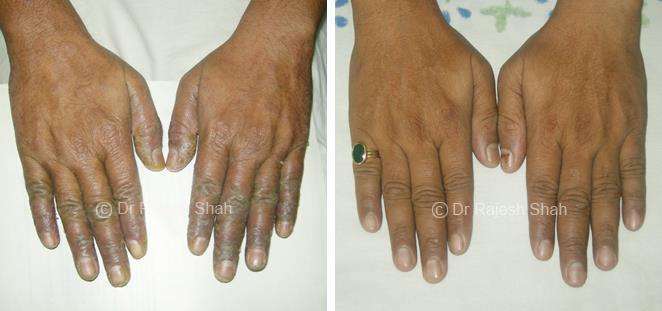
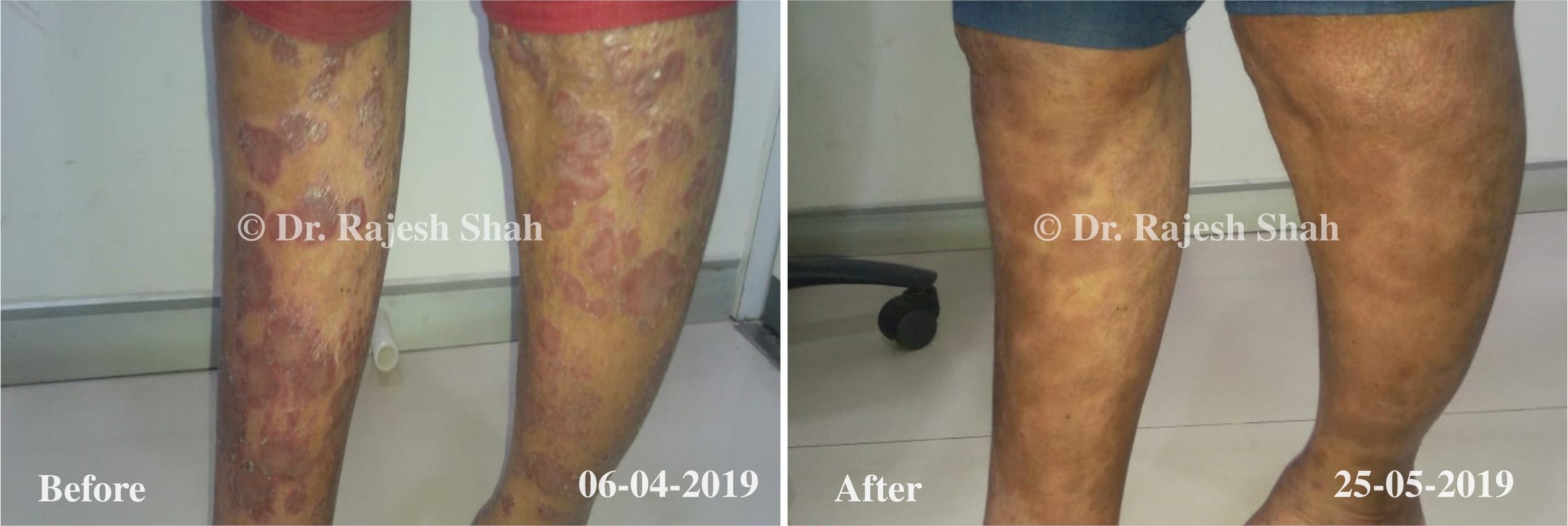
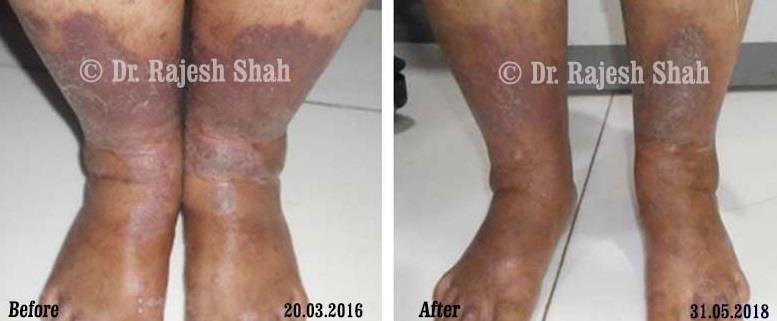
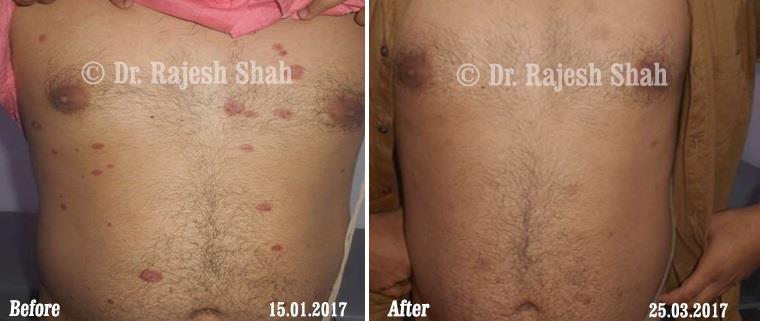
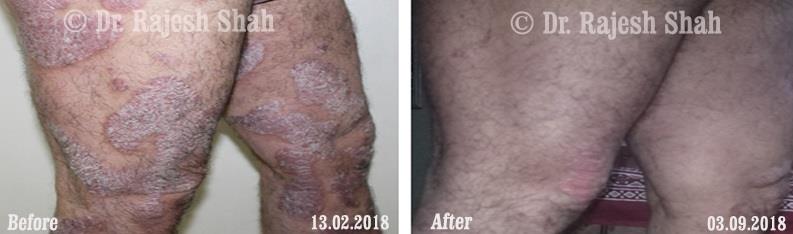
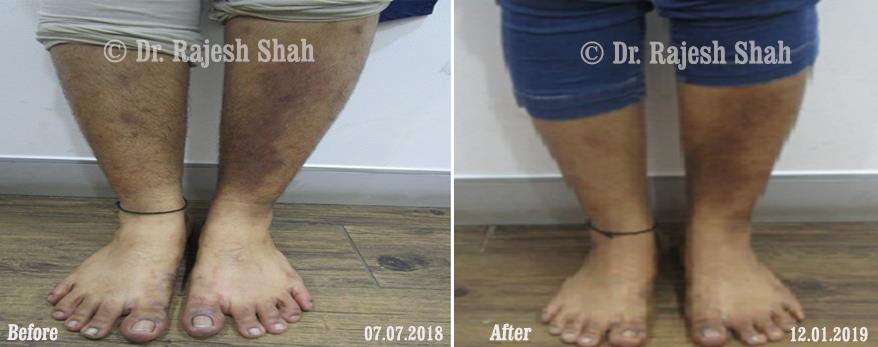
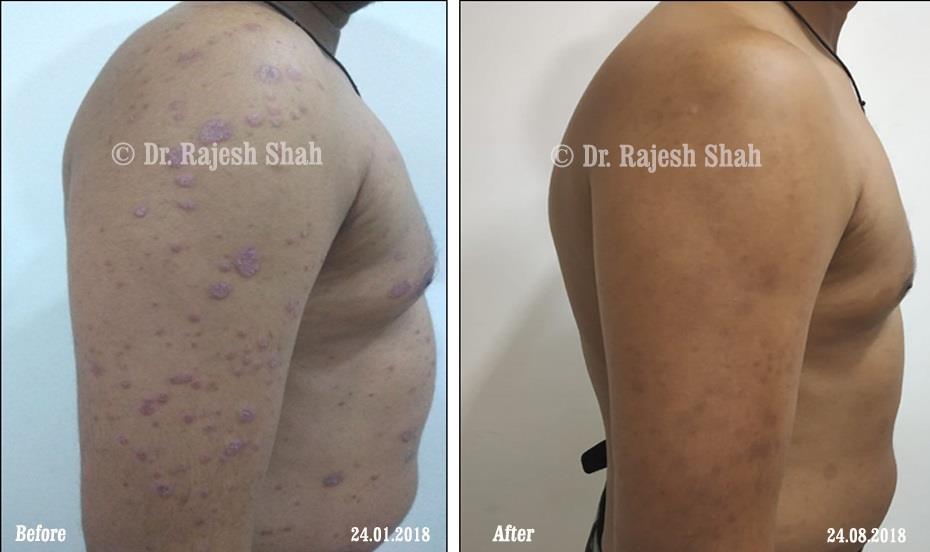
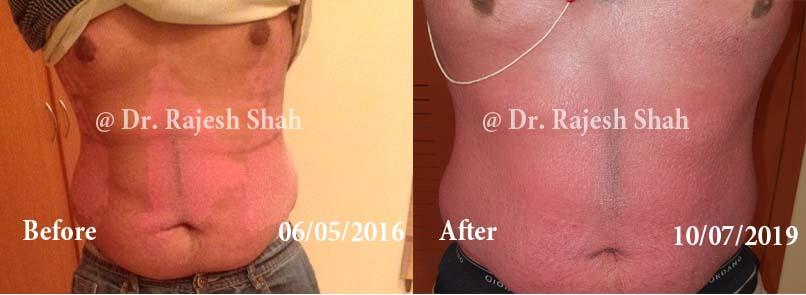
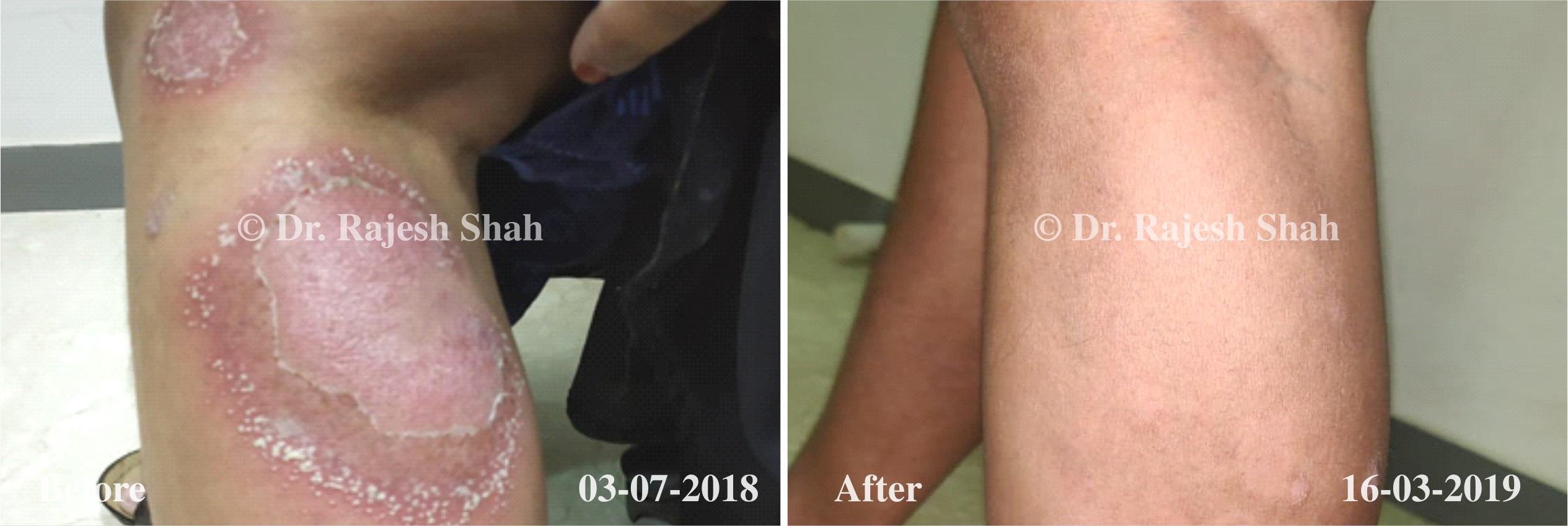
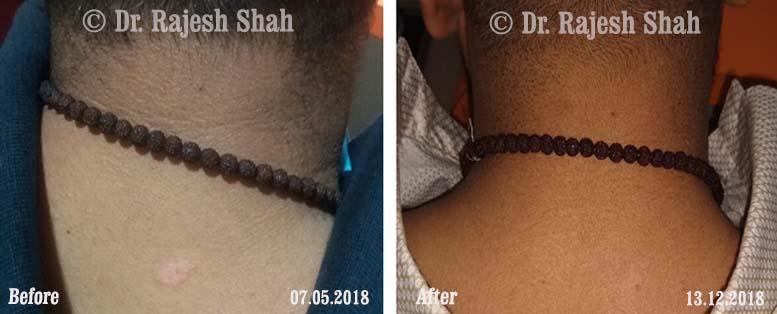
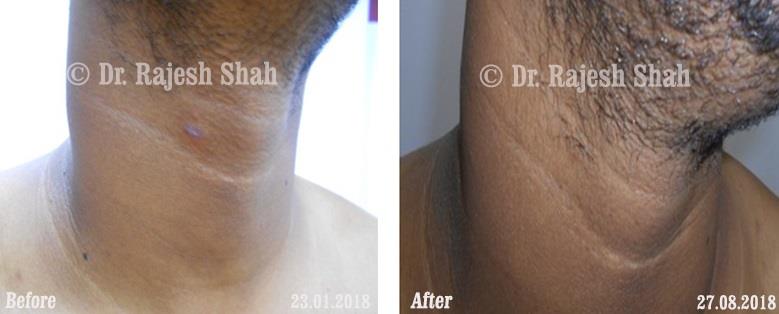
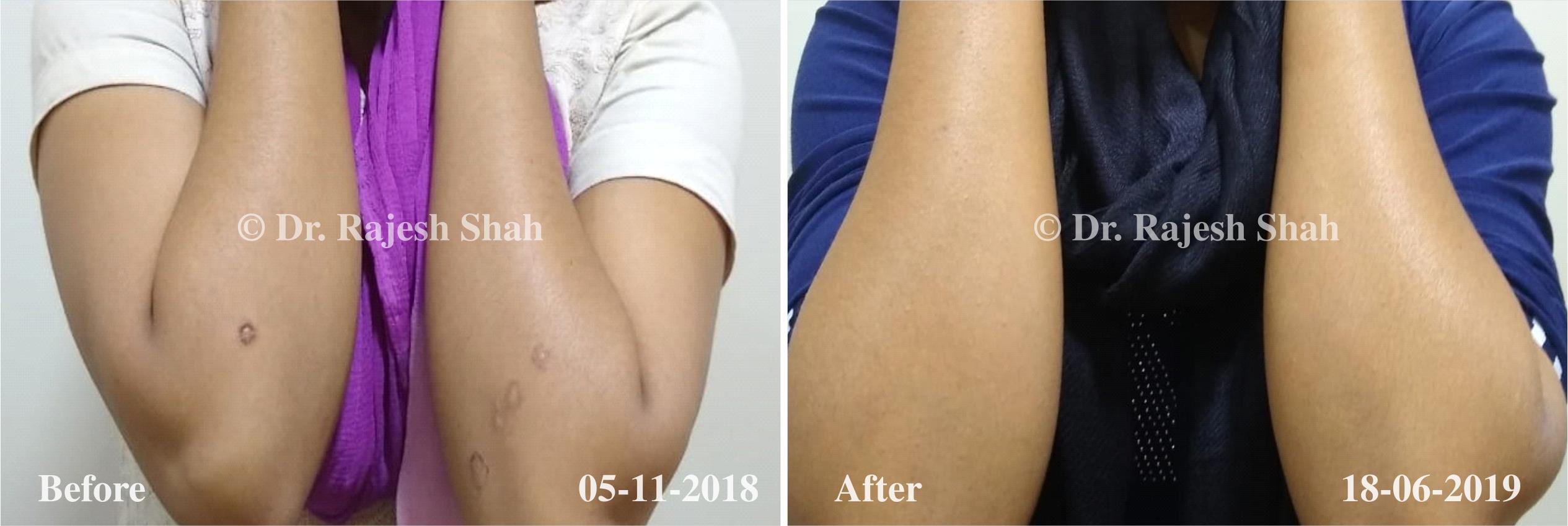
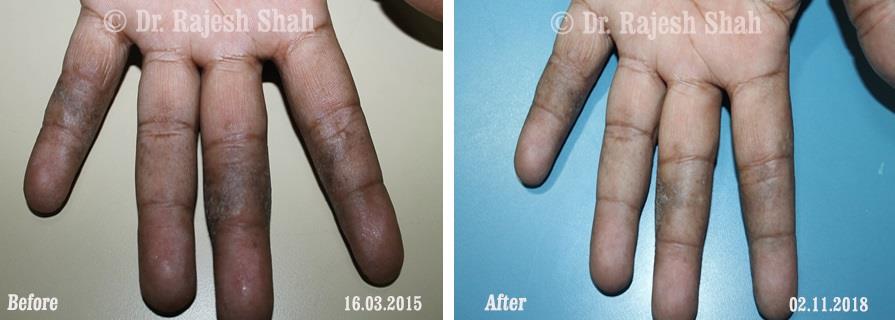
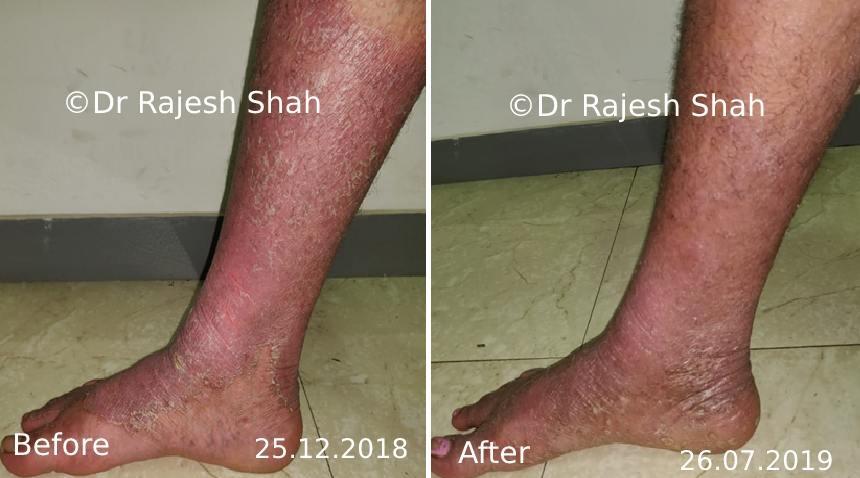
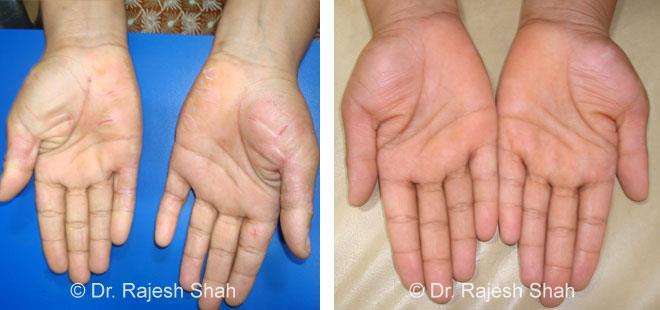
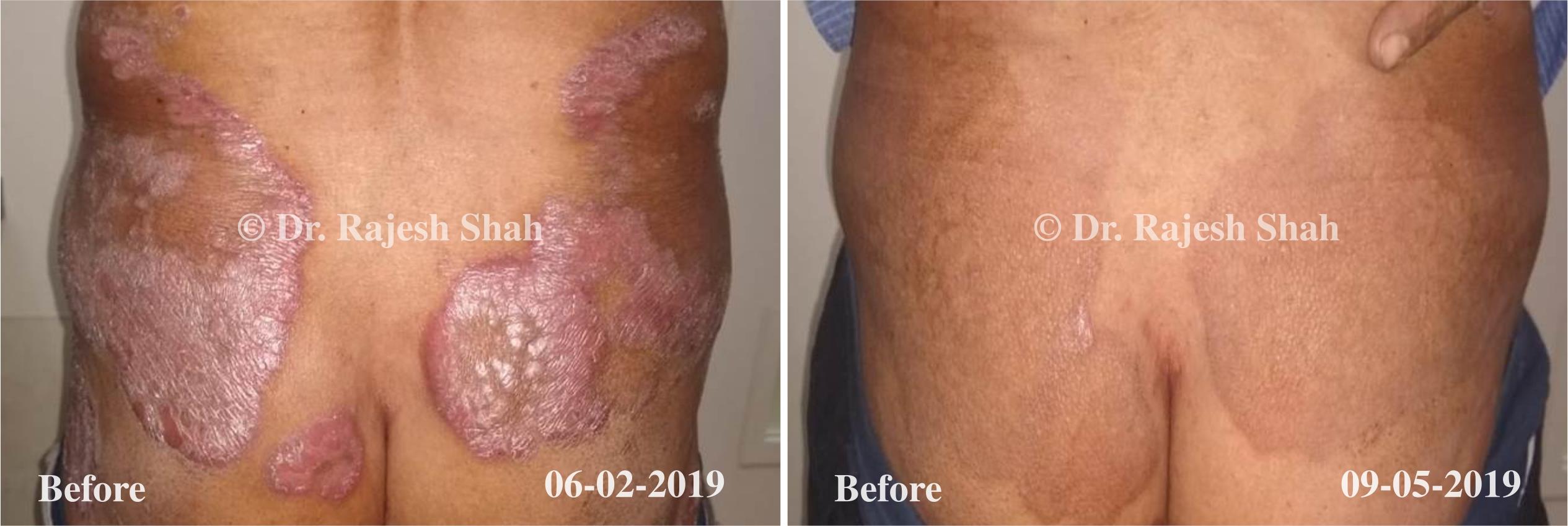
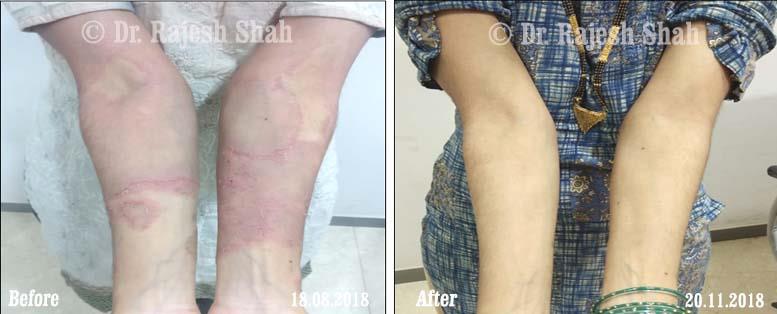
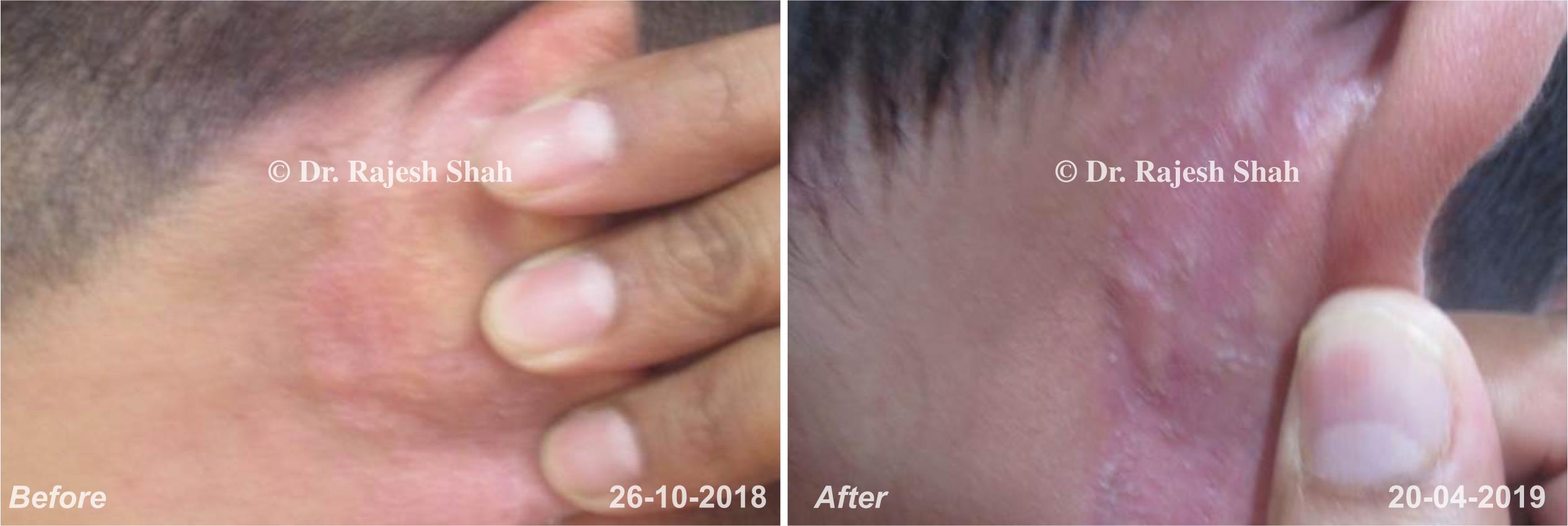
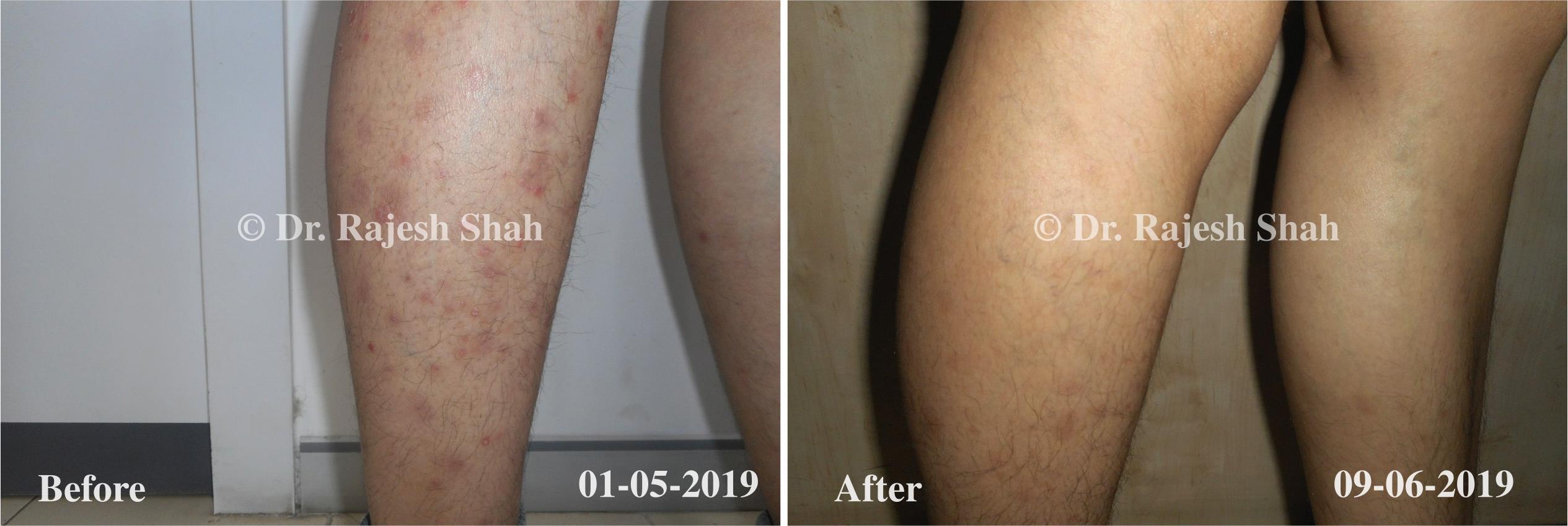
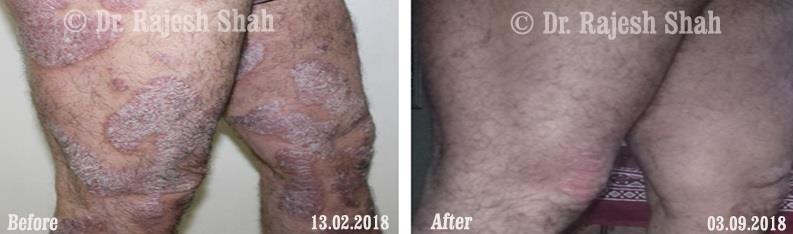
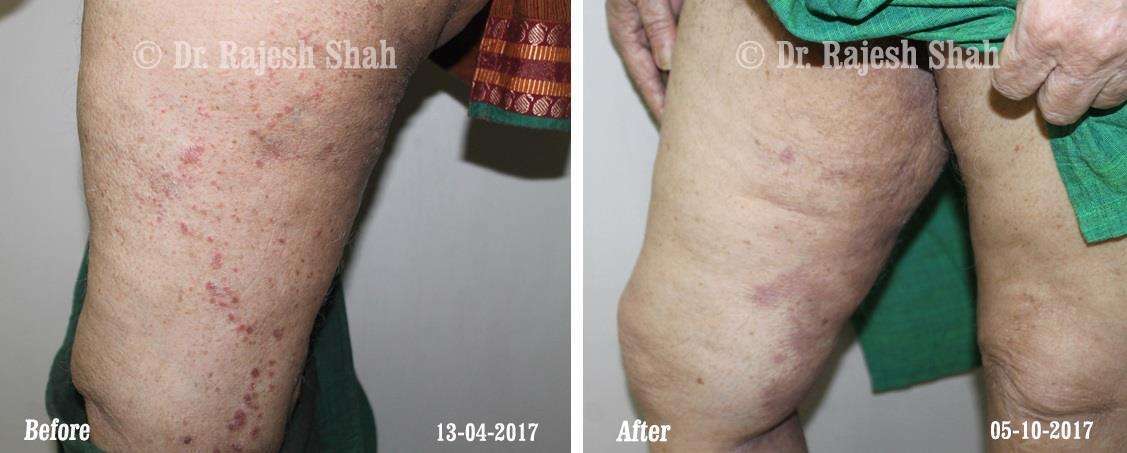
Dr. Rajesh Shah brings over 40 years of focused clinical experience in managing psoriasis at Life Force Homeopathy. With more than 8,000 psoriasis cases treated and documented, many patients have achieved sustained remission, though outcomes naturally vary. Based on our clinical data, approximately 60–70% of cases show significant improvement, while around 10–15% may not respond as desired. We do not claim to cure every case.
-
Over decades of practice, Dr. Shah has developed a research-informed approach that emphasizes immune balance, a central aspect of psoriasis management. His methodology integrates scientific homeopathy with modern clinical understanding.
-
In our experience, psoriasis of recent onset tends to respond more favorably to homeopathy. Conversely, long-standing cases with extensive prior use of immunosuppressive drugs such as methotrexate may show a limited response.
