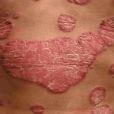
Dr. Rajesh Shah's Insights on Psoriatic Arthritis
In Dr. Rajesh Shah’s clinical experience, psoriatic arthritis treatment remains one of the most challenging areas in autoimmune care. Many patients who approach us have already been treated with strong immunosuppressants such as methotrexate, which often limits the response to psoriatic arthritis treatment in homeopathy. Tapering or discontinuing methotrexate can be difficult, as relapse is commonly seen soon after withdrawal.
At Life Force, our experience suggests that outcomes in psoriatic arthritis are modest, and expectations must remain realistic. While homeopathy may not reverse the condition in most cases, it can help support symptom control, reduce stiffness, and slow disease progression to some extent, especially when used alongside careful medical supervision.
180+
Countries
570+
Psoriatic Arthritis Patients Treated (Oct 2025)
30+
Team of Expert Doctors
40+
Years of Experience
100% Satisfaction
If you are not satisfied after 6 weeks of treatment, you may return the unused medicines and request a refund for the unused portion of services, in accordance with our policy. Our team is available to assist you through the refund process. No cure is assured within six weeks. For full terms, please visit our Detailed Refund Policy page.
What is Psoriatic Arthritis?
Psoriatic Arthritis (PsA) is a chronic autoimmune condition that affects the joints and connective tissues, often in people with psoriasis. It causes joint pain, swelling, stiffness, and fatigue. About one-third of people with psoriasis may develop PsA.
In some cases, joint symptoms appear before skin lesions, and a few individuals may not show visible psoriasis. PsA can occur at any age but is most common between 30 and 50 years and affects men and women equally. Early diagnosis and timely care are important for reducing joint damage and maintaining mobility.
Understanding Psoriatic Arthritis
Types of Psoriatic Arthritis
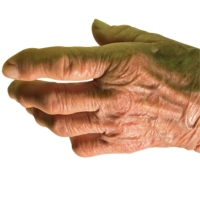
Asymmetric Oligoarthritis
Affects a few joints unevenly, often causing mild to moderate swelling and discomfort.