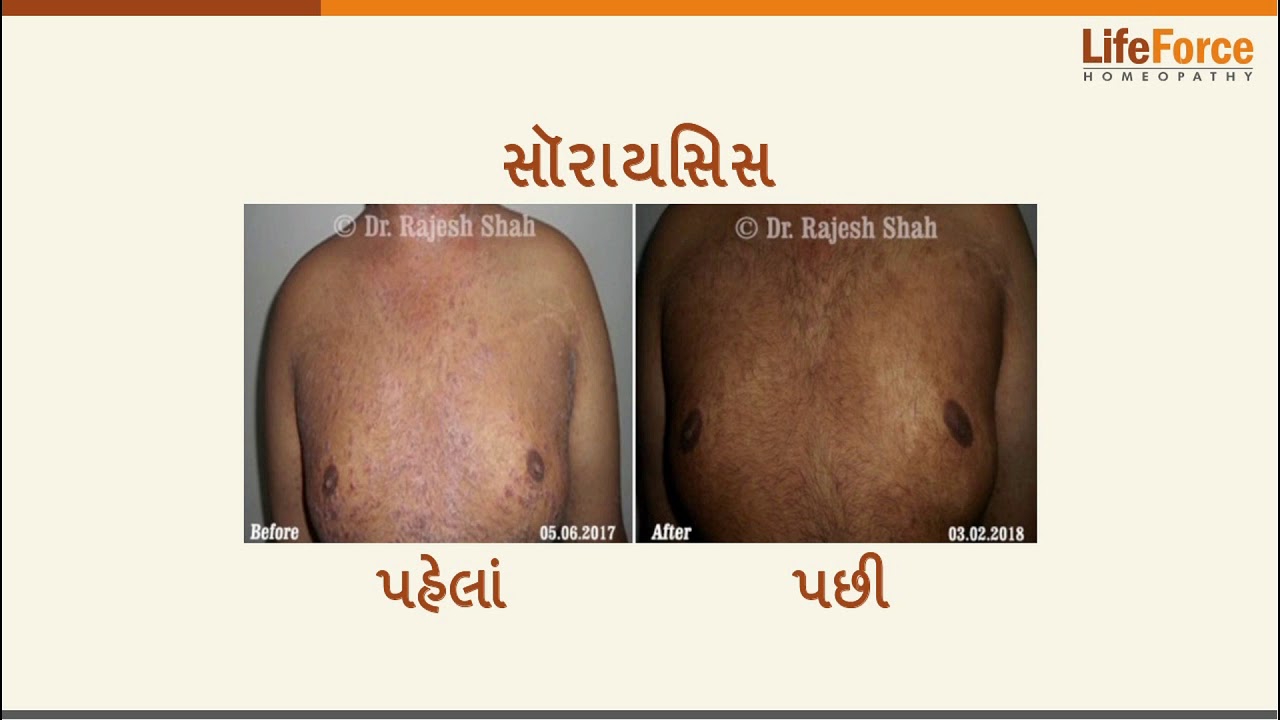
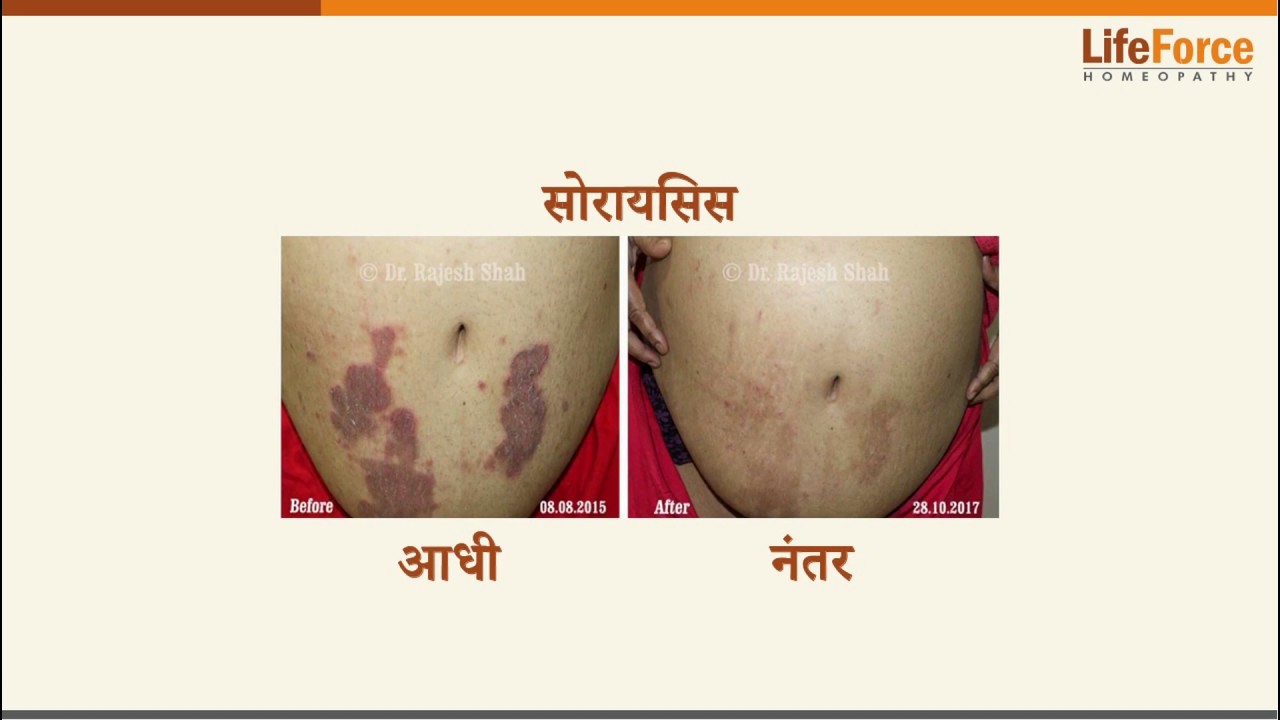
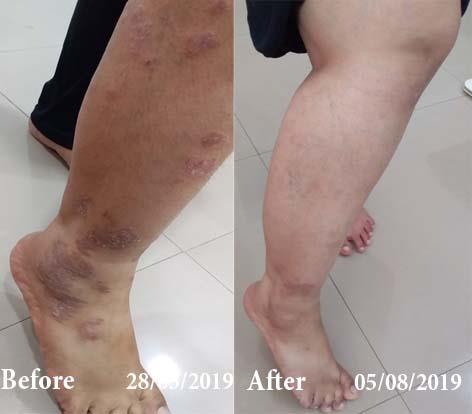
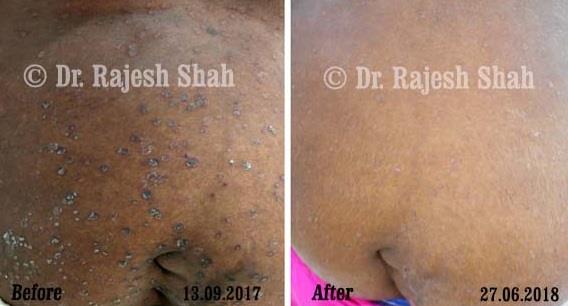
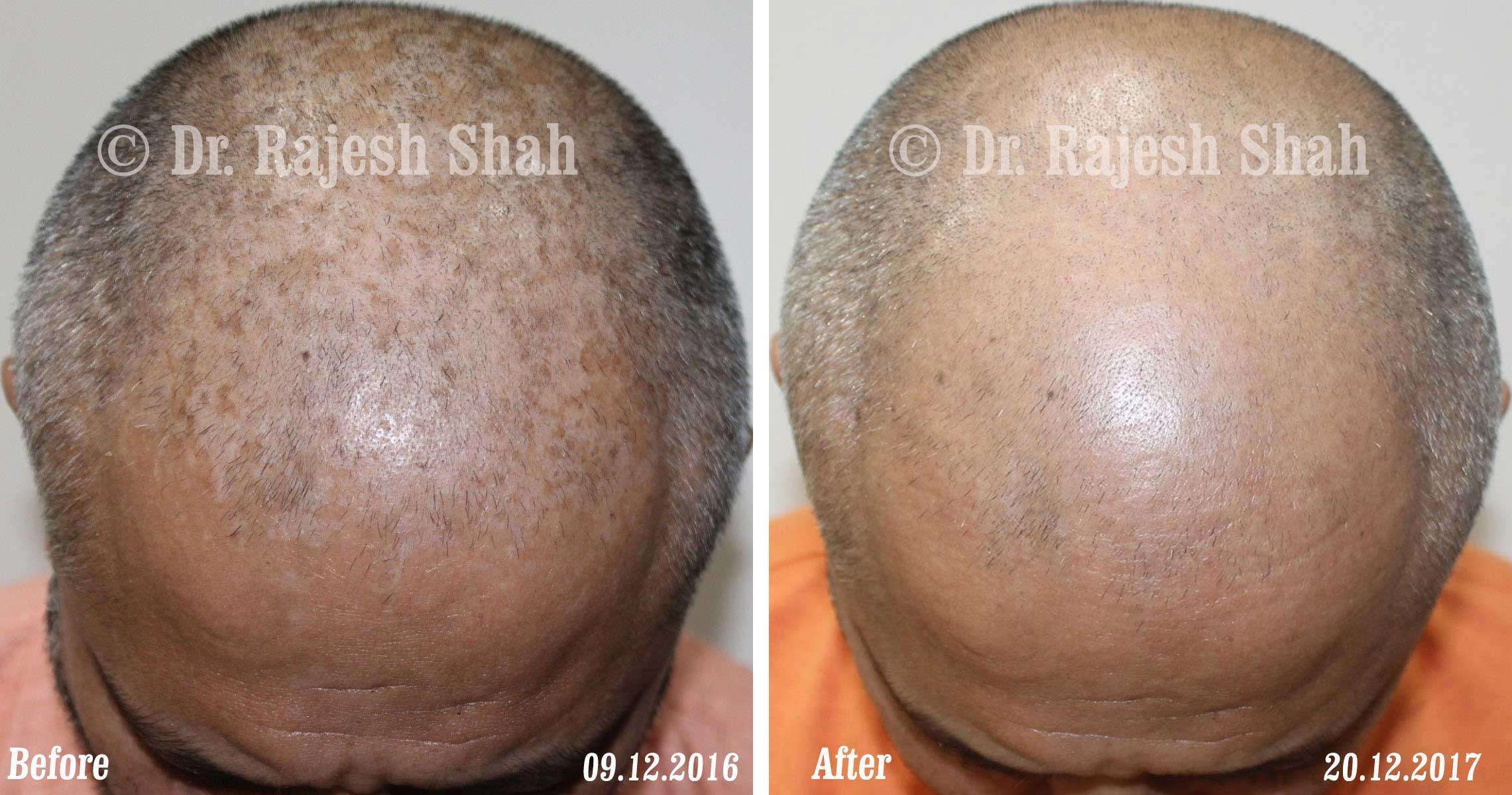
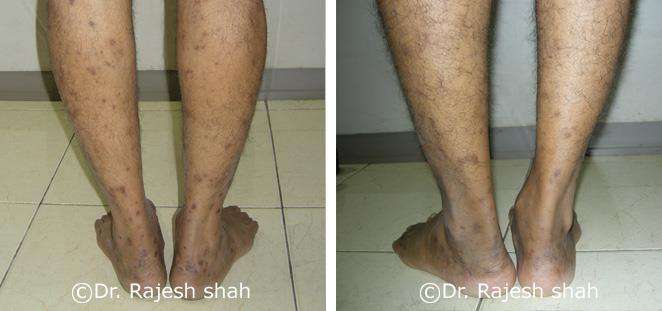
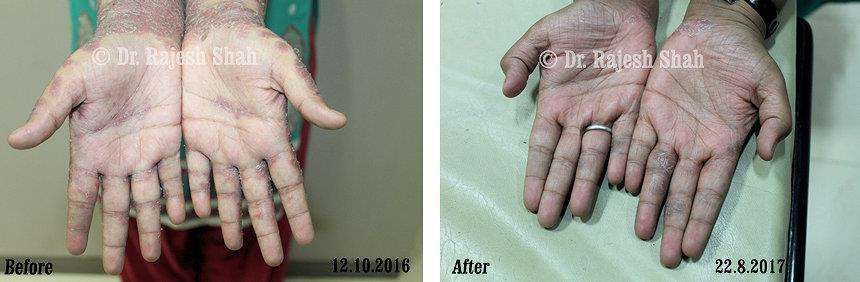
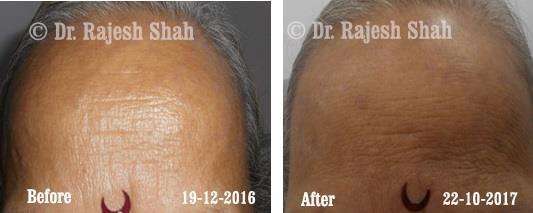
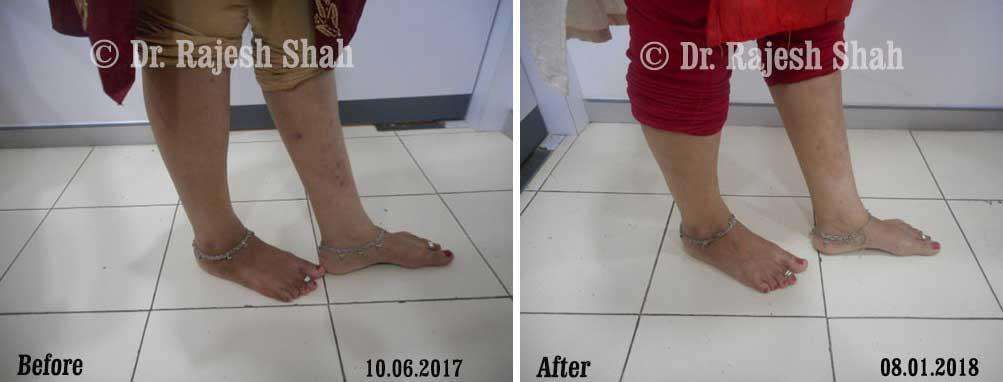
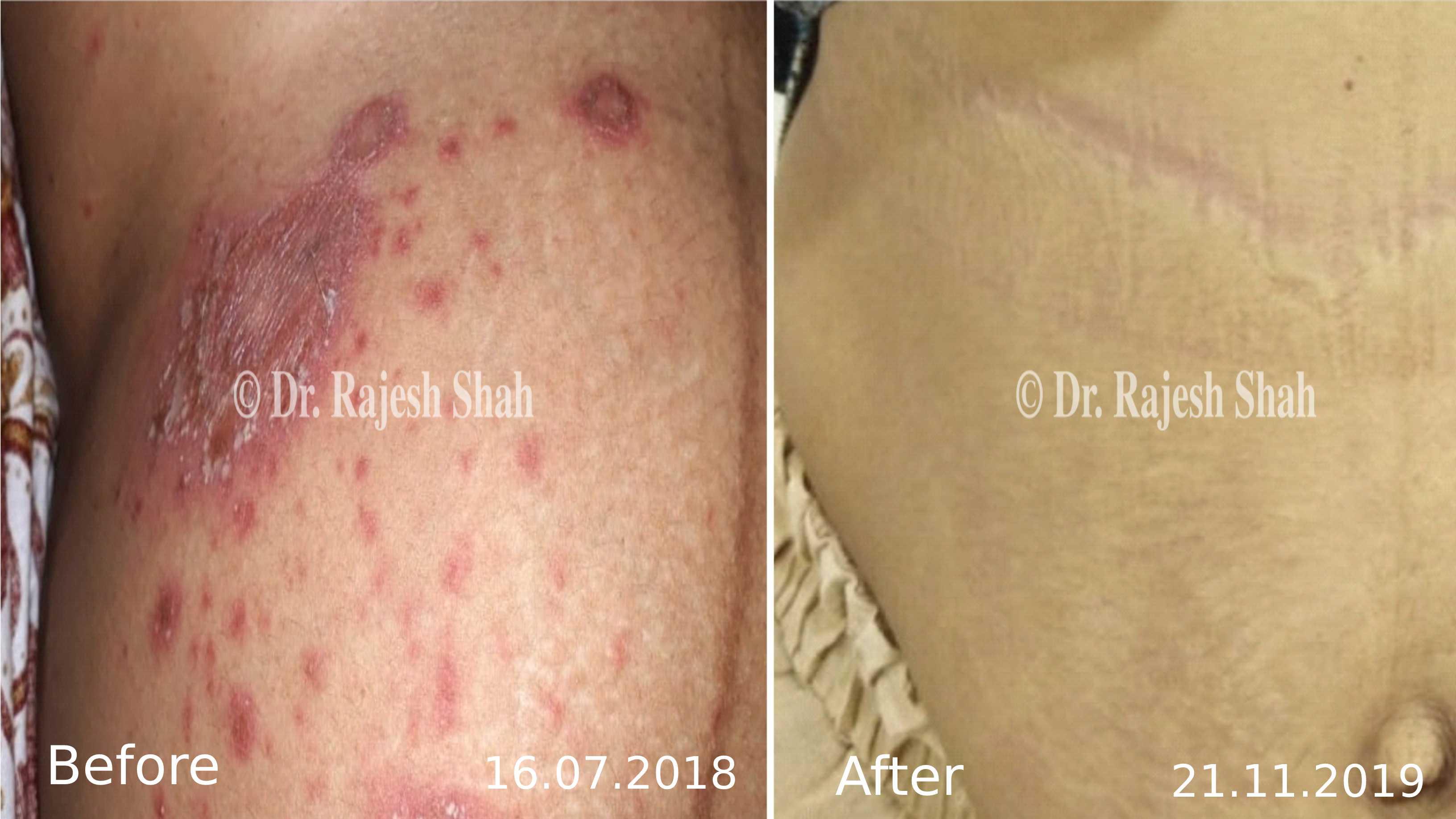
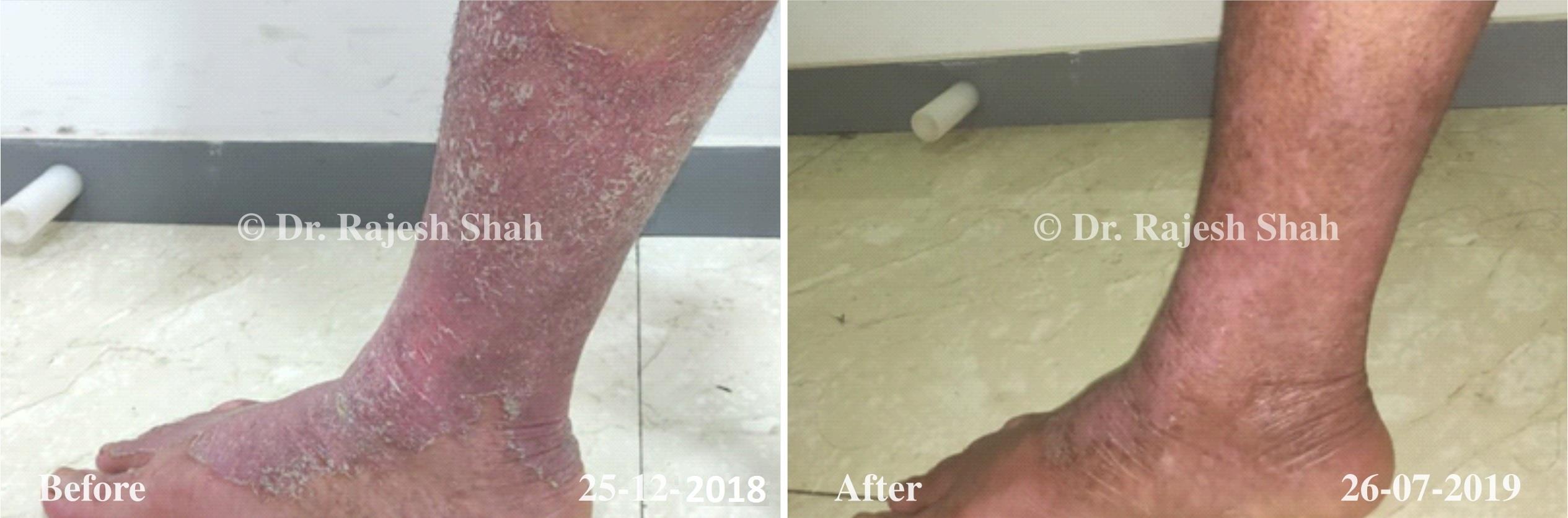
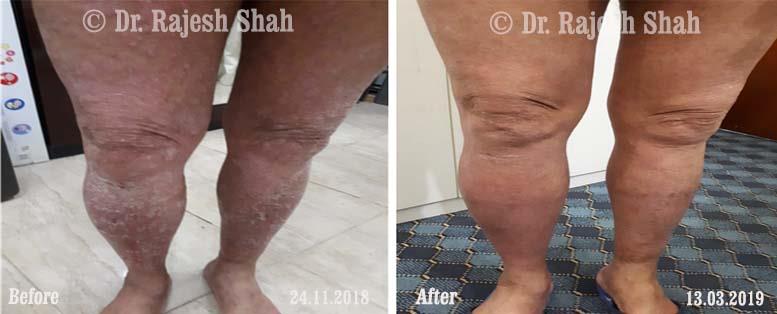
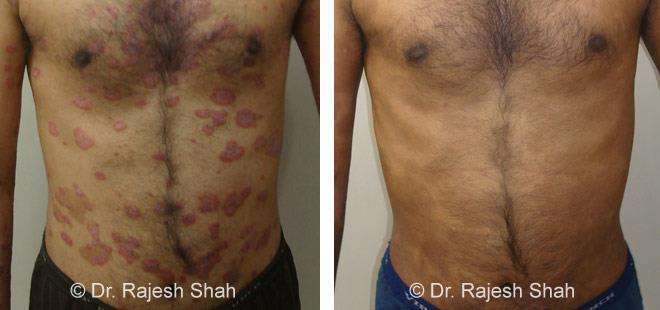
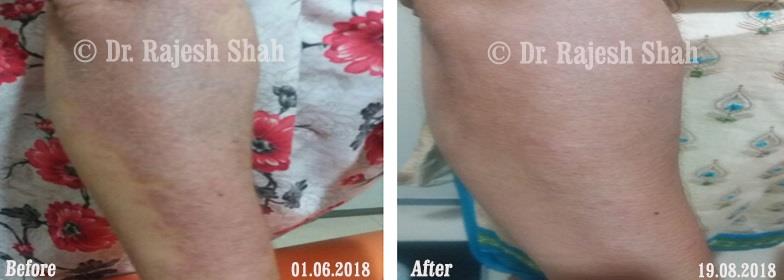
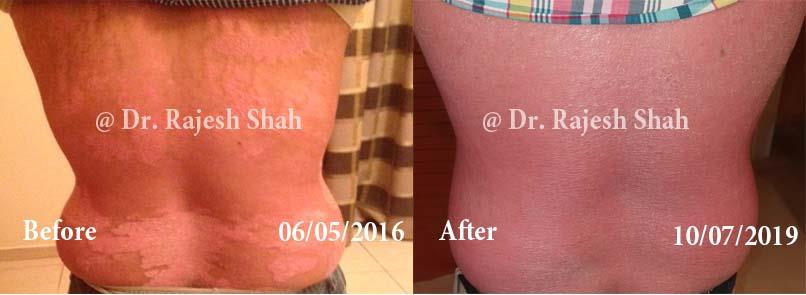
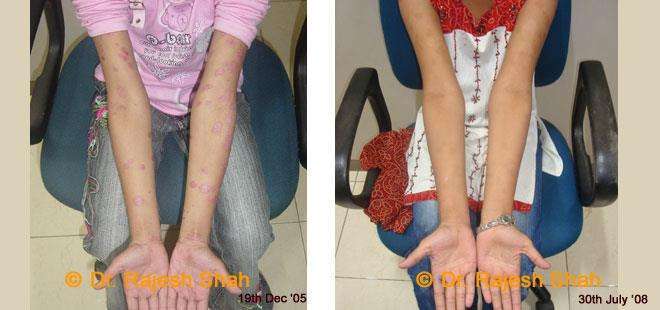
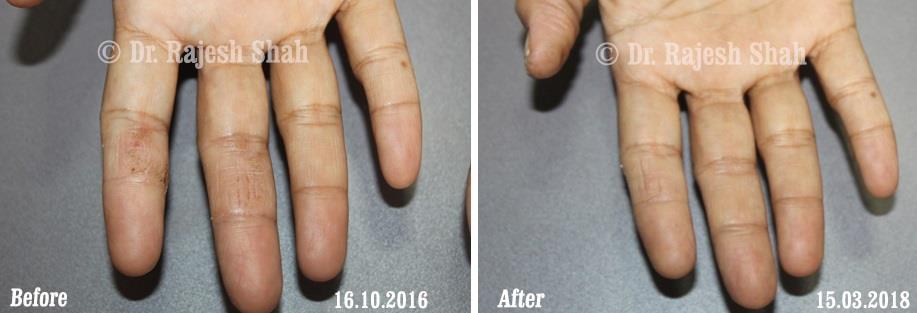
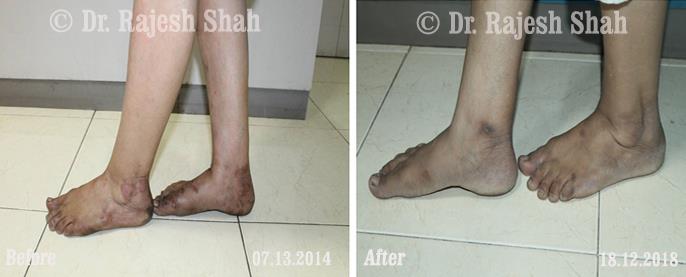
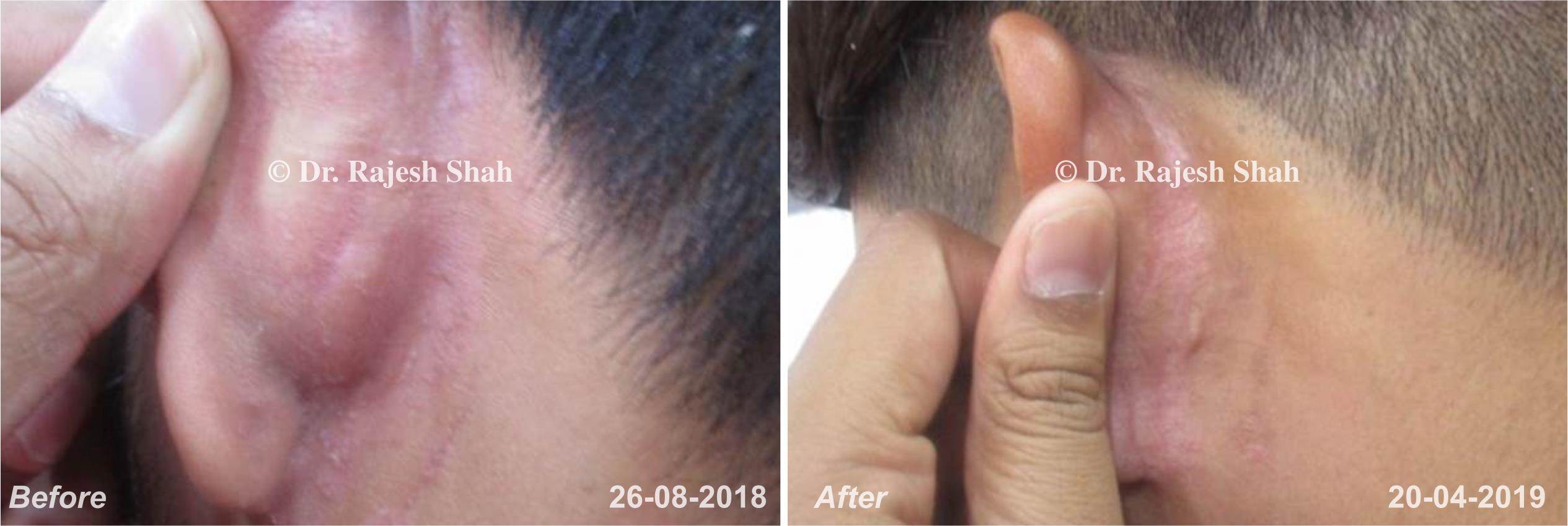
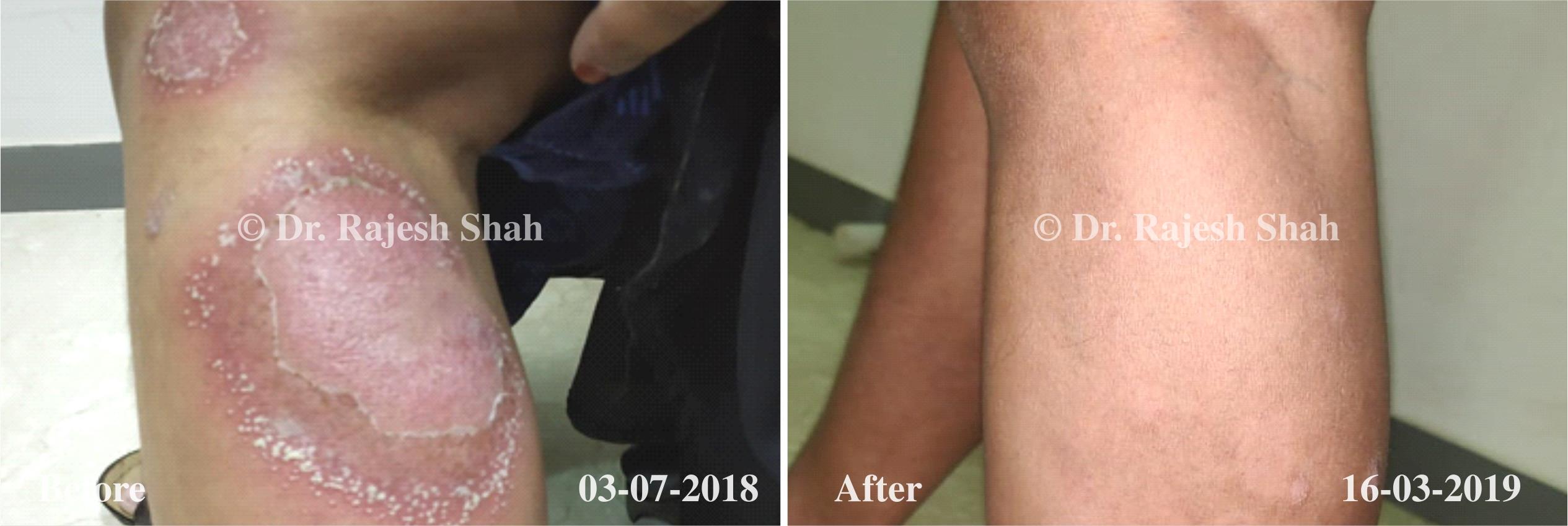
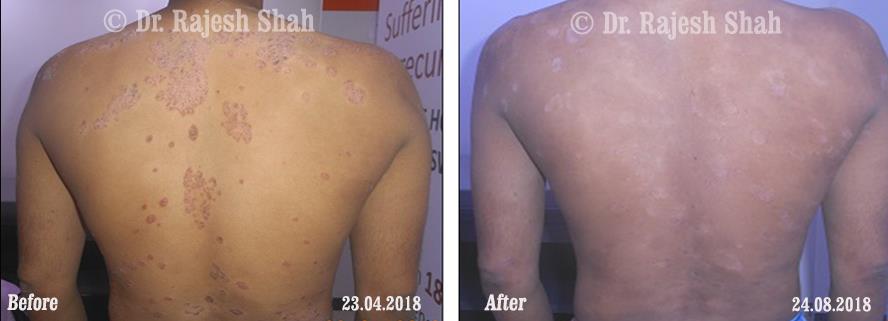
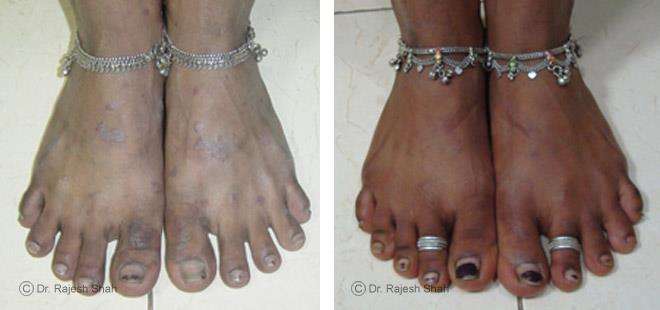
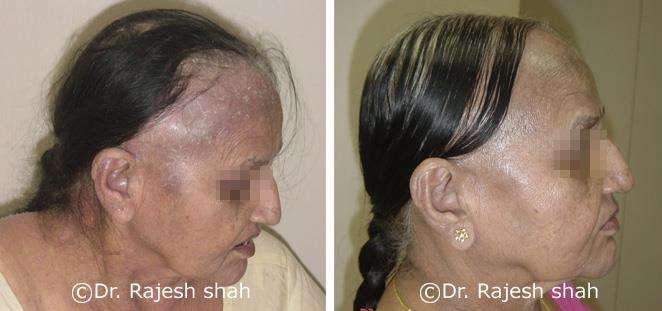
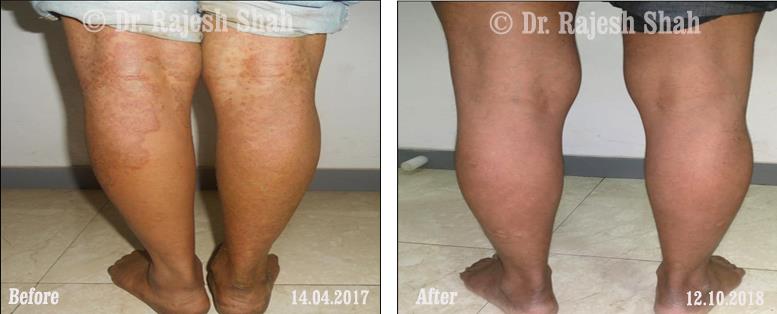
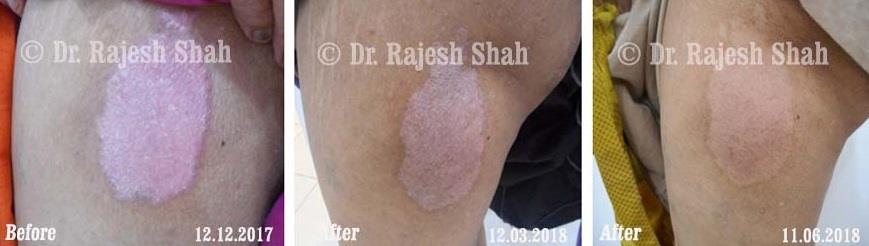
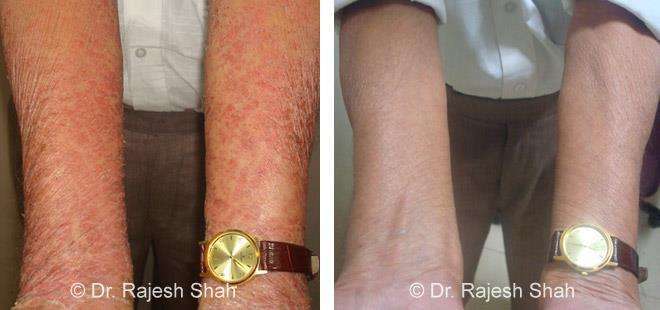
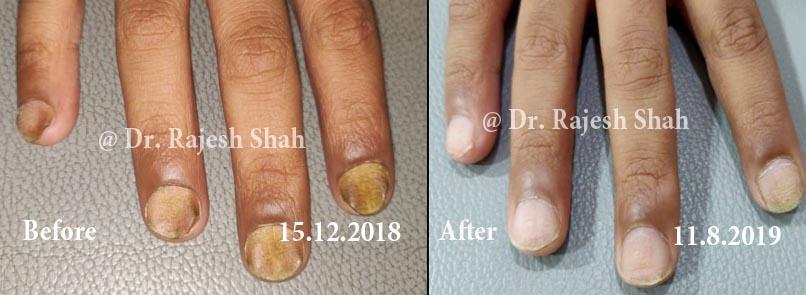
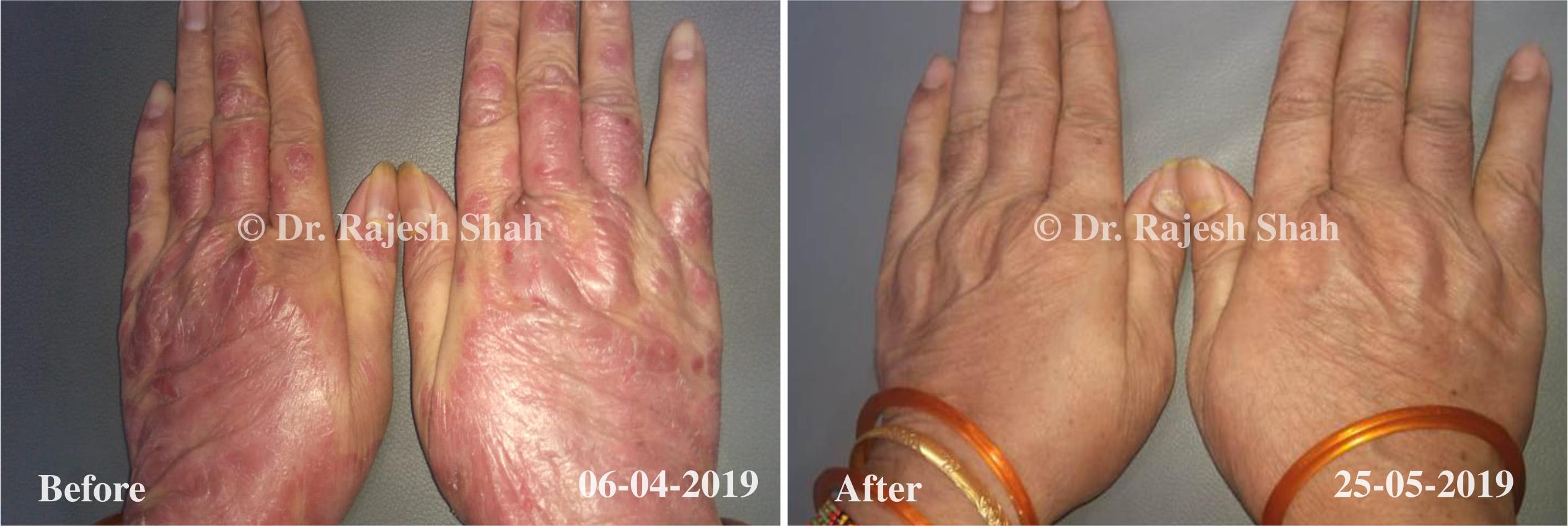
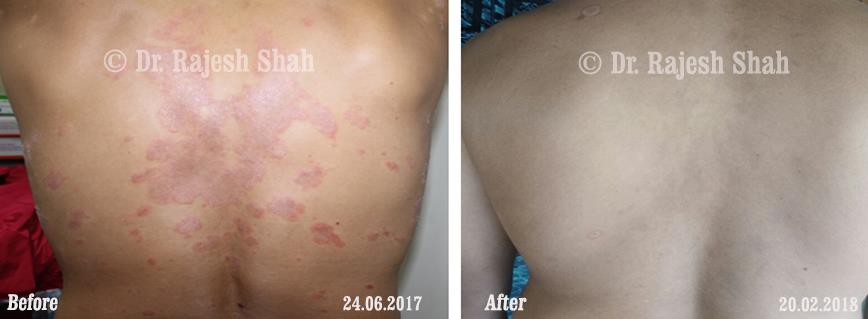
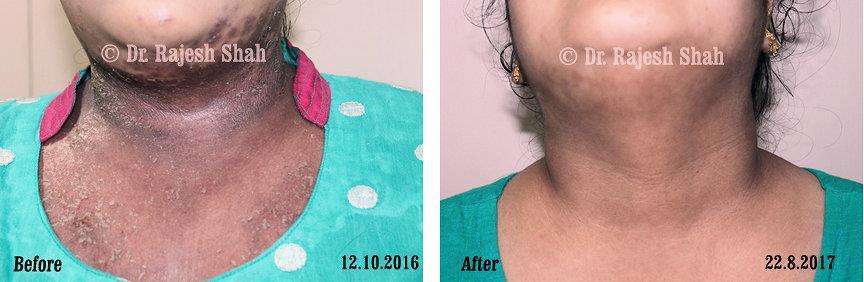
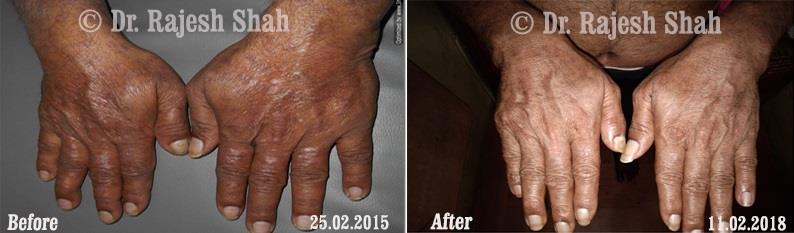
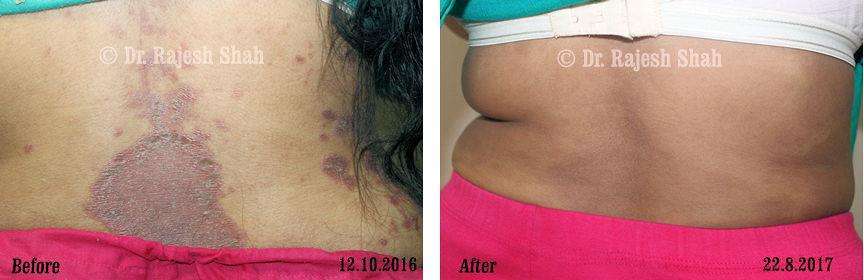
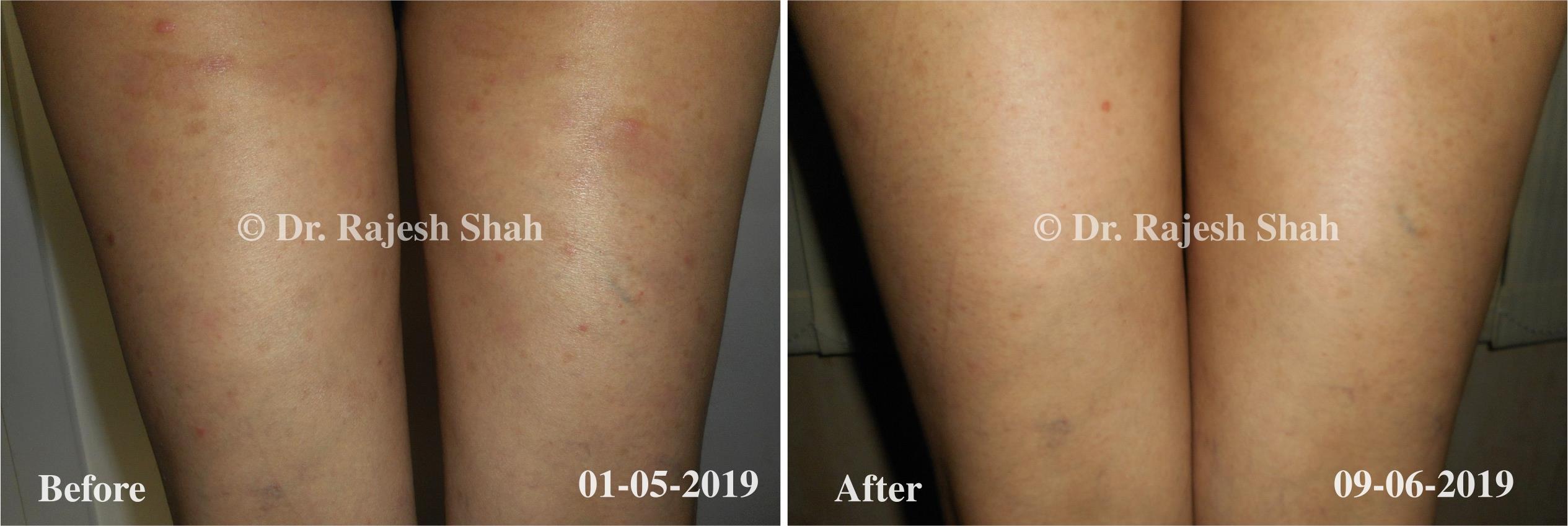
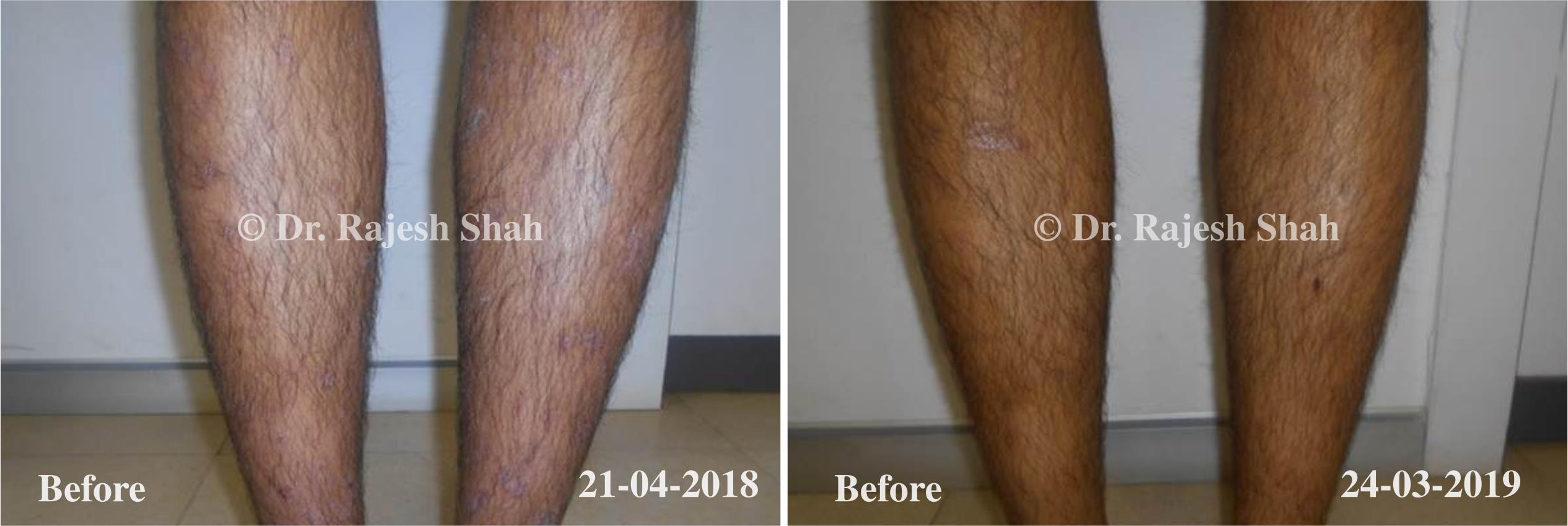
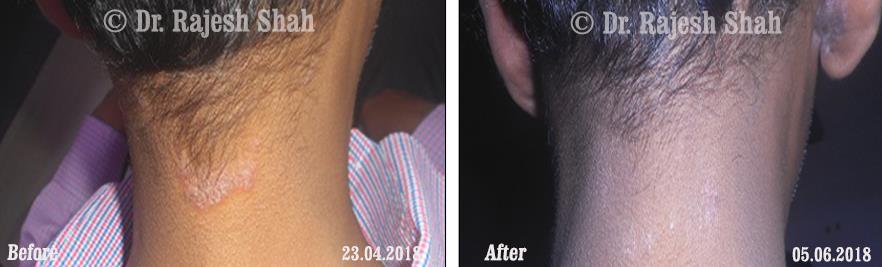
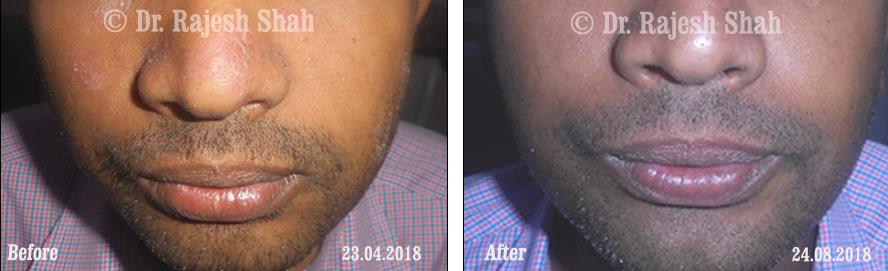
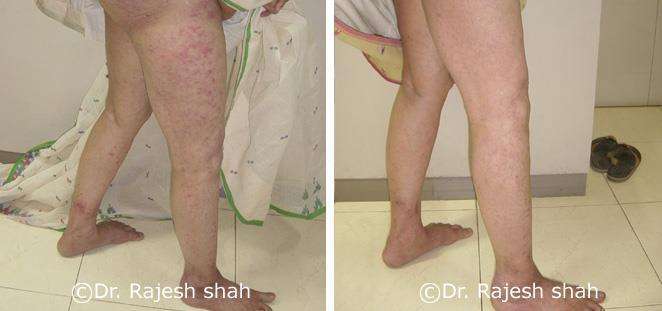
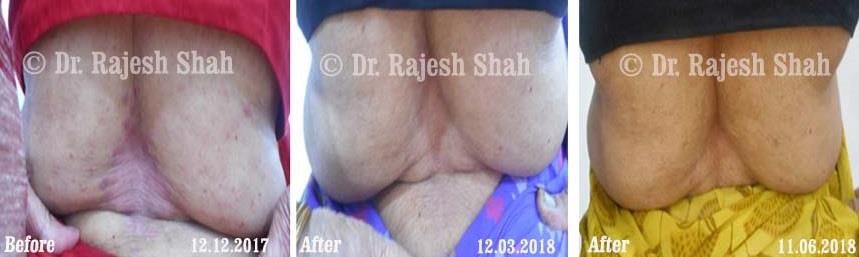
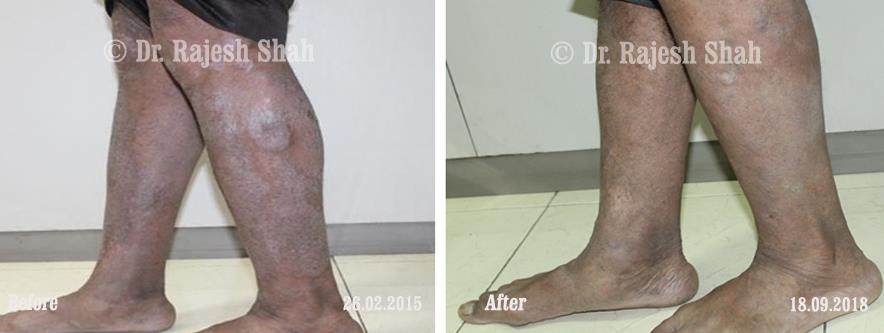
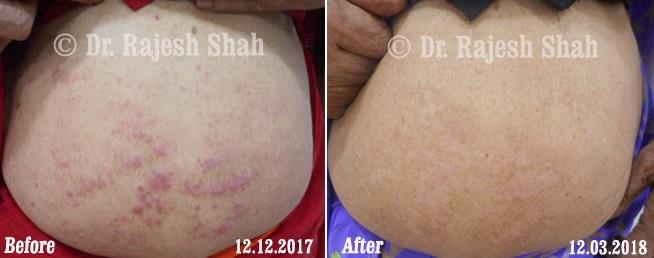
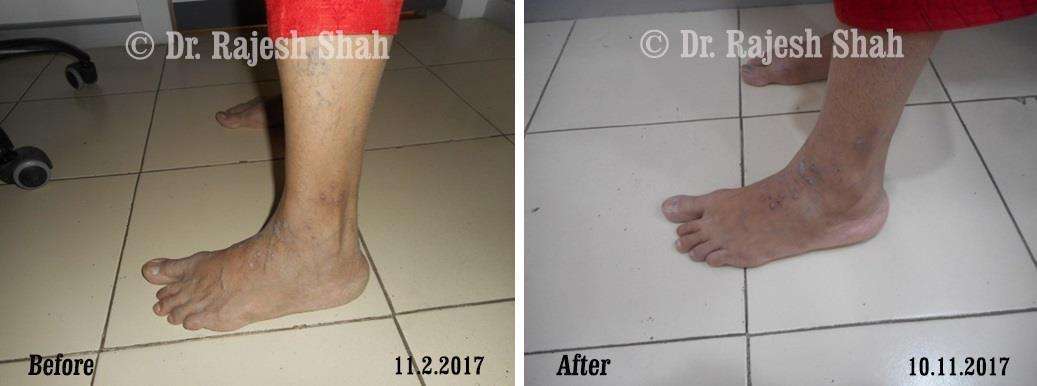
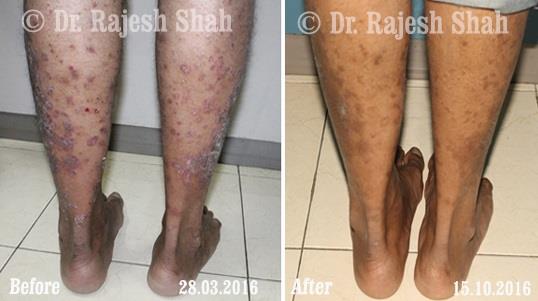
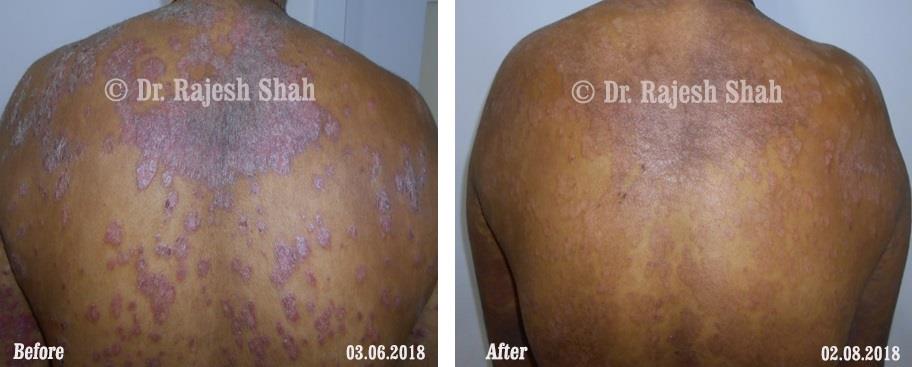
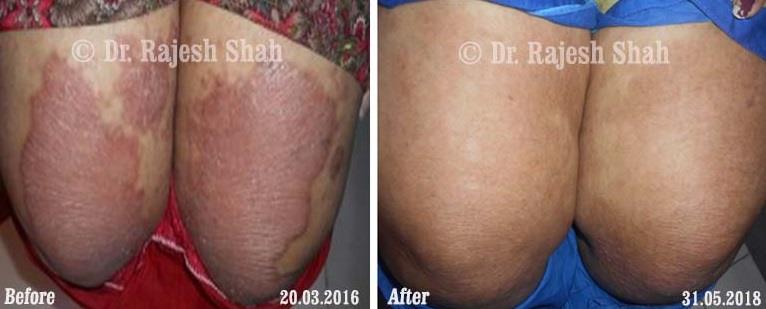
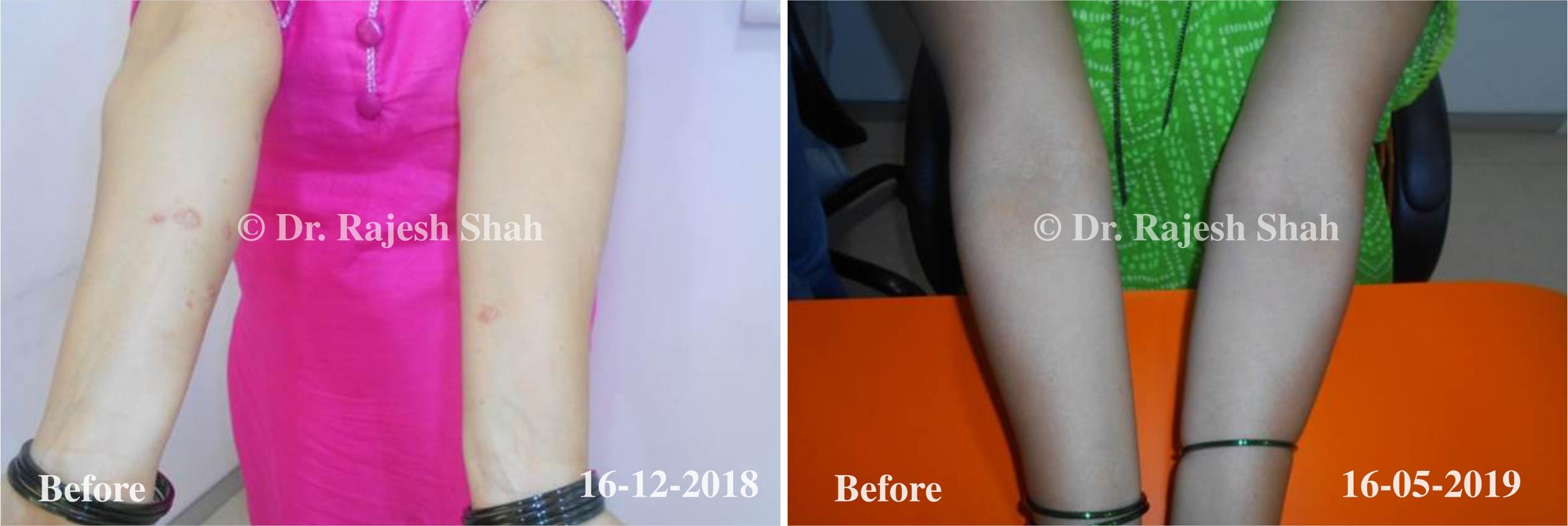
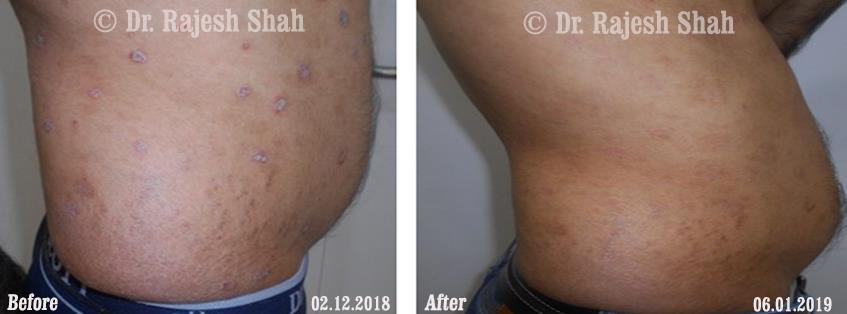
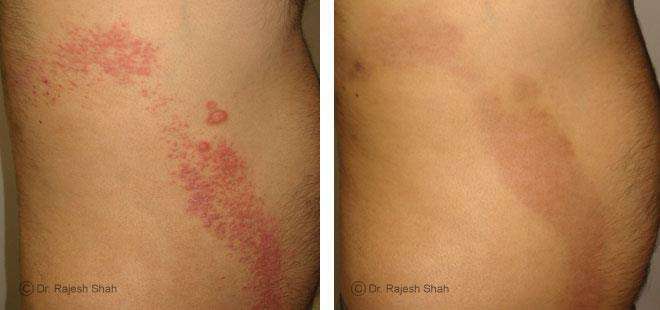
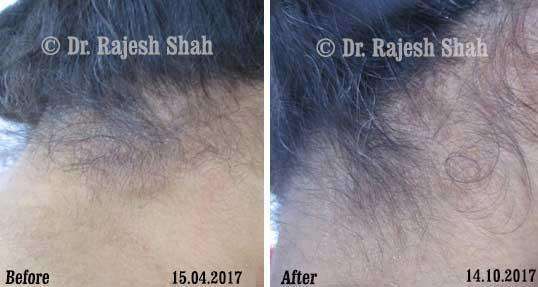
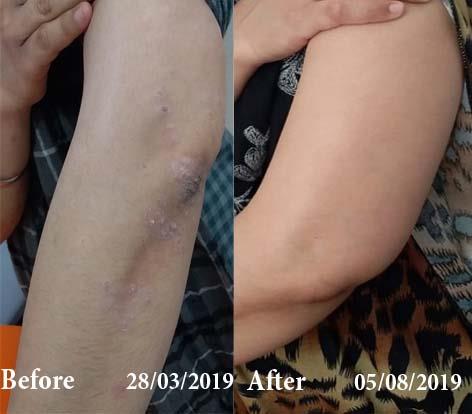
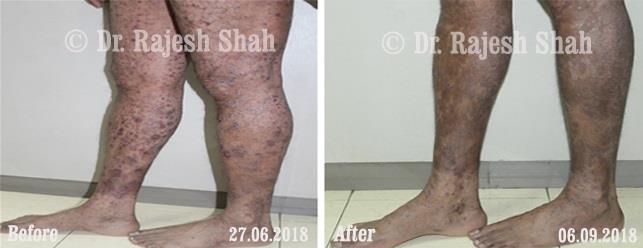
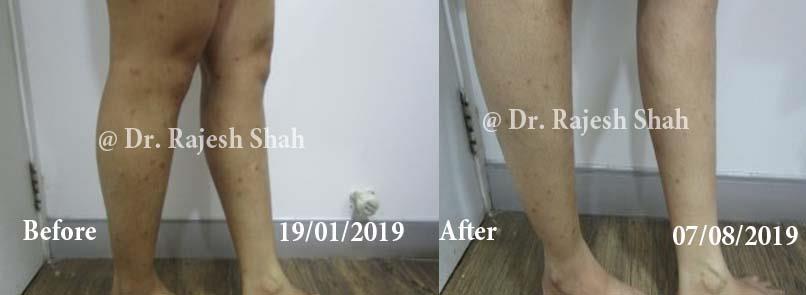
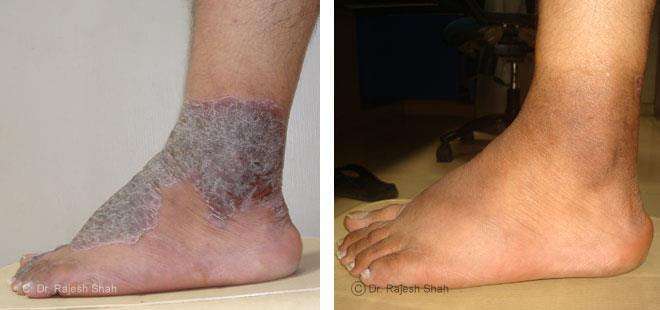
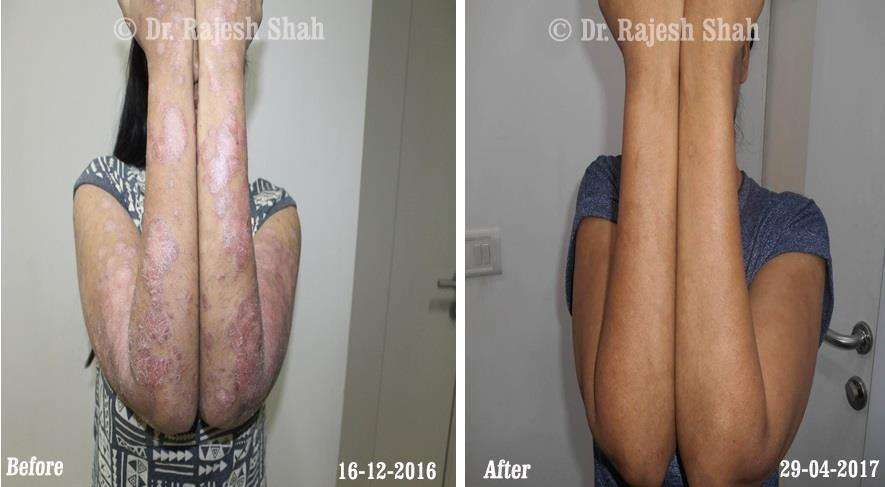