Symmetric Polyarthritis
Involves joints on both sides of the body, resembling rheumatoid arthritis in its presentation.
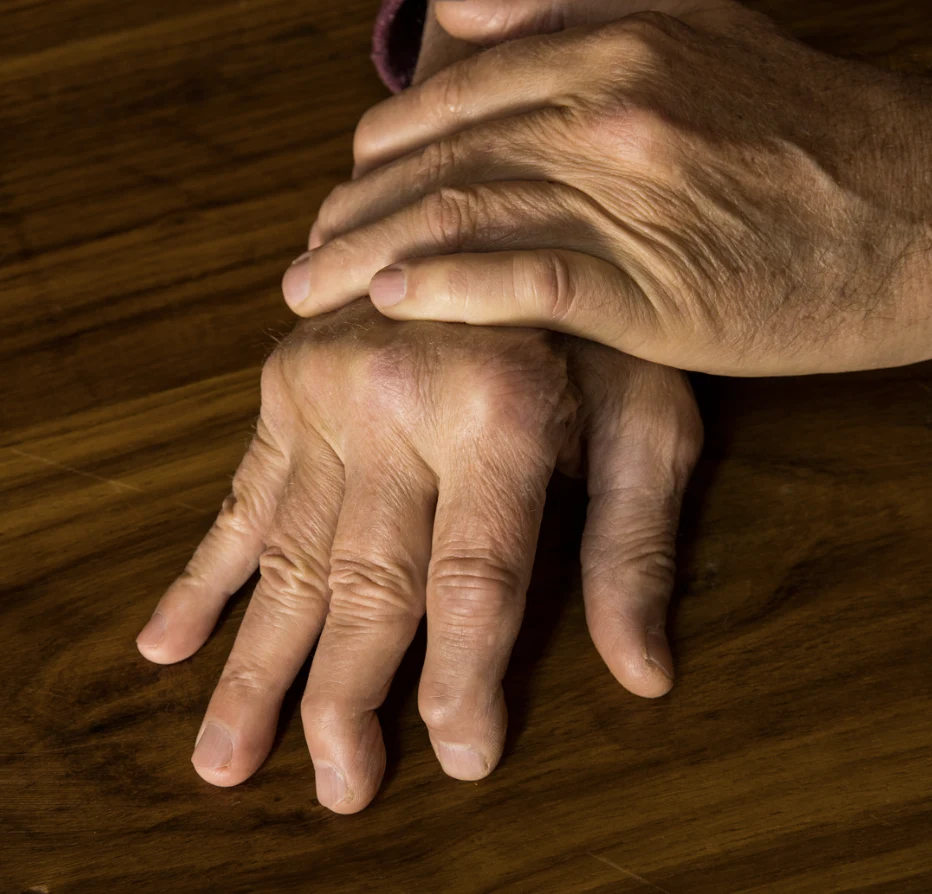
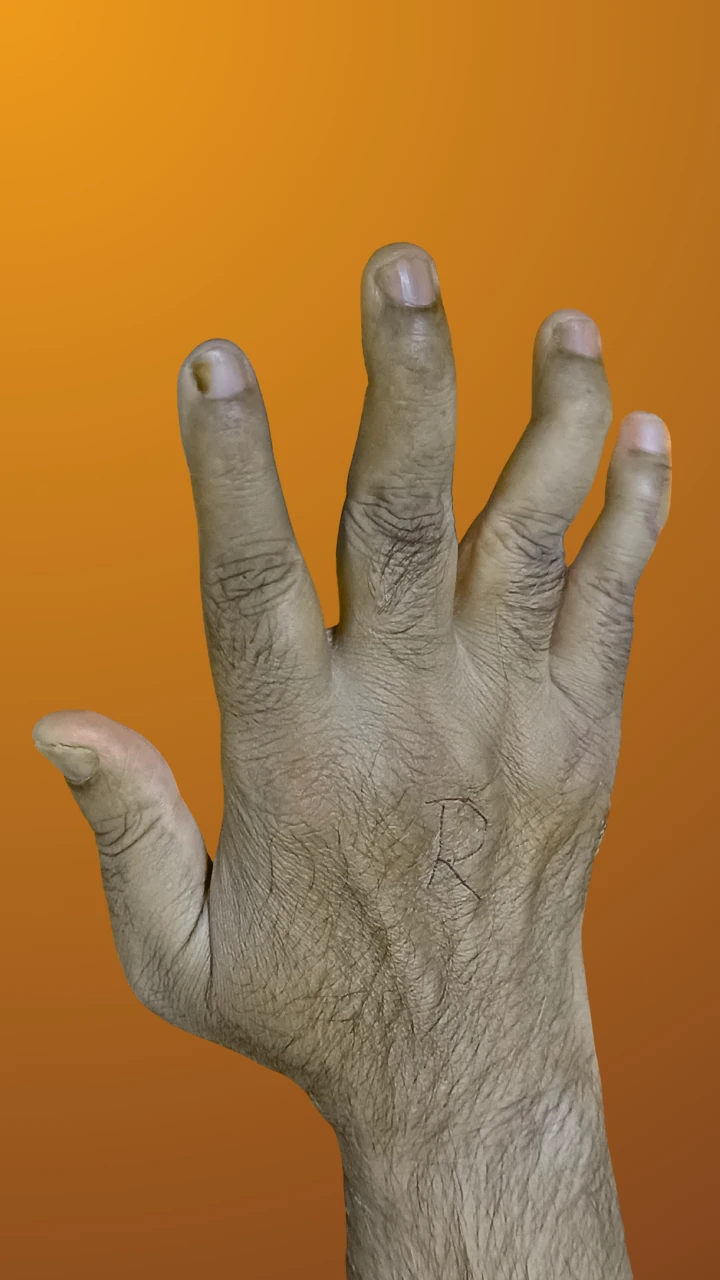
Distal Interphalangeal Predominant (DIP)
Primarily affects the small joints near the nails, leading to pain, stiffness, and nail changes.
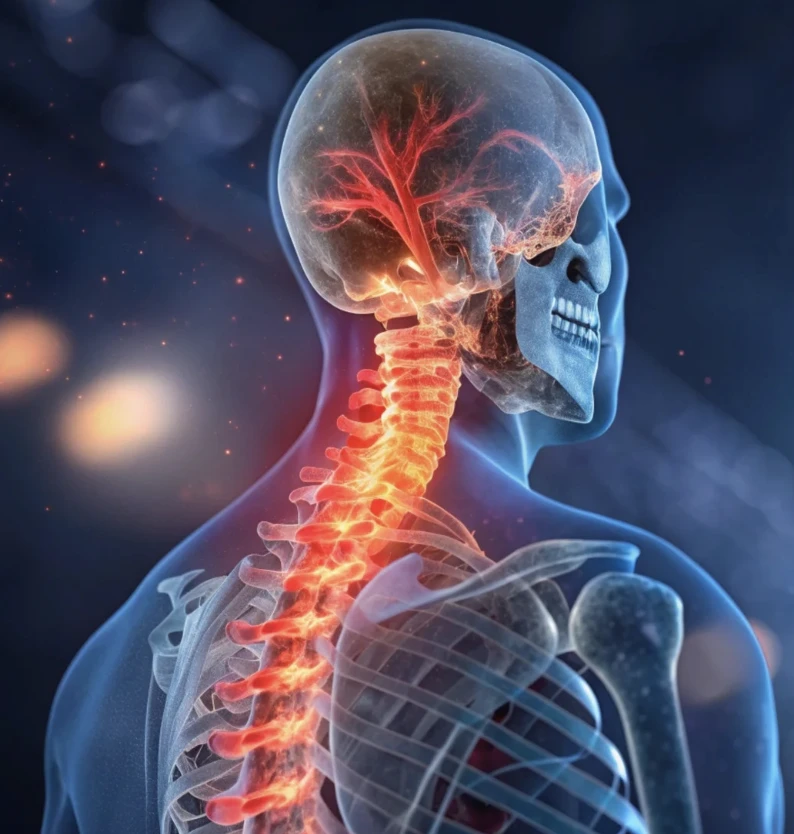
Spondylitis (Axial Psoriatic Arthritis)
Involves the spine and sacroiliac joints, causing back stiffness and reduced flexibility.
Our Expertise
At Life Force Homeopathy, Dr. Rajesh Shah’s experience indicates that homeopathy has a limited yet meaningful role in managing psoriatic arthritis. While a complete cure is unlikely, individualized care helps support joint comfort, mobility, and quality of life.
Experience in Managing Autoimmune and Chronic Conditions
With over four decades of experience, Life Force has managed multiple autoimmune and chronic inflammatory conditions, including psoriatic arthritis. The focus remains on addressing immune-driven inflammation while maintaining realistic expectations.
Integrated Care for Skin and Joint Involvement
Because psoriatic arthritis affects both skin and joints, an integrated care approach is essential. Homeopathy is often used alongside conventional treatment under professional guidance to support long-term disease control and daily functioning.
________________________________________
Homeopathy for Psoriatic Arthritis
Homeopathy offers a supportive and controlling approach to psoriatic arthritis treatment in homeopathy, aiming to reduce inflammation, improve mobility, and enhance daily comfort. Guided by Dr. Rajesh Shah’s clinical experience, treatment focuses on long-term symptom management and improved quality of life.
Case Studies