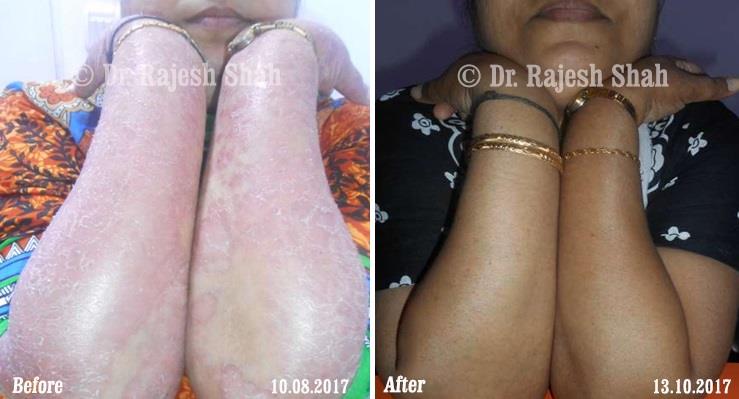
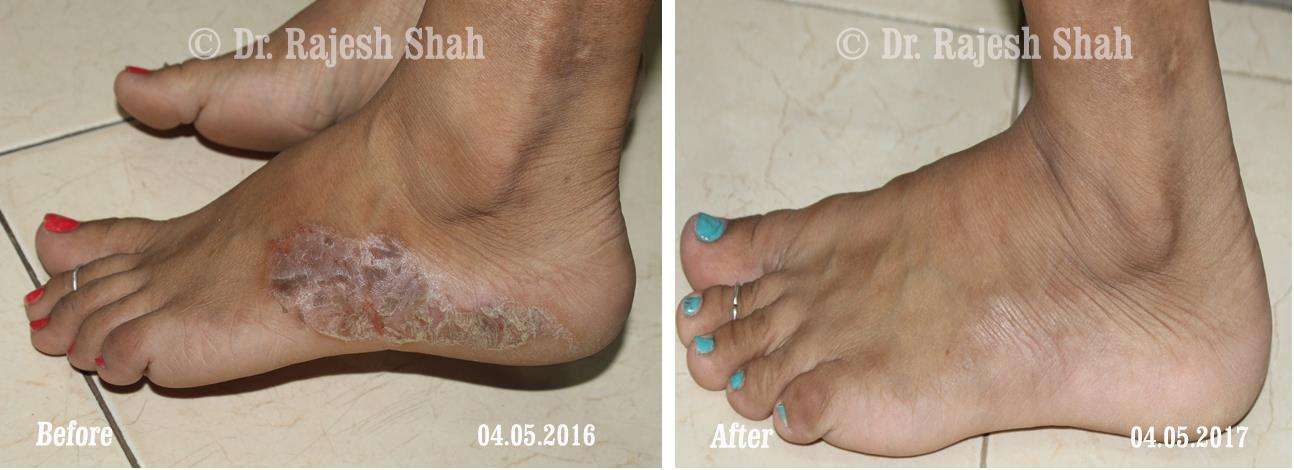
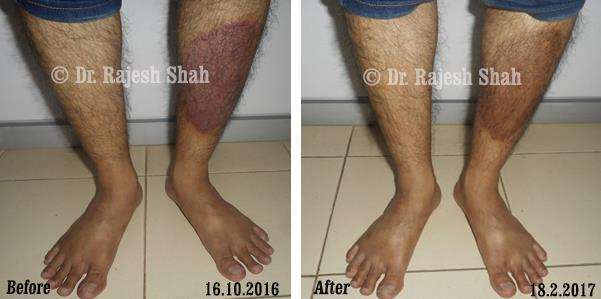
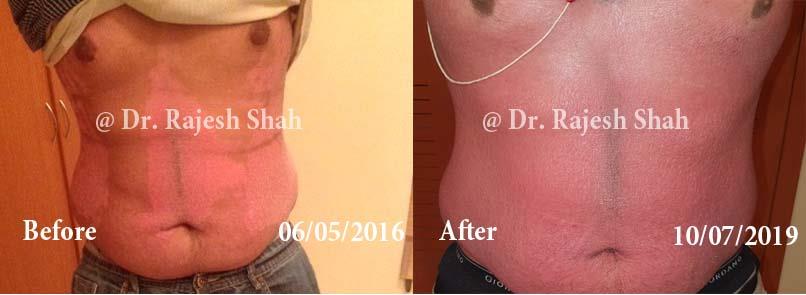
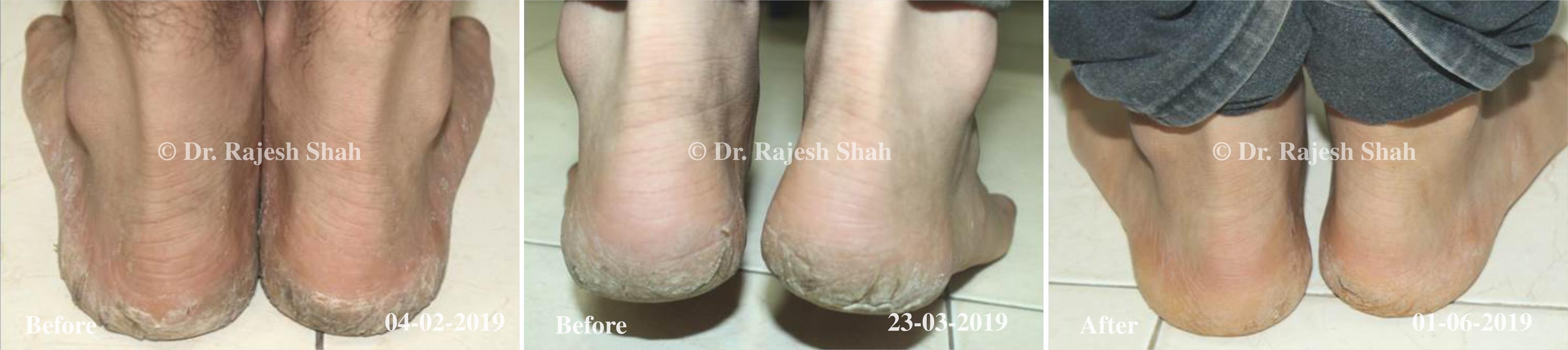
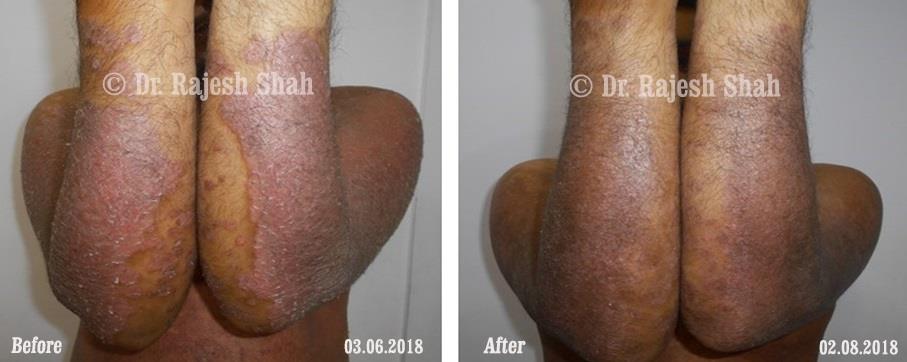
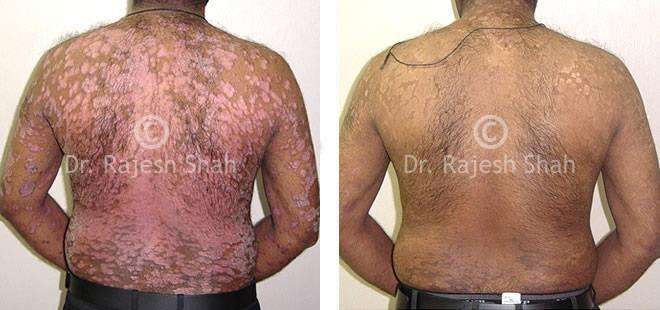
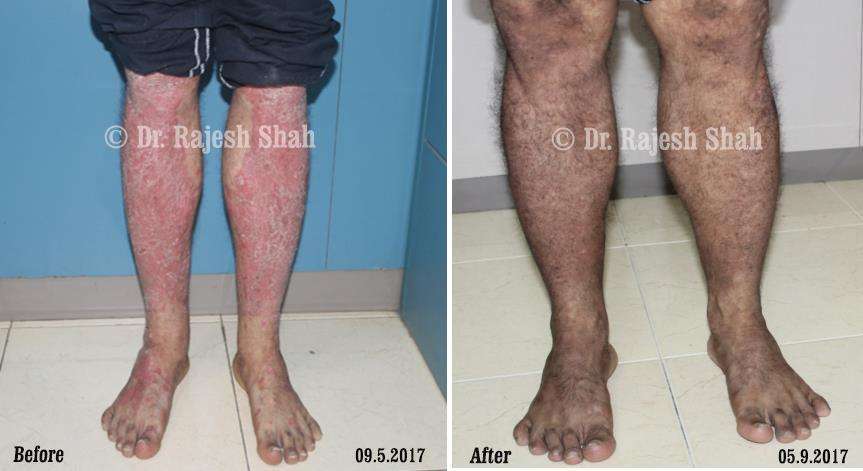
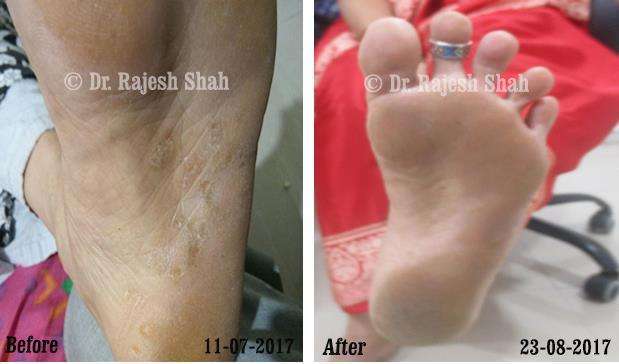
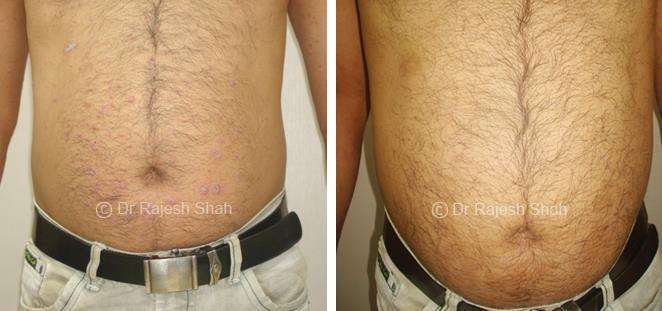
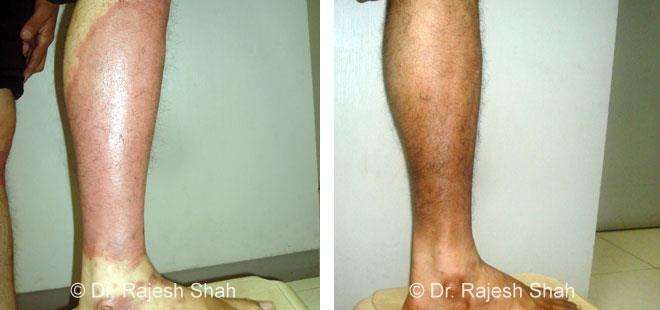
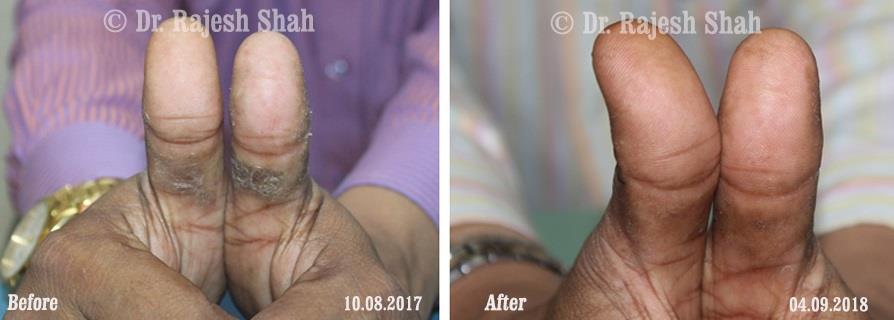
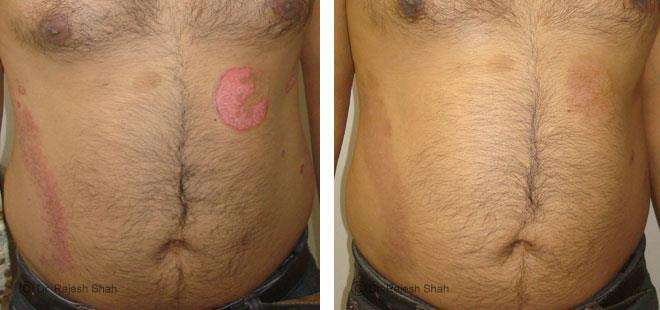
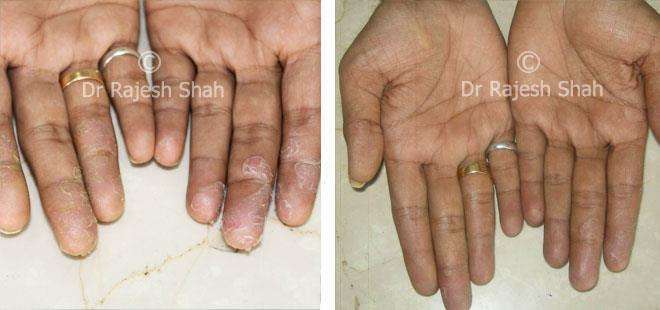
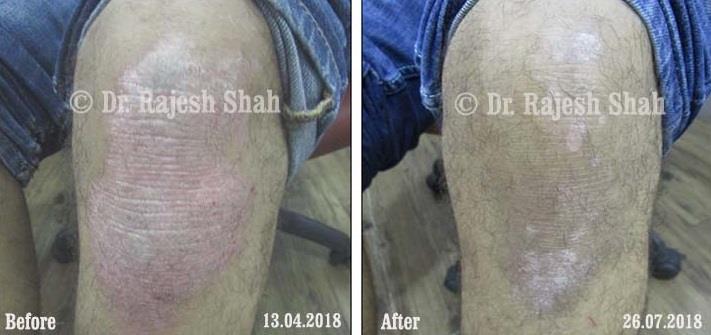
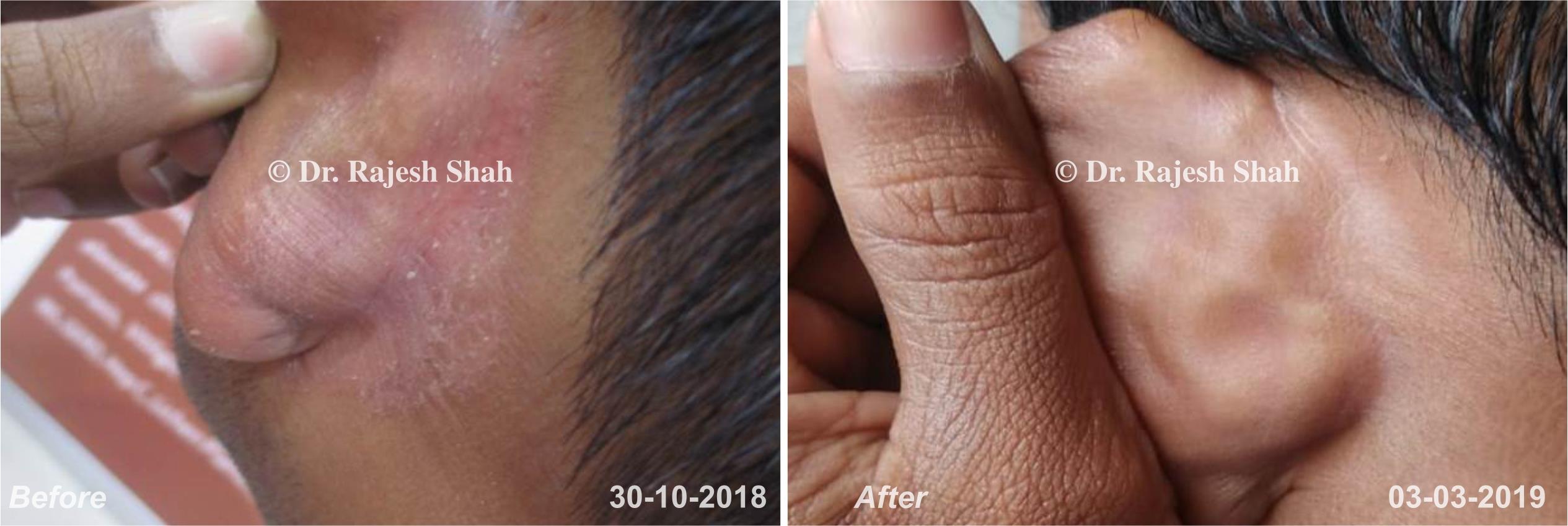
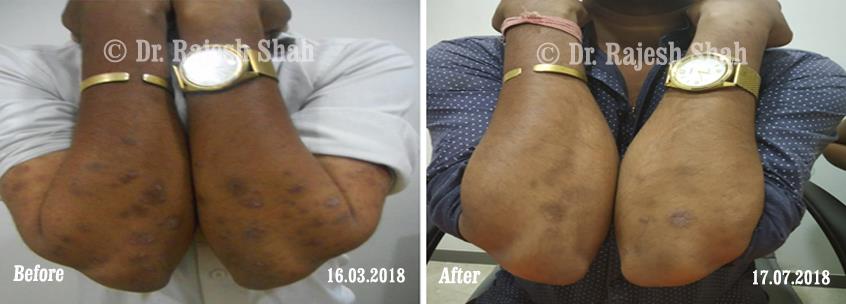
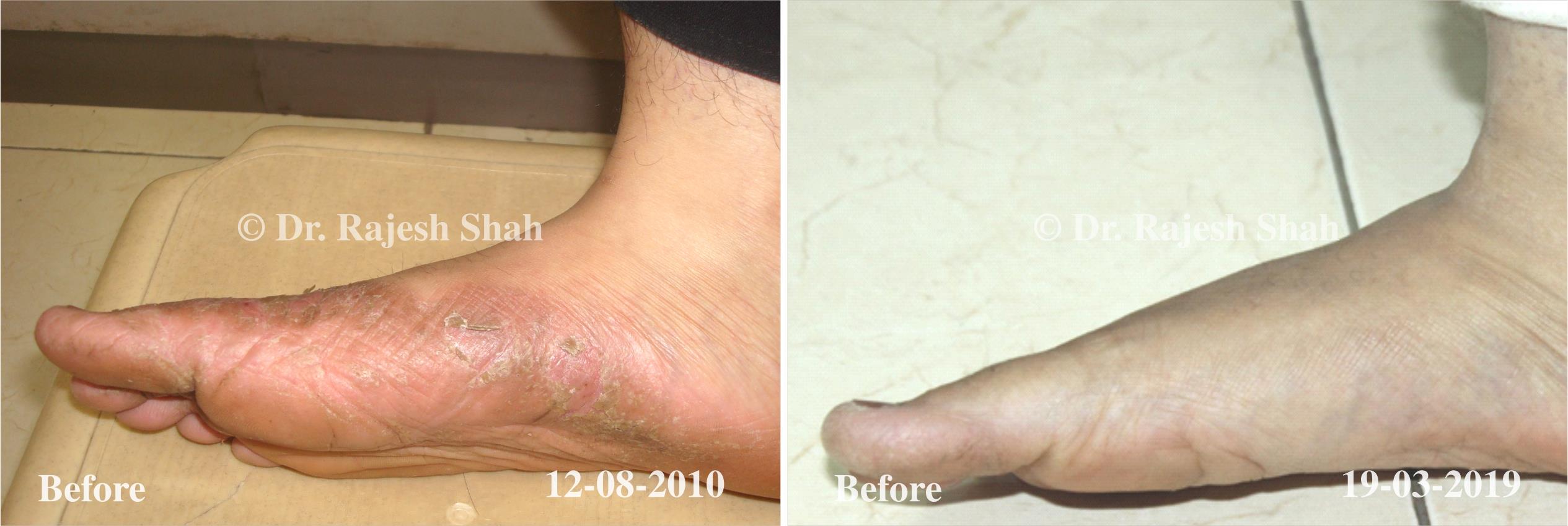
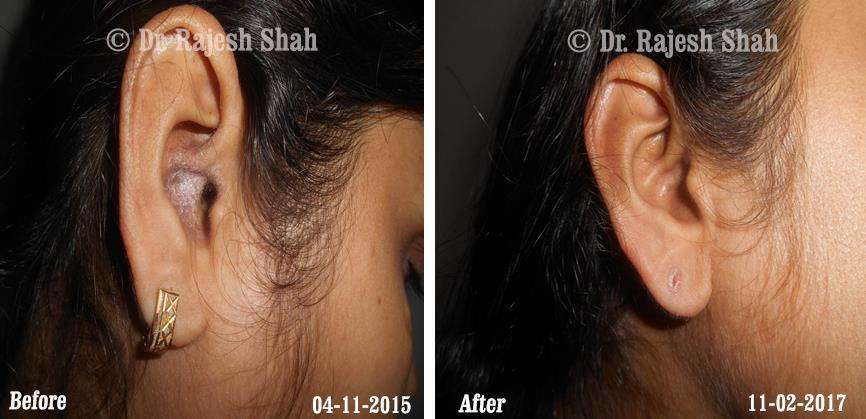
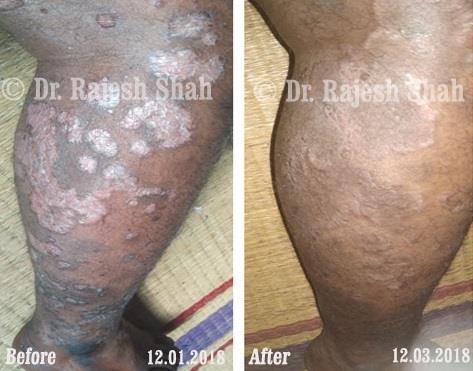
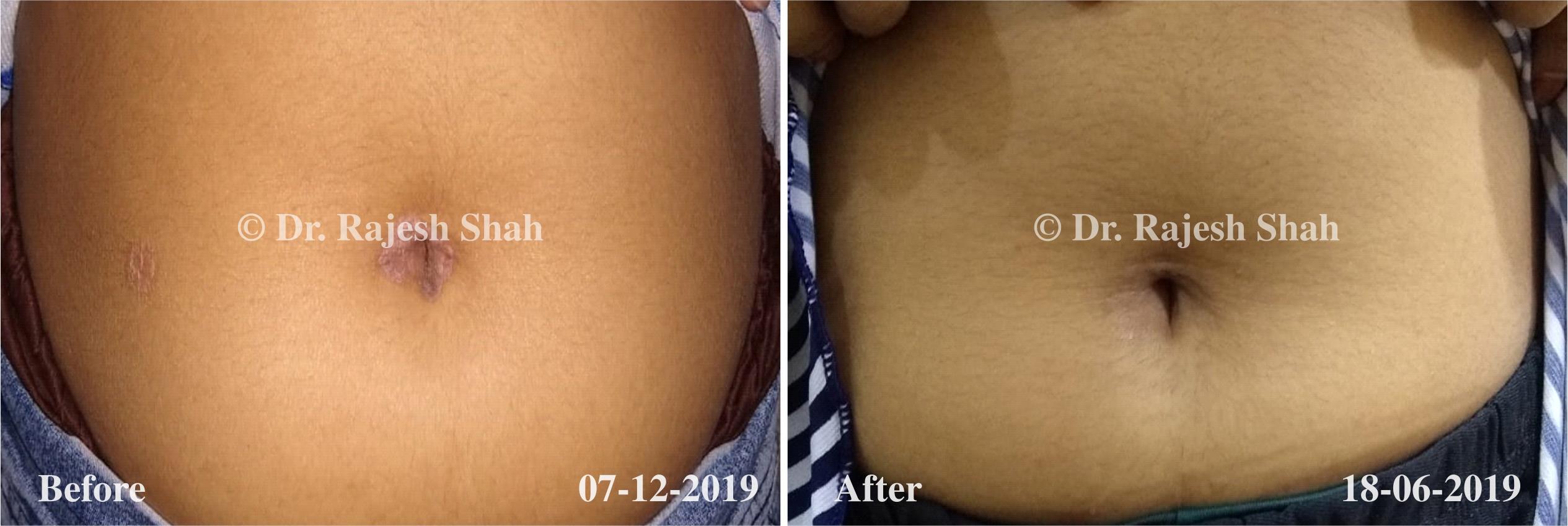
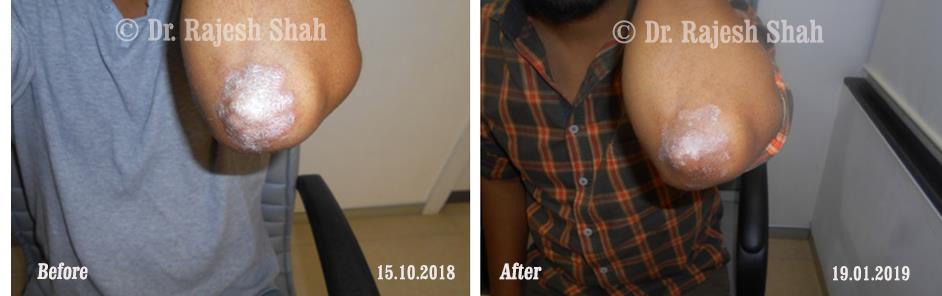
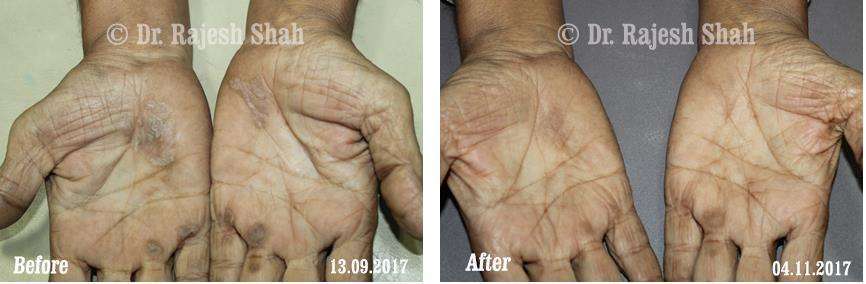
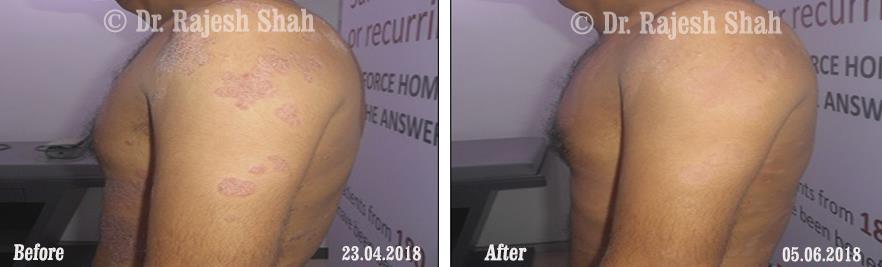
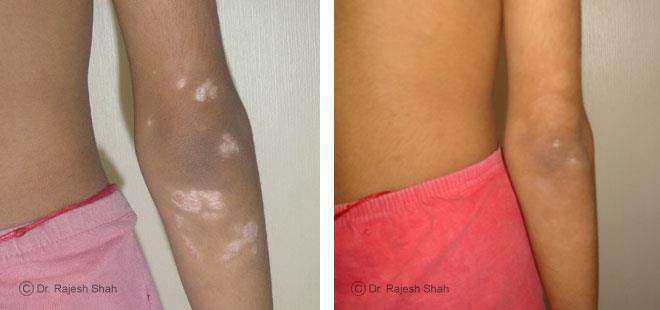
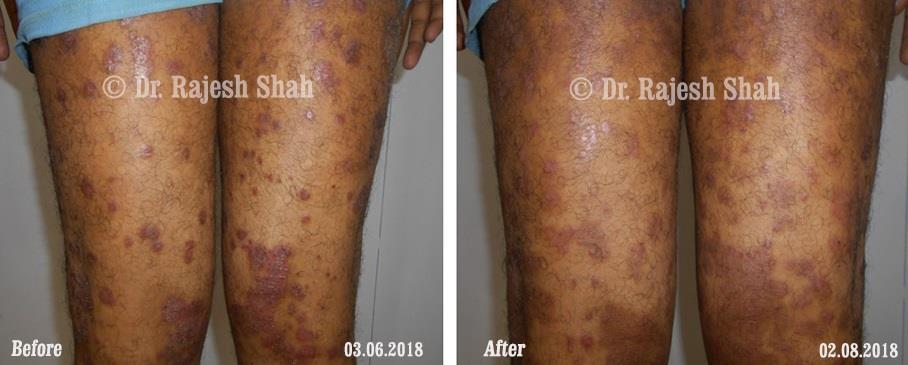
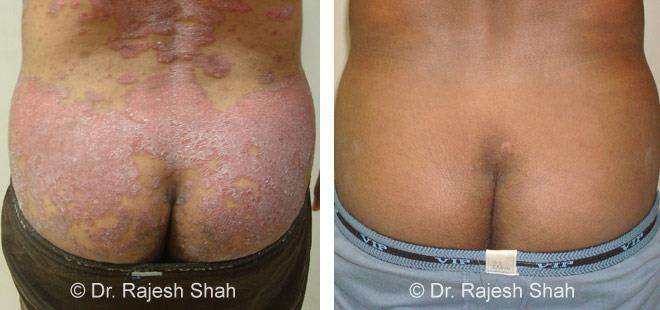
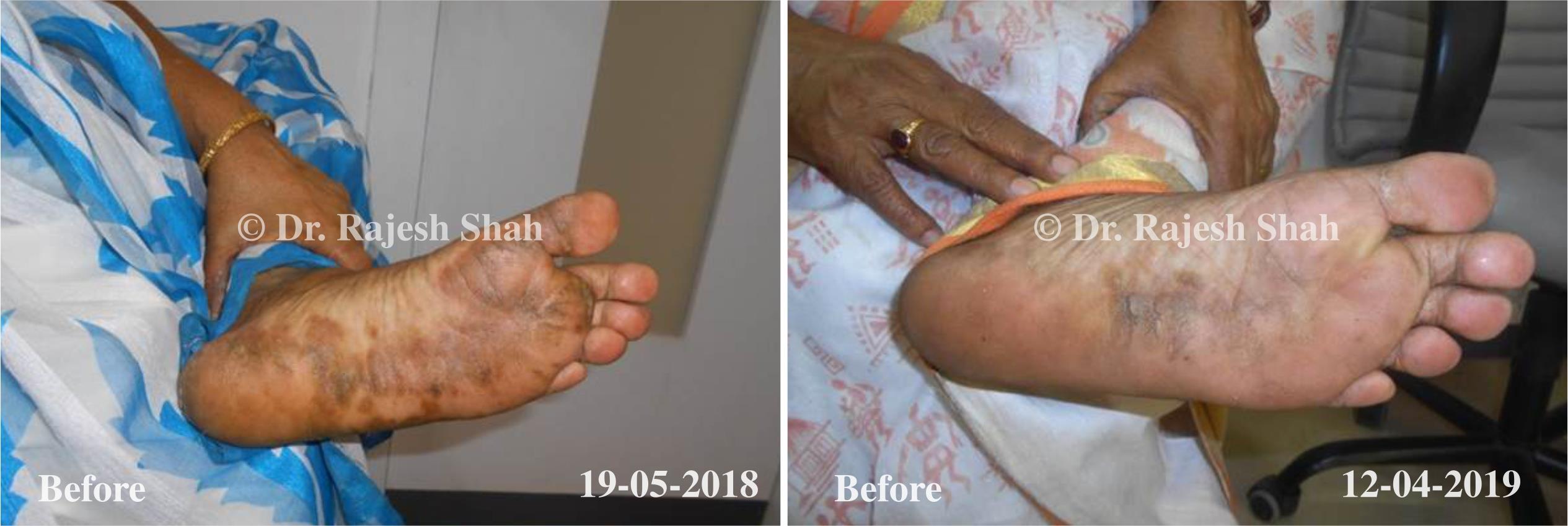
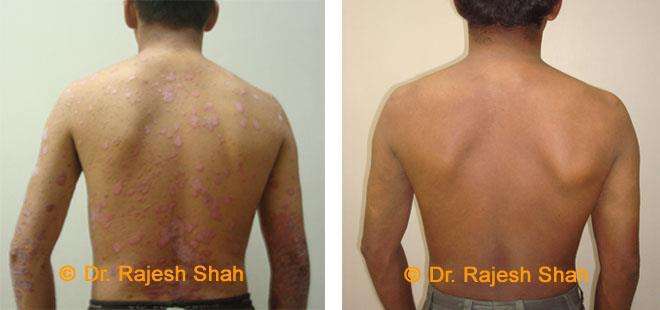
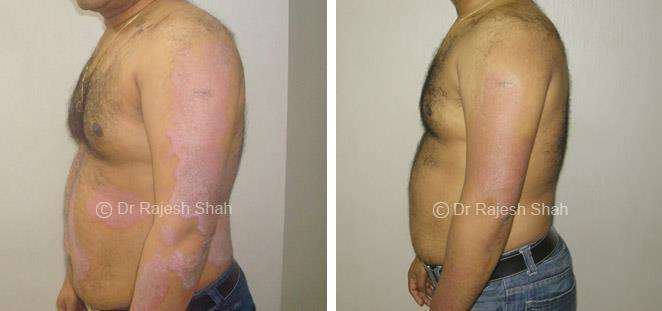
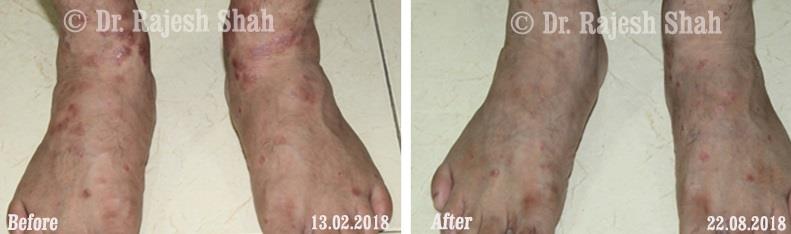
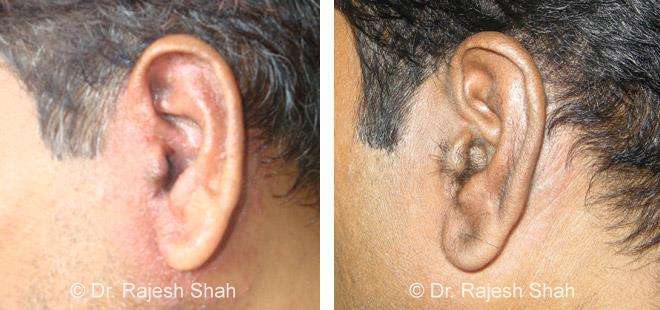
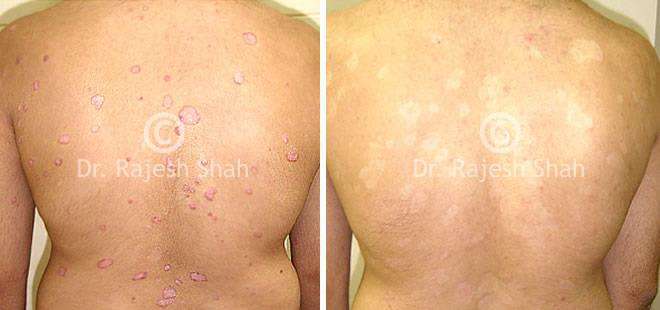
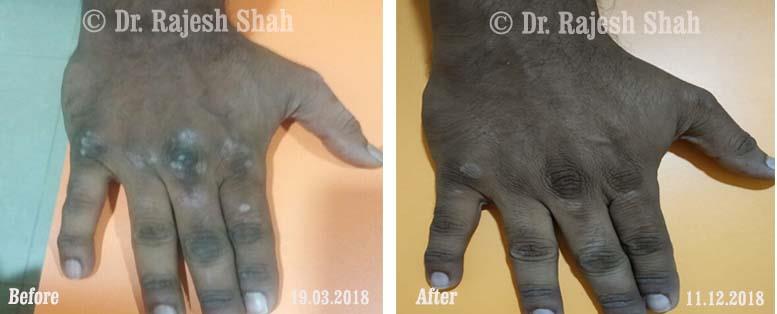
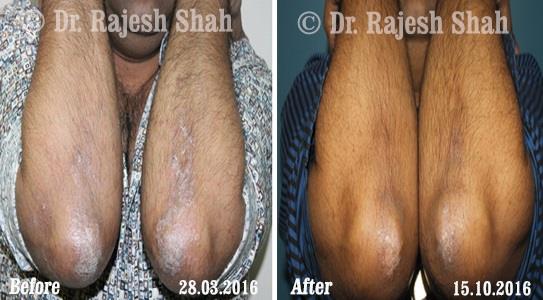
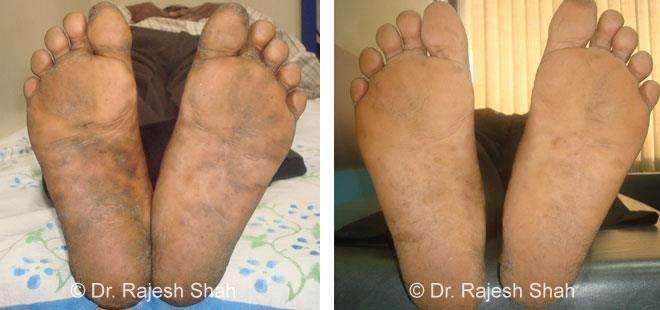
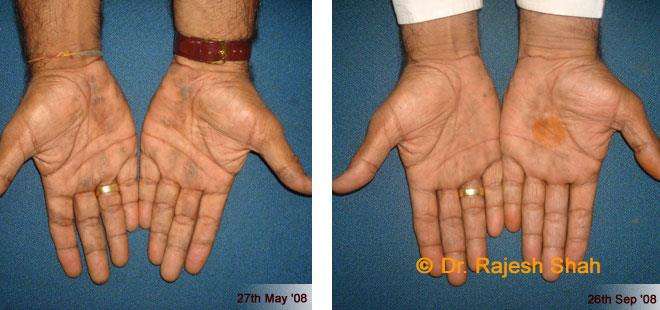
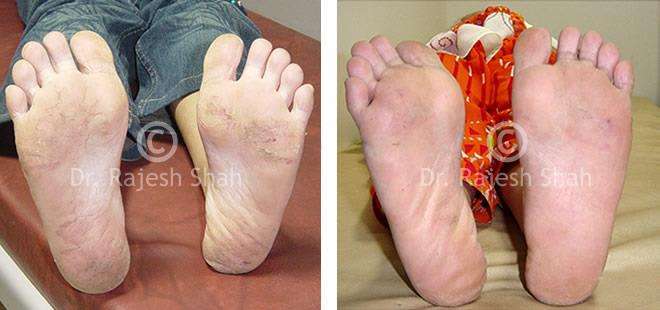
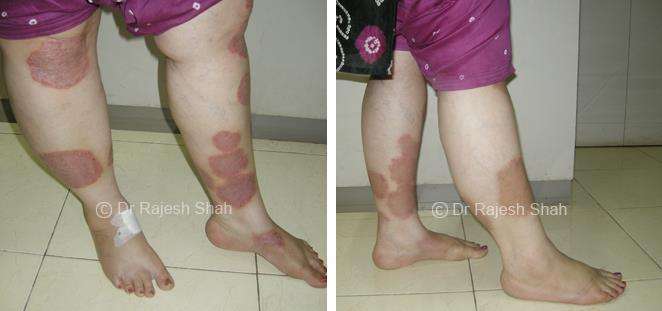
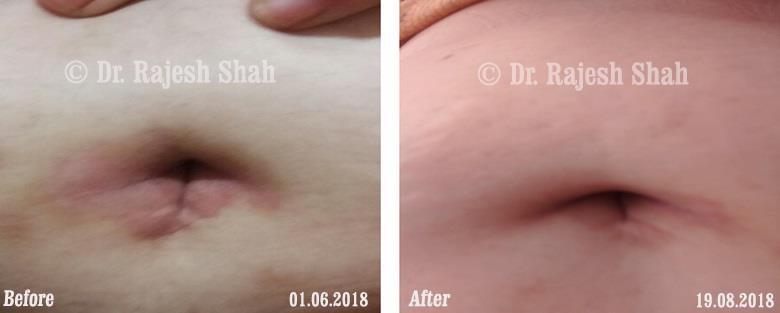
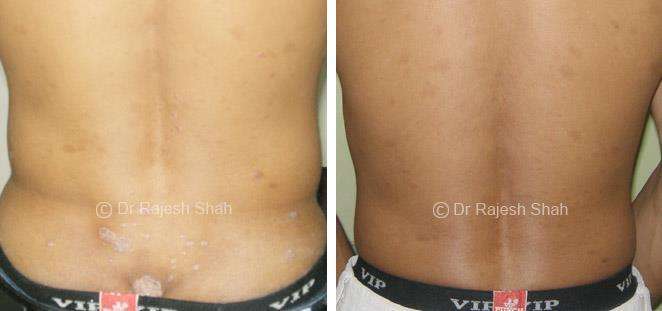
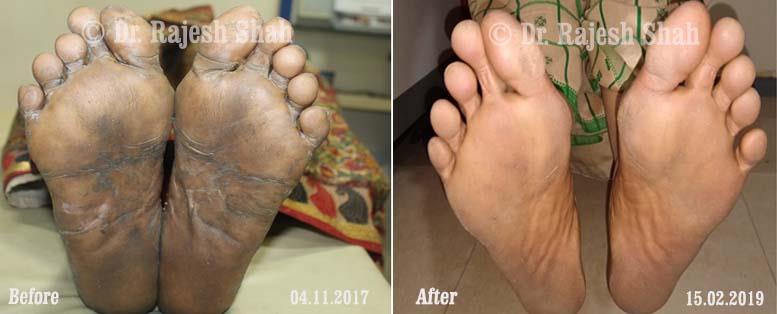
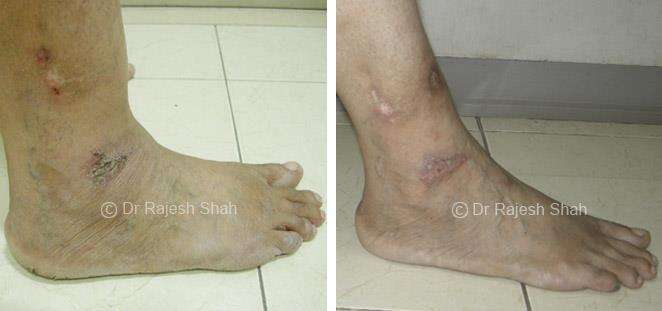
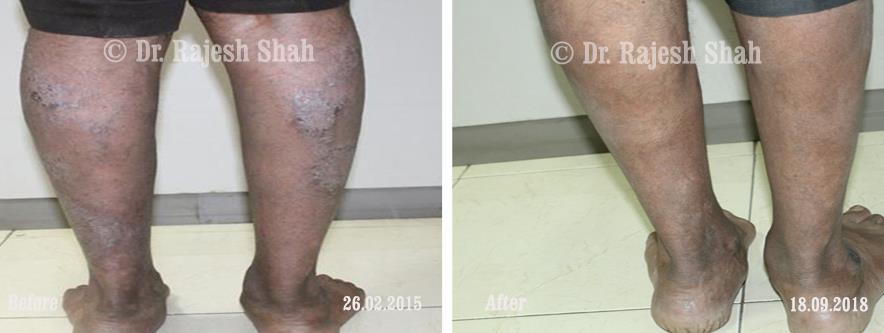
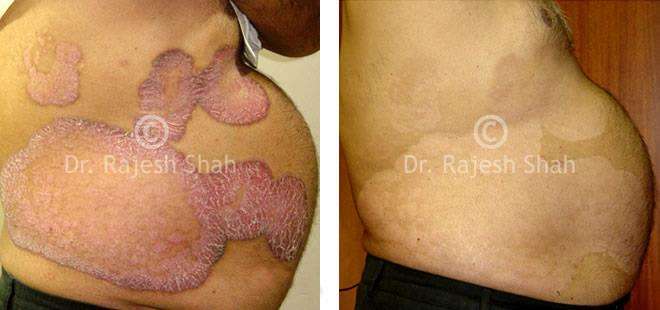
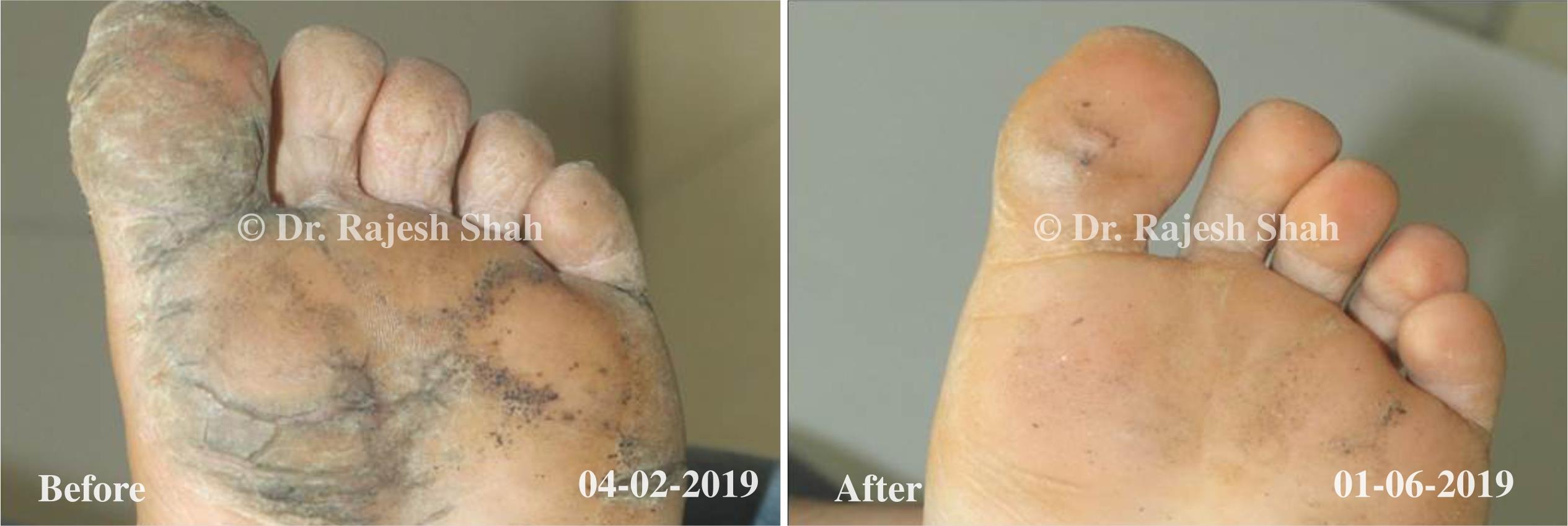
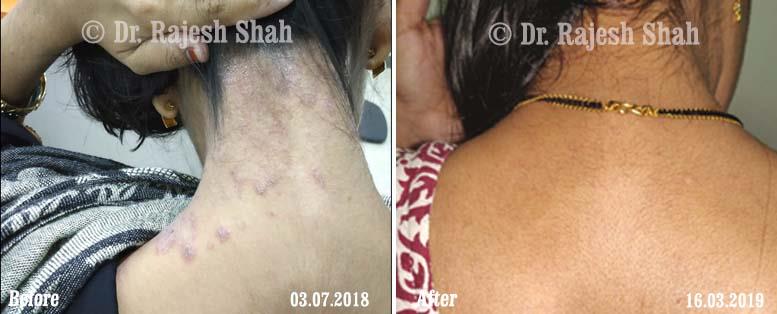
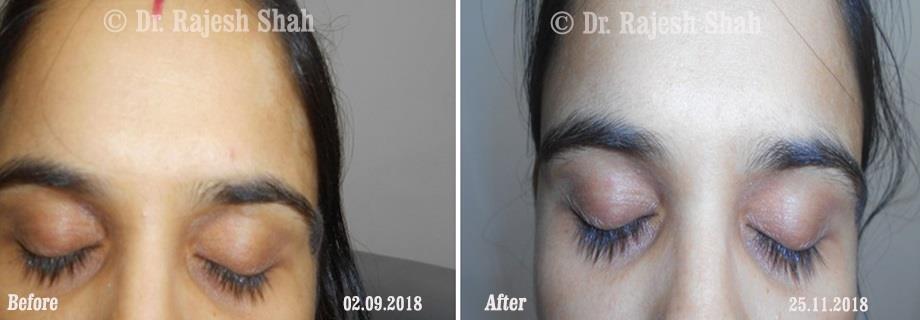
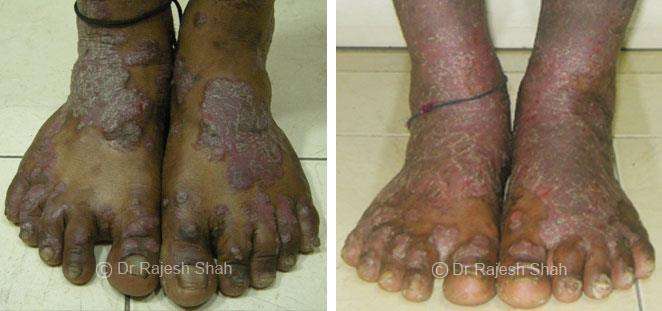
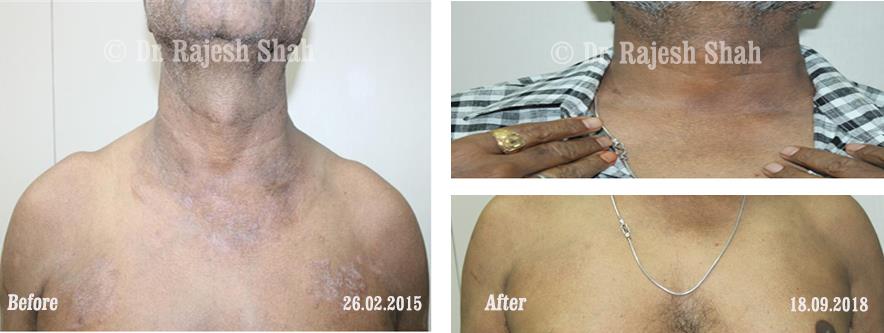
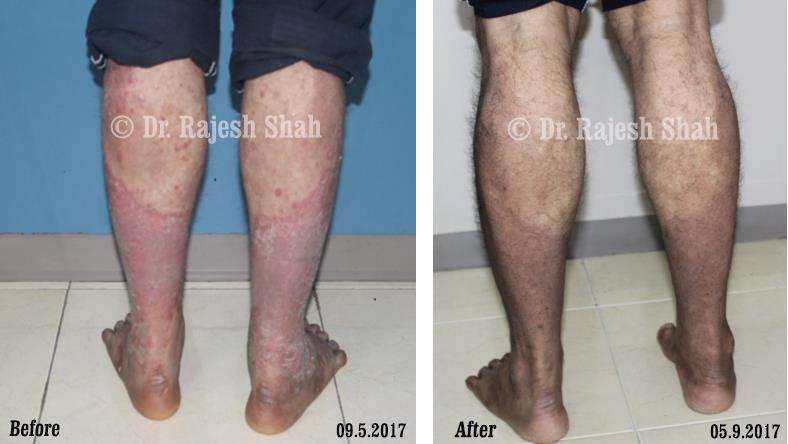
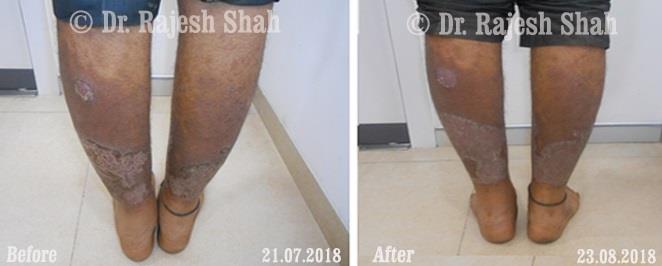
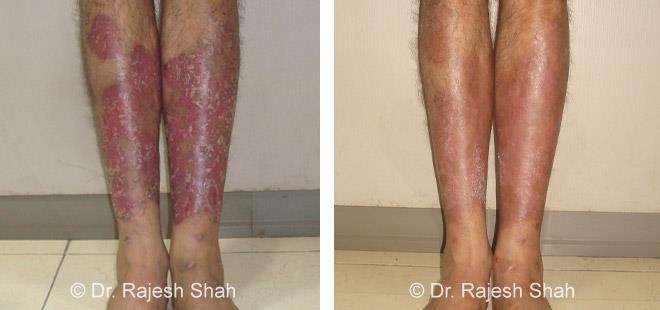
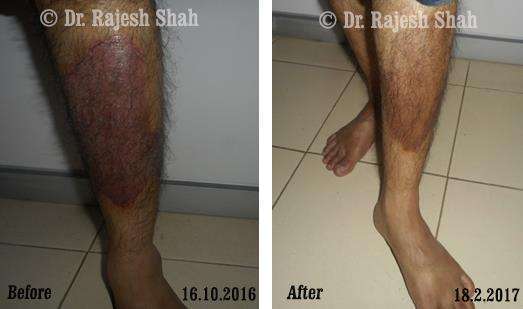
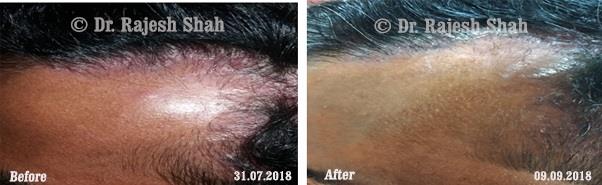
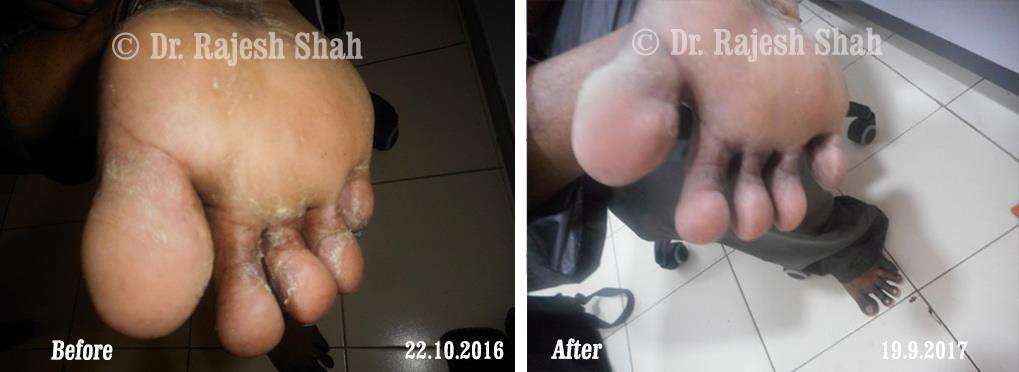
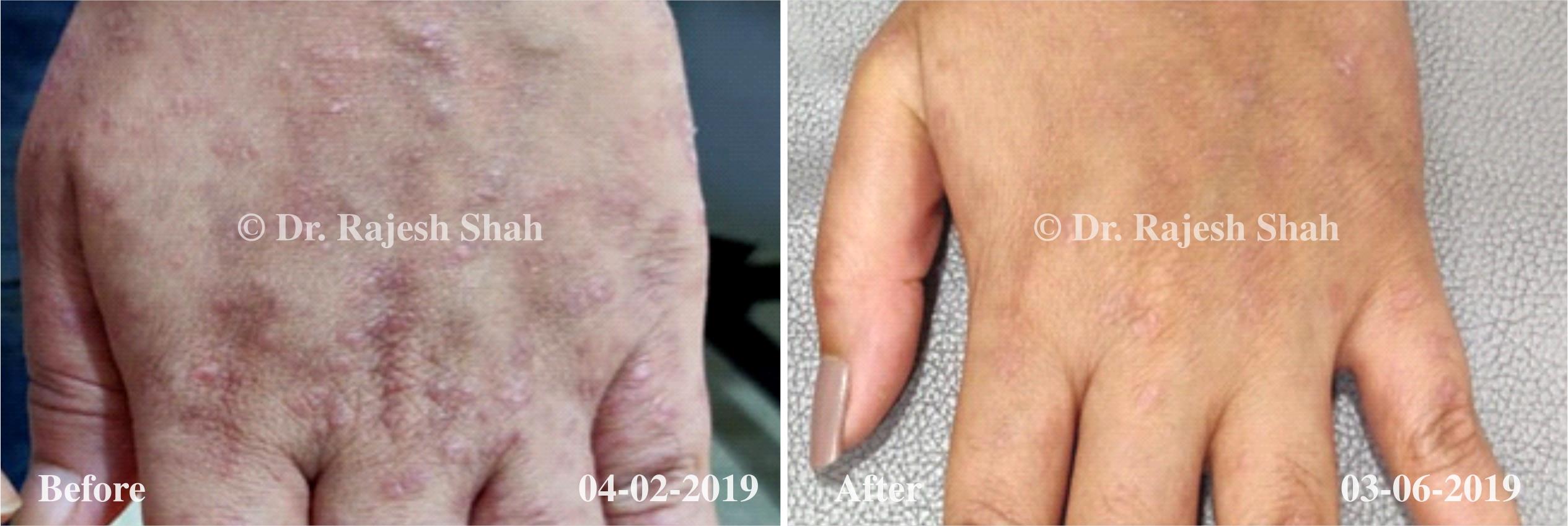
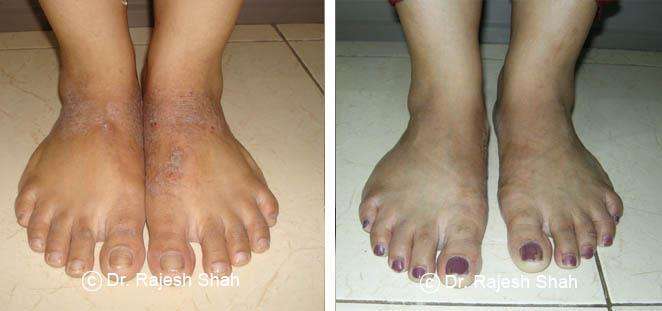
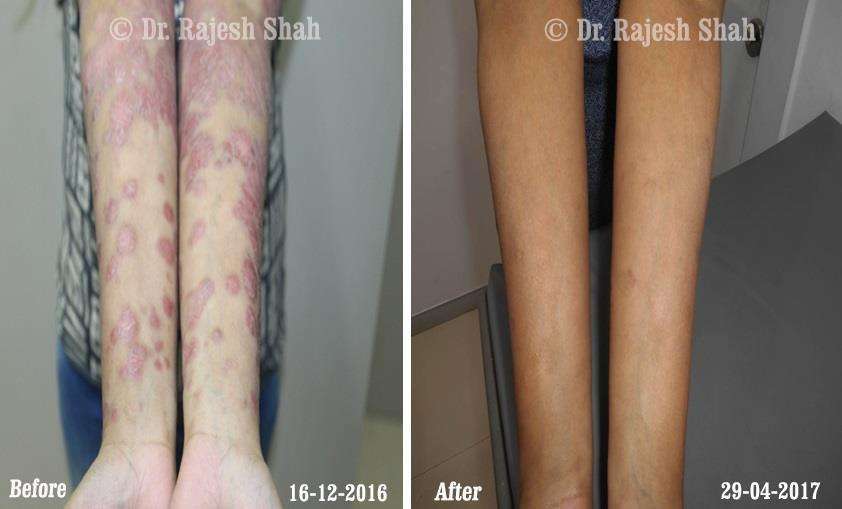
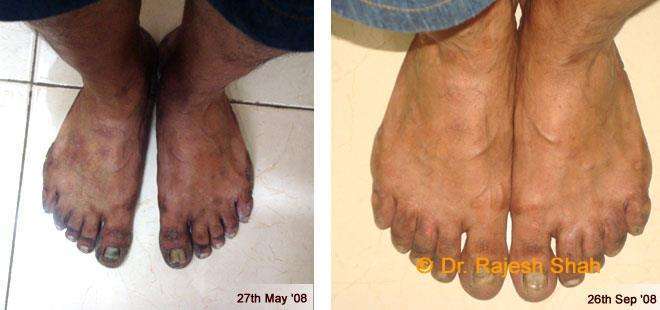
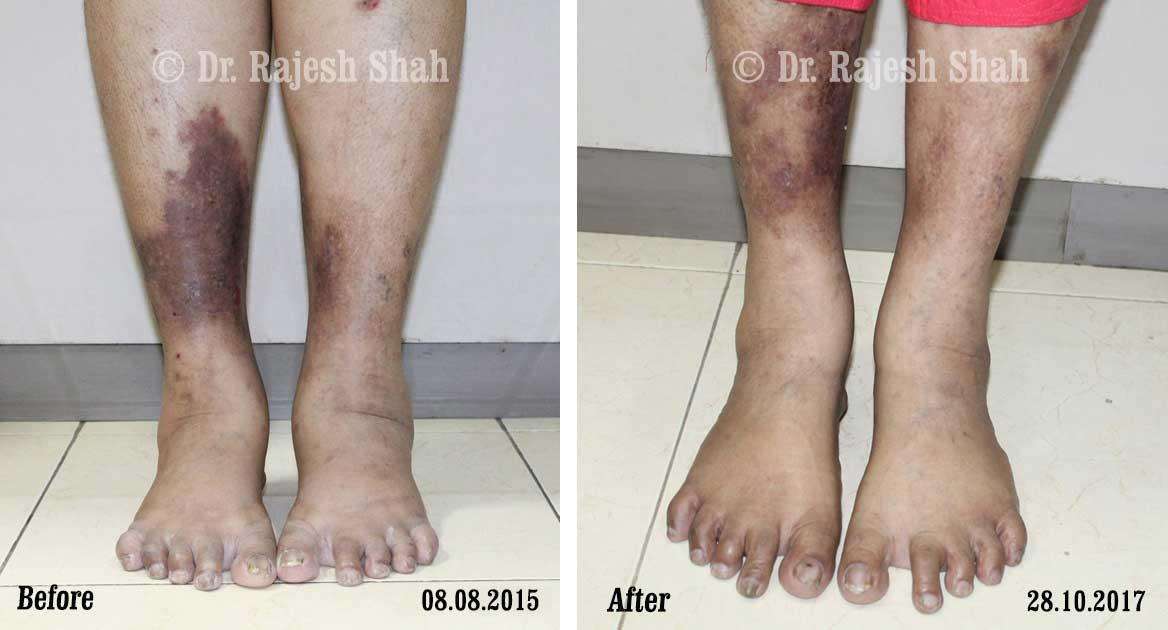
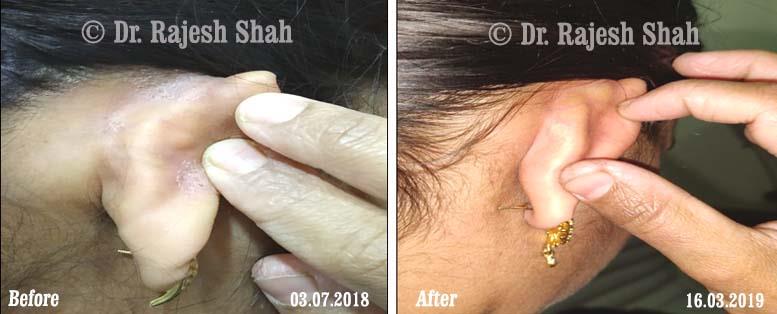
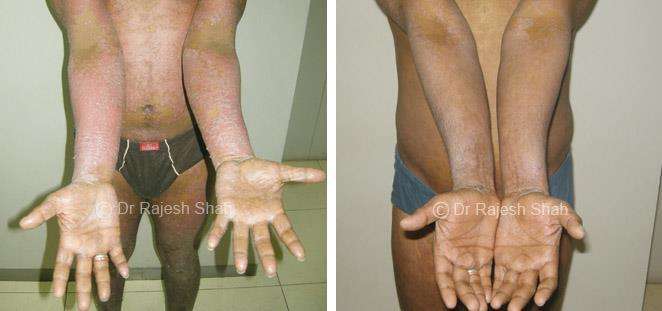
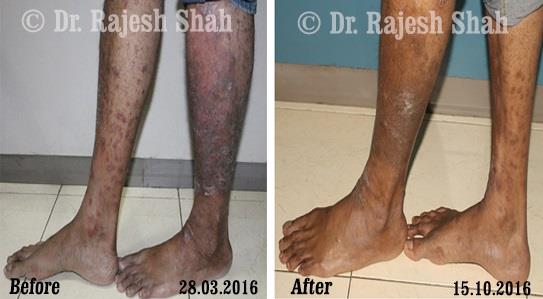
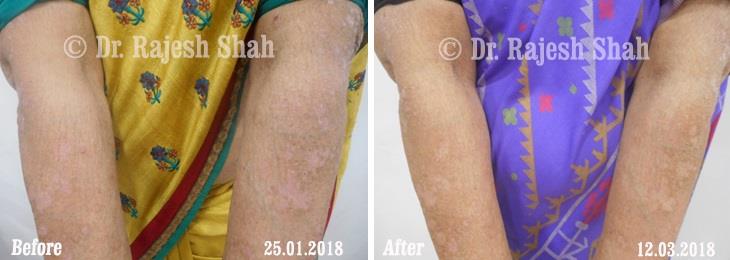
Case Studies

Psoriasis
Homeopathy Healed 5 Years Chronic Psoriasis Patient In Just 9 Months
A 32-year-old female, Mrs. J.Y.J. (PIN: 42631) approached Life Force on 14th February 2020 with the complaints of Psoriasis that she…

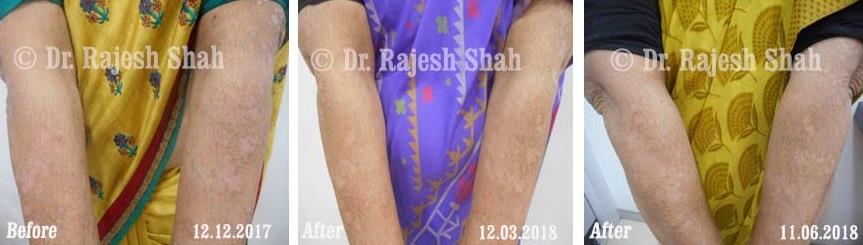
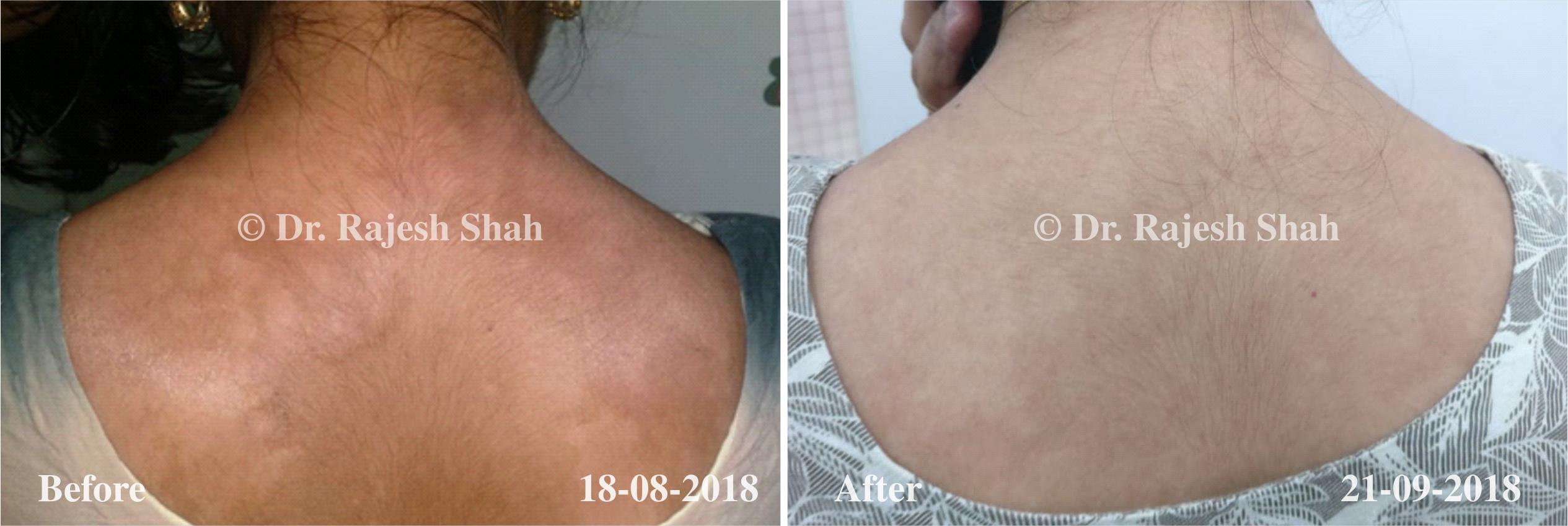
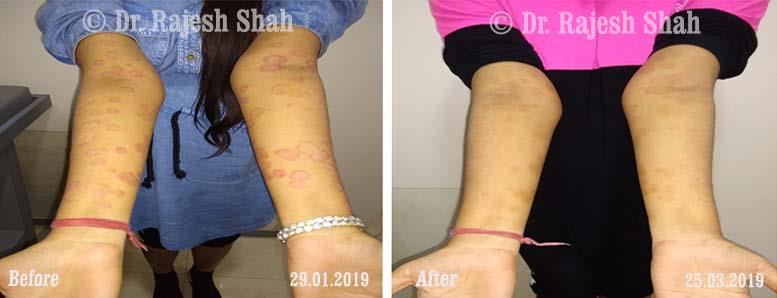
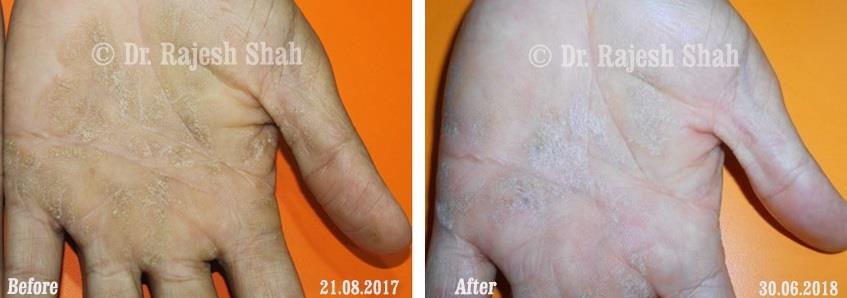
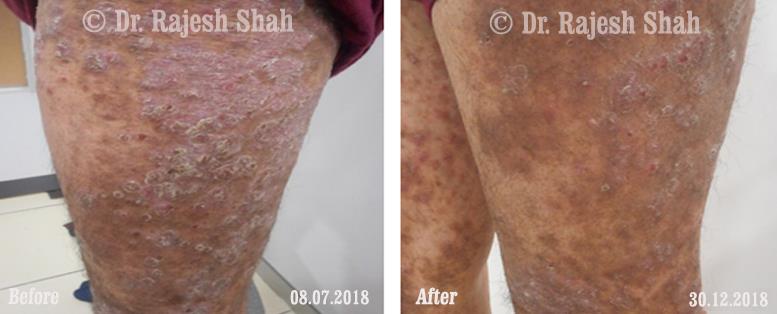
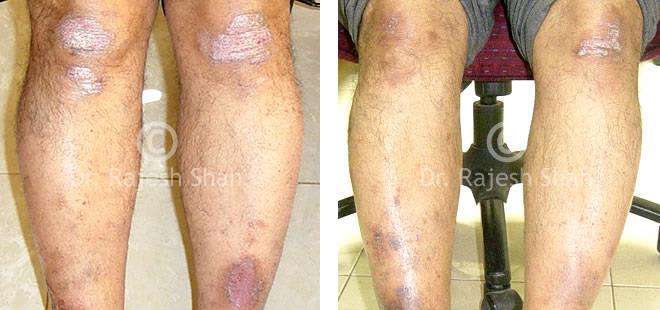
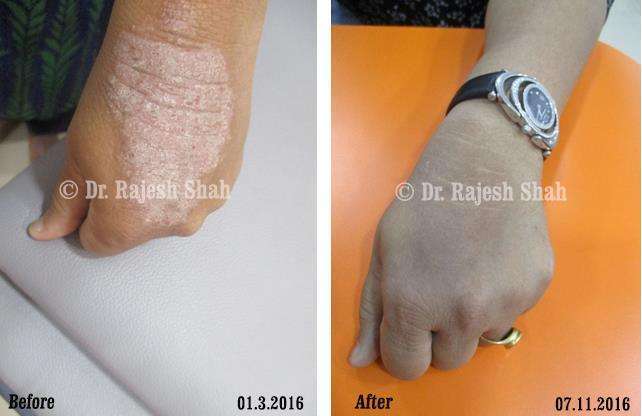
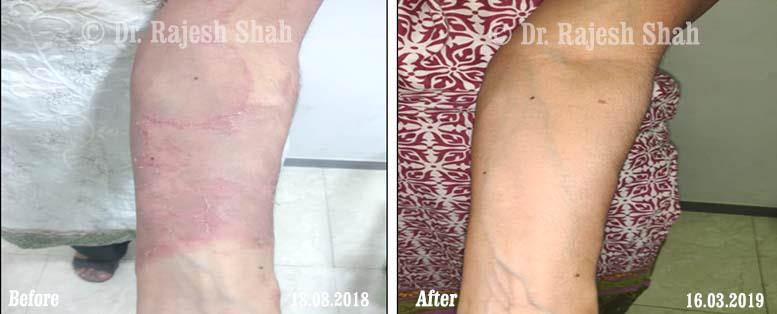
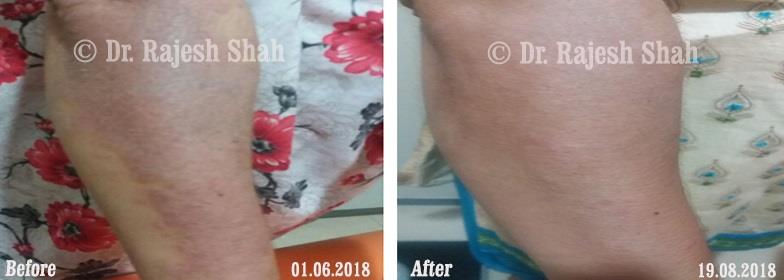
Psoriasis
An Early Diagnosed Psoriasis Patient Experienced 90% Healing With Homeopathy
A 58-year-old lady, Mrs. H.B. (PIN: 42999) visited Borivali Clinic of Life Force on 30th April 2020 for the treatment of…

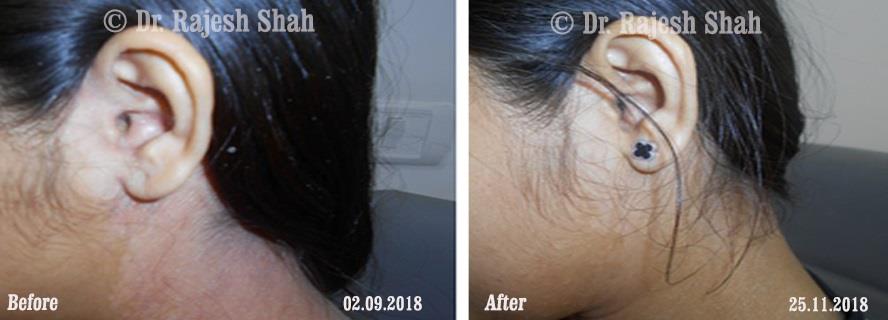
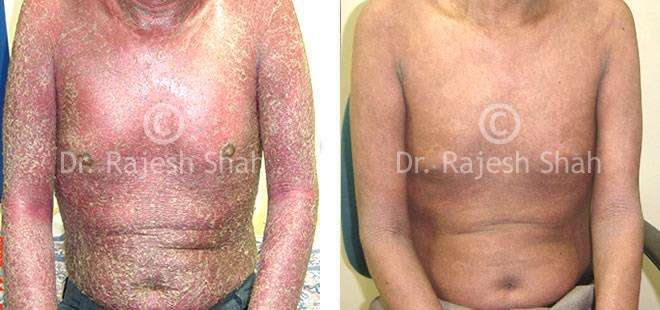
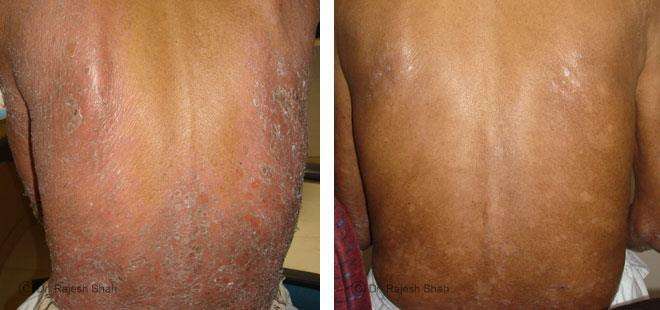
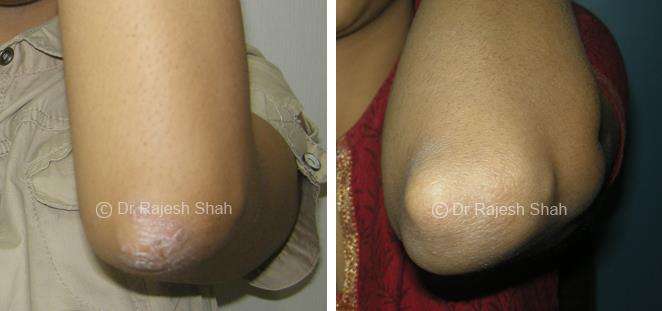
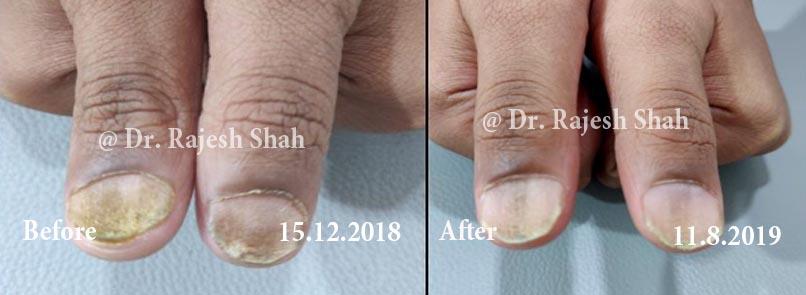
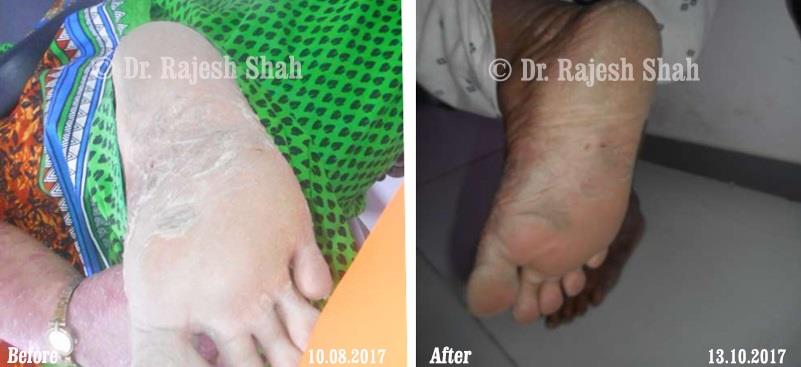
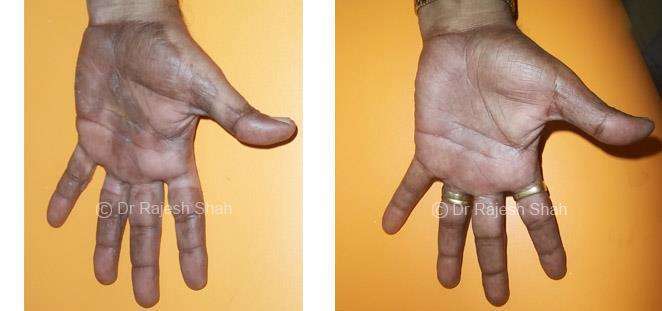
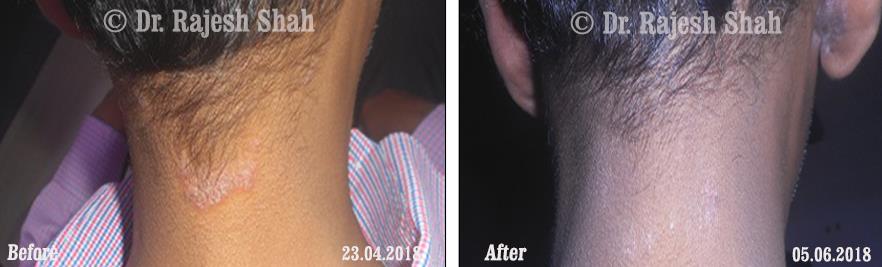
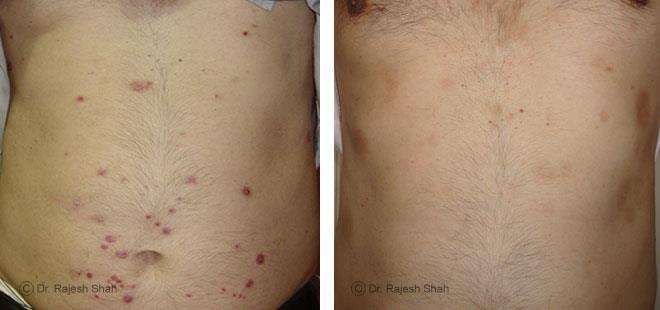
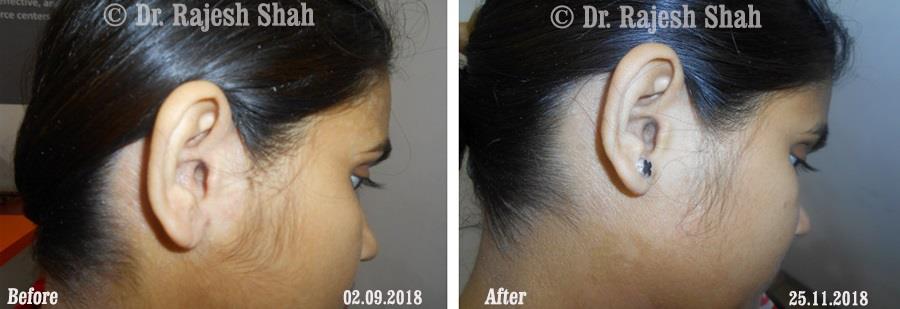
Psoriasis
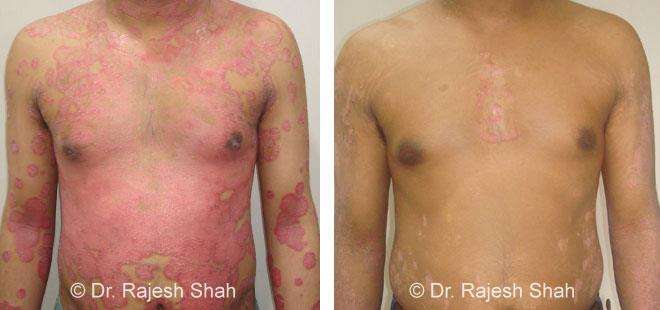
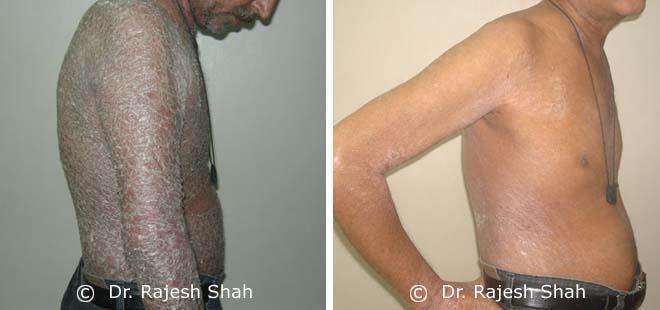
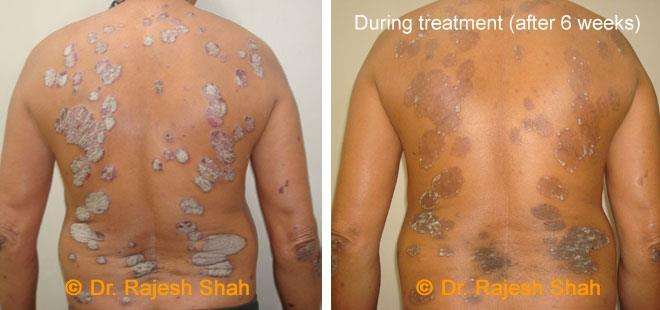
Chronic Plaque Psoriasis Wonderfully Healed With Dr. Shah’s Homeopathy
Psoriasis is an autoimmune disease. There are different types of psoriasis, and plaque psoriasis is one of its types. It…
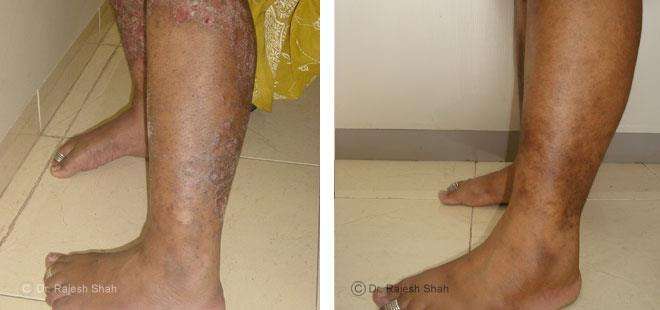
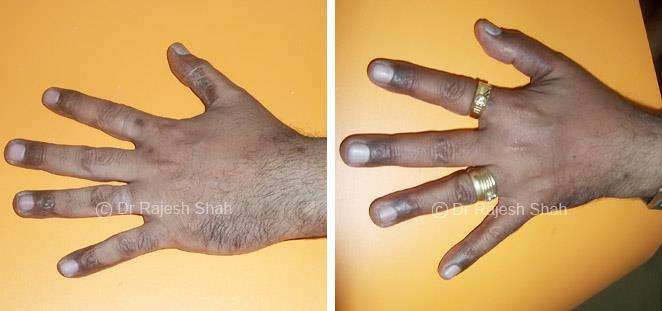
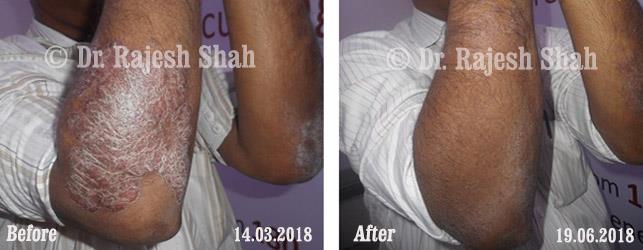
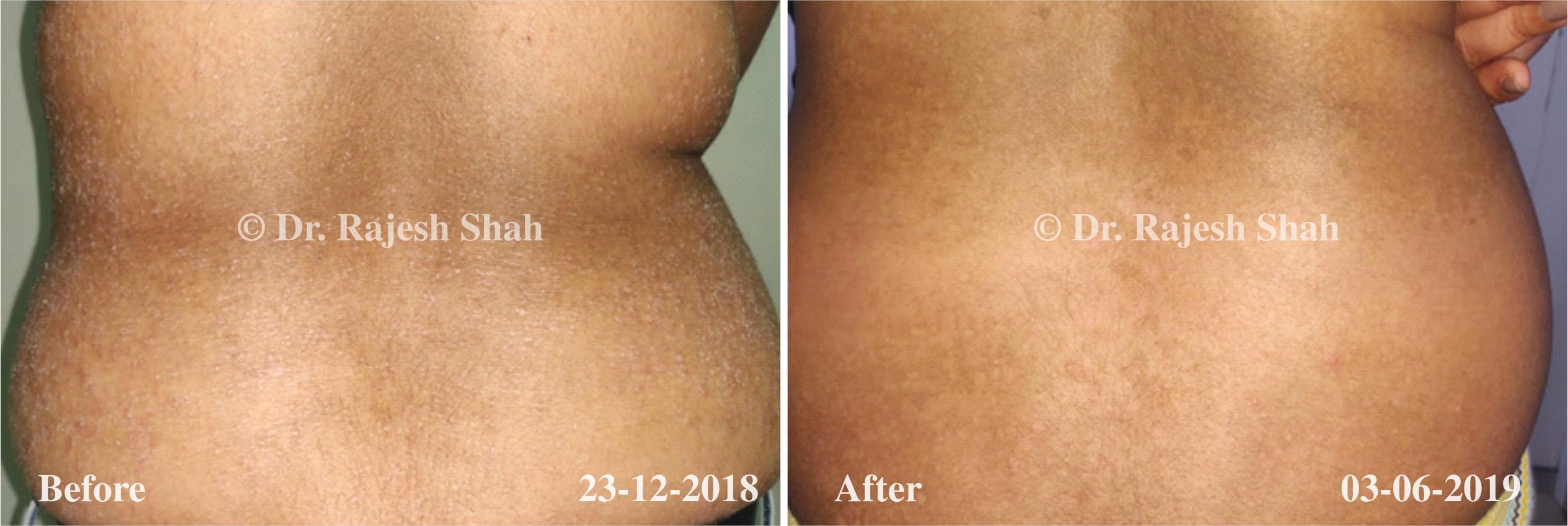