Psoriatic Arthritis
I wanted long-lasting solution for my Psoriasis and Psoriatic arthritis; I achieved it at Life Force
Mr. H.G.S. (Patient Identification Number: 21464) aged thirty-eight years visited Life Force on 6th August 2013 for the treatment of…

Psoriatic Arthritis
A Patient Got A Good Relief From Psoriatic Arthritis By Homeopathy At Life Force
A 51-years old lady, Mrs S.L. (Pin no- 28121) visited our Pune’s Life Force centre on 1st March 2016 with the…

Psoriatic Arthritis
Associated with the skin complaints also had pain in both the knees with occasional swelling since last 2 years
Mr. R .J (Patient Ref. No. L-6973) aged 43 yrs, reported to the clinic on August 10, 2004 with psoriatic…
-
Alopecia Areata
-
Ankylosing Spondylitis
-
Asthma
-
Cancer
-
Child Asthma
-
Eczema
-
Frequent Colds
-
Hair Fall
-
Hepatitis C
-
Irritable Bowel Syndrome (IBS)
-
Lichen Planus
-
Psoriasis
-
Trigeminal Neuralgia
-
Ulcerative Colitis
-
Underactive Thyroid
-
Urticaria
-
Vitiligo
Find out your chances of recovery, now
Select the disease from the list

STEP 01
Select your condition

STEP 02
Submit the Form

STEP 03
Get report Instantly
FAQ on Psoriatic Arthritis
Dr Rajesh Shah's Answers to Common Questions
Psoriatic arthritis is mainly diagnosed based on a detailed medical history and physical examination by the doctor. Imaging studies, such as X-rays of the affected joints, may support the diagnosis.
There is no single, definitive blood test for psoriatic arthritis. However, certain laboratory markers, along with imaging tests such as X-rays or CT scans, may help support the diagnosis in some cases.
The use of biologic medicines is considered one of the more recent advances in treating psoriatic arthritis.
Psoriatic arthritis is a chronic, progressive condition and, in many cases, requires long-term management.
Based on current medical understanding and clinical experience, psoriatic arthritis cannot be permanently cured at this time.
Homeopathic treatment may help slow disease progression, reduce pain and joint stiffness by controlling inflammation, and may help limit further joint damage to some extent. However, homeopathy does not claim to cure psoriatic arthritis.
Yes. Homeopathic treatment can be safely used alongside conventional medicines under proper medical supervision.
As psoriatic arthritis is a chronic condition, treatment is often required for many years and, in some cases, may be lifelong.
Yes. Early diagnosis and timely treatment aim to control inflammation and help prevent joint damage and deformities.
Yes. A healthy lifestyle can support overall management. This may include a balanced diet, reducing pro-inflammatory foods, maintaining a healthy weight, and engaging in regular, appropriate exercise.
Both are autoimmune conditions. Rheumatoid arthritis typically causes symmetrical joint inflammation and is associated with a positive rheumatoid factor, without skin involvement. Psoriatic arthritis is associated with psoriasis and often presents with asymmetric (one-sided) joint involvement.
Yes. In rare cases, psoriatic arthritis may develop even in the absence of visible skin psoriasis.
Yes. Psoriatic arthritis can affect the spine and other joints of the back.
Yes. Psoriatic arthritis can involve any joint in the body, but the hands, fingers, knees, feet, and toes are commonly affected.
Based on our clinical experience at Life Force, prolonged use of immunosuppressive medicines such as methotrexate may make psoriatic arthritis more challenging to manage with homeopathy. Long-term suppression of the immune system can reduce the body’s responsiveness to homeopathic treatment.
Ask Dr. Shah
Dr. Rajesh Shah, MD (Homeopathy), is a renowned Mumbai-based homeopath, recognized for treating patients from 180 countries, including celebrities and underprivileged individuals.
Contact Us