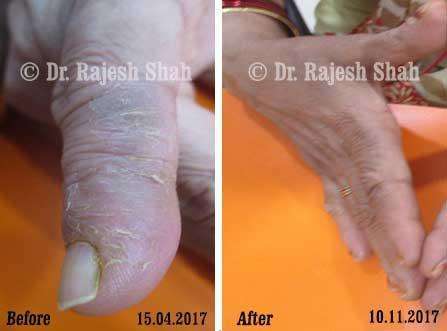
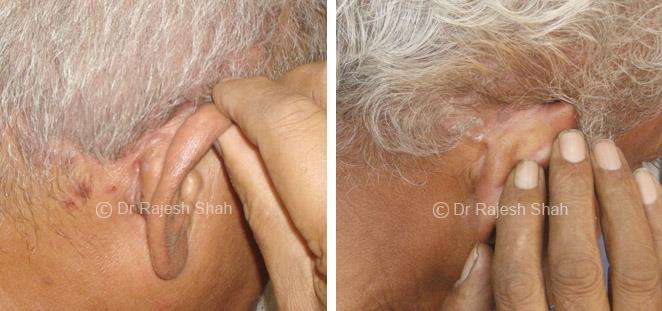
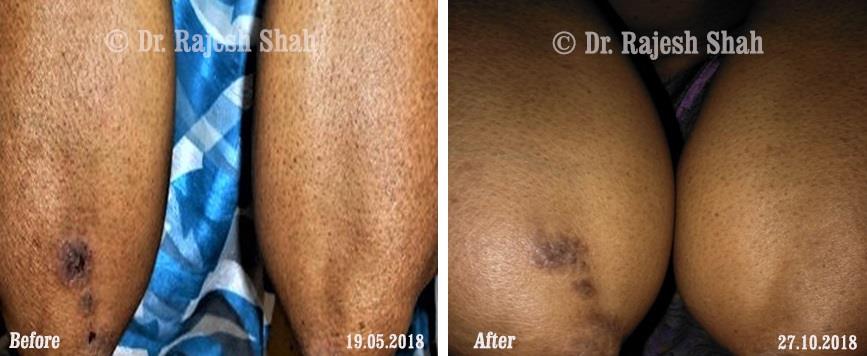
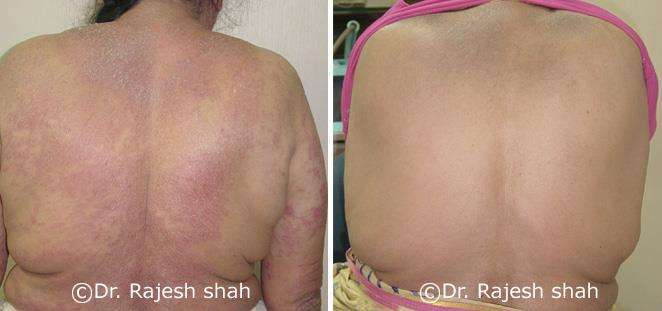
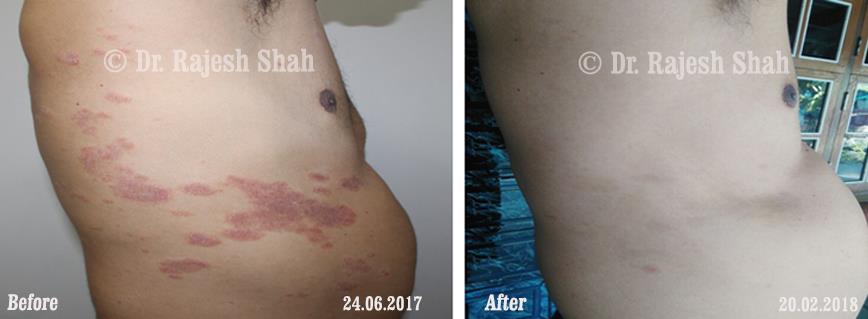
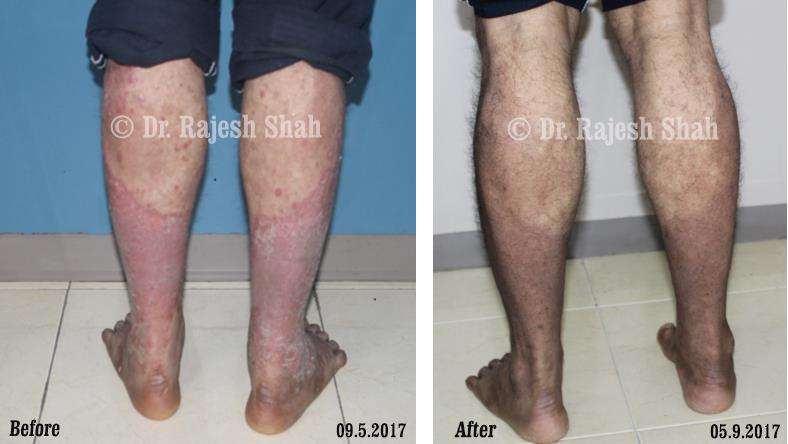
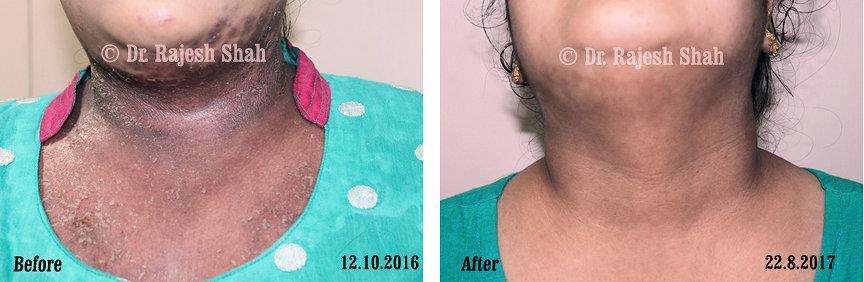
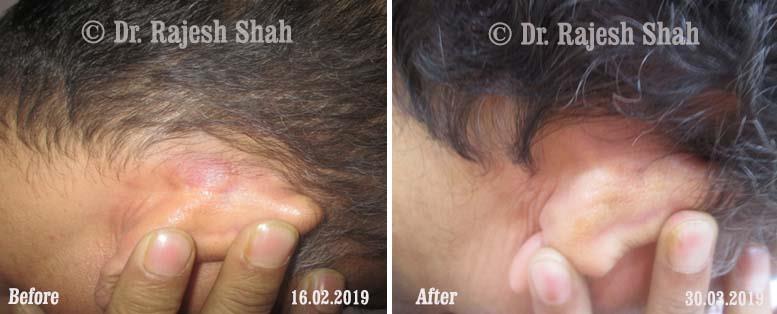
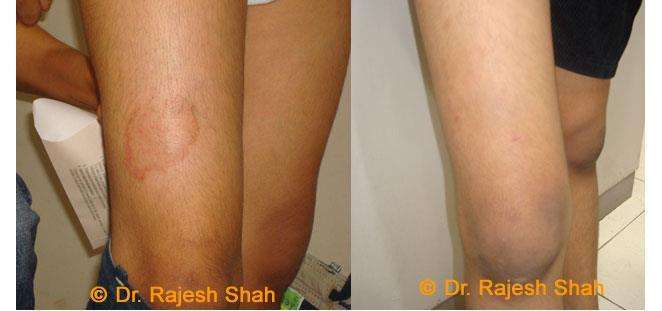
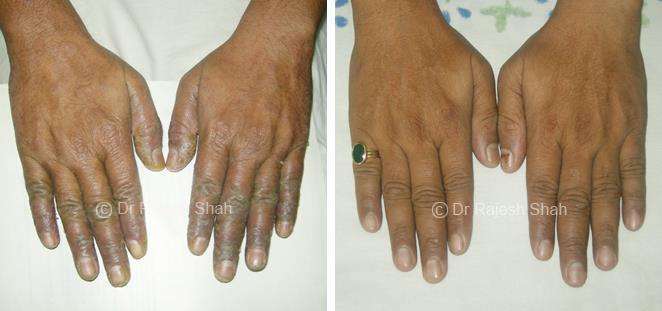
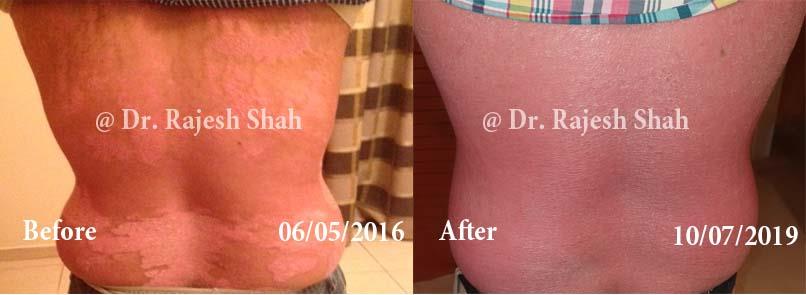
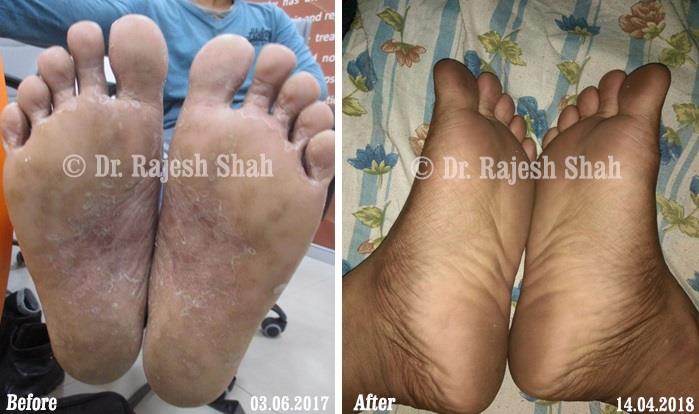
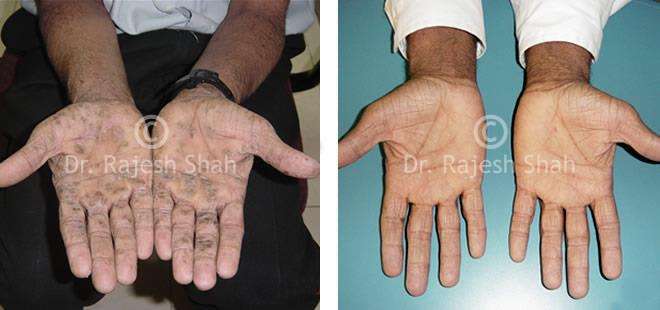
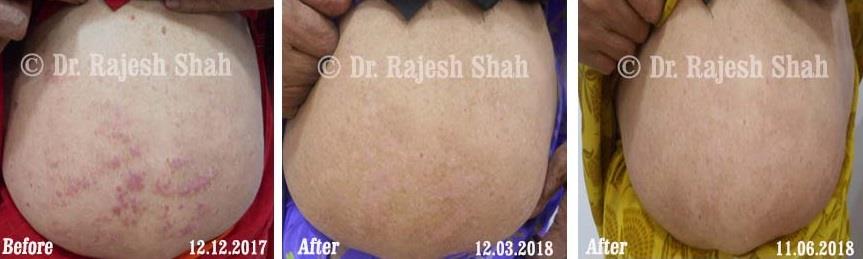
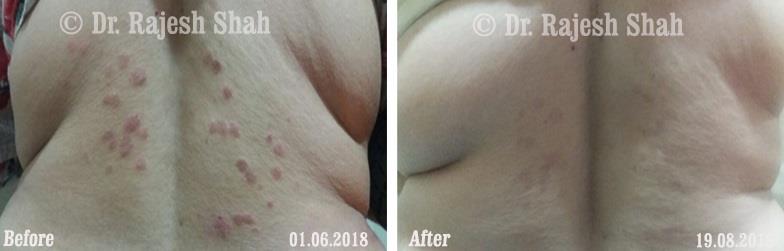
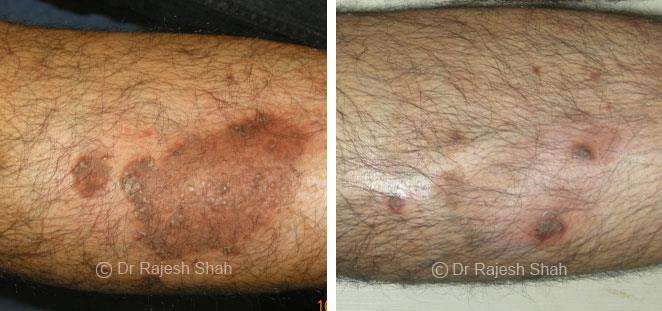
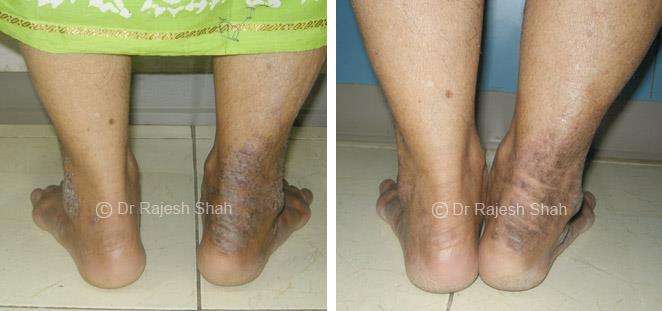
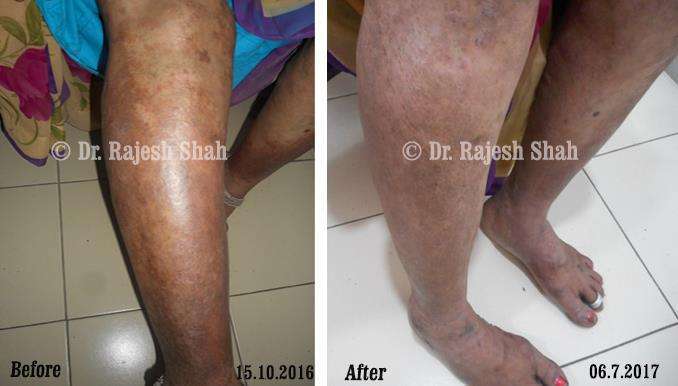
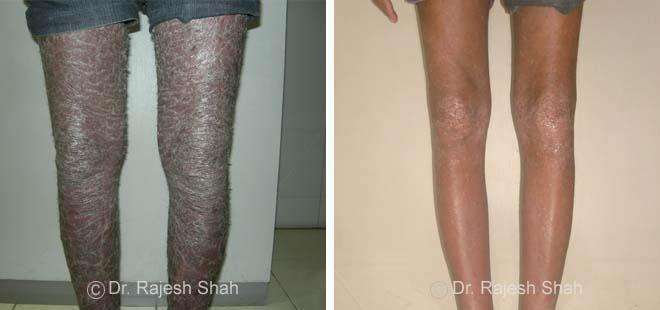
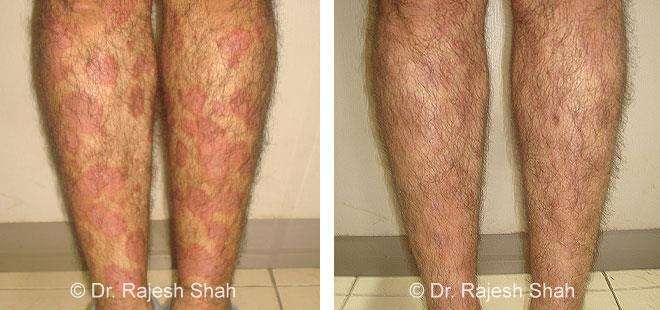
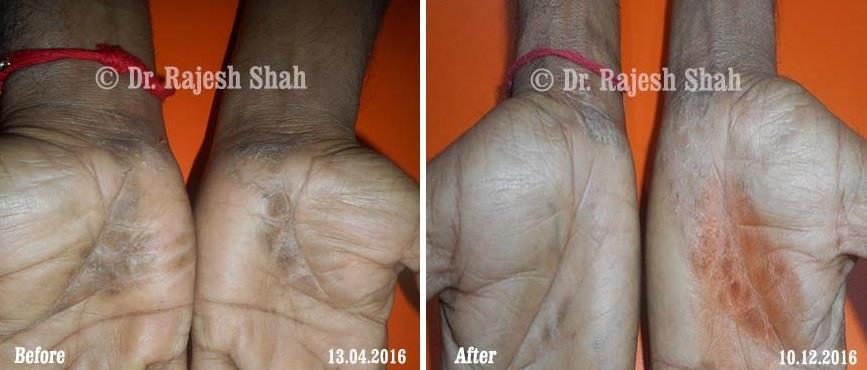
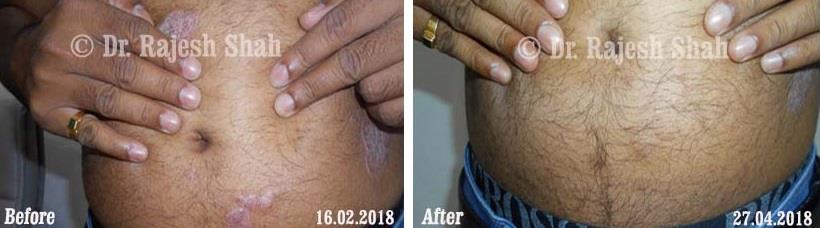
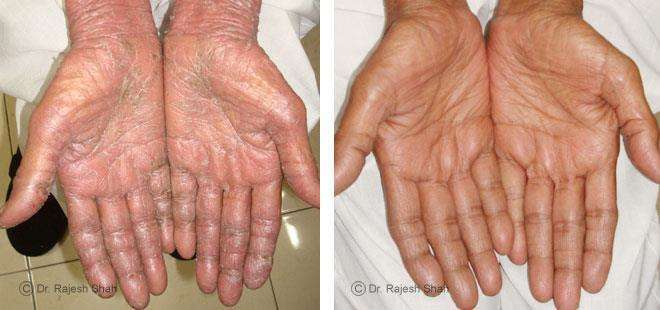
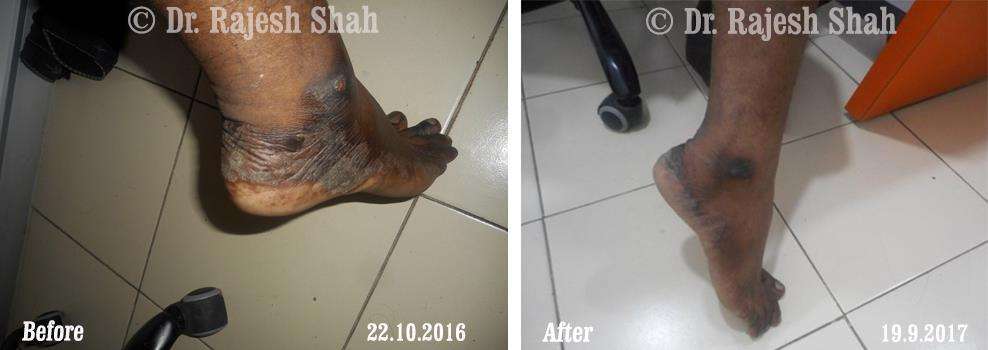
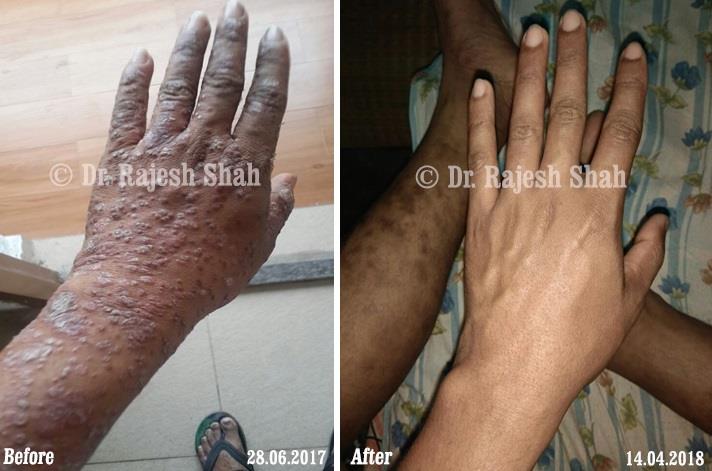
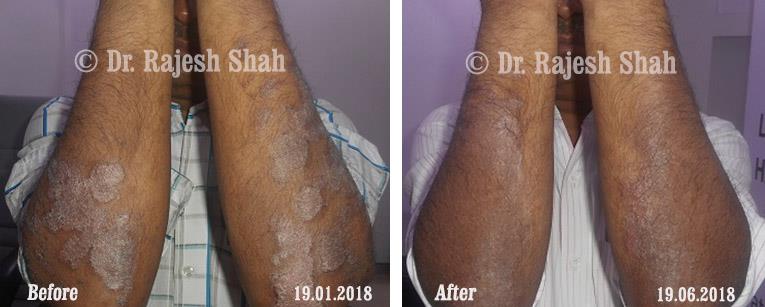
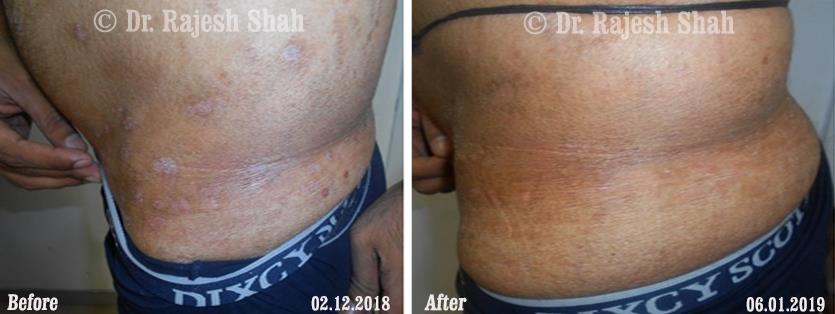
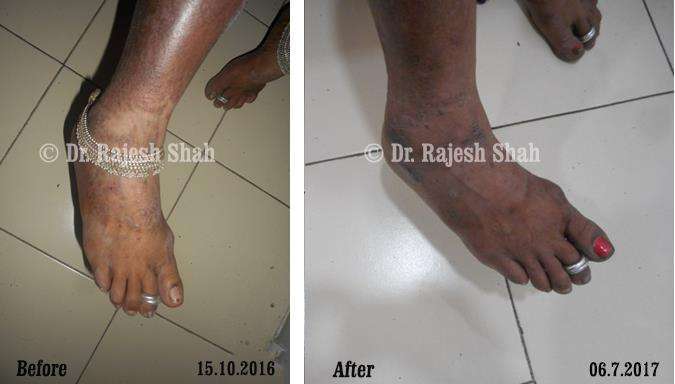
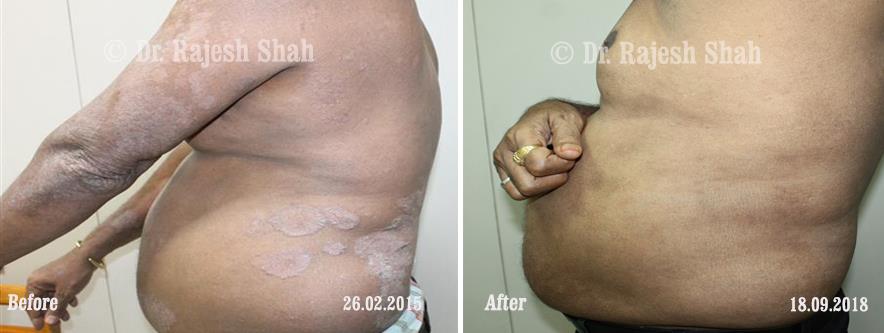
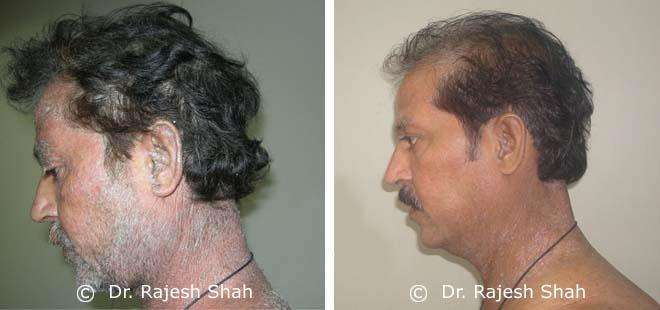
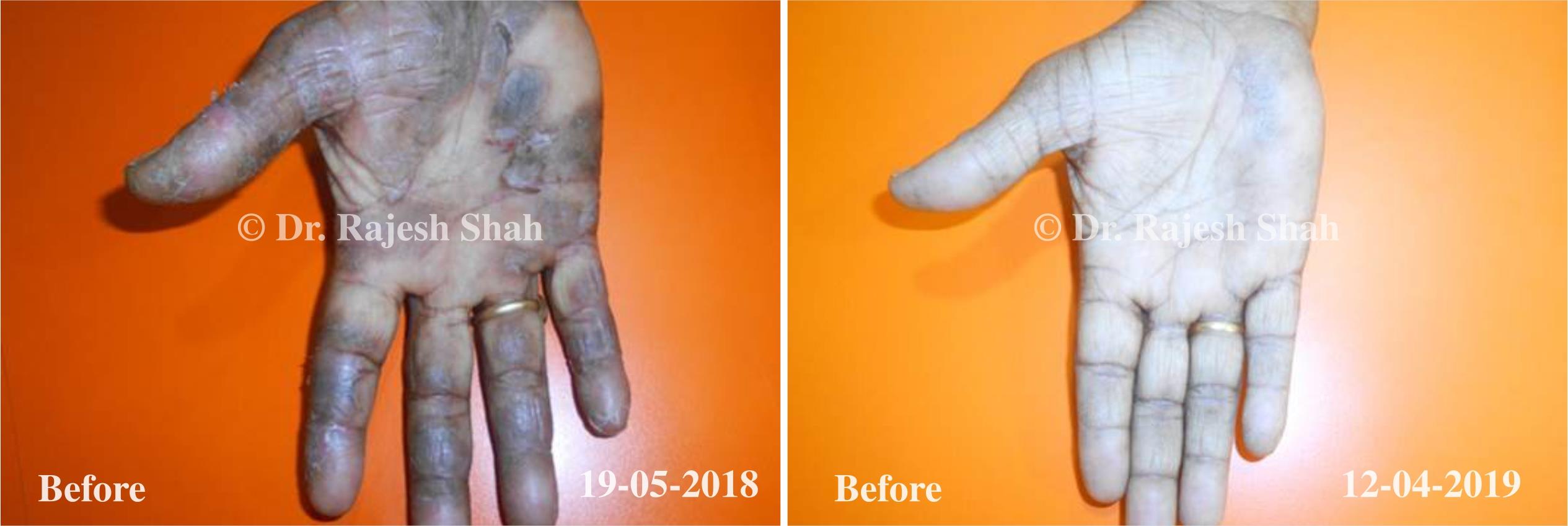
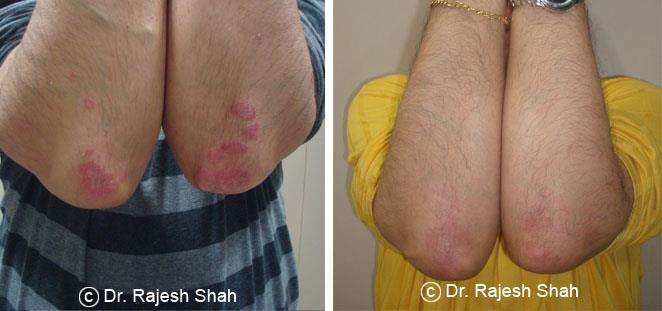
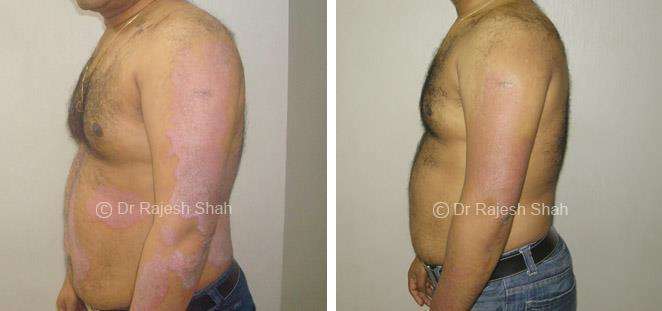
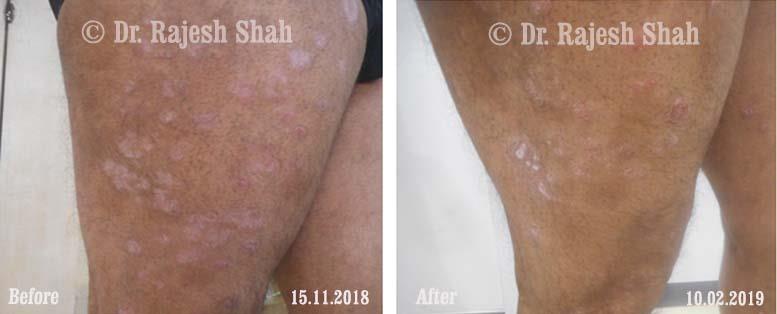
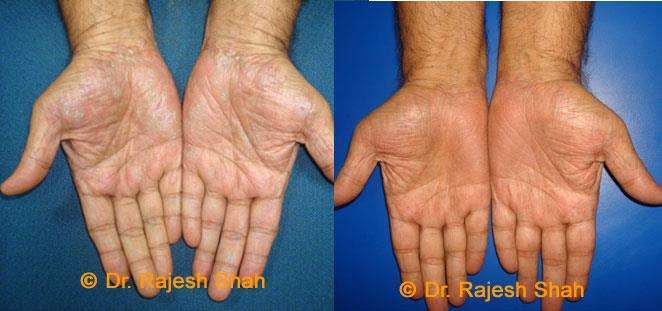
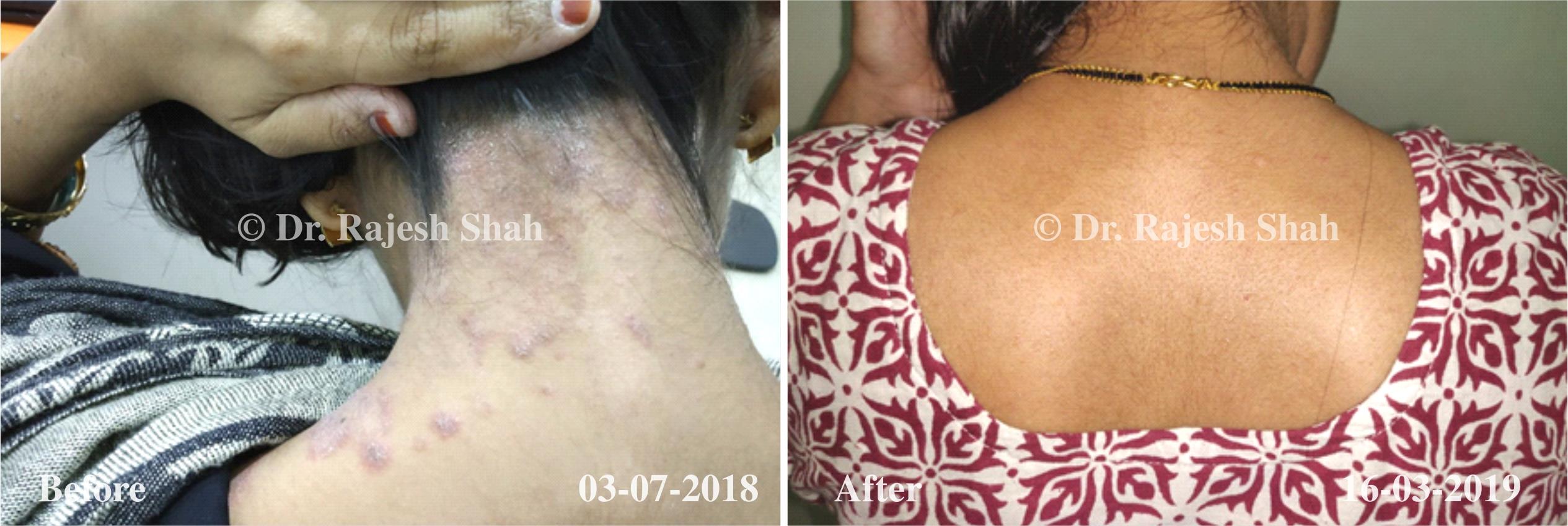
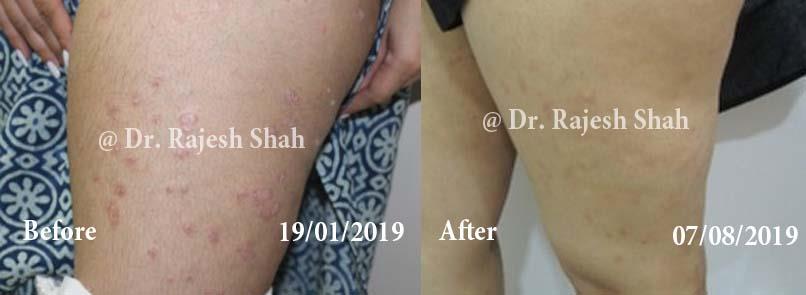
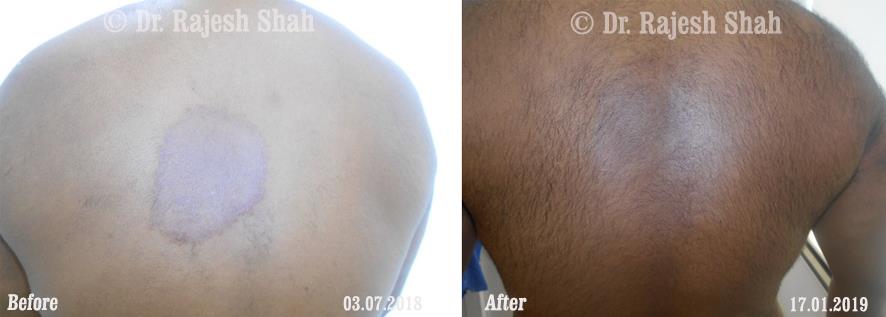
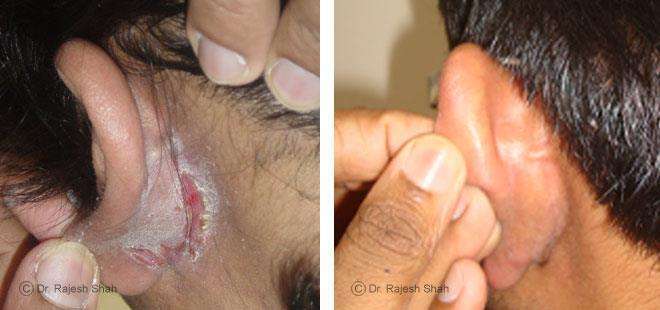
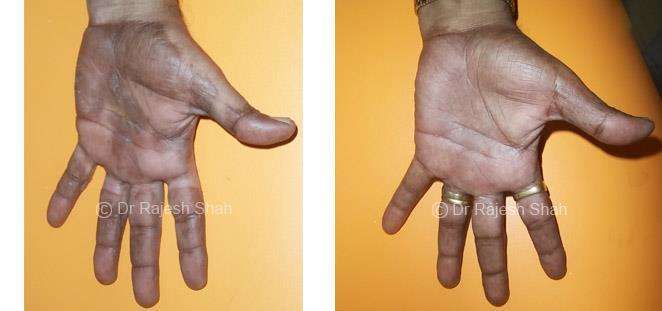
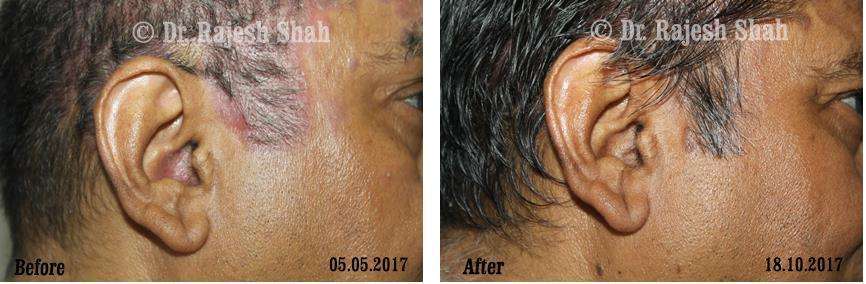
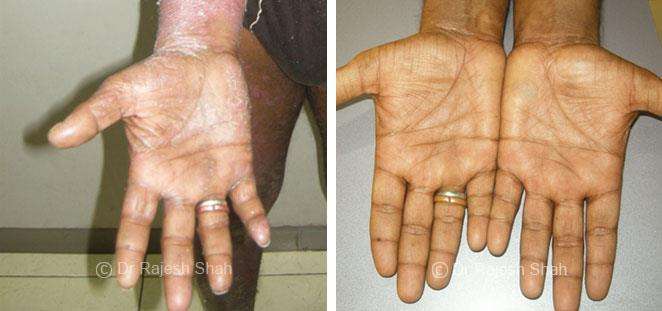
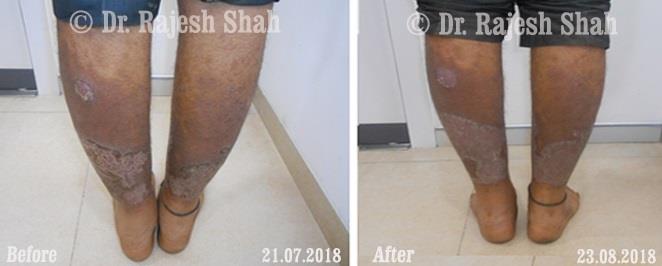
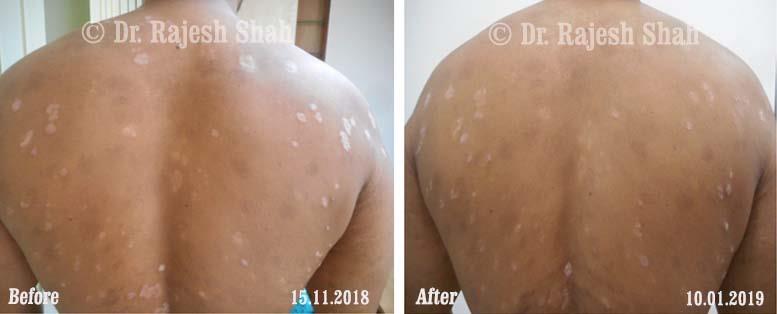
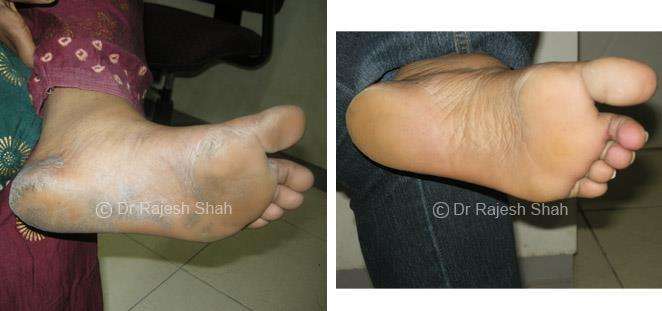
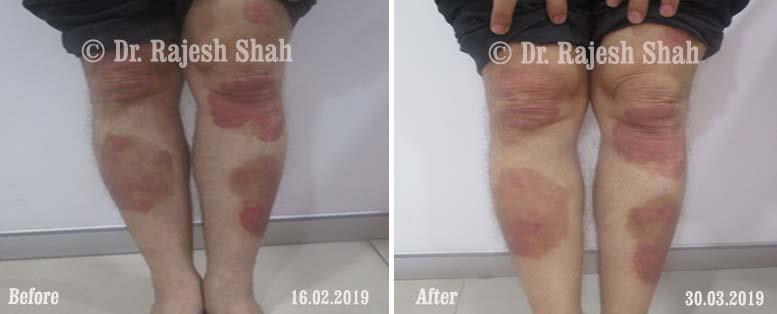
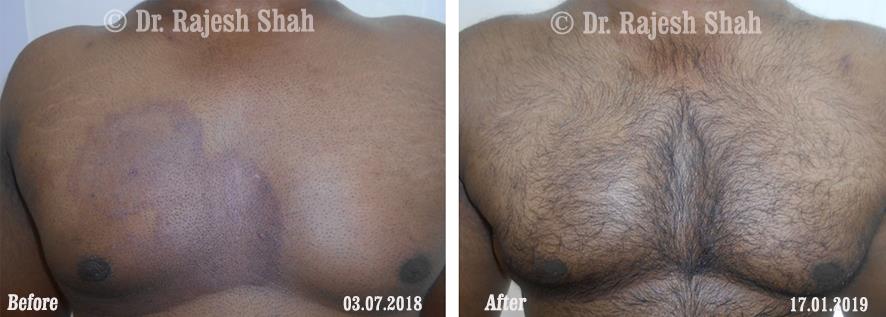
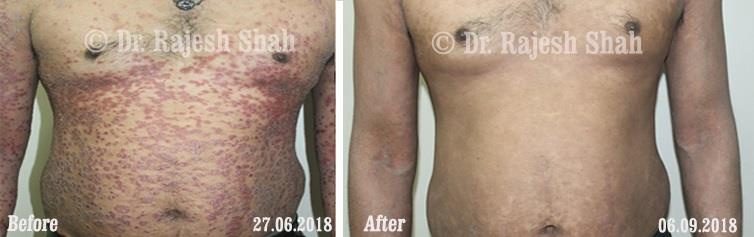
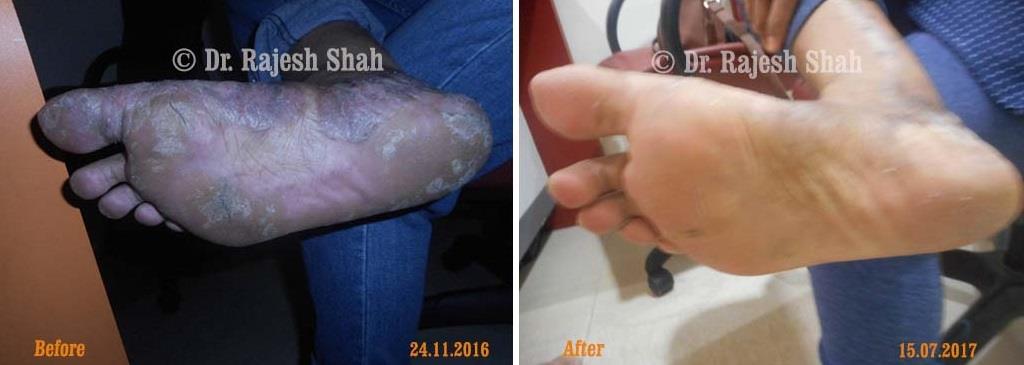
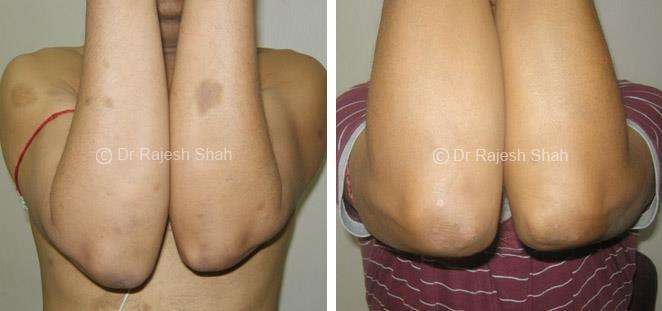
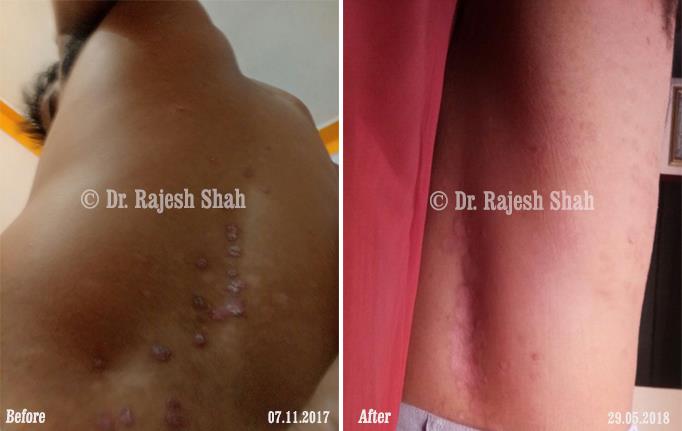
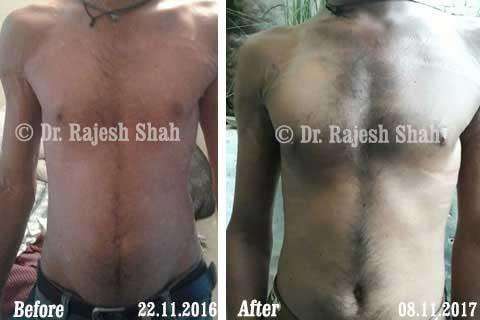
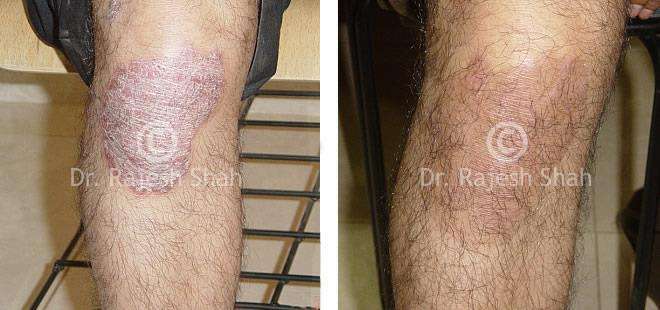
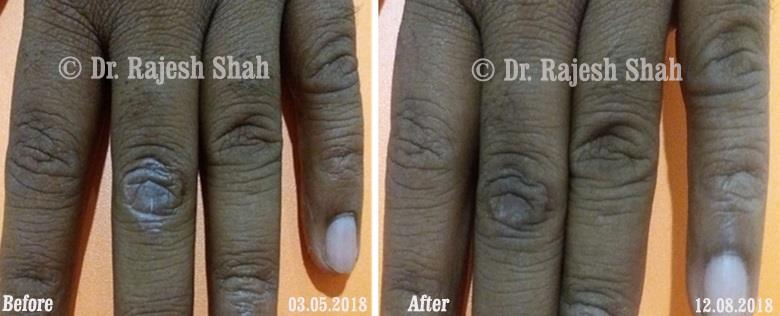
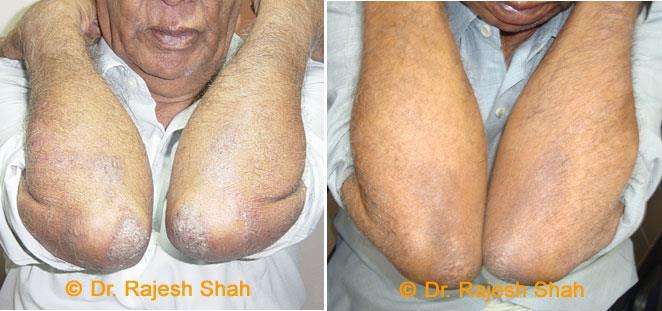
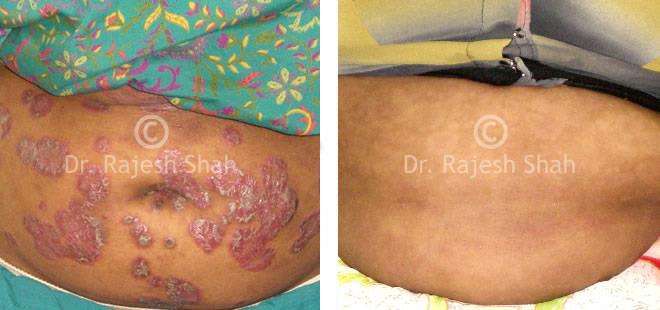
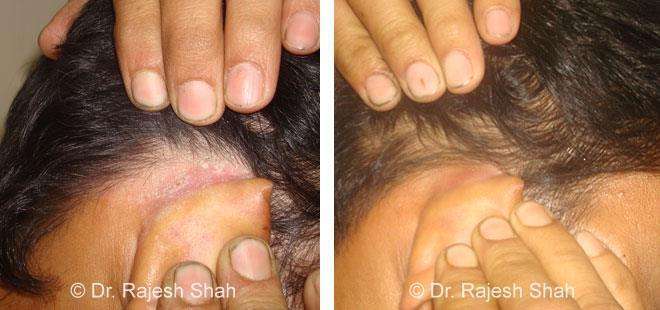
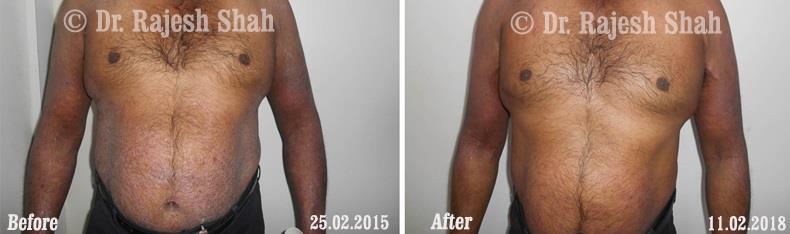
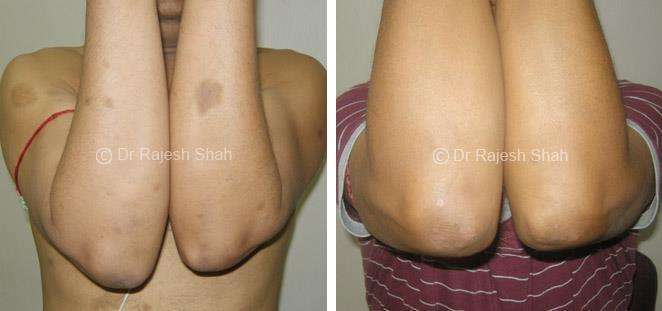
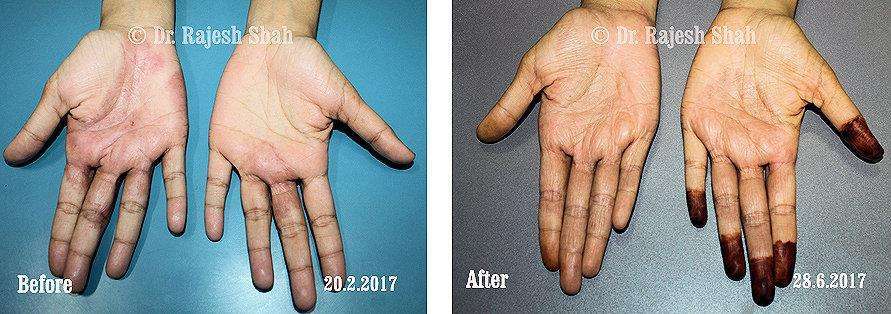
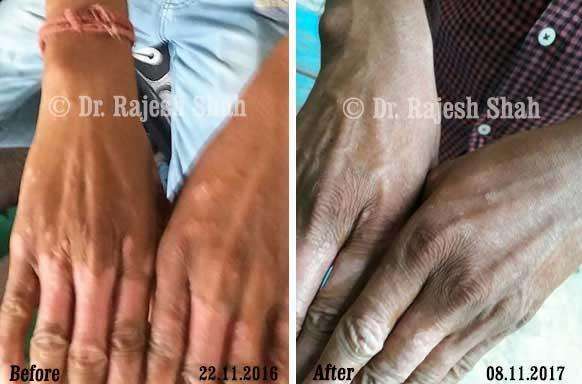
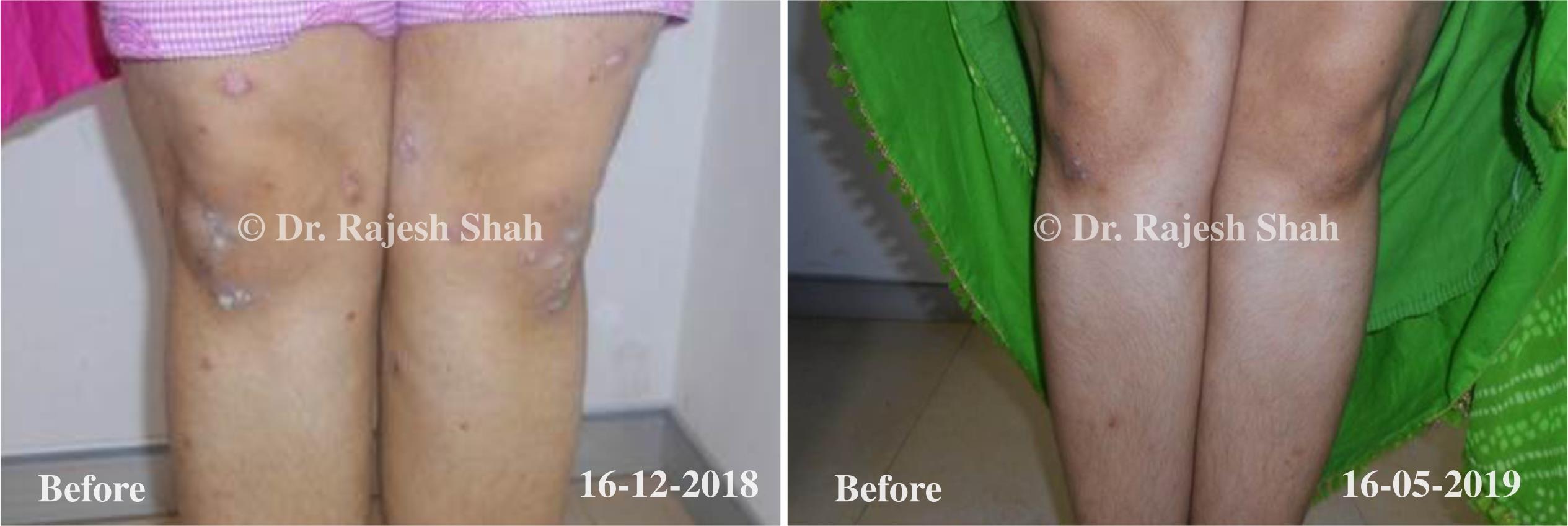
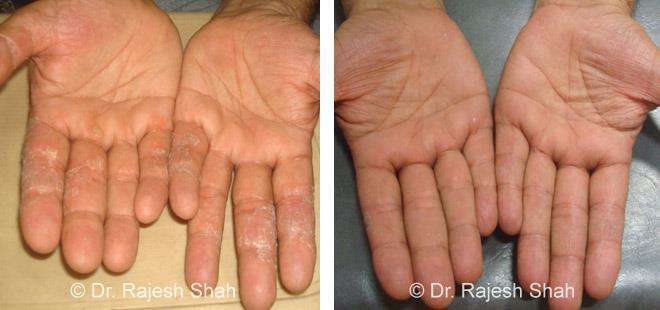
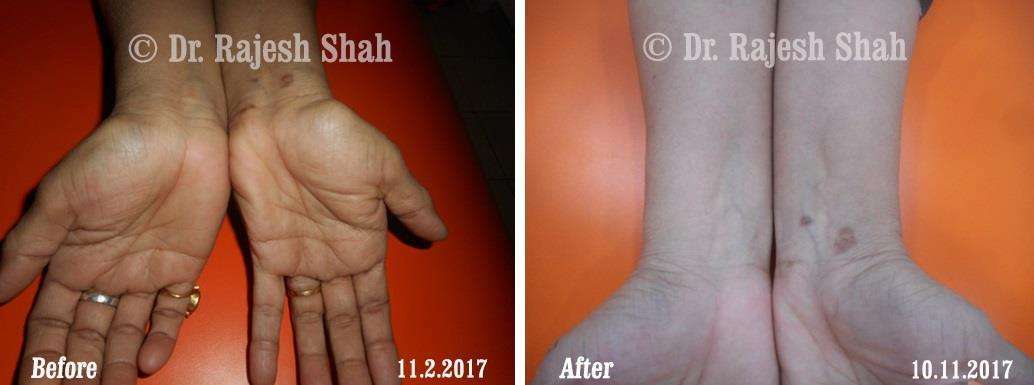
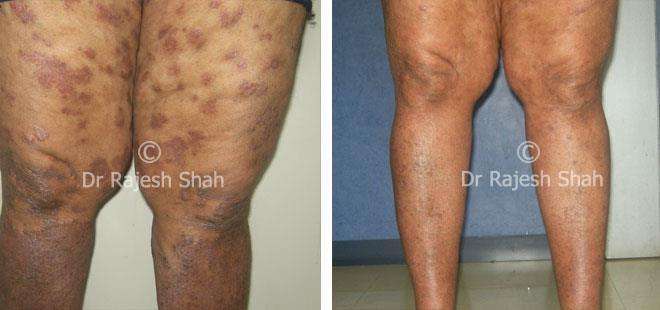
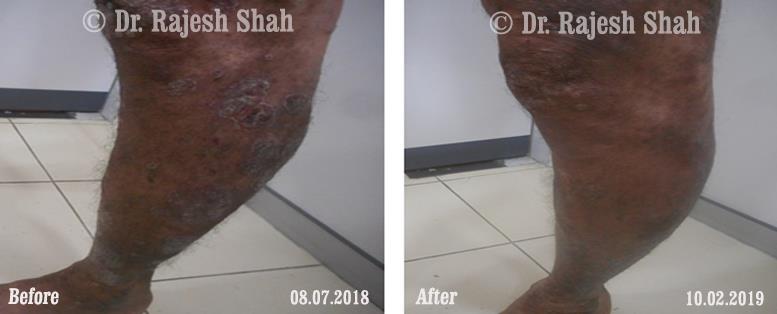
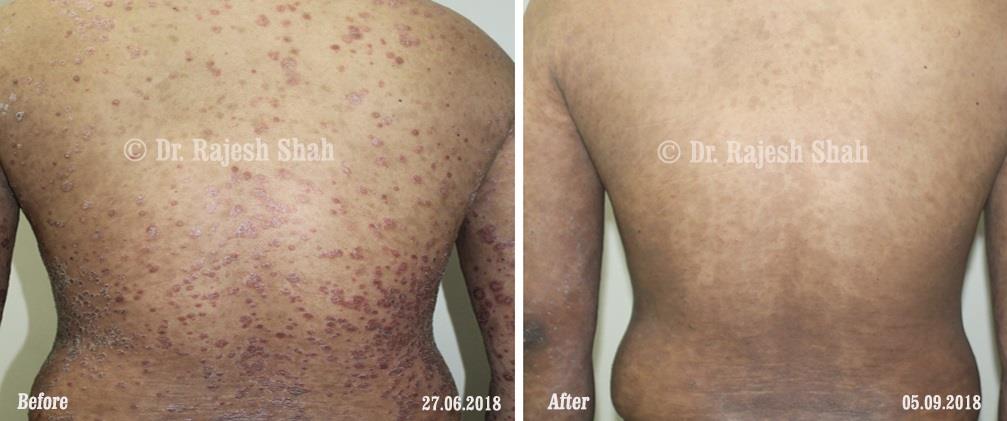
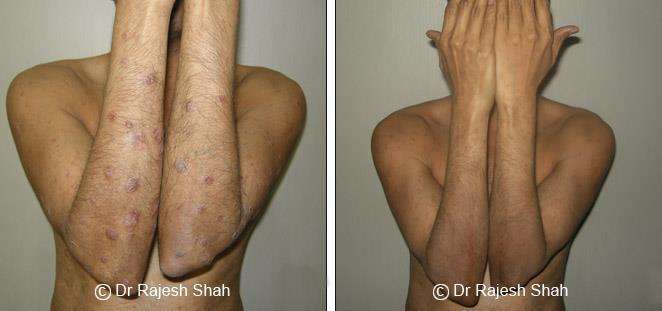
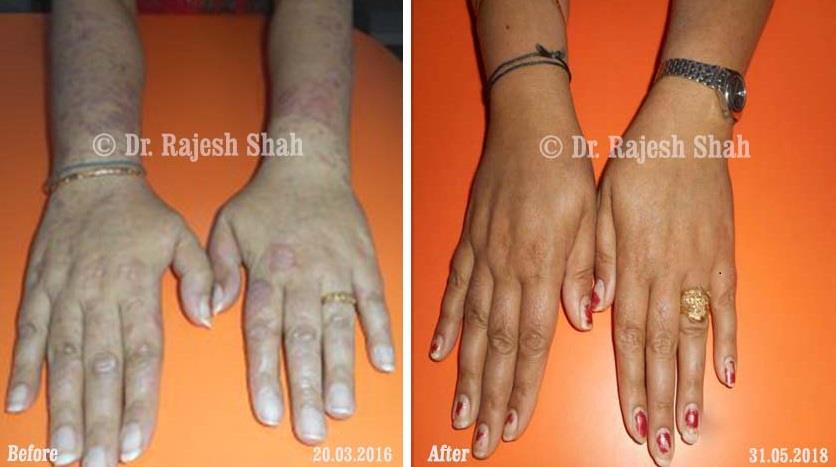
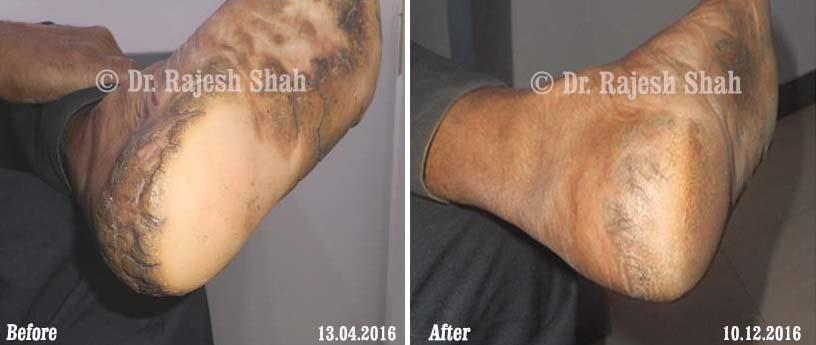
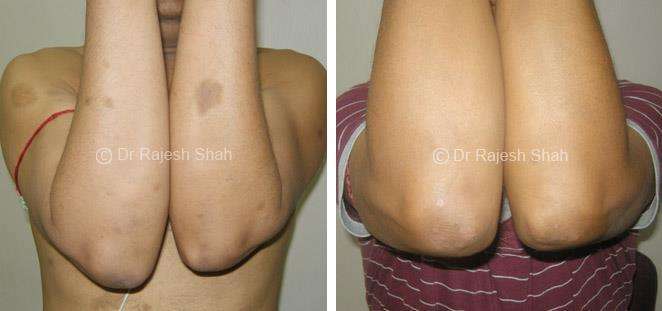
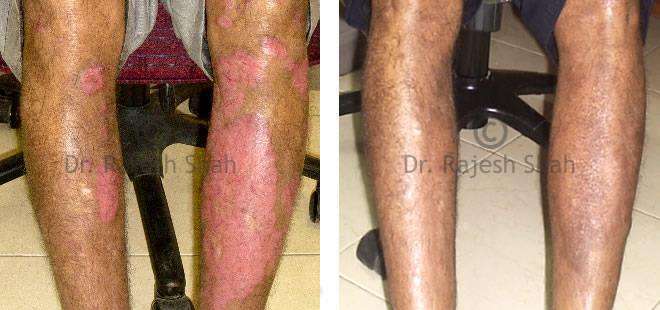
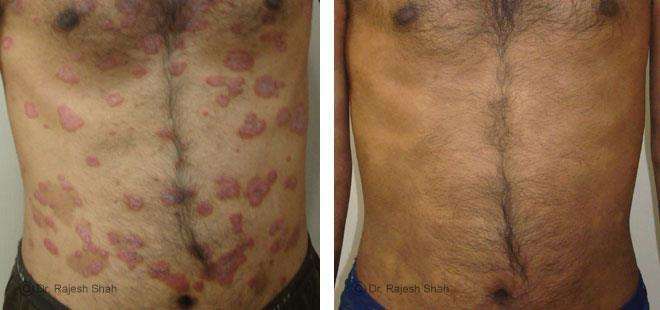
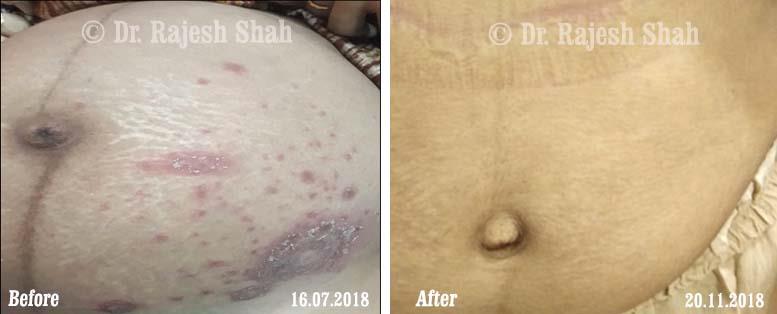
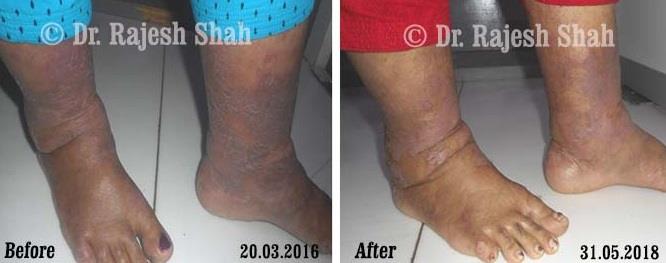
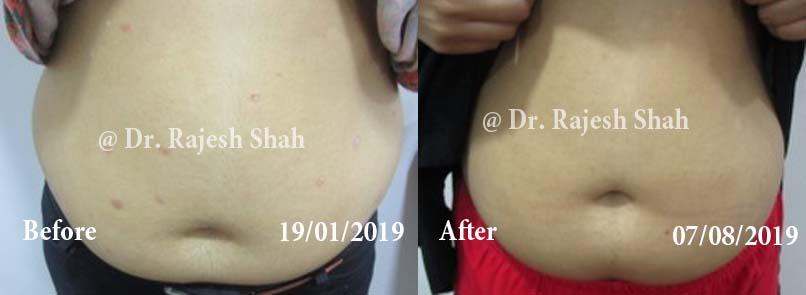
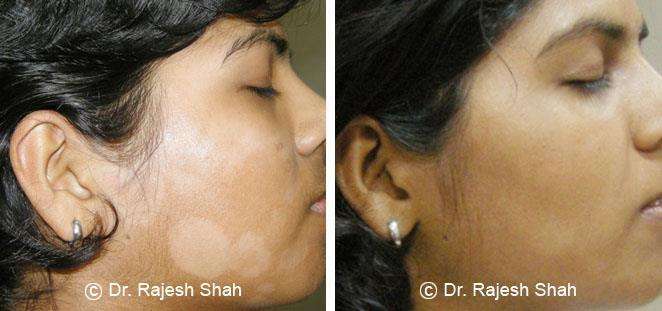
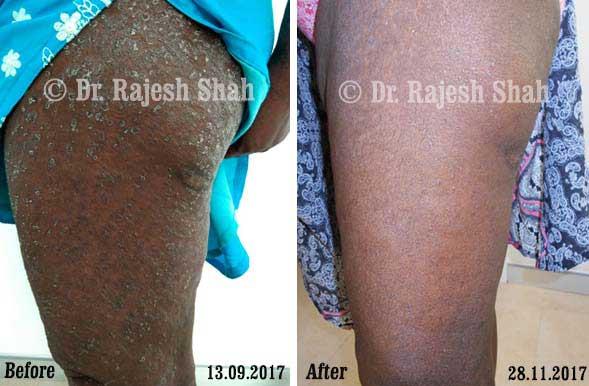
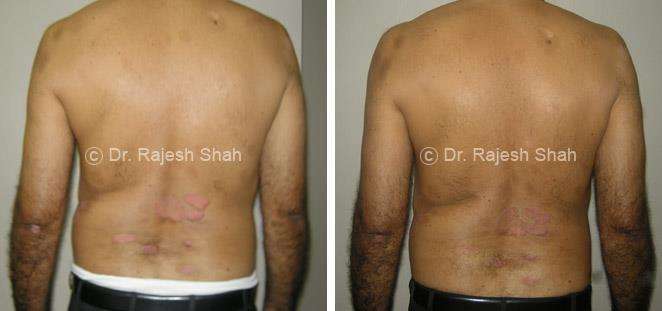
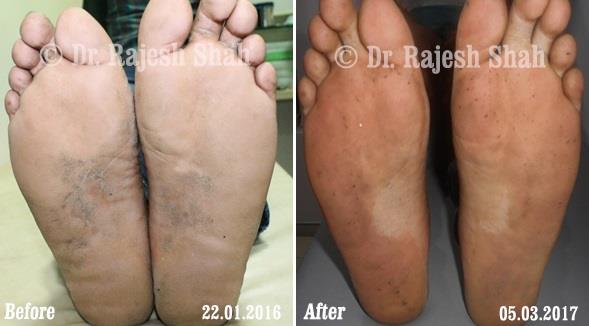
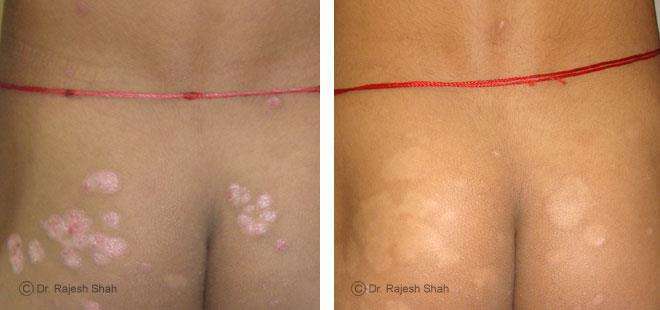
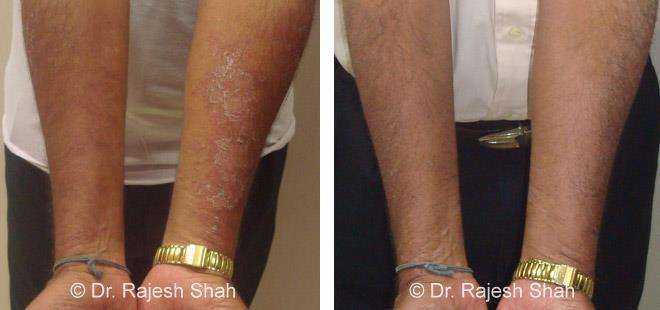
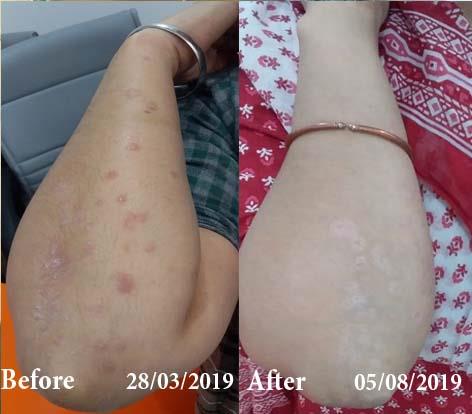
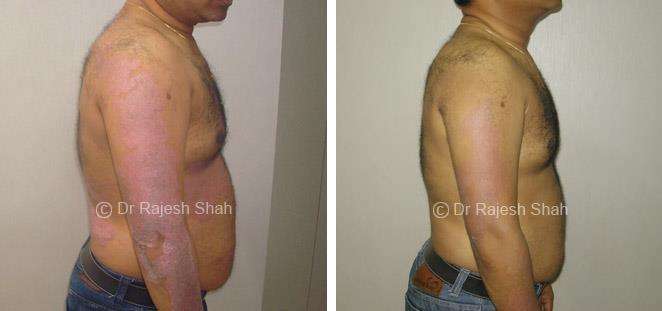
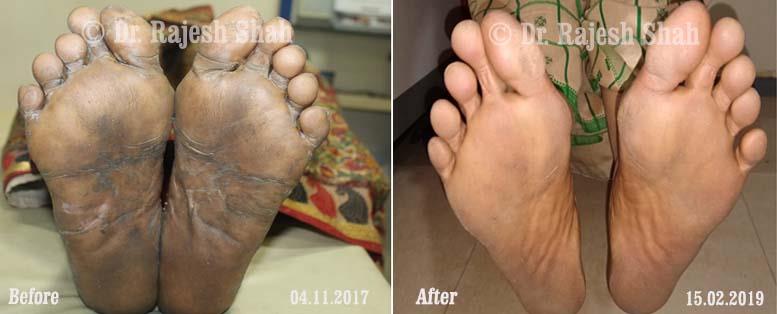
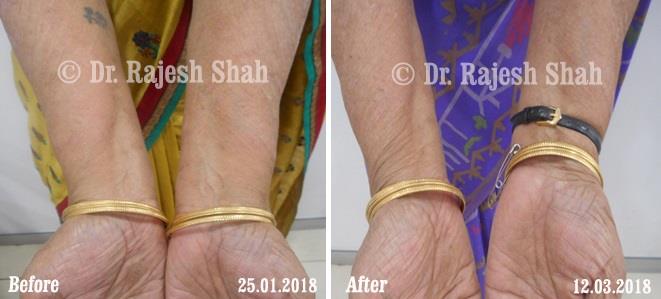
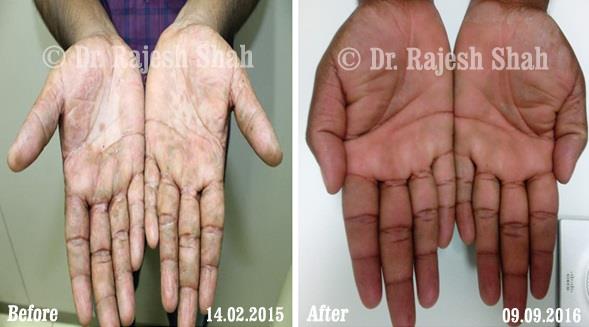
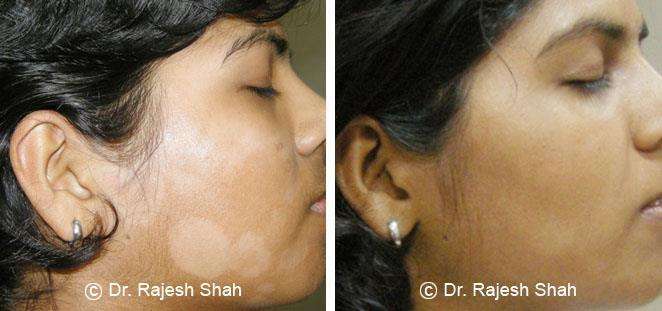
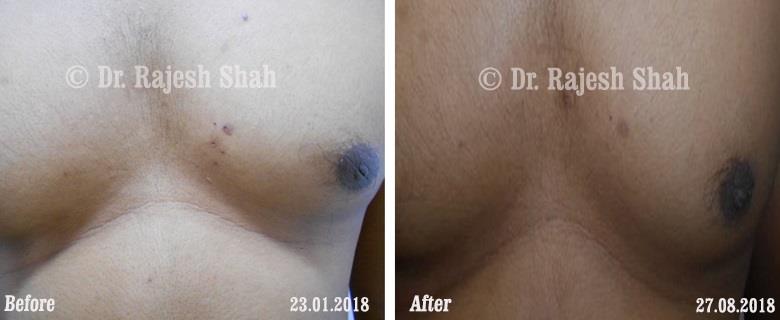
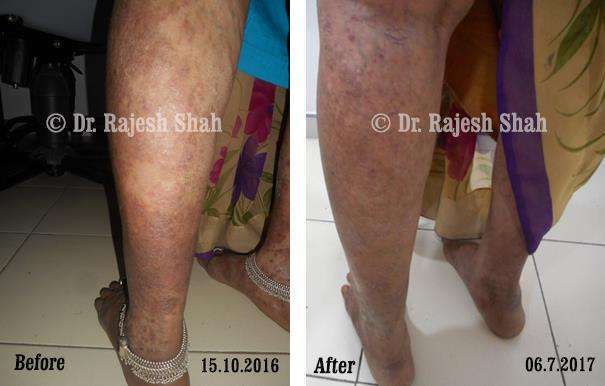
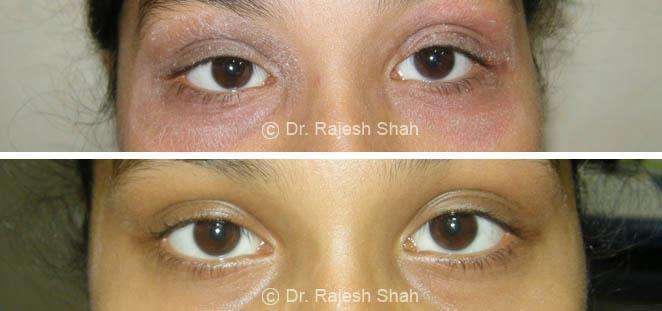
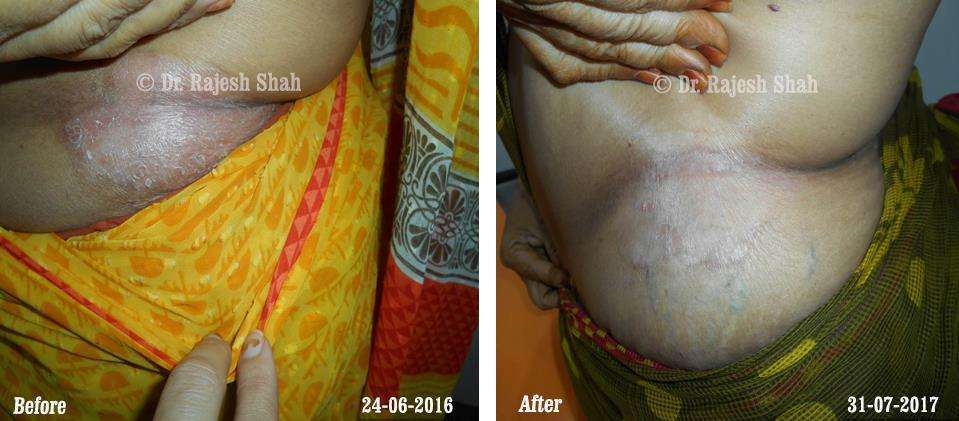
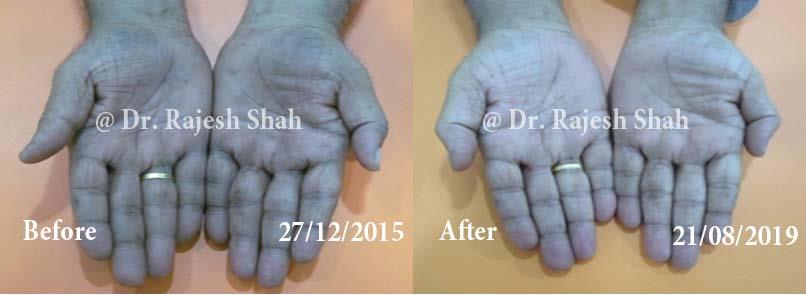
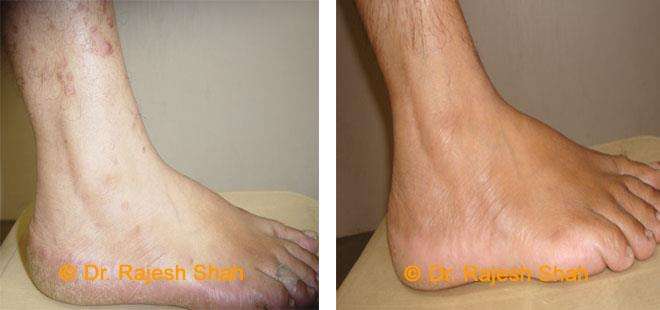
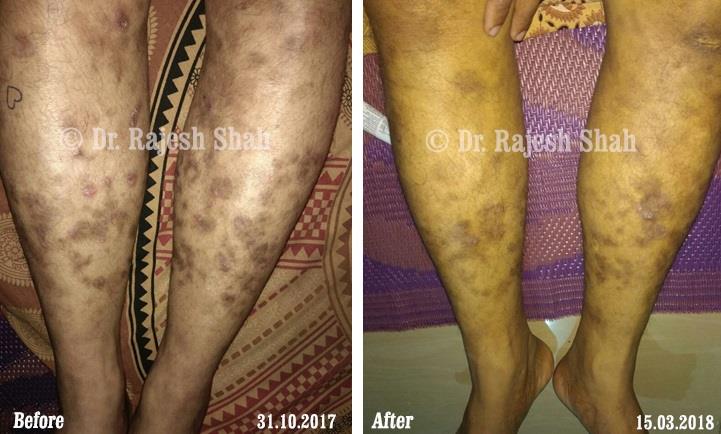
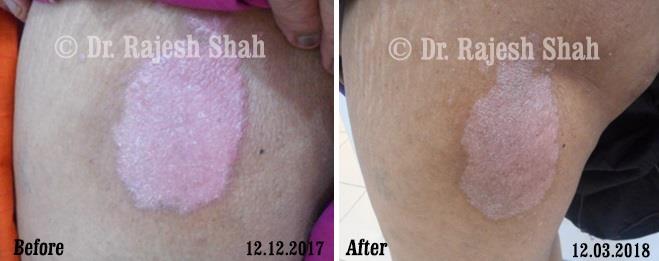
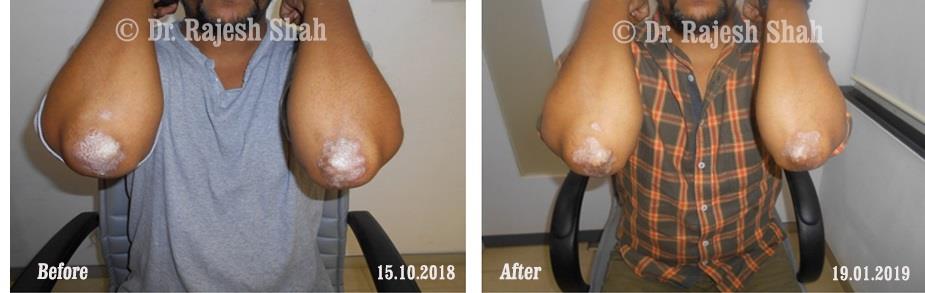
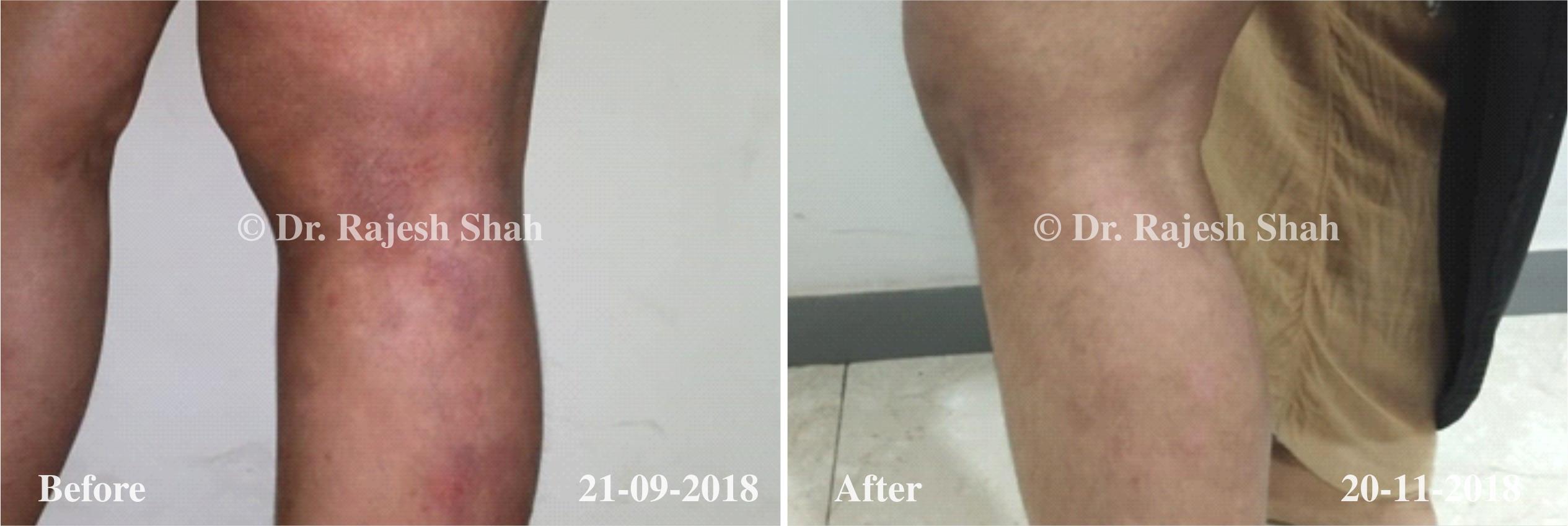
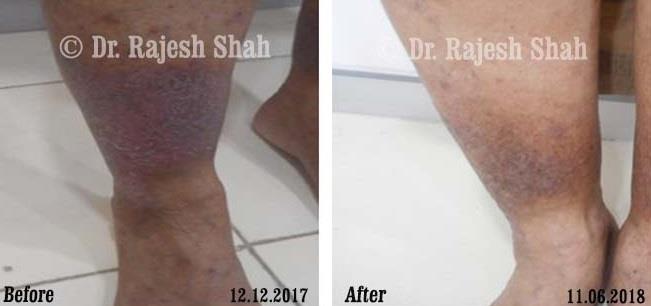
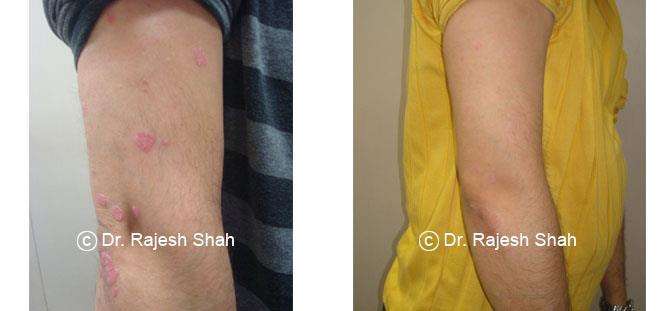
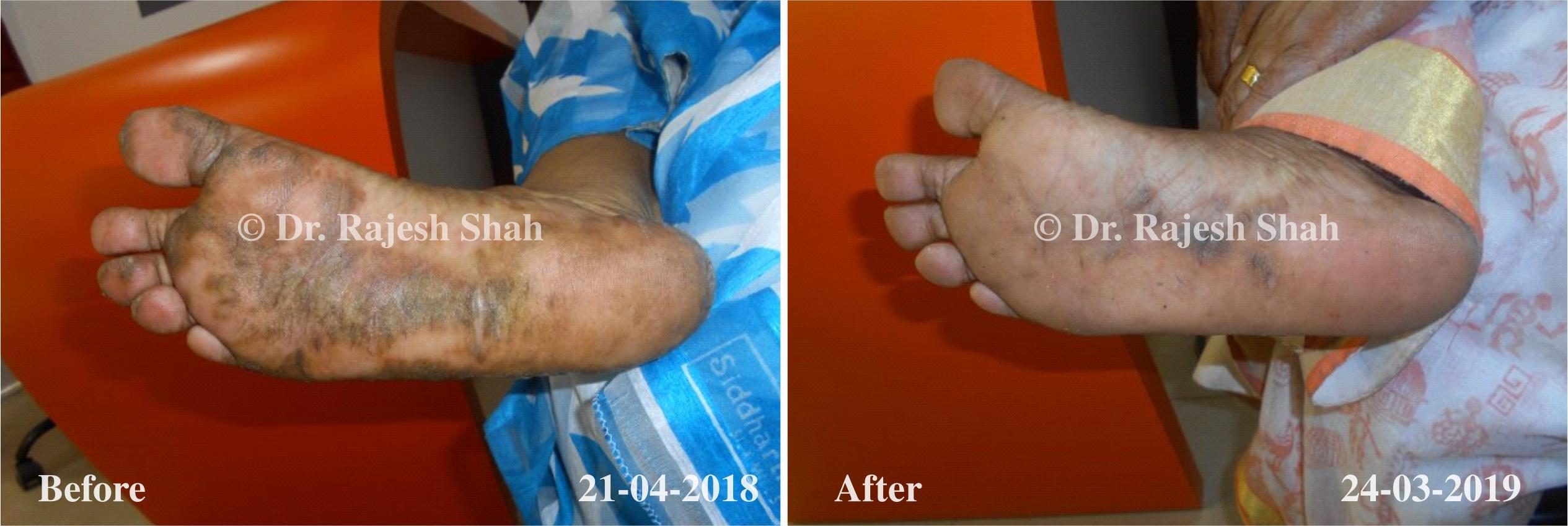
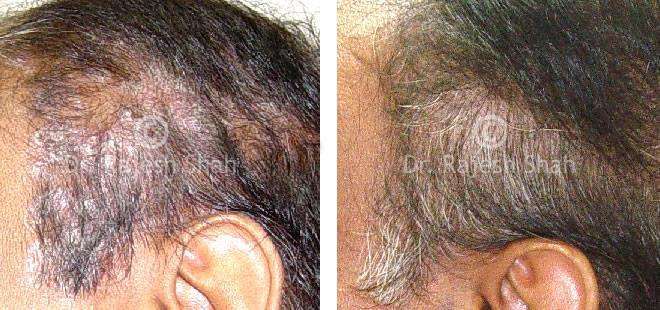
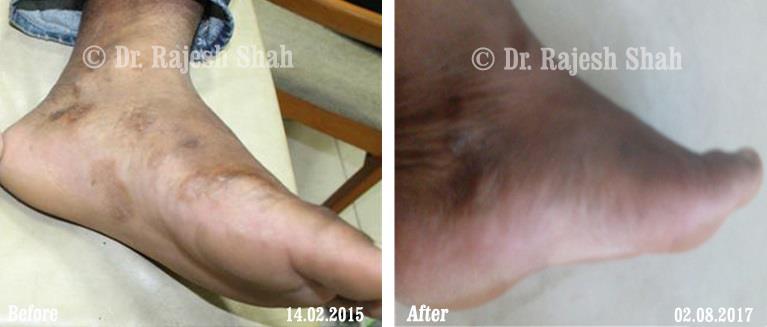
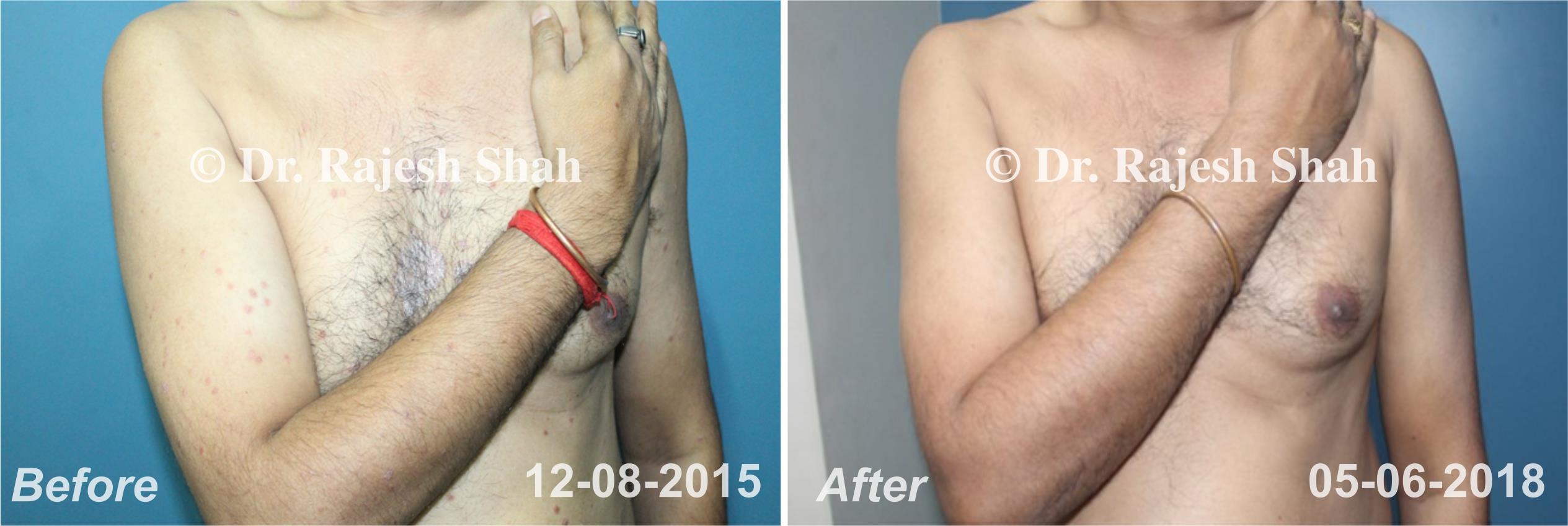
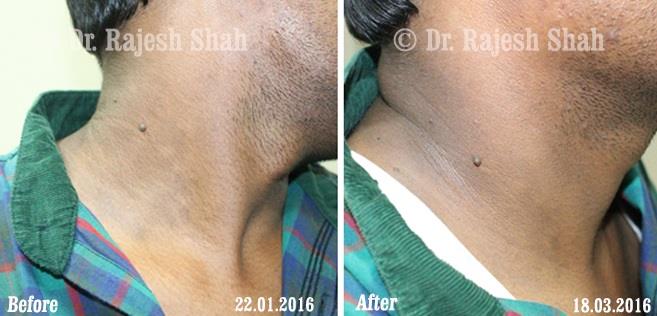
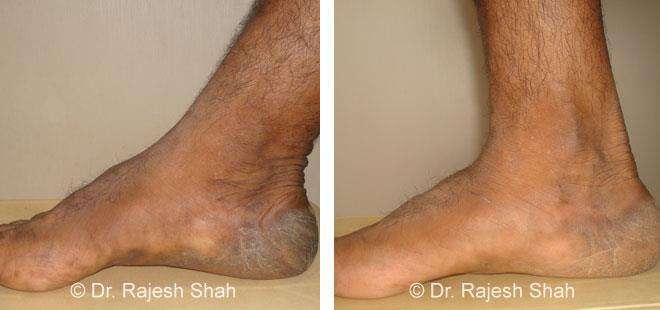
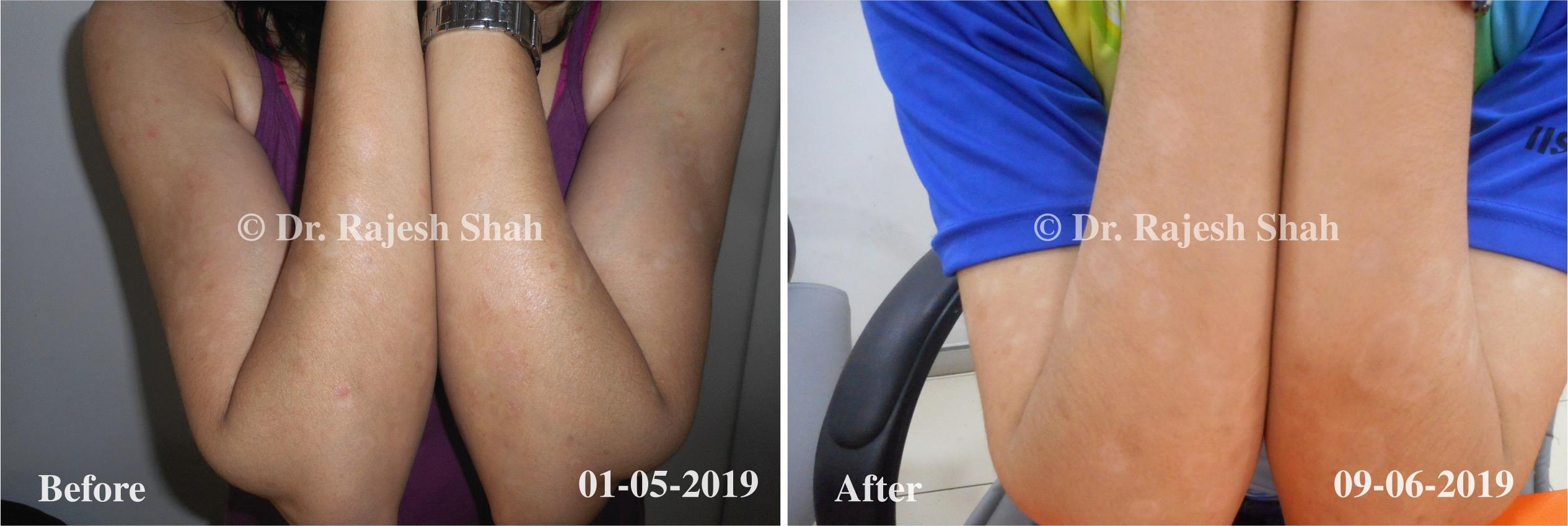
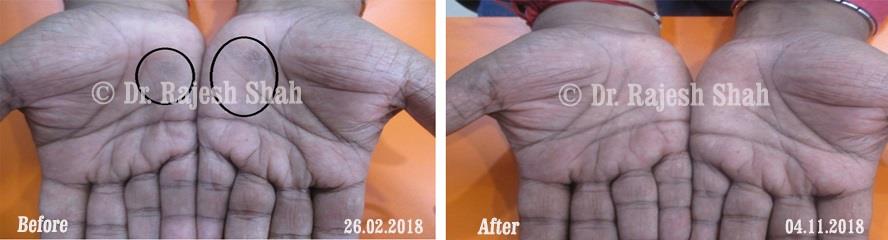
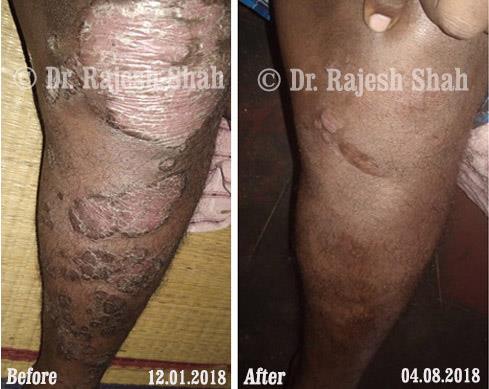
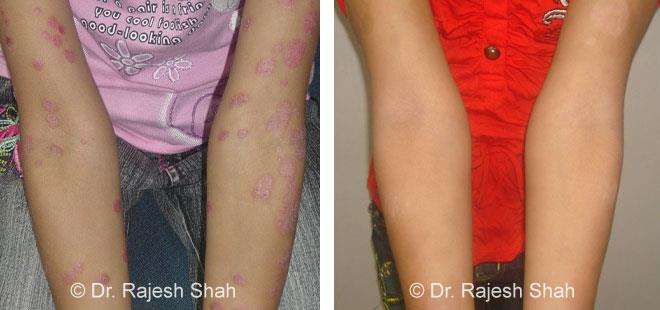
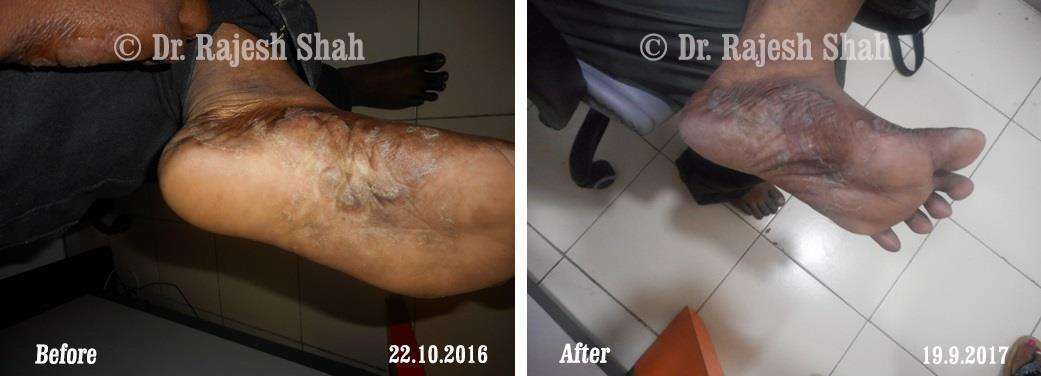
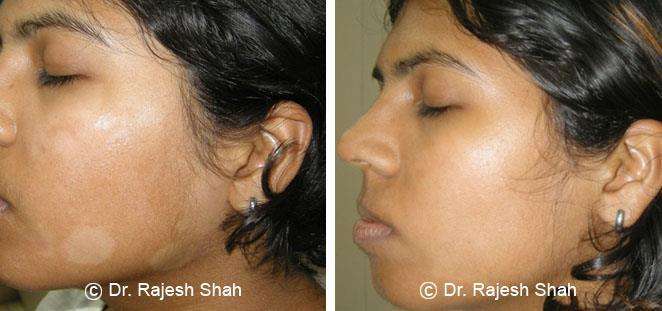
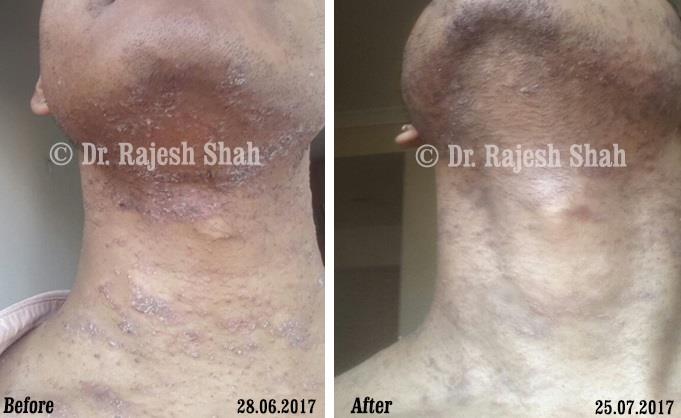
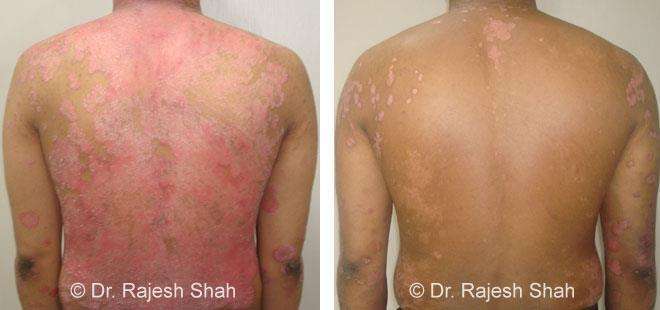
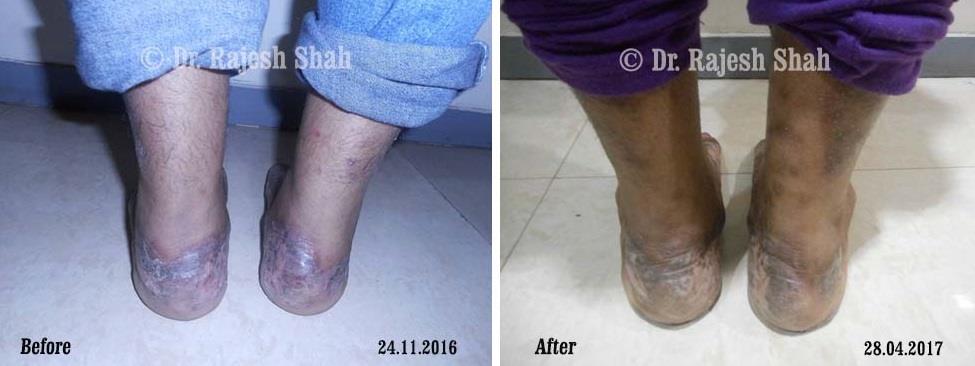
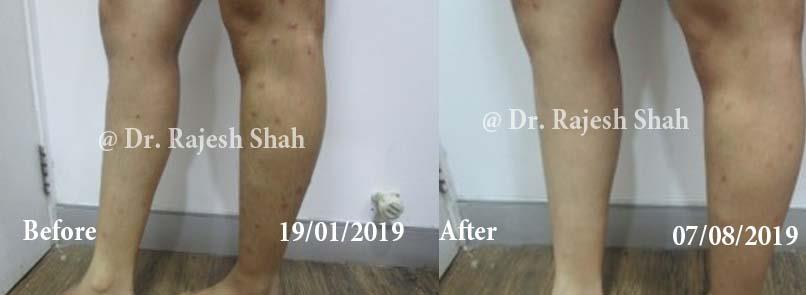
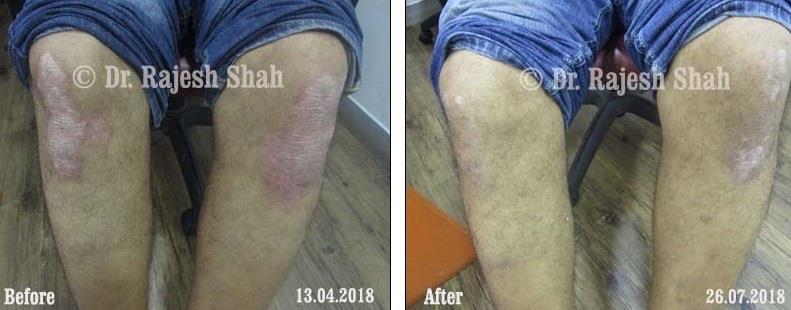
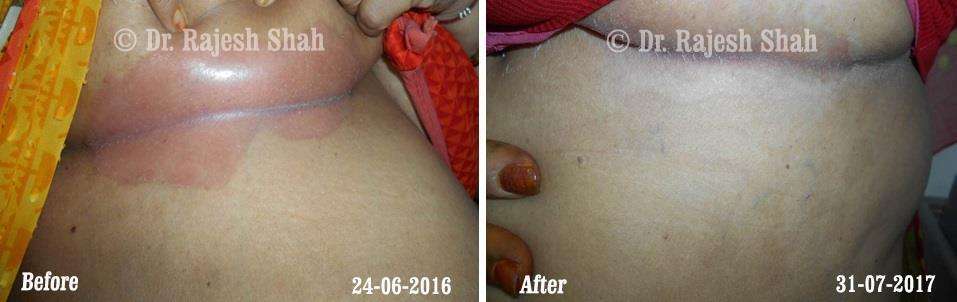
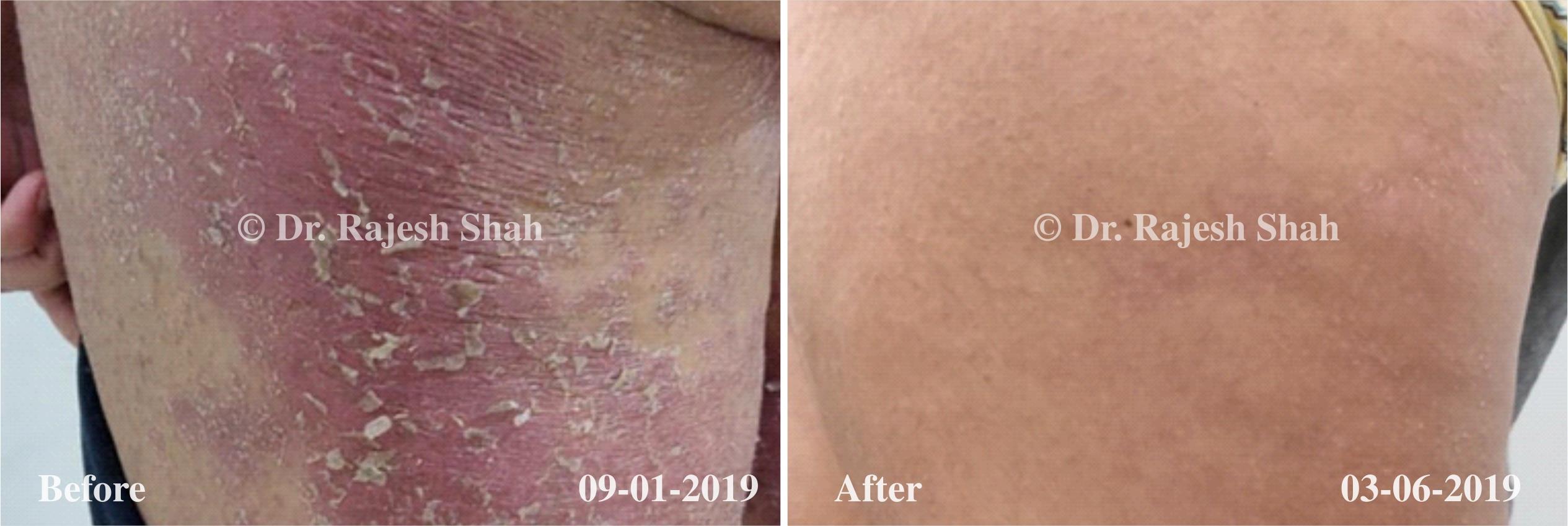
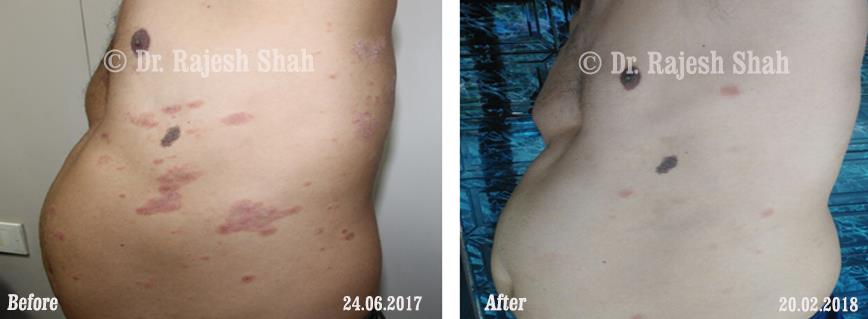
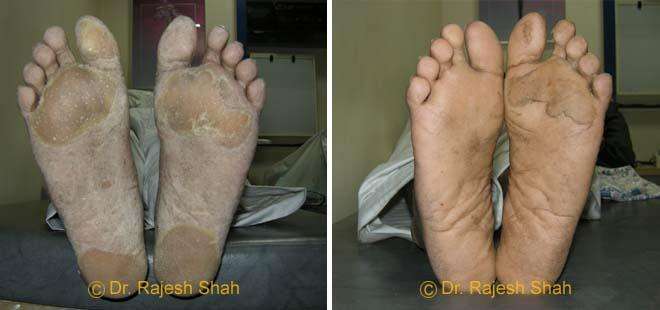
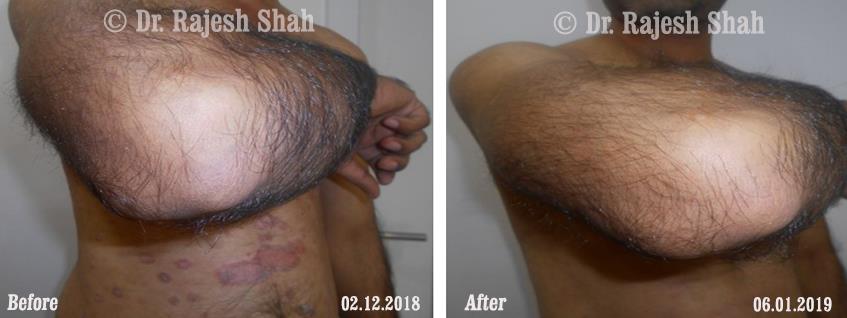
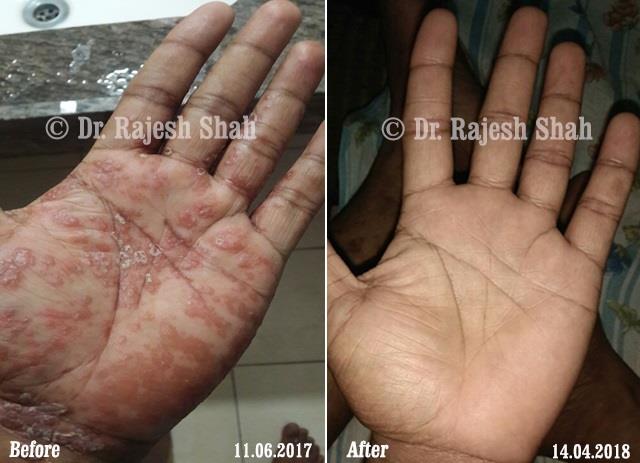
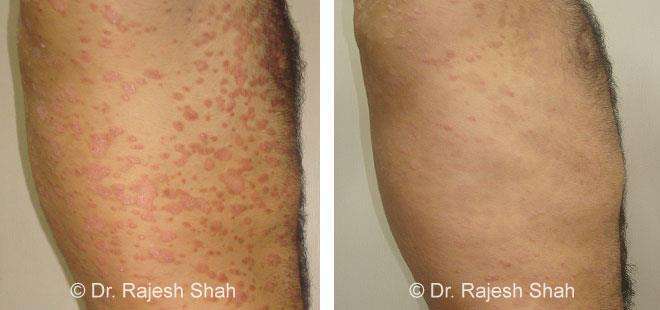
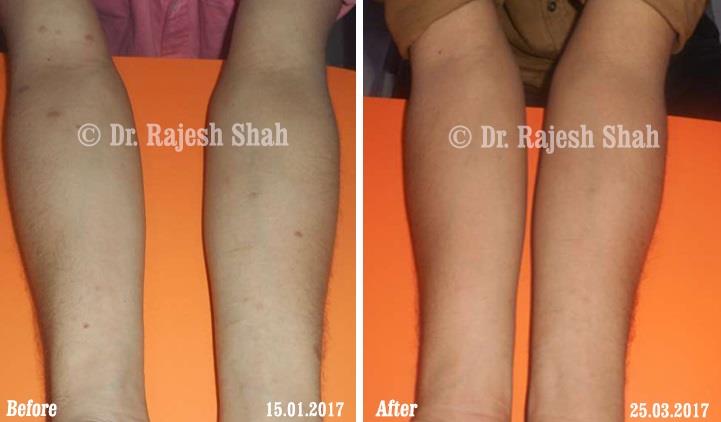
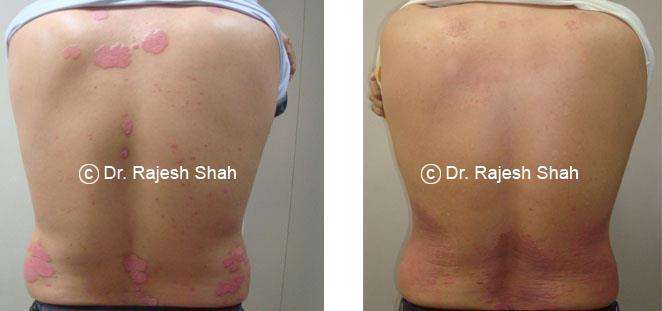
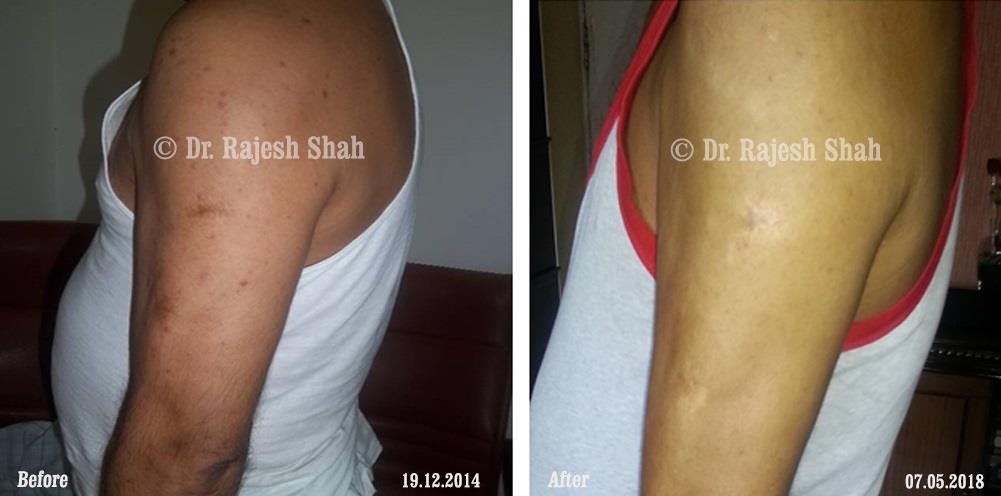
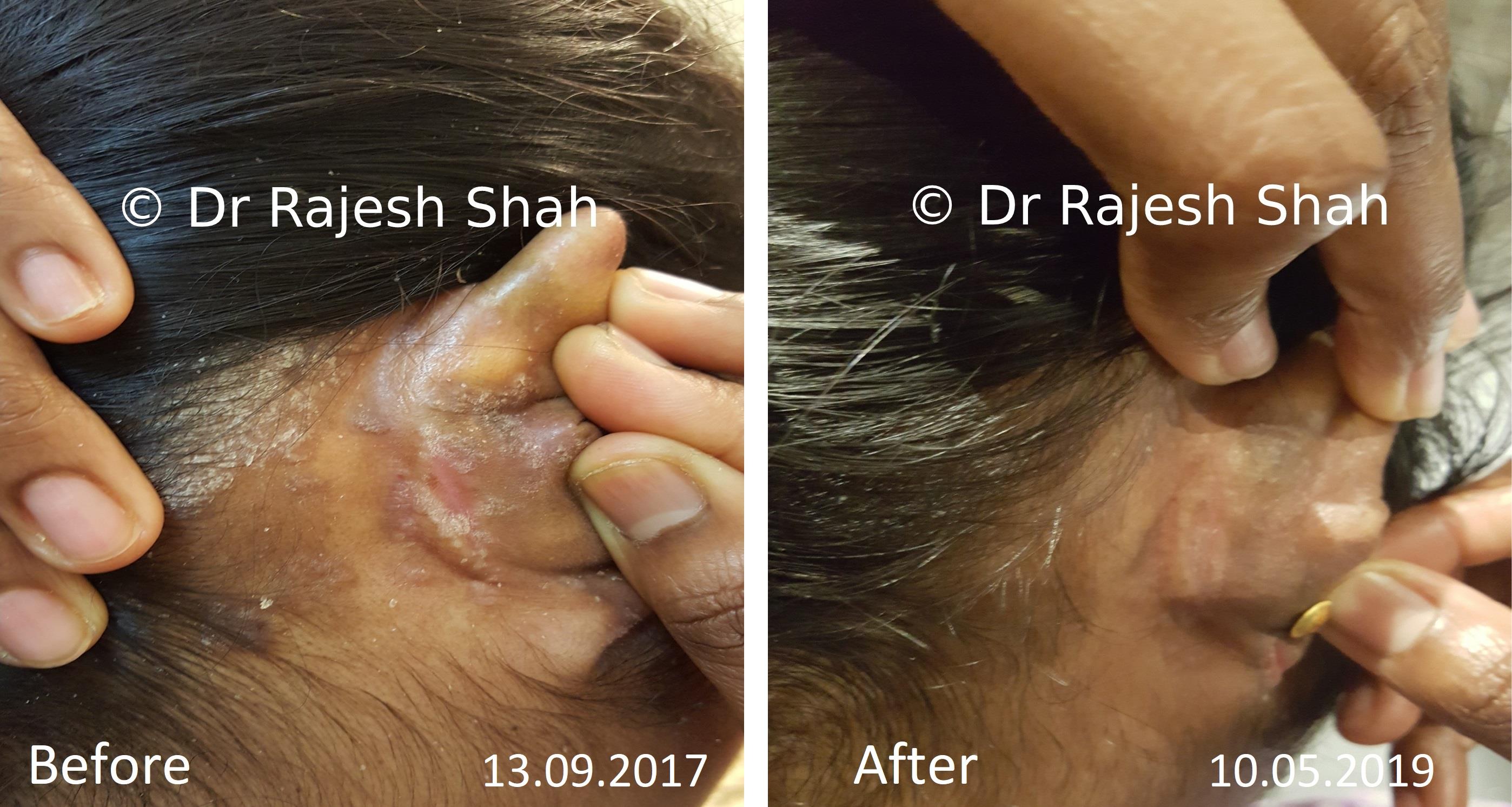
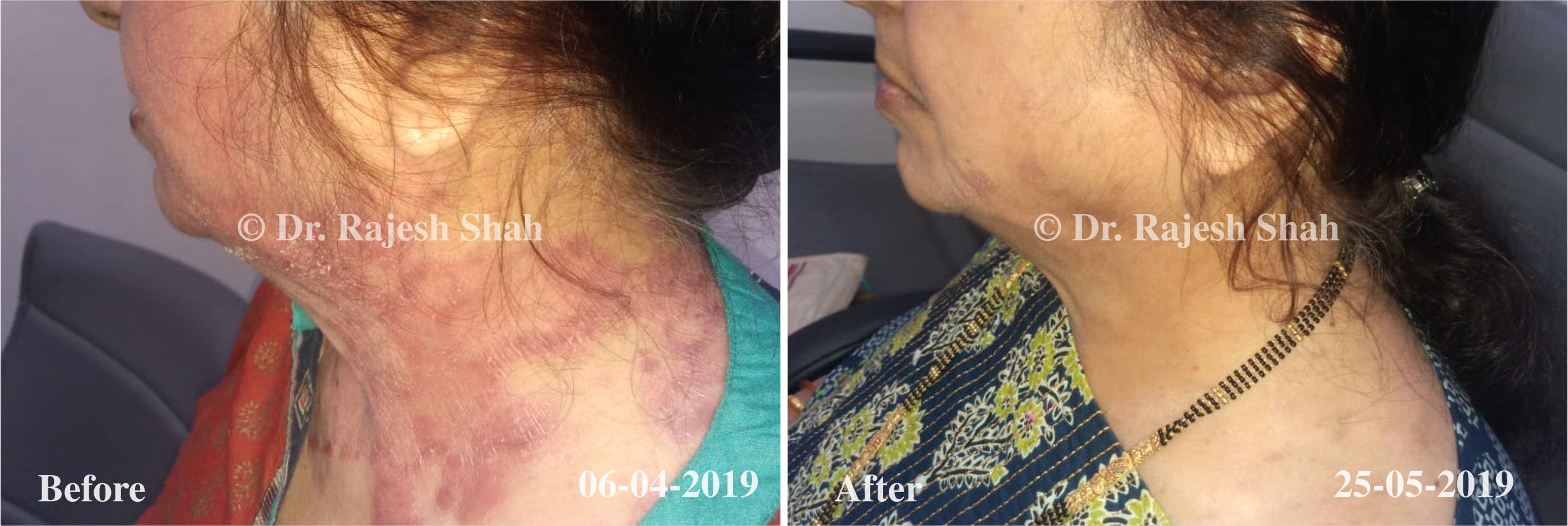
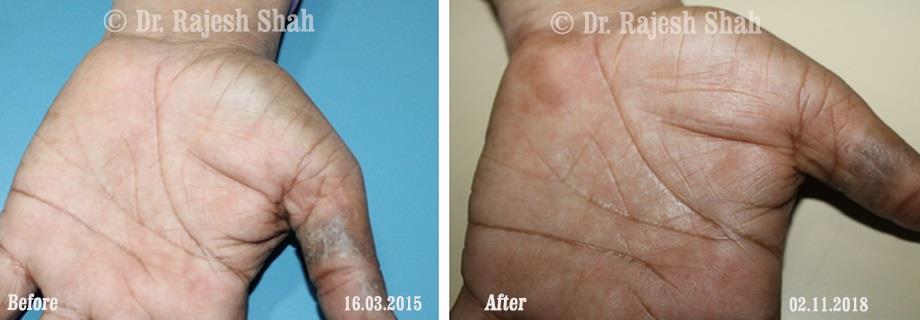
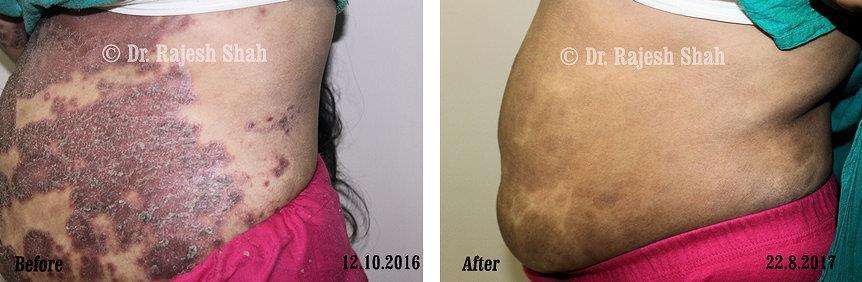
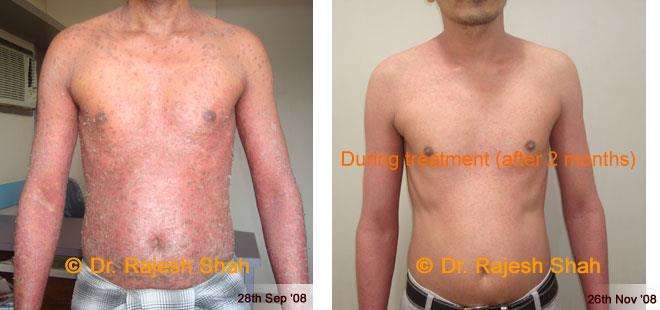
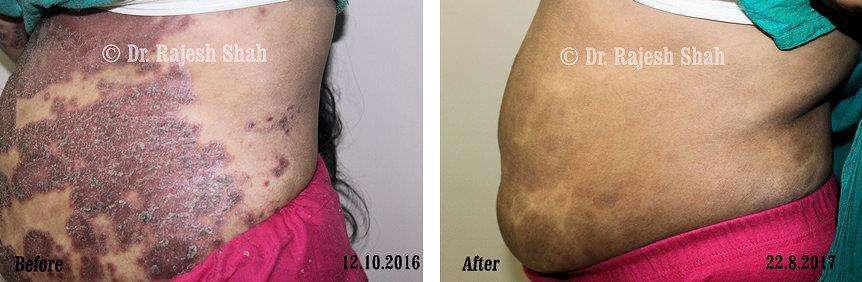
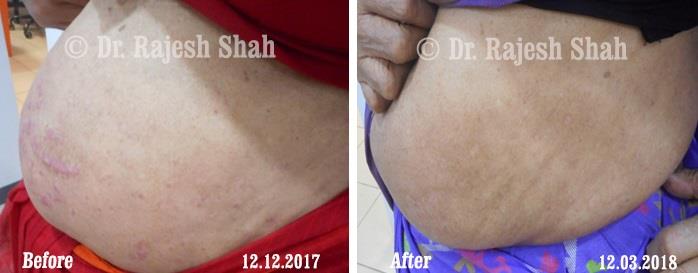
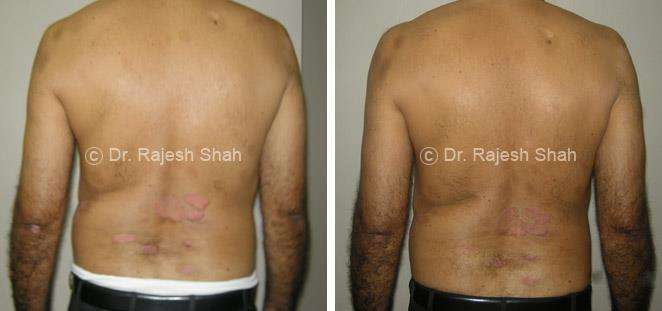
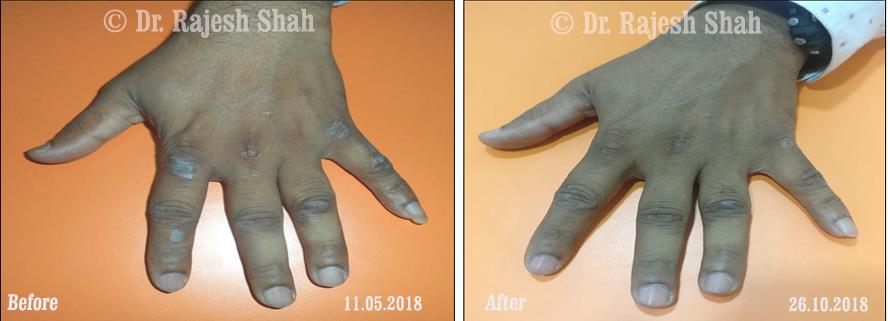
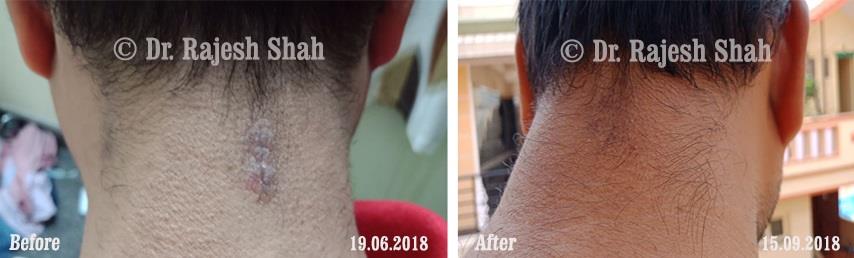
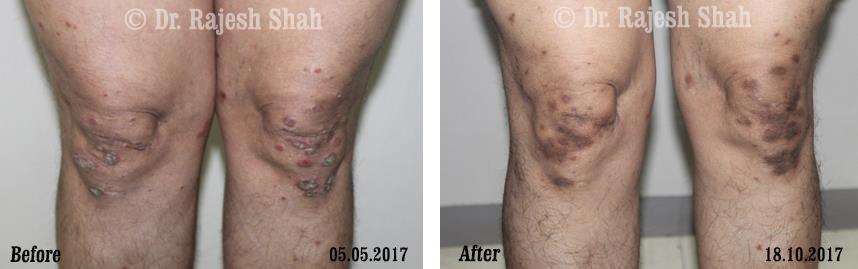
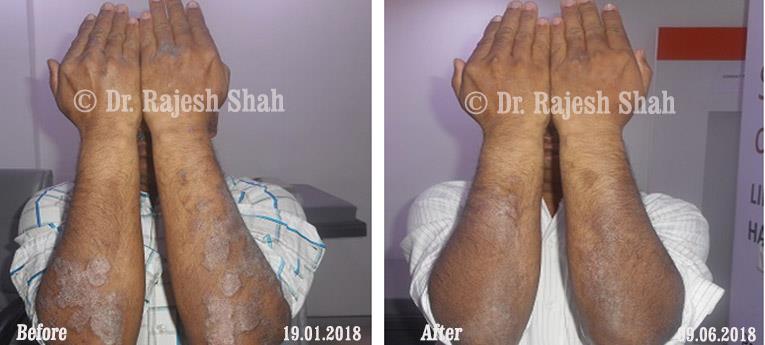
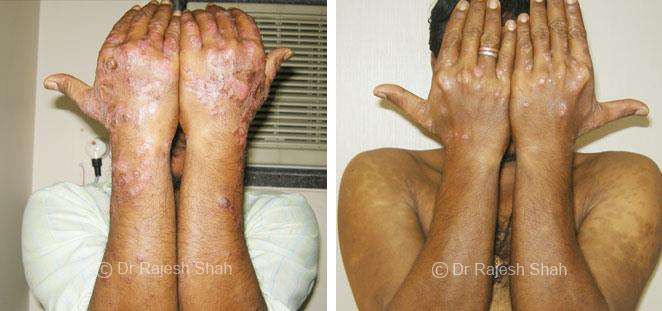
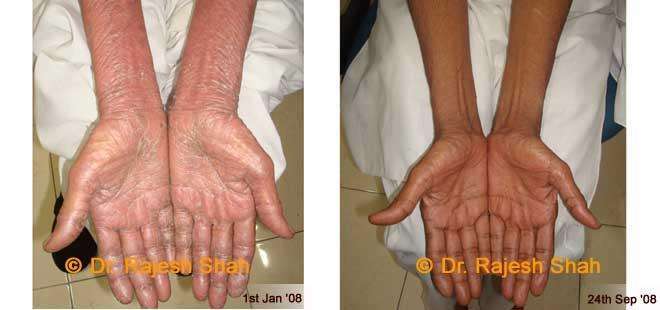
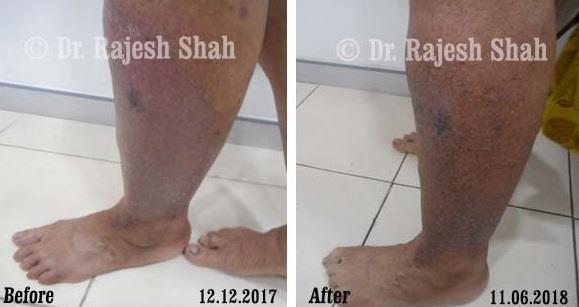
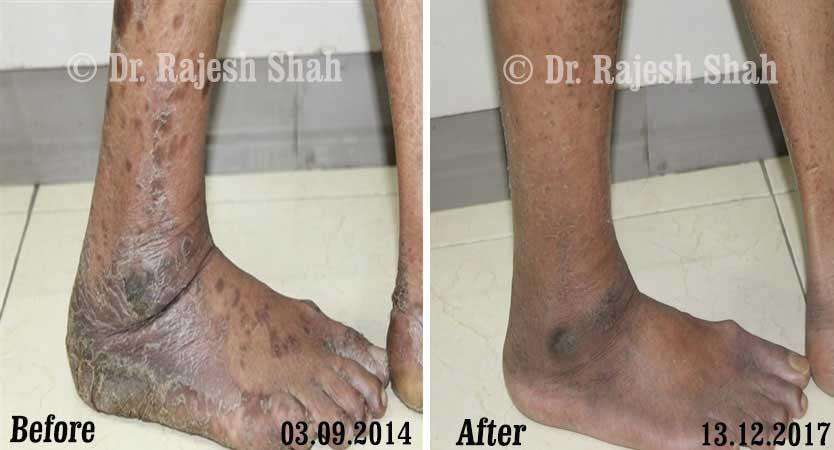
Real Case Outcomes
FAQ on Psoriasis
Expert Answers to Common Questions
Psoriasis is a chronic immune-mediated skin condition in which immune cells, especially T-cells, become overactive and release inflammatory cytokines. This leads to excessive production of skin cells, inflammation, and the formation of thick, scaly patches on the skin. Genetic and environmental factors both play a role in its development.
“Stage 4” generally refers to a severe form of psoriasis with extensive skin involvement affecting large areas of the body. Such cases may be more persistent and difficult to manage. Some patients may also develop associated joint involvement known as psoriatic arthritis.
Homeopathic treatment is based on an individualized approach and aims to support the body’s self-regulatory mechanisms and immune balance. Conventional treatments typically focus on reducing inflammation and suppressing immune activity through topical or systemic medications.
Homeopathic treatment may help reduce skin inflammation and immune hypersensitivity, which can lead to improvement in itching, redness, and scaling in many patients.
Itching in psoriasis results from immune-driven inflammation, increased sensitivity of skin nerves, and disruption of the skin barrier, which together cause dryness, irritation, and persistent itch.
Lifestyle measures that may support psoriasis management include reducing stress, maintaining regular sleep, using gentle skin care, and avoiding personal dietary or environmental triggers. Some individuals may benefit from limiting alcohol, smoking, and highly processed or inflammatory foods.
Psoriasis flare-ups may occur without a clear cause. Common triggers include stress, infections, weather changes (especially cold and dry conditions), alcohol, smoking, skin injuries, and exposure to certain chemicals or irritants.
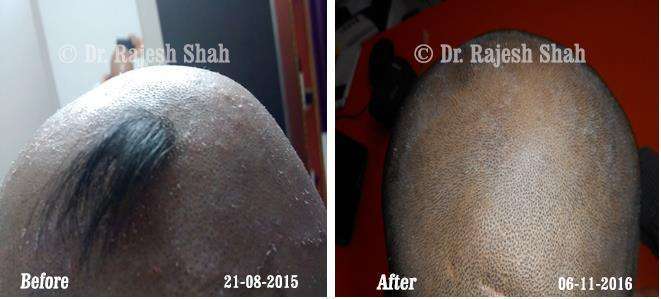
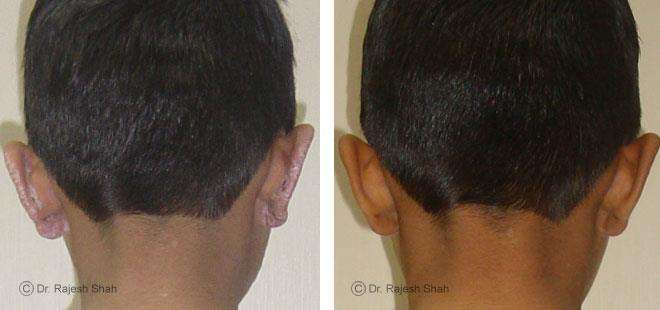
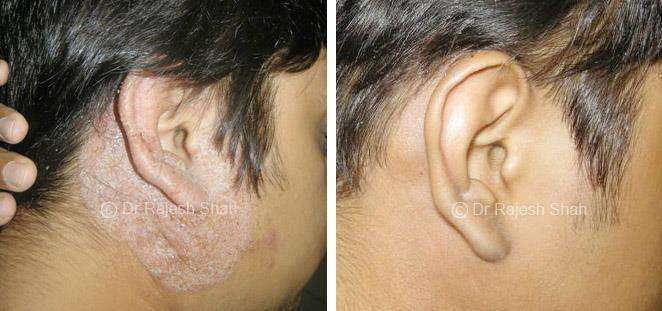
Scalp psoriasis follows the same disease mechanism as psoriasis elsewhere on the body. However, it can be more challenging to manage due to hair and frequent exposure to shampoos, dyes, and styling products.
Long-term use of corticosteroids and immunosuppressive medicines like methotrexate may be associated with side effects and potential disease rebound after discontinuation. These medications should always be used under medical supervision with regular monitoring.
Homeopathic medicines may be used alongside conventional treatments under medical supervision. Any reduction or discontinuation of conventional medicines should be done gradually and only on the advice of the treating physician.
Related Diseases
Ask Dr. Shah
Dr. Rajesh Shah, MD (Homeopathy), is a renowned Mumbai-based homeopath, recognized for treating patients from 180 countries, including celebrities and underprivileged individuals.
Contact Us